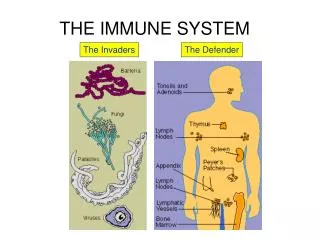
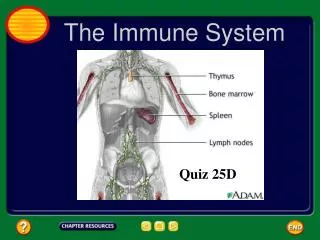
THE IMMUNE SYSTEM.
THE IMMUNE SYSTEM. Introduction. INTRODUCTION. Is a bodywide network of cells and organs that has evolved to defend the body against attacks by “ foreign “ invaders. Its success relies on incredibly elaborate and dynamic communications and interactions among millions of cells.

THE IMMUNE SYSTEM.
E N D
Presentation Transcript
THE IMMUNE SYSTEM. Introduction.
INTRODUCTION. • Is a bodywide network of cells and organs that has evolved to defend the body against attacks by “ foreign “ invaders. • Its success relies on incredibly elaborate and dynamic communications and interactions among millions of cells. • The result is a system that produces a response prompt, appropriate,effective & self-limiting.
TYPES OF IMMUNITY. • Nonspecific: Skin and mucous membranes, Phagocytosis, Inflammation, and The Complement System. • Specific: Humora(Antibody-Mediated) and Cell-Mediated.
THE SKIN: First Line Of Defense. • Repels many organisms: difficult to get through. • Epithelium lines all body systems exposed to external environments including the respiratory, digestive and urinary systems. • Secretes liquid which are mildly acidic which hinder bacterial growth. • Stomach secretes HCL.
Tears and saliva contain lysozymes which dissolve the wall of bacteria. • Cilia of respiratory tract trap bacteria in mucus.
SKIN AND MUCOUS MEMBRANES:1st line of defens • Mechanical Factors: • Skin. • The Epidermis. • Keratin. • Mucous Membranes. • Lacrimal Apparatus------> • Cilliary Escalator.
Epiglottis. • Urine and Vaginal secretions.
CHEMICAL FACTORS. • Sebum. • Perspiration. • Gastric Juice. • Transferrins.
NORMAL MICRIBIOTA AND NONSPECIFIC RESISTANCE. • Microbial Antagonism. • Commensalism. • Competitive Exclusion: Opportunistic pathogens.
PHAGOCYTOSIS: 2ND LINE OF DEFENSE. • Cell Eating. • Phagocytes: Cells that perform phagocytosis. • Are mostly types of white blood cells or derivatives of white blood cells.
FORMED ELEMENTS IN BLOOD. • Plasma contains formed elements.Leukocytes: white blood cells. • Leukocytosis. • Leukopenia. • Differential white blood cell count.
LEUKOCYTES. • Divided into two main categories based on their appearance under the light microscope: • Granulocytes Versus Agranulocytes. • Granulocytes: Neutrophils(stain lilac), Basophils(stain blue-purple), and Eosinophils(stain red or orange).
NEUTROPHILS • Commonly called polymorphonuclear leukocytes(PMNs). • Multinucleated. • Highly phagocytic and motile. • Active in the initial stages of infection.
BASOPHILS. • Role is not clear. • Release substances, such as histamine, that are important in inflammation.
Eosinophils. • Somewhat phagocytic. • Have the ability to leave to leave the blood. • Major function is to produce toxic proteins against certain parasites such as worms.
AGRANULOCYTES. • Monocytes. • Macrophages. • Lymphocytes.
MONOCYTES. • Not actively phagocytic until they leave circulating blood, enter the body tissues, and mature into macrophages.
MACROPHAGES. • Maturation and proliferation of is one factor that is responsible for the swelling of lymph nodes during an infection. • Also dispose of worn out blood cells.
LYMPHOCYTES: B and T. • Not phagocytic, but play a key role in specific immunity. • Occur in lymphoid tissues of the lymphatic system. • They also circulate in the blood.
ACTION OF PHAGOCYTIC CELLS. • Wandering macrophages. • Fixed macrophages. • Mononuclear phagocytic (reticuloendothelial) system. • During the initial infection, granulocytes, especially neutrophils are many and they dominate.
As the infection progresses, the macrophages dominate; they scavenge and phagocytize remaining living bacteria, and dead or dying bacteria.
THE MECHANISM OF PHAGOCYTOSIS. • Chemotaxis. • Adherence. • Ingestion. • Digestion.
INFLAMMATION: Second line of defense. • Inflammatory response results in increased blood flow to infection; chemical attractants and flow of fluid to wound ( vasodilation). • Together these cause swelling, heat, and pain. • Fluids include histamine( causes arterioles to dilate), and plasma( contains clotting factors to wall off area.
Kinins: cause vasodilation and increased permeability of blood vessels. • Prostaglandins: released by damaged cells, and intensifies the effects of histamin and kinins. • Leukotrienes: produced by mast cells and basophils- Cause increased permeability, and attract phagocytes to pathogens.
Vasodilation and increased permeability of blood vessels also help to deliver clotting elements to injured area. • Blood clots prevent microbe from spreading, so a localized collection of pus results(abcess).
PHAGOCYTE MIGRATION. • Flow of blood decreases, phagocytes stick to the inner surface of the endothelium( lining) of the blood vessels( margination). • Collected phagocytes squeeze b/w the endothelial cells like amoeba(emigration/diapedesis). • Phagocytes destroy microbes by phagocytosis.
TISSUE REPAIR. • Final stage of inflammation.Ability of tissue to repair or regenerate, depends on type of tissue.
FEVER. • Chemical attractants which include interleukin, formerly referred to as pyrogen are released by macrophages exposed to bacteria. • Sends signal to hypothalamus to raise body temperature. • Fever increases metabolism and inhibits bacterial reproduction.
ANTIMICROBIAL SUBSTANCES. • Complement System: • Composed of many blood proteins. • No specific response to infection • Inactive state till needed. • When needed it starts a chain of “fighting proteins”. • Final 5 proteins create a “membrane attack complex”.
Membrane attack complex creates a hole in the microorganism, into which water flows causing the microbe to burst. • Some chemical attractant proteins flag down WBC cell types. • Components include C1 through C20.
INTERFERONS. • Counters viral infection. • Principal function is to interfere with viral multiplication. • Are host- cell- specific. • Produced by human cell. • Protect human cells, but produce little antiviral activity for cells of other species.