The Immune System
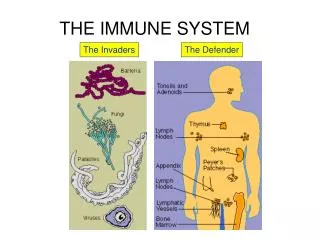
The Immune System. The body’s protective response to invading foreign organisms. Immune System: Functions. Protects from pathogens and foreign molecules Parasites Bacteria Viruses Removes dead/damaged cells Attempts to recognize and remove abnormal cells. Immune System: Pathologies.

The Immune System
E N D
Presentation Transcript
The Immune System The body’s protective response to invading foreign organisms
Immune System: Functions • Protects from pathogens and foreign molecules • Parasites • Bacteria • Viruses • Removes dead/damaged cells • Attempts to recognize and remove abnormal cells
Immune System: Pathologies • Incorrect responses • Autoimmune disease • Overactive responses • Allergies • Lack of response • Immunodeficiency disease (AIDS)
Body Defenses: Two Lines • First line of defense • Physical and chemical barriers: • Skin, epithelial linings, and cilia • Acids, mucous, and lysozymes • Second line of defense • Innate, non-specific, immediate response • Acquired; attack a specific pathogen (antigen)
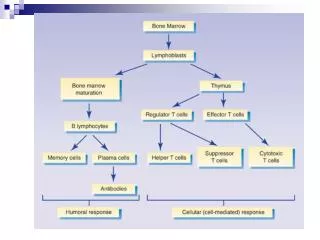
3 processes needed for immunity: Inflammation Immunity Antibody-mediated/Humoral Cell-mediated Immunity
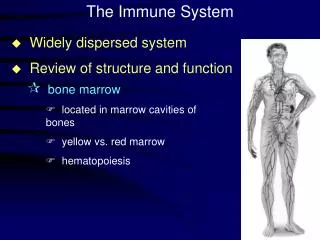
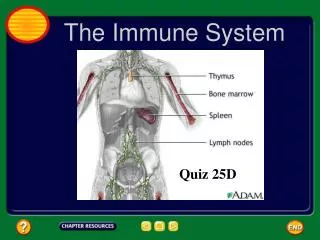
Lymphatic System: Anatomy Figure 24-2a
Key Cells of the Immune System Leukocytes (white blood cells)
Cells • Leukocytes: 5 major categories. • Neutrophils: Phagocytic cells that wander throughout the connective tissue destroying bacterias. • Eosinophils: Phagocytic cells that destroy allergens, antigen & anti-body complexes, & some inflammatory chemicals. • Surround larger parasites & attack them with enzymes to weaken or destroy them. • Defend against allergies & parasitic worm infections. • Basophils: Helper cells that secrete vasodilators & anticoagulants in order to speed other leukocytes to the infected zone.
Cells • Lymphocytes: A variety of cells active in the immune response. • Natural Killer Cells (NK Cells): Attack any cell with an unusual plasma membrane, such as cells that are infected by a virus or have become cancerous. • Cytolysis: Perforin protein is injected into the cell to cause it to “explode”. • Granzymes: Cause the cell to self-destruct. • Found in the spleen, red bone marrow, & lymph nodes. • Monocytes: Wandering cells that eventually turn into macrophages.
Inflammation(natural immunity) • Inflammation: One of the body’s most common responses to tissue damage. Occurs in roughly the same way in any tissue. • Four Cardinal signs of Inflammation: • Redness • Swelling • Heat • Pain
Major cells of inflammation: • Neutrophils: • 1st line defense against invaders in blood and ECF. • Destroy invaders by phagocytosis • Absolute neutrophil count is used to determine a person’s risk for infection
Major cells of inflammation: • Macrophages • Preform phagocytosis, repair injured tissue • Stimulate CMI + AMI • Long life span and plenty of energy to degrade many foreign proteins.
Cells Phagocytes Cells under attack release histamine. Purpose is to engulf and destroy invaders
Major cells of inflammation: • Basophils • Cause the manifestation of inflammation • Contain chemicals that act on b. vessels • Heparin inhibits blood clotting • Histamine constricts small veins & respiratory smooth muscle
Major cells of inflammation: • Eosinophils • Act against infestations of parasitic larvae • Can inhibit and induce inflammation • Number increases during allergic reaction
Immune System Specific Immune Defenses: Cells specifically geared toward fighting certain invaders, and remembering previous foreign invaders so that they can be rapidly eliminated in the future.
Immune System • Two Divisions of the Immune System: • Humoral Immunity aka Antibody-Mediated Immunity: • Driven by B cells. • Cell-mediated immunity: • Driven by T cells.
What is specific immunity? • Specific response • Memory for future reinvasion • Antibody-based • B cells primary actors • Cell-mediated • T cells only
Antigens • Antigen: • Typically large molecules, often proteins.
Antigen Processing • Major Histocompatability Complex (MHC): “Self-antigens” that are unique to all of your body cells except red blood cells. • Help T-cells recognize which cells are foreign. • MHC-1s: Cells that posses MHC and are labeled “you” by the T-cells.
Antibodies • Also known as immunoglobulins • Some act as labels to identify antigens for phagocytes • Some work as antitoxins • i.e. block toxins for e.g. those causing diphtheria and tetanus • Some attach to bacteria making them less active • easier for phagocytes to engulf • Some cause agglutination (clumping together) of bacteria
Humoral Immunity • Humoral Immunity aka Antibody-Mediated Immunity • B cells (B-lymphocytes) produce antibodies to engage in a complex purging process. • Immunoglobulins (Igs) • Antibodies made up of glycoproteins called globulins. • Antigen-Binding Site • Tips of each chain are called variable regions & are areas where the antibody attaches to the antigen.
B -Lymphocytes • Receptors recognize an antigen on the surface of the invader, the B-cell divides rapidly. • Antigens are presented to the B-cells by macrophages
When help arrives . . . Antigen & T-helper cell Naïve cell Proliferation of cell line The T-helper cell receptor “docks” with the B cell’s MHComplex B cells proliferate . . .
B cells differentiate into . . . Antigen & T-helper cell antibodies memory • Antibody producing cells [attack mode] • Memory cells [remembers & future protection]
AMI in summary • An invaders attacks… • Antigen is phagocytized by the B cell • Broken into non-infective pieces & attached to MHC which is placed on the cell membrane surface here it is recognized by the helper T cell…
Cell Mediated Immunity • Cellular Immunity: • Lymphocytes directly attack & destroy foreign cells & infected host cells. • T-Cells or T-lymphocytes activated by a specific antigen.
Cellular Immunity • Types of T-Cells involved in Cell-mediated Response: • Cytotoxic T-Cells: Responsible for actual attacking of the foreign body or infected cell. • Helper T-Cells: Stimulate other helper T-cells, cytotoxic T-cells, and B cells. • Suppressor T-Cells: Help regulate the attack & prevent tissue destruction. • Memory T-Cells: Remain as an immune response and stimulate faster responses if the same antigen invades again.
T Lymphocytes: Cell-Mediated Roles of T lymphocytes and NK cells in cell-mediated immunity Figure 24-16
What happens in a cell-mediated response? • The key events: • Surveillance and recognition • Attack • Memory
Types of Immunity Active Immunity: You encountered the pathogen yourself and developed your own antibodies to it. Passive Immunity: You received antibodies directly introduced into the body. Naturally Acquired: Antibodies are received through natural means. Artificially Aquired: Antibodies are received through artificial (scientific) methods.
Vaccination A preparation containing antigenic material: • Whole live microorganism • Dead microorganism • Attenuated (harmless) microorganism • Toxoid (harmless form of toxin) • Preparation of harmless ags
Disorders of the Immune System • Hypersensitivity Disorders • Allergy • Anaphylaxis • Transfusion reactions, transplant rejection • Immunodeficiency Disorders • HIV/AIDS • Autoimmune • Systemic lupus erythematosus, rheumatoid arthritis etc.
Hypersensitivity • Excessive reaction to an antigen (allergen) to which most people do not react • Includes • Allergies • Transplant reaction • Transfusion
Hypersensitivity Disorders • Reaction may be Local (gastrointestinal, skin, resp, conjuctaval) or systemic (anaphylactic) • Q: What factors affect the severity of a hypersensitivity reaction? • Host response • Exposure amount • Nature of the allergen • Route of allergen entry • Repeated Exposure (
Hypersensitivity Assessment • Subjective Information • Pruritus, nausea and uneasiness • History of present illness • Onset, frequency and duration of symptoms • Nature and progression of s/s • Possible exposures of known allergens/common allergens • Chronic, seasonal or single episode • Aggravating & alleviating factors
Hypersensitivity Assessment • Physical Assessment • Respiratory • S/Sx caused by Bronchoconstriction—SOB, difficulty breathing, wheezing, & coughing • Sneezing, excessive nasal secretions, inflamed nasal membranes • Cardiovascular • S/Sx caused by Vasodilation—Flushing, Hypotension, Edema • Shock followed by cardiovascular collapse and respiratory arrest • GI • Nauses, vomiting, diarrhea • Skin • Rash, areas of raised inflammation (urticaria/hives)
Hypersensitivity Studies & Medical Management • Studies—CBC, Total serum IgE levels, skin testing • Medical Management • Immediate intervention • Symptom management & long term control • Environmental control
Hypersensitivity—Medications • Oxygen—if respiratory assistance needed • Bronchodilators • Emergency bronchodilator—Epinephrine 1:1,000 SQ–Anaphylactic reactions (may need to following with IV Epi) • Antihistamines—symptom management & long term control • First Generation—Prototype Diphenhydramine • Second Generation—Prototype Fexofenadine • Leukotrieneinhibitors—Inhibits the release of leukotrienes from mast cells & basophils) • Prototype—montelukast (Singulair) • Steroids—symptom management & long term control • Systemic—Prototype Prednisone
Allergies • When the immune system responds to harmless substances • Allergens – antigenic substances • Allergens include house dust, animal skin, pollen, house dust mite and its faeces
Immunoglobulins and Allergic Response • Allergen triggers the B cell to make IgE antibody, which attaches to the mast cell; when that allergen reappears, it binds to the IgE and triggers the mast cell to release its chemicals