Digestive System Digestive Glands
850 likes | 1.85k Views
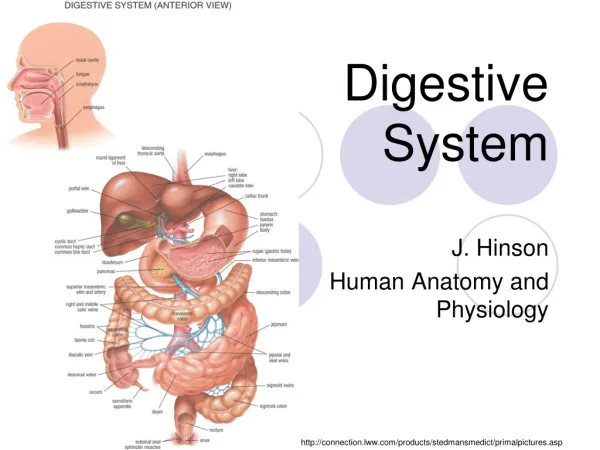
Digestive System Digestive Glands. Components of Digestive Glands. Salivary glands Pancreas Liver. Small digestive glands: found in the wall of digestive tract Accessory glands (large digestive glands). General structure of Digestive Glands. Parenchyma: (functional portion of an organ )

Digestive System Digestive Glands
E N D
Presentation Transcript
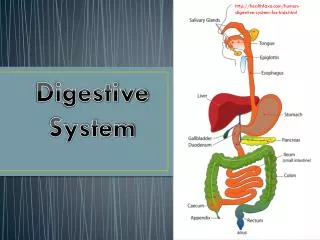
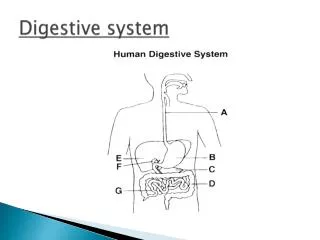
Digestive System Digestive Glands
Components of Digestive Glands Salivary glands Pancreas Liver • Small digestive glands: found in the wall of digestive tract • Accessory glands (large digestive glands)
General structure of Digestive Glands • Parenchyma:(functional portion of an organ) acini/gland cells ducts • Stroma: (non-functional portion of an organ) capsule CT inside the organ
Salivary Glands General structure of the large salivary glands Serous acinus Mucous acinus Seromucous/mixed acinus acinus Parenchyma Intercalated duct Striated/secretory duct Interlobular duct Excretory duct duct
Salivary Glands Structural characteristic of gland cell: Serous acinus:comprised by serous cells. ﹡zymogen granulesin apical cytoplasm. Mucous acinus:comprised by mucous cells. ﹡mucinogen granulesin cytoplasm. Seromucous acinus: comprised by both cells. /mixed acinus﹡demilume
Serous acinus ﹡zymogen granulesin apical cytoplasm.
Serous cell: Basal lamina(bl); Connective tissue (ct); Desmosome (d); Endothelium (en); Golgi comples (g); Intercellular space (is); Lumen (l); Microvilli (mi); Mitochondria (m); Nucleus (nu); RER (re); Secretion granule (sg). 10.000x
Mucous acinus: ﹡mucinogen granulesin cytoplasm.
Detail of mucous cells: mucous cell (sc); Golgi complex (gc); Intercellular space (is); Secretion granule (sg); Lumen (l); Nucleus (n); RER (re). 10000x.
Seromucous acinus /mixed acinus demilume
Salivary Glands Acinus Duct Intercalated duct: Simple squamous/cuboidal epith. Striated/secretory ducts: simple tall columnar epith. Interlobular duct: pseudostratified columnar epith. Excretory ducts: stratified squamous epith.
Salivary Glands Intercalated duct: Simple squamous or cuboidal epith.
Salivary Glands Intercalated duct:simple squamous or cuboidal epith.
Detail of intercalated duct cell Basal laminar (bl); Desmosome (d); Nerve fibers (nf); Golgi complex (g); Intercellular space (is); Mitochondria (m); Nucleus (nu); RER (re). 13.000x
Salivary Glands Striated/secretory duct: simple tall columnar epith.
Salivary Glands Striated /secretory duct
Salivary Glands Striated/secretory duct The secretory ducts, which are continuous with intercalated ducts, are wider and lined with a simple columnar epithelium. As the secretion from the acini passed through the secretory ducts, the epithlium can re-absorb sodium (Na+) and water from the lumen to the interstitium and transport potassium (K+) into the saliva, thus changing the consistency of the saliva. The secretory ducts drain into interlobar ducts which run between lobules.
Salivary Glands Interlobular duct: excretory duct: Pseudostratified columnar epith. Stratified squamous epith.
Salivary glands Include ﹡Parotid G. ﹡Submandibular G. ﹡Sublingual G. Function: ﹡Moistening food. ﹡Carbohydrate digestion. ﹡Secrete IgA.
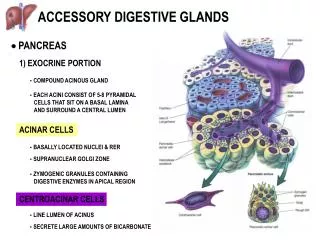
Pancreas The pancreas is a lobular organ. The pancreas has both exocrine functions (releases digestive enzyme secretions into the intestines) and endocrine functions (releases hormones into the blood).
Pancreas Parenchyma exocrine gland endocrine gland produces produces pancreatic juice hormones
Pancreas Exocrine pancreas Acini Ducts Intercalated ducts Interlobular ducts Main pancreatic ducts Major duodenal papilla Wholly consists of serous acini. Small centroacinar cells in the lumen
Exocrine Pancreas It releases the pancreatic juice. Pancreatic juice contain many kinds of enzyme: ﹡amylase: hydrolyses starch & glycogen. ﹡lipase: hydrolyzes triglycerides into fatty acids and mono-glycerides ﹡cholesterol esterase: breaks down ﹡trypsin and chymotrypsin: hydrolyze proteins. ﹡ribonuclease & deoxyribonuclease: split nucleic acids.
Pancreas Endocrine pancreas ﹡Islets of Langerhans Scatter throughout the exocrine pancreas. ﹡Three types of cells: A-cells (20%) glucagon (glycogen→ glucose) B-cells(75%)insulin D-cells (5%)somatostatin ﹡Capillaries:each islet is richly supplied with blood vessels.
Pancreas Endocrine pancreas
Glucagon Purpose: Assist insulin in regulating blood glucose (sugar) in the normal rangeAction: Forces many cells of the body to release (or produce) glucose (increasing blood sugar)Secreted in response to: Low blood glucoseSecretion inhibited by: High blood glucoseDisease due to deficient action: Some times nothing, sometimes hypoglycemiaDisease due to excess action: HyperglycemiaTumor called: Glucagonoma Insulin Purpose: Regulate blood glucose (sugar) in the normal range Action: Forces many cells of the body to absorb and use glucose thereby decreasing blood sugar levelsSecreted in response to: High blood glucoseSecretion inhibited by: Low blood glucoseDisease due to deficient action: Diabetes Disease due to excess action: HypoglycemiaTumor called: Insulinoma.
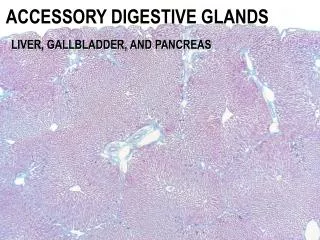
Liver General Introduction ﹡The largest gland(--2% of body weight in adult). ﹡respectively receives both venous & arterial blood through the portal v. (--75%) & hepatic A (--25%). ﹡CT of capsule extended into the parenchyma, forming “classical” liver lobules. ﹡Functions as an exocrine gland (secreting bile) and other very important roles.
Liver Structrues of Liver lobule
Liver Structures of Liver lobule
Liver Structures of Liver lobule ﹡six-sided prism with a central V. at its center. ﹡sheets of hepatocytes (or hepatic plates) extend radially from the central V. ﹡sinusoids between hepatic plates. Portal triads (or portal area): In the corner of lobules.
Liver Structures of Liver lobule
Liver Portal Triads (or Portal Area) ﹡Definition: The area of CT found in the angles where adjacent hepatic lobules meet. ﹡Components: CT.+portal triad interlobular A interlobular V interlobular bile duct
Liver Portal Triads (or Portal Area)
Liver Portal Triads (or Portal Area)
Liver Sinusoids ﹡Dilated anastomosing venules between the hepatic plates. ﹡Blood pathway: periphery→central V. ﹡Kupffer cells line in the wall of sinusoids. ﹡EM (endothelium of sinusoid) significant gaps; numerous fenestration; incomplete basal lamina.
Liver Sinusoids
Sinusoids TEM