The Adrenal Cortex
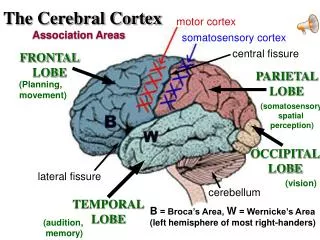
The Adrenal Cortex. Basic principles of steroid endocrinology. Steroid effects fall into 3 categories: Mineralocorticoid Glucocorticoid Androgen/Estrogen Small differences in steroid molecules have large effects on activity

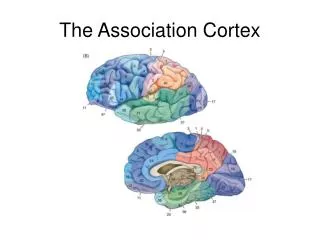
The Adrenal Cortex
E N D
Presentation Transcript
Basic principles of steroid endocrinology • Steroid effects fall into 3 categories: • Mineralocorticoid • Glucocorticoid • Androgen/Estrogen • Small differences in steroid molecules have large effects on activity • Steroids act through nuclear receptors, so their major effects involve changes in the expression of particular genes
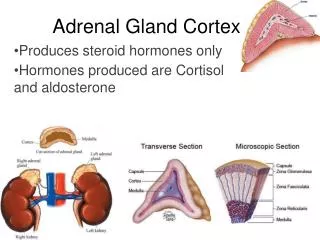
Major Corticosteroid Hormones • Aldosterone – mineralocorticoid • Cortisol (human); corticosterone (some mammals) – glucocorticoid • Adrenal androgens: dehydroepiandrosterone (DHEA), androstenedione, androstenediol,
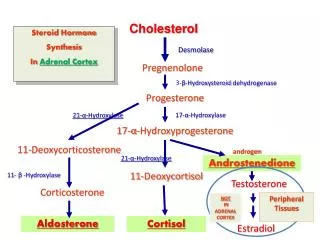
Pathways of adrenal steroid biosynthesis Important points: multiple reactions are catalyzed by the same enzymes – however, in different regions of the cortex, different parts of the map are favored. This reaction occurs in the periphery, not in the adrenal itself
Enzyme mutations are responsible for a number of clinical syndromes: for example – 21 alpha hydroxylase deficiency • Leads to inadequate production of both mineralocorticoid and glucocorticoid, but excessive production of adrenal androgen • Symptoms: salt-losing diuresis, increased susceptibility to infection, premature masculinizing puberty • Adrenal hypertrophy occurs as a result of the lack of feedback from cortisol – so ACTH levels are elevated. • Appropriate therapy: replacement cortisol
Control of ACTH secretion • The hypothalamus releases CRH in regular pulses, about every 20 min. • Circadian rhythm: greatest secretion (increased pulse amplitude) occurs in the early morning before awakening • Stress or hypoglycemia strongly stimulate pulse amplitude. • ADH also stimulates ACTH secretion.
What is stress, anyway? • Emotional • Situational • Surgical • Forced exercise • Confinement/handling (animals) • Pain • Ultimately, physiologists have decided to define stress as any stimulus that elevates ACTH secretion.
Hyper and hypoadrenal syndromes • Cushing’s Syndrome: excessive corticosteroid – hypertension, hyperglycemia, hypokalemia, alkalosis, characteristic pattern of fat loss from lower body and fat deposition around neck and face. This syndrome is very commonly iatrogenic. • Addison’s Syndrome: hypotension, poor survival in fasting, increased susceptibility to infection, hyperkalemia, acidosis, potential for ‘Addisonian crisis’. • Causes may be at level of hypothalamus, pituitary or adrenal itself – diagnosis involves measurement of ACTH levels
Post-translational processing of POMC in pituitary corticotrophs ‘POMC’ is proopiomelanocortin. The primary gene product can be clipped at different places to produce a variety of hormones. During adult life, the major corticotroph products are ACTH and beta-lipotropin. During fetal life and in pregnant women, the pars intermedia of the pituitary processes the gene product differently, yielding gamma lipotropin, beta endorphin, and two versions of melanocyte stimulating hormone.
Addison’s Syndrome - hypoadrenalism • Hypoglycemia • Hypotension • Poor resistance to infection • Fatigue, muscle weakness • Susceptibility to Addisonian crises • Hyperpigmentation – in primary hypoadrenalism
Primary versus secondary disease • In primary hypoadrenalism, the adrenal cortex is the site of the lesion and ACTH levels are elevated, giving hyperpigmentation. • In secondary hypoadrenalism, the pituitary or brain is the site of the lesion, and ACTH levels are low.
Symptoms of Hyperadrenalism • Obesity – including characteristic fat deposit on back of neck • Skin changes • Symptoms of androgen excess • Muscle and bone loss • Menstrual irregularity • Hypertension • Glucose intolerance