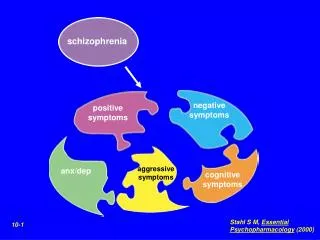
Schizophrenia
Schizophrenia. The Unwell Brain. Disturbance in the Neurochemistry. The first discovery in the mid 1950s was that chronic usage of large daily doses of Amphetamines could produce a psychosis that was virtually indistinguishable from schizophrenia.

Schizophrenia
E N D
Presentation Transcript
Schizophrenia The Unwell Brain
Disturbance in the Neurochemistry The first discovery in the mid 1950s was that chronic usage of large daily doses of Amphetamines could produce a psychosis that was virtually indistinguishable from schizophrenia. The second discovery was that Chlorpromazine could improve symptoms for schizophrenia. The effects of Amphetamines and Chlorpromazine on the neurochemistry of the brain were unknown.
Further Discoveries It was found that Amphetamine could enhance neurotransmission of Dopamine, Norepinephrine and (to a lesser extent) Serotonin Synapses. It was also discovered that Chlorpromazine could prevent Dopamine from activating it’s D2 receptor subtype. The knowledge that Chlorpromazine improves symptoms of schizophrenia while blocking D2 receptors for Dopamine has led to the development of drugs that have similar pharmacological properties to chlorpromazine.
Neuroleptics & Atypicals The Neuroleptics (older generation) are identified in two categories: Phenothiazines & Butyrophenones. Chlorpromazine (Thorazine) is the original phenothiazine anti-schizophrenic drug. Haloperidol (Haldol) is the most familiar and widely used butyrophenone. What do these drugs have in common and what are their effectiveness with treating schizophrenic symptoms?
Positive symptoms The symptoms that are the most responsive to these types of drugs came to be called the ‘positive symptoms’ because they showed a positive response to neuroleptic drug therapy. These positive symptoms included: delusions, hallucinations, disorganised speech and bizarre behaviour. The negative symptoms included: flattened emotional response, impoverished speech, diminished initiative and motivation, social withdrawal, lack of feeling pleasure (anhedonia) and intellectual impairment.
D2 receptors Phenothiazines & Butyrophenones also share the ability to bind to D2 dopamine receptors and act as antagonists, thereby preventing endogenous (proceeding from within) dopamine from activating those receptors. Different phenothiazines & butyrophenones drugs bind to D2 receptors to varying degrees, and also alter neurochemical processes other than dopamine. There is a correlation between the potency of the drug and the ability to improve symptoms of schizophrenia in a clinical setting.
“Problem Schizophrenics” Newer generation antipsychotics (Atypicals) can be effective in these normally unresponsive schizophrenics. They also lack some of the debilitating side effects of the older neuroleptics. These newer generation antipsychotics appear to block multiple subtypes of dopamine receptors (including D1 D2 D3 D4 D5); they are also reported to alter serotonin neurotransmission and to effect several other neurotransmitters, including, acetylcholine, norepinephrine, and histamine.
Clozapine (Clozaril) Clozapine is effective in some schizophrenics whose symptoms do not improve on haloperidol. A patient maintained on clozapine is less likely to show side effects related to involuntary movements (tardive dyskinesia). It tends not to block the receptors for dopamine in the striatum (could explain it’s lack of motor side effects). Haloperidol tends to block D2 receptors in the caudate and putamen areas of the brain whereas clozapine blocks D1, D2, D3, D4 and D5 receptors as well as multiple subtypes of serotonin receptors.
Brain processes & Schizophrenia Neuroimaging studies show that excessive D2 receptors have been found in the striatum and frontal cortex. Dopamine D1 receptors are deficient in number in the prefrontal cortex of schizophrenics. This deficiency is correlated with some of the negative symptoms of schizophrenia.
Dopamine Neurons Dopamine neuron cell bodies originate in the Ventral Tegmental Area (VTA) and SubstantiaNigra (SN). D2 abnormality appears to be localised in mesolimbic and mesocortical dopamine neurons, which connect the prefrontal cortex with subcorticol areas, including the striatum, caudate, putmen and hippocampus. The prefrontal cortical and limbic (hippocampus) link may represent the key vulnerability for development of schizophrenia, which has long been considered to be a disorder of cognitive (cortical) and emotional (limbic) interactions.
Clinical Effectiveness Older generation neuroleptics that block D2 receptors in the caudate/putamen regions is presumed to have secondary effects on the basal ganglia, thalamus, hippocampus, and cortex. The newer generation Atypicals, Risperidone (Risperdal) can cause greater effects upon dopamine neurotransmission in the frontal cortex and the striatum. It’s ability to improve both positive and negative symptoms may be due to it’s simultaneous alteration of dopamine neurotransmission and blockade of serotonin 5HT-2A receptors in the cortex.