Digestive System
Digestive System. Human Anatomy Chapter 22.

Digestive System
E N D
Presentation Transcript
Digestive System Human Anatomy Chapter 22
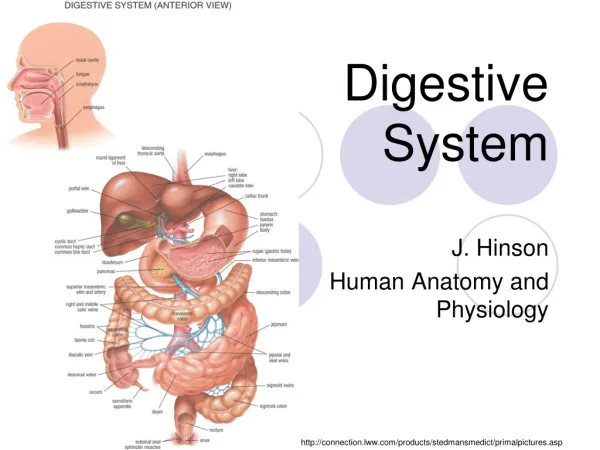
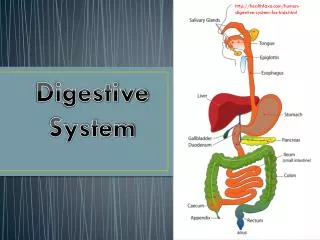
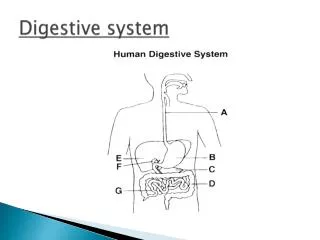
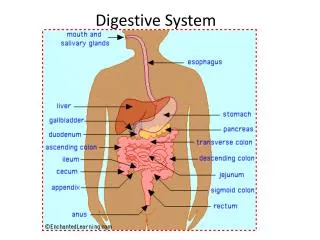
Organs of the digestive system are either part of the gastrointestinal tract (alimentary canal) or accessory digestive organs. The GI tract includes the mouth, esophagus, stomach and intestines, it is considered to be part of the outside of the body because the mouth and anus both open to the outer environment. The accessory organs include the teeth, tongue, salivary glands, pancreas, and liver. These organs assist in the digestion of food.
A. Digestive Processes- there are six food processing activities: 1. Ingestion- brining food into the mouth (eating) 2. Propulsion- moving food through the GI tract, peristalsis (contractions of smooth muscle in GI tract) helps to move the food along. 3. Mechanical digestion- physical change of the food particles from large to small, this helps to increase the surface area to make chemical digestion more effective. Actions include chewing, churning of food in stomach, and mixing food with digestive juices. 4. Chemical digestion- chemical change of the food particles, bonds are broken to change a large molecule into a smaller one so absorption can happen more effectively. This involves the use of enzymes, hydrochloric acid, and other digestive juices. 5. Absorption- transport of digested food molecules from the GI into the blood and lymphatic vessels 6. Defecation- elimination of feces (indigestible substance/digestive waste)
Peristalsis Segmentation
B. Abdominal Regions and Quadrants- Review the regions and quadrants as presented in Chapter 1. Digestive organs are located in the abdominal cavity. Be familiar with the approximate location of the intestinal organs within the nine regions regions and four quadrants as shown. )
II. Anatomy of the digestive System- This section focuses on the gross anatomical and microscopic anatomical characteristics of the digestive organs. A. The peritoneal cavity and peritoneum- The peritoneum is an extensive serous membrane in the abdominal cavity, the visceral peritoneum covers the surfaces of digestive organs. A cavity is found in between the visceral and parietal peritoneum. The parietal peritoneum lines the wall of the abdominal cavity. The peritoneal cavity is a slit like space filled with serous fluid. A double layer of serous membranes that hold digestive organs in place is called the mesentery. Organs surrounded by mesentery and suspended in the cavity are called intraperitoneal or peritoneal organs. Some are not surrounded by mesentery; they are called retroperitoneal
B. Histology of the alimentary Canal Wall- the following are the layers found in all organs of the gastrointestinal tract. The thickness of each layers varies with location or organ. 1. The Mucosa- inner most layer, closest to the lumen, it is called a mucous membrane and has three layers- 1) lining epithelium that secretes mucus and absorbs nutrients, it contains intrinsic glands; 2) a lamina propia that has loose connective tissue rich in capillaries and lymphoid tissue; 3)a muscularis mucosa made up of smooth muscle. 2. The submucosa- contains connective tissue that helps to reshape the organs once food passes by, major blood and lymphatic vessels, and some gland tissue 3. The muscularis Externa- two layers of smooth muscle: the circular and longitudinal layers that help to contract the tube so food passes by (peristalsis) 4. The serosa-outermost layer, actually the visceral peritoneum, organs that don't have a serosa have a layer of fibrous connective tissue called the adventitia, such as the esophagus. Some organs have both a serosa and adventitia. 5. Nerve plexuses- the GI tract and accessory organs are innervated by the autonomic nervous system (sympathetic and parasympathetic). There are two plexuses: the myenteric nerve plexuses that innervates the smooth muscle in tunica muscularis externa and controls contraction. The submucosa nerve plexus innervates the submucosa and controls glandular secretion.
C. The mouth and associated Organs- the mouth is primarily used for mechanical digestion. 1. Mouth- also known as the oral cavity, its opening is the oral orifice, and it is the site of ingestion. The lips are also known as vestibule and the oral cavity proper is the space inside the mouth (internal to teeth). a. Mouth tissue- the mouth is lined by stratified squamous epithelium and this is also called a mucous membrane. The mouth also has layers called internal mucosa, submucosa, and external layer of muscle and bone instead or a serosa. The tongue, lips, gums, and palate are lined with cells that are slightly keratinized for extra protection. b. Cheeks- made up primarily by the buccinator muscle, they help to keep food within oral cavity. c. Lips- muscular flaps that have a translucent area called the red region. This is the area that can become dried or chapped because there are no lubricating glands. The labial frenulum connects the lips to the gums.
2. Tongue- composed of skeletal muscle, it repositions food during chewing and shapes it into a bolus. The tongue contains taste buds and also helps to shape sounds when one is speaking. The tongue is attached to the floor of the mouth by the lingual frenulum. The tongue also contains lingual tonsils.
3. Salivary glands- compound tubular glands that produce a liquid containing water, mucus, proteins, a buffer, and enzymes. The purpose of saliva is to moisten, begin the digestion of starch, neutralize acids, stimulate growth of beneficial bacteria in the mouth and dissolve food chemicals so we can taste them (stimulate the chemoreceptors of the mouth). a. Salivary glands include the parotid, submandibular, and sublingual.
4. Teeth- The first set of teeth humans develop is the deciduous (20 milk teeth) and then the permanent teeth (32 teeth). Teeth are pecialized structures found within sockets of the gum called alveoli and are held in place by the periodontal ligament. They form an immoveable joint. Teeth are composed of three layers called enamel (hardest substance in the body), dentin (bone like tissue that is harder than bone), and the pulp cavity (hollow centered filled with blood vessels and nerves). The teeth can also be divided into three sections, the crown, the neck, and the root. Every tooth has its own blood and nervous supply (pulp).
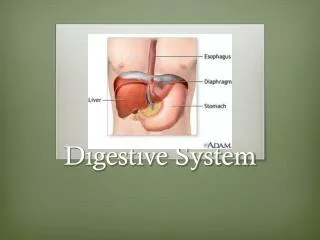
D. Pharynx- once food leaves the mouth it passes into the pharynx (the cavity behind the mouth) and moves from the oropharynx into the laryngopharynx. There it is routed to enter the esophagus by contractions of the pharyngeal constrictor muscles. Swallowing is avoluntary actions that is controlled by skeletal muscle. E. Esophagus- long muscular tube that moves food through peristalsis. The lumen is typically collapsed. 1. Gross anatomy- It extends from the laryngopharyx, through the thorax, exits via the esophageal hiatus, and meets the stomach at the cardiac orifice. The cardiac sphincter controls the entering and exiting of substances into/ out of the stomach. 2. Microscopic anatomy- It has non-keratinized stratified epithelium, the mucosa and submucosa form folds when esophagus is empty (pg 623). Tthe submucosa contains glands that lubricate the food as it passes by. The upper part of the esophagus contains skeletal muscle and the rest contains smooth muscle. The esophagus contains an adventitia layer not a serosa layer.
C.S. of Esophagus Junction at stomach (L.S.)
F. Stomach- A pouch with sphincter muscles at both ends: superiorly is the cardiac sphincter and inferiorly is the pyloric sphincter. They contract to contain the food within the stomach while it is liquefied, mixed with stomach acid (hydrochloric acid) and turned into chyme. This is the site where proteins are first digested by pepsin enzymes. Substances absorbed through the stomach are: water, electrolytes and some drugs. Food is process in the stomach for about 4 hours. 1. Gross anatomy- It is inferior to the diaphragm and anterior to spleen and pancreas, The stomach is generally J shaped and has the following features: cardiac sphincter, cardiac region, fundus, body, pyloric antrum, pyloric canal, and pyloric sphincter. The curves of the stomach are described as the greater and lesser curvature. Internally large folds called rugae are visible. These folds allow the stomach to expand so it can hold up to 4L of food at one time. It has three layers of smooth muscle: longitudinal layer, circular layer, and oblique layer.
2. Microscopic anatomy- the lining is composed of simple columnar epithelial cells and many goblet cells that secrete bicarbonate buffered mucus. The mucus protects the stomach lining. Gastric pits are also visible, these open into gastric glands. There are some enteroendocrine cells that release hormones related to digestion and undifferentiated stem cells that divide to replace the damaged lining a. Mucous neck cells- secret a mucus different of that secreted by goblet cells. b. Parietal (oxyntic) cells- produce the hydrochloric acic c. Chief (zymogenic) cells- secrete enzyme called pepsinogen that becomes pepsin when activated by the hydrochloric acid.
G. Small intestine- this is the longest section, an area where chemical digestion is completed and most nutrients are absorbed. Food remains here for about 3-6 hours. The small intestine can be divided into three section: duodenum, ilelium, jejunum. It uses peristalsis to move chyme along and for segmentation movements. 1. Gross anatomy- the tube runs from the pyloric sphincter of the stomach to the beginning of the large intestine. The first division is the duodenum (5%) short area where the digestive chemicals from the pancreas and gall bladder are received. The second division is the jejunum (40%) a longer region where food is digested and nutrients are absorbed. The last section is the ileum (60%) it connects to the large intestine.
2. Microscopic anatomy- the small intestine is designed for absorption of nutrients, thus its modifications increase its surface area by 200 square feet. • Circular folds- transverse ridges (1 cm tall) that force the chyme to spiral as it slows it down to increase absorption. • b. Villi- these are finger-like projections (1mm tall) made up of simple columnar epithelial cells specialized for absorption (enterocytes). They are in close contact with capillaries and lacteal (lymph vessels that absorb fat) • c. Microvilli- microscopic folds on the apical side of the simple columnar epithelial cell in the mucosa. The folds increase the surface area of the cell's membrane allowing for greater interaction. This is also the area where chemical digestion is completed. • Intestinal crypts contain cells that produce digestive juice in the small intestine and stem cell replace the epithelium every 3-6 days. Duodenal glands also secrete a solution that neutralizes stomach acid.
H. Large intestine- Area where food remains for 12-24 hours. Some absorption and digestion occurs (by bacteria) it is primarily designed to reabsorb water and electrolytes. 1. Gross anatomy- It is wider than the small intestine but shorter. It is divided into the cecum (opening of ileum to large intestine, has iliocecal valve), the vermiform appendix (opens to the cecum, contains lymphoid tissue), the colon (has at least four sections), the rectum (has rectal valves that prevent feces from being passed along with gas) and the anal canal (external to abdominal pelvic cavity, has external anal canal). The sections of the colon and bends are: ascending colon, right colic (hepatic) flexure, transverse colon, left colic (splenic) flexure, descending colon, and sigmoid colon and rectum. Some of the feature are: the teniae coli (longitudincal strips that run along the colon), the haustra (pockets or sacs) and the epiploic appendages (hanging fat filled pouches)
2. Microscopic anatomy- has no villi or microvilli, has intestinal crypts with goblet cells that provide mucus to lubricate the feces. Stem cells are present to fully replace the epithelium every week. Has more lymphoid tissue than other GI tract organs. At the anal canal the epithelium changes to stratified squamous and eventually merges with true skin surrounding the anus.
Rectum and anal canal Defication Reflex
I. Liver- considered the largest gland, it performs over 500 functions that influence several systems beside the digestive system. In regards to the digestive system it produces bile. A substance that emulsifies fat and makes it accessible to fat digesting enzymes. The liver is involved in balancing blood glucose levels, it responds to hormones, and clears toxins or drugs from the blood and makes blood proteins. 1. Gross anatomy- It is protected by the rib cage. It has a diaphragmatic surface and a visceral surface, the bare area is fused to the diaphragm. It has four lobes: right and left lobes that are divided by the falciform ligament, the caudate lobe, and the quadrate lobe. The posterior and inferior view also shows the round ligament (ligamentum teres) and the ligamentun venosum. The port heptis is also on this side. Major blood vessels, nerves, and ducts enter through the porta hepatis. Bile is carried from the liver by the right and left hepatic ducts that merge into the common hepatic duct that also connects to the cystic duct of the gall bladder. Bile reaches the small intestine through the common hepatic duct.
2. Microscopic anatomy- liver tissue shows multiple hexagonal sections called liver lobules. Each lobule contains a central vein, hepatocytes arranged into “plates”, and is surrounded by connective tissue. At the corners there are portal triads containing a hepatic vein, artery, and bile duct. Liver cells are called hepatocytes and aside from the many functions they perform they have the ability to regenerate the liver.
2. Microscopic anatomy- liver tissue shows multiple hexagonal sections called liver lobules. Each lobule contains a central vein, hepatocytes arranged into “plates”, and is surrounded by connective tissue. At the corners there are portal triads containing a hepatic vein, artery, and bile duct. Liver cells are called hepatocytes and aside from the many functions they perform they have the ability to regenerate the liver.
J. Gall bladder- muscular sac that stores bile, it is attached to the cystic duct and when the muscle contract bile exits through this duct and into the common hepatic duct. K. Pancreas- a gland that is both exocrine (has a duct) and endocrine (releases hormones into the blood stream). It produces 22 different enzymes for digestion by acinar cells and buffers to neutralized stomach acid by epithelial cells. It joins gall bladder secretions and both enter the duodenum via the hepatopancreatic ampulla at the major duodenal papilla.
L. Mesenteries- double layer sheets of serosa membranes that hold organs in place by connecting them to the dorsal and ventral abdominal walls. Sometimes they are referred to as ligaments. Ventral Mesenteries- 1) falciform ligament- connects liver to anterior wall 2) lesser omentum- runs from the liver to the lesser curvature Dorsal Mesenteries- 1) Greater omentum- from the greater curvature to the posterior wall, however it also connect to the intestines. It also holds a lot of fat 2) Mesentery proper- support and hold the jejunum and ileum. 3) Transverse mesocolon- attaches the transverse colon, it fuses with the greater omentum. 4) Sigmoid mesocolon- connects sigmoid colon to posterior pelvic wall.