TOPIC 8 Digestive System
Biology 221 Anatomy & Physiology II. TOPIC 8 Digestive System. Chapter 18 pp. 651-677. E. Lathrop-Davis / E. Gorski / S. Kabrhel. Digestive System Functions. Provide nutrients in usable form Remove unusable wastes. Digestive System Overview . Two main groups of organs:

TOPIC 8 Digestive System
E N D
Presentation Transcript
Biology 221 Anatomy & Physiology II TOPIC 8Digestive System Chapter 18 pp. 651-677 E. Lathrop-Davis / E. Gorski / S. Kabrhel
Digestive System Functions • Provide nutrients in usable form • Remove unusable wastes
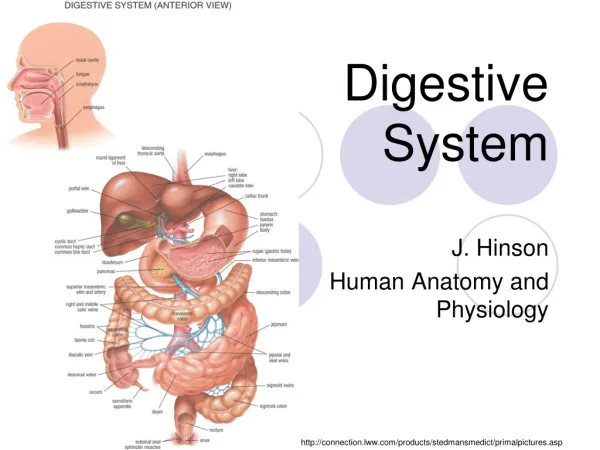
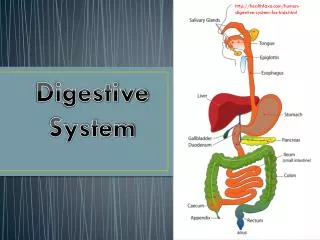
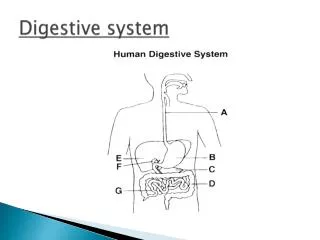
Digestive System Overview Two main groups of organs: • Alimentary canal (a.k.a. Gastrointestinal tract) • tube through which food passes • responsible for digestion and absorption of food • mouth, pharynx, esophagus, stomach, small intestines, large intestines • Accessory organs • organs, glands and structures which aid digestion but not part of GI tract itself • teeth, tongue, salivary glands, pancreas, liver, gall bladder Fig. 24.1, p. 888
Processes of Digestion • Ingestion – entrance of food and drink into mouth • Mechanical digestion – physical breakdown into smaller pieces • Propulsion – movement through gut • Chemical digestion – breakage of molecules into smaller compounds • Absorption – uptake of nutrients from lumen • Defecation – removal of indigestible material Fig. 24.2, p. 889
Peritoneum • Serous membrane • parietal peritoneum – lines abdominal cavity • organs posterior to the parietal peritoneum are retroperitoneal • visceral peritoneum (serosa)– covers surfaces of most abdominal organs • Mesenteries – double layer of peritoneum extending from body wall to digestive organs • intraperitoneal organs are those in mesentaries • Peritoneal cavity – fluid-filled “space” between visceral and parietal peritoneum • Peritonitis – inflammation of the peritoneum See also Fig. 24.5, p. 891 Fig,. 24.30, p. 929
Splanchnic Circulation Arteries serving the digestive organs: • Celiac Trunk – very short; gives rise to: • hepatic artery – liver; gall bladder; stomach; duodenum • left gastric artery – stomach; inferior esophagus • splenic artery – spleen; stomach; pancreas • Superior Mesenteric Artery – small intestines; most of large intestine; pancreas • Inferior Mesenteric Artery – large intestine Fig. 20.22, p. 761 Fig. 20.22, p. 759
Hepatic Circulation: Hepatic portal system • Veins draining digestive organs and carrying nutrient-rich blood to liver • gastric vein– drains stomach • superior mesenteric vein– drains small intestine • splenic vein– drains spleen • inferior mesenteric vein – drains large intestine • Venous blood from hepatic portal system mixes with arterial blood (hepatic artery) in liver Fig. 20.27, p. 771
Hepatic Circulation: Hepatic Veins • drain venous blood from liver into inferior vena cava Fig. 20.27, p. 771
Mucosa • Mucous membrane lining gut • Consists of: • epithelium – lining • lamina propria – areolar connective tissue layer • muscularis mucosae – smooth muscle http://www.usc.edu/hsc/dental/ghisto/gi/d_1.html
Mucosa: Epithelium • Type varies depending on location • stratified squamous epithelium found in mouth, esophagus and anal canal • simple columnar epithelium found in stomach and intestines • Secretes mucus, digestive enzymes, hormones • Provides intact barrier to protect against entry of bacteria http://www.usc.edu/hsc/dental/ghisto/gi/c_2.html http://www.usc.edu/hsc/dental/ghisto/gi/d_15.html
Mucosa: Lamina Propria • Layer of areolar connective tissue • Blood capillaries nourish epithelium, absorb and transport digested nutrients • Lymphatic capillaries provide drainage for interstitial fluid and transport fats to venous circulation http://www.usc.edu/hsc/dental/ghisto/gi/d_60.html
Mucosa: Muscularis Mucosae • Smooth muscle used for local movement and to hold mucosa in folds (small intestine) http://education.vetmed.vt.edu/Curriculum/VM8054/Labs/Lab19/EXAMPLES/Exileum.htm
Submucosa • Dense connective tissue superficial to mucosa • Highly vascularized • Many lymphatic vessels • Lymph nodules • MALT = mucosa-associated lymphatic tissue • especially in small (Peyer’s Patches) and large intestines http://education.vetmed.vt.edu/Curriculum/VM8054/Labs/Lab19/EXAMPLES/Exileum.htm
Muscularis Externa (Muscularis) • Two layers in most organs (3 in stomach) • circular layer • longitudinal layer • Peristalsis moves material through gut • Segmentation helps mix material with digestive enzymes in small intestine Fig. 24.3, p. 890
Serosa • Visceral peritoneum – simple squamous epithelium (mesothelium) with areolar CT • Adventitia – dense connective tissue covering without epithelium; found around esophagus • Retroperitoneal organs have both a serosa (of parietal peritoneum) and adventitia (on side abutting body wall)
Enteric Nervous System Intrinsic nerve plexuses: • Enteric neurons • neurons able to act independently of central nervous system • communicate with each other to control GI activity • Two main enteric plexuses: • submucosal nerve plexus – regulates glands in submucosa and smooth muscle of muscularis mucosae • myenteric nerve plexus – regulates activity of muscularis externa (with aide of submucosal nerve plexus)
Central Nervous System Control • Enteric nerve plexuses linked to CNS by visceral afferent (sensory) fibers • Digestive system receives motor input from sympathetic and parasympathetic divisions of autonomic nervous system • parasympathetic outflow generally increases activity • sympathetic outflow generally decreases activity
Mouth (Oral Cavity) • Oral oriface is anterior opening • Mouth is continuous with oropharynx • Lips and cheeks keep food in oral cavity • Three layers of tissue: • mucosa (stratified squamous epithelium) • submucosa • muscularis externa (skeletal muscle)
Mouth: Palate • Hard palate • palatine process of maxilla • palatine bones • Soft palate • muscle only • prevents food from entering nasopharynx during swallowing • uvula (part that hangs down in middle) Fig. 24.7, p. 895
Mouth: Arches • Palatoglossal arch – anchors soft palate to tongue • Palatopharyngeal arch anchors soft palate to wall of oropharynx • Fauces – area between arches • palatine tonsils – located in fauces Fig. 24.7, p. 895
Mouth: Tongue • Lingual tonsil – sits at base of tongue; protects against invasion by bacteria • Taste buds • contain receptors for taste • found in some papillae Fig. 24.8, p. 896
Mouth: Tongue • Tongue forms bolus • ball of food • makes food easier to swallow • keeps food between teeth • Muscles – served by nerve XII • intrinsic muscles – within tongue (not attached to bone); allow tongue to change shape for swallowing and speech • extrinsic muscles – attach to bone or soft palate; alter tongue position (protrusion, retraction, side-to-side) Fig. 24.7, p. 895
Salivary Glands • Produce saliva • Two groups of salivary glands • intrinsic glands (buccal glands) – within oral cavity • extrinsic glands – 3 pairs (see A&P I Unit VI for innervation) • parotid glands (connected to oral cavity by parotid duct; mumps is a viral infection of the parotid glands) • sublingual glands • submandibular glands Fig. 24.9, p. 897
Saliva • Mucus cells produce mucus (less common) • Watery saliva produced by serous cells; composition: • 97-99.5% water • slightly acidic (pH ~ 6.8) • electrolytes (ions such as Na+, K+, Cl-, PO4=, HCO3-) • metabolic wastes (urea, uric acid) • proteins
Salivary Proteins • Mucin – glycoprotein portion of mucus that lubricates oral cavity) • Lysozyme – antibacterial • IgA– antibodies that prevent antigens from attaching to mucus membrane • Defensins – secreted by neutrophils; act as local antibiotic and chemotatic agent when mucosa is damaged • Salivary amylase – hydrolyzes starch
Control of Salivation • Sympathetic division • stimulates production of mucin-rich saliva, or • inhibits salivation altogether at high levels
Control of Salivation • Parasympathetic division of ANS stimulates activity • chemoreceptors (excited most by acidic substances) and baroreceptors (excited by mechanical stimuli) send messages to salivatory nuclei in pons and medulla • parasympathetic motor output results in salivation • psychological control – response to visual, olfactory stimuli, even thoughts of food • salivary nuclei are stimulated by irritation to lower GI tract • Parasympathetic nerves • facial – to submandibular, sublingual • glossopharyngeal – to parotids
Teeth • Lie in alveoli of mandible and maxilla (see A&P I axial skeleton lab) • Primary dentition = deciduous teeth (20 milk or baby teeth) • roots are absorbed as permanent teeth grow in, causes baby teeth to fall out Fig. 24.10, p. 899
Teeth Permanent dentition = adult teeth (32) • 8 Incisors (central and lateral) • 4 Canines (eyeteeth) • 8 Bicuspids = premolars • Molars • 4 first molars • 4 second molars • 4 third molars • wisdom teeth • may become impacted as grow in Fig. 24.10, p. 899
Tooth Structure • Crown - covered by enamel (hardest substance in body); underlain with dentin • Neck • Root • cementum – calcified connective tissue covering dentin of root; attaches root to periodontal ligament which anchors tooth to alveolus • no enamel (dentin is under cementum) • pulp cavity – houses blood vessels and nerves that enter/leave via apical foramen in the root canal Fig. 24.11, p. 900
Pharynx • Only oropharynx and laryngopharynx are involved in digestion (nasopharynx is only respiratory) • Lined with nonkeratinized stratified squamous epithelium • Mucus-producing glands in submucosa produce mucus that lubricates food • Skeletal muscle responds to somatic reflexes to move food quickly past laryngopharynx • No serosa or adventitia
Esophagus • Runs from laryngopharynx through mediastinum to stomach • All 4 layers present in wall • Mucosa – consists of stratified squamous epithelium • Submucosa – mucus-secreting esophageal glands http://www.usc.edu/hsc/dental/ghisto/gi/c_2.html
Esophagus • Muscularis – changes type as goes down • top 1/3 – skeletal muscle • middle 1/3 – mix • bottom 1/3 – smooth muscle • Adventitia – dense connective tissue covering http://www.usc.edu/hsc/dental/ghisto/gi/d_8.html http://www.usc.edu/hsc/dental/ghisto/gi/d_3.html
Structures Associated with the Esophagus • Upper esophageal sphincter – controls movement of material from pharynx into esophagus • Esophageal hiatus – opening in diaphragm that allows esophagus to pass from thoracic cavity into abdominal cavity • Gastroesophageal (cardiac) sphincter • thickening of smooth muscle of inferior esophagus • aided by diaphragm to close bottom of esophagus • helps prevent reflux of acidic gastric juice
Esophageal Disorders • heartburn – failure of lower esophageal sphincter to close completely allowing acidic gastric juice into esophagus • hiatus hernia – protrusion of the superior portion of stomach above diaphragm • esophageal ulcer – erosion of wall due to chronic reflux of stomach acid
Digestive Processes in Mouth, Pharynx and Esophagus • Ingestion • Mechanical Digestion • mastication by teeth (with aid of tongue) • formation of bolus • Chemical digestion by salivary amylase produced by salivary glands • breaks starch and glycogen into smaller fragments (including maltose [disaccharide] if left long enough) • continues activity until reaches acid stomach • Absorption– essentially none (except some drugs, e.g., nitroglycerine)
Digestive Processes in Mouth, Pharynx and Esophagus • Movement – deglutition (swallowing) • moves food from oral cavity to stomach • voluntary in oral cavity (buccal phase) • reflexive in pharynx • involuntary peristalsis where smooth muscle is found Fig. 24.13, p.904
Stomach: Gross Anatomy • Cardiac region (cardia) • Fundus - temporary storage area • Body • greater curvature • lesser curvature • Pyloric region– distal portion • Pyloric sphincter– controls movement of chyme into small intestine http://medlib.med.utah.edu/WebPath/GIHTML/GI194.html Fig. 24.14, p. 905 http://medlib.med.utah.edu/WebPath/GIHTML/GI194.html
Stomach Histology • Mucosa • simple columnar epithelium • muscularis mucosae throws mucosa into folds called rugae • Submucosa– connective tissue • Muscularis – 3 layers create mixing waves in addition to peristalsis • longitudinal layer • circular layer • oblique layer • Serosa - covers stomach http://www.gutfeelings.com/STOMACH.HTML Fig. 24.14, p. 905
Microscopic Anatomy • Surface composed mainly of goblet cells (secrete mucus) • Gastric pits • tight junctions between epithelial cells prevent acidic gastric juice from reaching underlying layers • contain gastric glands which secrete gastric juice • mucus neck cells • parietal (oxyntic) cells • chief (zymogenic) cells • enteroendocrine cells Fig. 24.15, p. 906 http://www.usc.edu/hsc/dental/ghisto/gi/d_15.html
Gastric Pit Cells • Mucous neck cells secrete bicarbonate-rich mucus • Parietal (oxyntic) cells secrete: • HCl (buffered by bicarbonate rich mucus) • intrinsic factor (essential to absorption of Vit. B12 by small intestine) • Chief (zymogenic) cells secrete: • pepsinogen (inactive form of the protease pepsin for protein hydrolysis) • minor amounts of lipases (lipid hydrolysis)
Gastric Pit Cells • Enteroendocrine cells – release hormones and hormone-like products into the lamina propria where they are picked up by blood and carried to other digestive organs • gastrin – generally stimulatory • histamine – stimulates H+ secretion • somatostatin – generally inhibitory
Digestive Processes in Stomach • Mechanical digestion • mixing waves help break food into smaller particles • Chemical digestion – produces chyme (pH ~ 2) • acid (HCl) secreted by parietal cells breaks some bonds and activates pepsinogen into pepsin • pepsin – • produced as pepsinogen by chief cells • hydrolyses proteins • rennin – protease secreted in children that acts on milk proteins
Digestive Processes in Stomach • Movement • mixing waves mix food with acid and enzymes • peristalsis moves material through stomach and into small intestine • Absorption – limited to lipid soluble substances • alcohol • aspirin • some other drugs
Regulation of Gastric Secretion Controlled by nervous system and hormones • Hormonal control • gastrin stimulates secretion • somatostatin, gastric inhibitory protein (GIP), and cholecystokinin inhibit secretion • Neural control: • autonomic control (CNS) • parasympathetic division • Vagus (X) nerve • sympathetic division - thoracic spinal nerves • local enteric nerve reflexes • distension of stomach stimulates activity • distension of duodenum inhibits activity See Fig. 24.16, p. 910
Stimulation of Gastric Secretion • Cephalic Phase (cerebral) • Gastric Phase (stomach) • Intestinal Phase (duodenum) Fig. 24.16, p. 910
Inhibition of Gastric Secretion • Cephalic Phase (cerebral) • Gastric Phase (stomach) • Intestinal Phase (duodenum) Fig. 24.16, p. 910
Gastric Disorders • Gastritis –inflammation of underlying layers of wall • Gastric ulcers –erosions of stomach wall • Helicobacter infections associated with ~90% of all ulcers (uncertain as to whether it is causitive agent) • non-infectious ulcers associated with persistent inflammation
Gastric Disorders (con’t) • Emesis = vomiting • usually caused by • extreme stretching of stomach or small intestine, or • presence of irritants in stomach (e.g., bacterial toxins, excessive alcohol, spicy foods, certain drugs) • emetic center in medulla initiates impulses to • contract abdominal muscles (increases intra-abdominal pressure) • relax cardiac sphincter • raise soft palate (closes off nasal passages) • excessive vomiting results in dehydration and metabolic alkalosis (increased blood pH)
Small Intestine: Gross Structure • Diameter ~ 2.5 cm • Length ~ 2-4 m (8-13’) (in cadaver, 6-7 m [20-21’] because muscle is not contracted) • Small intestine designed for secretion (especially proximal end) and absorption • site of most chemical digestion • site of most absorption • pH 7-8 • Three areas: • duodenum (25 cm) • jejunum • ileum Fig. 24.21, p. 916