Chronic obstructive pulmonary disease (COPD)
621 likes | 2.06k Views
Chronic obstructive pulmonary disease (COPD). What is COPD?. COPD is the fourth most common cause of death in the USA . Progressive Disease (Worsens Over time) Incurable Smoking is the leading Cause

Chronic obstructive pulmonary disease (COPD)
E N D
Presentation Transcript
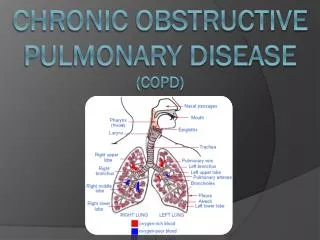
What is COPD? • COPD is the fourth most common cause of death in the USA. • Progressive Disease (Worsens Over time) • Incurable • Smoking is the leading Cause • Long-term exposure to other lung irritants—such as air pollution, chemical fumes, or dust may contribute to COPD • Coughing, large mucus production, wheezing, chest tightness, shortness of breath, and other symptoms. (NHLBI/NIH,2013)
History of COPD • COPD has been known to mankind for over 200 years. • The CIBA Guest Symposium in 1959 and the American Thoracic Society Committee on Diagnostic Standards in 1962 were the first to describe the definition of COPD. • It was in 1846 that John Hutchinson invented the spirometer. This was the key to diagnosing COPD. The spirometer is still used today for diagnosis and regular assessment regarding response to therapy in COPD • Laënnec described emphysema of the lungs in 1821 in his Treatise of diseases of the chest. He was the inventor of the stethoscope. • Baillie in 1789 published a series of illustrations of the emphysematous lung putting forth the pathology of the disease. Emphysema was known to be a part of COPD early on. It was much later that chronic bronchitis got included in COPD (Mandal)
History of COPD Continued… • Earlier the only therapies for COPD were antibiotics for pneumonia, a mucus thinner called potassium iodide and bronchodilators like ephedrine, theophylline etc. There were in addition sedatives to deal with the side effects of ephedrine. • It was in 1960’s that isoproterenol – a selective beta 2 agonist was used. Corticosteroids were almost never used and oxygen was not advised at the time. • Oxygen therapy and pulmonary rehabilitation also developed over the last half of the 20th century. (Mandal)
Who Can Get COPD? • People that smoke or have smoked. • Workers who are regularly exposed to chemicals or dust while at work • People with asthma who smoke. • People that are 35 to forty years old begin to show symptoms. COPD is a slowly progressing disease. • An uncommon genetic disorder known as alpha-1-antitrypsin deficiency is the source of some cases of COPD. (Mayo Clinic,2014)
People Who Have COPD • Chronic lower respiratory disease, primarily COPD, was the third leading cause of death in the United States in 2011. • Fifteen million Americans report that they have been diagnosed with COPD. • More than 50% of adults with low pulmonary function were not aware that they had COPD. • People aged 65–74 years. • Non-Hispanic whites. • Women. • Individuals who were unemployed, retired, or unable to work. • Individuals with less than a high school education. • People with lower incomes. • Individuals who were divorced, widowed, or separated. • Current or former smokers. • Those with a history of asthma. (CDC,2013)
Testing for COPD • CT scan-A CT scan of your lungs can help detect emphysema and help determine if you might benefit from surgery for COPD. • Pulmonary function tests-Spirometry is the most common lung function test.Spirometry can detect COPD even before you have symptoms of the disease. It can also be used to track the progression of disease and to monitor how well treatment is working. (Mayo Clinic,2014) (Mayo Clinic,2014) • Arterial blood gas analysis-This blood test measures how well your lungs are bringing oxygen into your blood and removing carbon dioxide. • Chest X-ray-Achest X-ray can show emphysema, one of the main causes of COPD. An X-ray can also rule out other lung problems or heart failure. (Mayo Clinic,2014) (Mayo Clinic,2014)
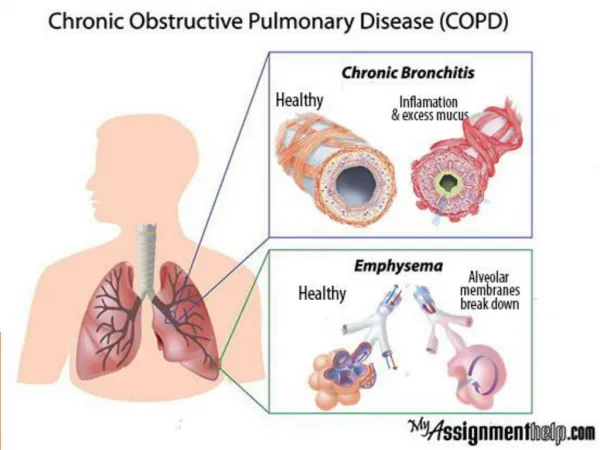
COPD: Emphysema • Emphysema occurs when the air sacs in your lungs are gradually destroyed. • Turns the spherical air sacs, clustered like bunches of grapes, into large, irregular pockets with gaping holes in their inner walls. This reduces the surface area of the lungs and, in turn, the amount of oxygen that reaches your bloodstream. • Slowly destroys the elastic fibers that hold open the small airways leading to the air sacs. This allows these airways to collapse when you breathe out, so the air in your lungs can't escape. (Mayo Clinic, 2014)
COPD: Chronic Bronchitis • Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to your lungs. • The inflamed bronchi produce a lot of mucus. This leads to cough and difficulty getting air in and out of the lungs. (MedlinePlus)
Symptoms • Constant coughing, sometimes called "smoker's cough" • Shortness of breath while doing everyday activities • Producing a lot of sputum (also called phlegm or mucus) • Feeling like you can't breathe or take a deep breath • Wheezing (American Lung Association, 2013)
Treatment of COPD • Bronchodilators -- can be administered as pills, liquids, or inhalers. They open up the air passages in the lungs. • Antibiotics -- COPD reduces the effectiveness of the lungs' natural defense systems. Antibiotics can get rid of bacterial infection in the lungs when they are in this compromised state. • Fluid clearing device -- The Flutter device is a small, drug-free unit designed to help patients easily cough out the extra fluid in their lungs. • Oxygen -- for severe cases of COPD, supplemental oxygen, using a tank and face mask, may be necessary. (Penn Medicine, 2007)
Treatment of COPD • Pulmonary rehabilitation -- a pulmonary rehabilitation program is provided by a team of health professionals to help COPD patients cope physically, psychologically, and socially with the disease. The program strives to help patients achieve the highest possible quality of life within the limitations of the disease. • Lung transplantation • Lung volume reduction surgery (LVRS) • Bullectomy • Pneumococcal Vaccine • Flu Shots (Penn Medicine, 2007) (NHLBI/NIH,2013)
Gender Differences • This is the tenth consecutive year in which women have exceeded men in the number of deaths attributable to COPD. In 2009, more than 70,000 females died compared to almost 64,000 males. • Women are about twice as likely to be diagnosed with chronic bronchitis as men. In 2011, 3.3 million men (29.6 per 1,000 population) had a diagnosis of chronic bronchitis compared to 6.8 million women (56.7 per 1,000 population). • Historically, men have been more likely than women to receive a diagnosis of emphysema. However, in 2011 more women reported a diagnosis of emphysema than men; 2.6 million (21.4 per 1,000 population) compared to 2.1 million (19.0 per 1,000 population), respectively. (American Lung Association,2013)
Prevalence and Incidence • In 2011, 12.7 million U.S. adults (aged 18 and over) were estimated to have COPD.However, close to 24 million U.S. adults have evidence of impaired lung function, indicating an under diagnosis of COPD. • In 2011, an estimated 10.1 million Americans reported a physician diagnosis of chronic bronchitis. Chronic bronchitis affects people of all ages, although people aged 65 years or more have the highest rate at 64.2 per 1,000 persons. • Of the estimated 4.7 million Americans ever diagnosed with emphysema, 92 percent are 45 or older. • In 2011, COPD prevalence ranged from less than 4 percent in Washington and Minnesota to more than 9 percent in Alabama and Kentucky. (American Lung Association,2013)
Prevalence and Incidence (CDC,2013)
Prevalence and Incidence (CDC,2013)
Prevalence and Incidence (CDC,2013)
Etiology • Tobacco smoking is by far the main risk factor for COPD. It is responsible for 90% of COPD cases and exerts its effect by causing an inflammatory response, cilia dysfunction, and oxidative injury. Air pollution and occupational exposure are other common etiologies. Oxidative stress and an imbalance in proteinases and antiproteinases are also important factors in the pathogenesis of COPD, especially in patients with alpha-1 antitrypsin deficiency, who have panacinar emphysema that usually presents at an early age. (Epocrates)
Pathophysiology • COPD is chronic inflammation that affects central airways, peripheral airways, lung parenchyma and alveoli, and pulmonary vasculature. • The main components of these changes are narrowing and remodeling of airways, increased number of goblet cells, enlargement of mucus-secreting glands of the central airways, and, finally, subsequent vascular bed changes leading to pulmonary hypertension. • The host response to inhaled stimuli generates the inflammatory reaction responsible for the changes in the airways, alveoli, and pulmonary blood vessels. Activated macrophages, neutrophils, and leukocytes are the core cells in this process. • In emphysema, which is a subtype of COPD, the final outcome of the inflammatory responses is elastin breakdown and subsequent loss of alveolar integrity. • In chronic bronchitis, another phenotype of COPD, these inflammatory changes lead to ciliary dysfunction and increased goblet cell size and number, which leads to the excessive mucus secretion. These changes are responsible for decreased airflow, hyper secretion, and chronic cough. • Increased airway resistance is the physiologic definition of COPD. (Epocrates)
National Intervention • Smoking Cessation Programs • CDC Anti-smoking Ads • Truth anti-smoking Ads • Anti-smoking laws • Increased Warning Labels • Increased Health Education about smoking, air pollutants, and chemical in the workplace.
Measures for Prevention • Avoid smoking tobacco or exposure to secondhand tobacco smoke. • Decrease exposure to environmental irritants. • Use appropriate protective gear (e.g. face mask) in the workplace to avoid inhaling hazardous substance. • Get plenty of physical activity for good lung health. • If you already have COPD, avoid colds, pneumonias, and flus, which can worsen the disease. Get pneumococcal and annual flu vaccinations to avoid such infections. (Penn Medicine, 2007)
Measures for control • Reduce risk factors (smoking, air pollutants, chemical exposure) • Prevent disease progression • Prevent and treat complications • Prevent and treat exacerbations • Relieve symptoms • Improve exercise tolerance • Improve health status • Reduce mortality (WHO,2014)
References • What Is COPD?. (2013, July 31). NHLBI, NIH. Retrieved April 1, 2014, from https://www.nhlbi.nih.gov/health/health-topics/topics/copd/# • Mandal, A. (n.d.). History of Chronic Obstructive Pulmonary Disease. News Medical. Retrieved April 1, 2014, from http://www.news-medical.net/health/History-of-Chronic-Obstructive-Pulmonary-Disease.aspxhttp://www.news-medical.net/health/History-of-Chronic-Obstructive-Pulmonary-Disease.aspx • Mayo Clinic. (2014).COPD. Retrieved March 31, 2014, from http://www.mayoclinic.org/diseases-conditions/copd/basics/risk-factors/con-20032017 • American Lung Association. (2013, August 1). Chronic Obstructive Pulmonary Disease (COPD) Fact Sheet - American Lung Association. Retrieved April 1, 2014, from http://www.lung.org/lung-disease/copd/resources/facts-figures/COPD-Fact-Sheet.html#Prevalence
References • Centers for Disease Control and Prevention. (2013, April 9). COPD Data and Statistics . Retrieved April 1, 2014, from http://www.cdc.gov/copd/data.htm • Mayo Clinic. (2014). Emphysema. Retrieved April 1, 2014, from http://www.mayoclinic.org/diseases-conditions/emphysema/basics/treatment/con-20014218 • U.S. National Library of Medicine. (n.d.).Chronic Bronchitis: MedlinePlus. Retrieved March 30, 2014, from http://www.nlm.nih.gov/medlineplus/chronic • Epocrates . (n.d.). COPD . Retrieved March 31, 2014, from https://online.epocrates.com/u/29247/COP • Pennmedicine. (2007, May 16). Chronic Obstructive Pulmonary Disease (COPD) . Retrieved April 1, 2014, from http://www.pennmedicine.org/health_info/a • Centers for Disease Control and Prevention. (2013, November 13). COPD. Retrieved April 1, 2014, from http://www.cdc.gov/copd/index.htm#learn • WHO. (2014).COPD management. Retrieved April 1, 2014, from http://www.who.int/respiratory/copd/mana