Tooth Eruption
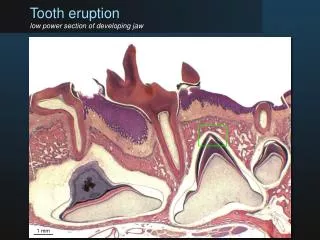
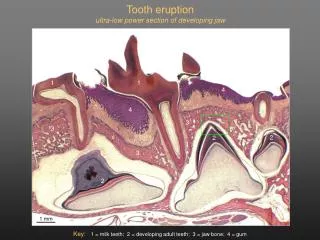
Tooth Eruption. Tooth eruption is the process by which a tooth moves from its site of development within the jaws to its final functional position in the oral cavity. it is a continuous process. Phases of tooth eruption. Pre-eruptive phase Pre-functional eruptive phase

Tooth Eruption
E N D
Presentation Transcript
Tooth Eruption • Tooth eruption is the process by which a tooth moves from its site of development within the jaws to its final functional position in the oral cavity. • it is a continuous process
Phases of tooth eruption • Pre-eruptive phase • Pre-functional eruptive phase • Functional eruptive phase
Pre-eruptive phase • All movements of primary and permanent tooth germs (crowns) from time of their early initiation and formation to the time of crown completion • ends with early initiation of root formation
Pre-Eruptive Phase • Early in the stage, the permanent anterior teeth begin developing lingual to the incisal level of the primary teeth. Later, as the primary teeth erupt, the secondary teeth are positioned lingual to the apical third of their roots. • Permanent premolars shift from a location near the occlusal area of the primary molars to a location enclosed within the roots of the primary molars
Permanent molars have no predecessors • Maxillary molars develop within the maxillary tuberosity with their occlusal surfaces slanted distally • Mandibular molars develop in the ramus with the occlusal surfaces slanting mesially
Pre-Functional Eruptive • Starts with the initiation of root formation and ends when the teeth reach occlusal contact • Four major events occur during this phase: • Root formation • Movement occurs incisally or occlusally through the bony crept to reach the oral mucosa • Penetration of the tooth crown tip into the oral cavity • Intraoral movement occlusally and incisally until clinical contact with the opposing crown occurs.
The rate of tooth eruption depends on the phase of movement • Intraosseous phase: 1 to 10 μm/day • Extraosseous phase (soft tissue): 75 μm/day
Functional Eruptive Phase • Takes place after the teeth are functioning and continues as long as the teeth are present in the mouth
Post eruptive tooth movement • 1. Movements to accommodate the growing jaws. • Mostly occurs between 14 and 18 years by formation of new bone at the alveolar crest and base of socket to keep pace with increasing height of jaws.
2. Movements to compensate for continued occlusal wear. • Compensation primarily occurs by continuous deposition of cementum around the apex of the tooth.
3. Movements to accommodate interproximal wear. • Compensated by mesial or approximal drift. • Mesial drift is the lateral bodily movement of teeth on both sides of the mouth. • Very important in orthodontics.
Environmental factors affecting the final position of the tooth: • Muscular forces • Thumb-sucking
Tongue thrust Palatal crib
Mechanisms of Eruptive Tooth Movement • Root formation • Bone remodeling • Dental follicle • Periodontal ligament • Role of hydrostatic pressure
Root formation • Should be an obvious cause of tooth eruption. But studies have not provided evidence for this. • If a tooth that is continuously erupting is prevented the root still forms by causing bone resorption.
Rootless tooth still erupt, some teeth erupt more than the total length of the roots and the teeth still erupt after completion of root formation. Therefore root formation is accommodated during eruption and may not be the cause of tooth eruption. Root formation produces a force which causes bone resorption by osteoclast.
Root growth theory suggested the presence of the cushion hammock ligament at the base of the socket that transmits the force to cause eruption but the ligament was never found histologically One point of importance is that, the tissue beneath the growing root resists the apical movement of the developing root. This resistance results in the occlusal movement of the tooth crown as the root lengthens
Bone Remodeling • An inherent growth pattern of the maxilla and mandible supposedly moves teeth by selective deposition and resorption of bone • not sure if bone remodeling plays a significant role but is involved
Dental follicle • Investigators indicate a pattern of cellular activity involving the reduced enamel epithelium (REE) and the follicles associated with tooth eruption. • Studies have shown that the reduced dental epithelium initiates a cascade of intercellular signals that recruit osteoclasts to the follicle.
By providing a signal and chemo-attractant for osteoclasts, it is possible that the dental follicle can initiate bone remodeling which goes with tooth eruption. • RDE also secretes proteases, which assist in breakdown of connective tissue to produce a path of least resistance.
Periodontal ligament • Periodontal Ligament Traction theory Formation and renewal of the PDL has been considered a factor in tooth eruption because of the traction power of the fibroblasts. • Most accepted theory Due to contraction of the FB situated in the PDL, a pressure is created which favors eruption
Hydrostatic Pressure • A number of studies exist to demonstrate that there is a hydrostatic pressure difference between the tissue around the erupting crown and its apical extent • The hydrostatic theory was investigated by Hassel and McMinn (1972) who demonstrated that the tissue pressure apically was greater than occlusally theoretically generating an eruptive force. • No association was found between the rate of eruption and the pressure gradient.
Shedding of Primary Teeth • Shedding is the loss of the primary dentition caused by the physiologic resorption of the roots, the loss of the bony supporting structure and therefore the inability of these teeth to withstand the masticatory forces. • Resorption of anterior teeth occurs on the lingual surface and these teeth are shed with their pulp chamber intact • Resorption of primary molars occurs in interradicular dentine with some resorption of the pulp chamber, coronal dentine and sometimes enamel
Resorption of dental hard tissues is achieved by cells with a histological nature similar to that of osteoclasts called Odontoclasts Pressure plays an important role in the exfoliation of primary teeth Stem cells ????
Hormonal Control Mechanisms • Eruption occurs only during a critical period between 8pm and midnight or 1am. • During the morning, tooth eruption ceases or even the tooth intrudes a bit. • This reflects Circadian Rhythm reflecting the possible involvement and control of growth hormone and thyroid hormone.
The time of eruption for primary and permanent teeth varies greatly. • A variation of 6 months on either side of the usual eruption date may be considered normal for a given child. • Girls eruption of their permanent teeth are 5 months earlier than the boys
Tooth eruption has three stages • Deciduous dentition • Mixed dentition • Permanent dentition
Primary dentition • starts on the arrival of the mandibular central incisors, typically from around six months, • lasts until the first permanent molars appear in the mouth, usually at six years. • The primary teeth typically erupt in the following order: (1) central incisor, (2) lateral incisor, (3) first molar, (4) canine, and (5) second molar
Mixed dentition • starts when the first permanent molar appears in the mouth, usually at five or six years, • lasts until the last primary tooth is lost, usually at ten, eleven, or twelve years.
Sequence of eruption • The sequence of calcification is not a sure clue to the sequence of emergence in the mouth • Wide variability • Max ( 6-1-2-4-3-5-7/ 6-1-2-4-5-3-7 ) • Mand ( 6-1-2-3-4-5-7/6-1-2-4-3-5-7 ) • Most common sequence Max ( 6-1-2-4-5-3-7 ) & Mand ( 6-1-2-3-4-5-7)
The permanent dentition • begins when the last primary tooth is lost, usually at 11 to 12 years, • and lasts for the rest of a person's life or until all of the teeth are lost
Infant occlusion • Upper anterior gum pad is wider than lower • Over jet= 5mm • Overbite= 0.5 mm
Normal features of the primary dentition • Spaced anterior • Primate spaces • Shallow overbite and overjet1-2mm • Mesial step plane molar relationship • Almost vertical inclination of the ant teeth
Primary dentition occlusion • Types of molar relationship • 1- Flush terminal plane: distal surface of opposing E are at the same level 37% of primary molar relationship 75% of them result in ideal class I permanent molar relationship 25% will shift to class II
2- mesial step: • Distal surface of lower E mesial to distal of upper • 49% of primary of molar relationship (most common) • mesial step will result in ideal class I molar relationship
3- Distal step : • Distal surface of lower E distal to distal of upper • 14% of primary molar relationship • Result in class II molar relationship
Permanent dentition occlusion Molar classification : • Class I mesiobuccal cusp of upper 1st molar in buccal groove of lower 1st molar55% • Class II mesiobuccal cusp of upper 1st molar mesial to opposing one 19% • Class III mesiobuccal cusp of upper 1st molar distal to opposing one • End-on relation ship : mesiobuccal cusp of both molars at the same level 25%