TOOTH MOVEMENT AND ERUPTION
TOOTH MOVEMENT AND ERUPTION. Tooth eruption. eruption takes place in chronological order involves active eruption – vertical movement of the tooth as opposed to passive eruption – receding of the gingiva how it occurs is not understood

TOOTH MOVEMENT AND ERUPTION
E N D
Presentation Transcript
Tooth eruption • eruption takes place in chronological order • involves active eruption – vertical movement of the tooth • as opposed to passive eruption – receding of the gingiva • how it occurs is not understood • root growth, hormonal action, contractile collagen, vascular pressure?? • no requirement for the root • three distinct phases to the development of the dentition • 1. pre-eruptive – initiation of tooth development • 2. tooth eruption – prefunctional phase • begins as the roots begin to form • 3. development and maintenance of occlusion – functional phase • after the teeth have emerged into the oral cavity
Tooth eruption • defined as the axial movement of tooth from its developmental position in the alveolar socket into its functional position within the oral cavity • no evidence to suggest that eruption entirely ceases once the tooth meets ints antagonist • outward axial movements experienced during the functional phase may also be a type of eruptive movement • also seen after tooth extraction • eruptive forces also experience in adolescents – “growth spurts” • preeruptive forces and those generated during the prefunctional and functional stages may be different mechanisms – not proven • accompanying eruptive forces are resistive forces which prevent eruption – soft tissues and alveolar bone, PDL and occlusal forces
Directions and rates of tooth eruption • main direction is axial (i.e. long axis of the tooth) • also movement in other planes – resulting in tilting and drifting • eruption rates are greatest during times of crown emergence • rates will differ based on tooth type – balance between eruptive forces and resistive forces • permanent maxillary incisors – 1mm/month • mandibular second molars – 4.5 mm in 14 weeks • permanent third molars – 1 mm in 3 months • eruption rates can slow to 1 mm/6 months in crowded dentitions
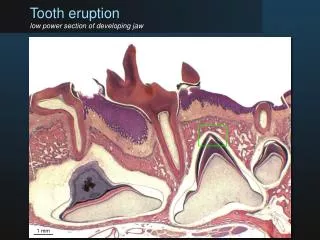
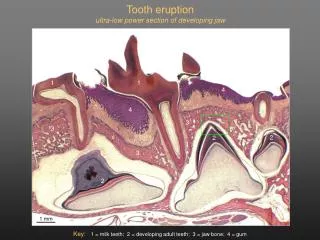
Primary tooth eruption • several stages • after apposition of the enamel into the crown area of the tooth stops, the ABs create an acellular dental cuticle on the new enamel’s surface • cuticle – protection of emerging enamel • two thin layers • degraded with mastication • as the tooth erupts it is still covered with a layer of amelobasts and the remaining layers of the enamel organ • these layers become compressed as the tooth moves – forming a reduced enamel epithelium (REE) or reduced dental epithelium • the REE is required for eruption • the REE fuses with the oral epithelium lining the oral cavity (see figure 6-28) • the REE produces enzymes which disintegrates the central portion of this fused tissue – results in an epithelial tunnel through which the tooth erupts • collagenases and acid hydrolases • this disintegration results in an inflammatory response – interpreted as the teething response
-as the tooth erupts, the portion of the epithelium covering the crown pulls back and exposes the crown -the cervical portion of the epithelium is still attached to the neck of the tooth (figure 6-28) -this fused tissue serves as the initial junctional epithelium (thin dotted line) and creates a seal between the tooth and the surrounding tissue -i.e. as the tooth pierces the oral epithelium, the cells of the reduced dental epithelium and the oral epithelium form the initial junctional epithelium (thin dotted line) -the REE portion of this junctional epithelium becomes replaced by oral epithelium -later replaced by the definitive dentogingival junction
Permanent tooth eruption • as the succedaneous permanent teeth develop below the primary teeth, the primary tooth is exfoliated • eruption is lingual to the roots of the primary teeth • exception is the maxillary incisors which move to a more facial position as they erupt • loss of primary teeth should occur first • involves the differentiation of osteoclasts which absorb the alveolar bone between the primary and permanent teeth • development of odontoclasts which resorb portions of the primary tooth’s root dentin and cementum • eruption process is the same for the primary teeth – formation of an epithelium lined tunnel for eruption • the process is also similar for the nonsuccedaneous teeth except no primary tooth is shed
Mechanisms of tooth eruption: current research • not well understood • bone deposition at the base of the underlying root may initiate eruption and move the tooth axially • role for growth factors • initiation of eruption – role for EGF and TGF alpha • also can be induced by macrophage colony-stimulating factor (MCSF) • production of TGF beta1, interleukin 1a by the stellate reticulum enhances the production of monocyte chemotactic protein/MCP1 and colony stimulating factor/CSF1 by dental follicle • CSF1 induces the dental follicle to make MCSF • MCSF and MCP induce the recruitment of monocytes into the dental follicle • monocytes transform into osteoclasts – resorb the overlying alveolar bone