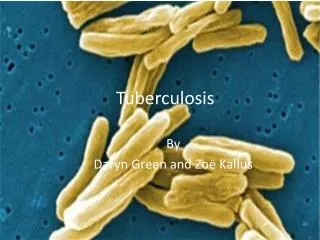
Tuberculosis
Tuberculosis. By Fion Kung. Objective. Describe tuberculosis Describe sigh and symptoms of tuberculosis Describe the nursing diagnosis for tuberculosis Describe the nursing intervention for tuberculosis Describe the treatment for tuberculosis. What is Tuberculosis?.

Tuberculosis
E N D
Presentation Transcript
Tuberculosis By Fion Kung
Objective • Describe tuberculosis • Describe sigh and symptoms of tuberculosis • Describe the nursing diagnosis for tuberculosis • Describe the nursing intervention for tuberculosis • Describe the treatment for tuberculosis
What is Tuberculosis? • Tuberculosis (TB) is caused by a bacterium called Mycobacterium tuberculosis. The bacteria usually attack the lungs, but TB bacteria can attack any part of the body such as the kidney, spine, and brain. If not treated properly, TB disease can be fatal. • TB is spread through the air from one person to another. When an infected individual coughs, laughs, sneezes, or sings, droplet nuclei containing tuberculosis bacteria enter the air and may be inhaled by others. • TB is not spread by shaking someone’s hand, sharing food or drink, kissing
Two Tuberculosis related conditions • Latent TB Infection: TB bacteria can live in the body without making you sick. In most people who breathe in TB bacteria and become infected, the body is able to fight the bacteria to stop them from growing. People with latent TB infection do not feel sick and do not have any symptoms. People with latent TB infection are not infectious and cannot spread TB bacteria to others. However, if TB bacteria become active in the body and multiply, the person will go from having latent TB infection to being sick with TB disease. • TB Disease: When TB bacteria are active (multiplying in your body). People with TB disease are sick. They may also be able to spread the bacteria to people they spend time with every day. • Many people who have latent TB infection never develop TB disease. Some people develop TB disease soon after becoming infected (within weeks) before their immune system can fight the TB bacteria. Other people may get sick years later when their immune system becomes weak for another reason.
Signs & Symptoms • People who have latent TB infection do not have any symptoms. • People who are TB active will have the following symptoms: • A bad cough for three weeks or longer • pain in the chest • weakness or fatigue • Unintentionally weight loss 10-15 lbs over 3 months • no appetite • chills • Low grade fever • sweating at night
Epidemiology • According to the Centers for Disease Control and Prevention • One third of the world’s population are infected with TB. • In 2011, nearly 9 million people around the world became sick with TB disease. There were around 1.4 million TB-related deaths worldwide. • TB is a leading killer of people who are HIV infected. • According to
Diagnostic Studies • 2 step testing initially for health care workers • TST or Mantoux ,PPD ( purified protein derivative) ; good for latent TB; measure induration • CXR if previous positive PPD(cannot make sole dx with CXR) • Cultures AFB may take 6-8 weeks (3 consecutive sputum) • QuantiFERON-TB rapid serum analysis • Chest x-ray can confirm TB • Acid fast bacteria- collect spudum ASP • TB test- postitive test means have been exposed doesn’t mean it’s active, needs to be treated with INH in addtion to antibiotivicstoxic to liver don’t drink alcohol and and have LFT’s every month and no tyenoel antibiotics therapy) needs chest x-ray • Active TB- I lost weight low grade fever, night sweat, need chest x-ray isolate from others, you are hospitalized,
Common Diagnosis tests • The tuberculin skin test was the only test available to detect latent tuberculosis until an interferon-release assay, called QuantiFERON-TB test
TREATMENT • Active • INH, ethambutol, rifampin, pynazinamide (PZA) Latent-(INH) alone • Tx time 6 to 9 months • Liver Function Tests No ETOH • Vaccine • BCG • Positive PPD
Nursing Considerations • Respiratory Isolation • HEPA masks • UV can damage mycobacterium • Hand washing • Droplet precautions • Adherence to tx
Risk Factors for Tuberculosis • Homeless individuals • Lower socioeconomic group, minority group, or refugee group • Individuals living in crowded areas such as long term care • Has HIV infection • Has been recently infected with TB bacteria (in the last 2 years) • Has other health problems, like diabetes, that make it hard for the body to fight bacteria • Abuses alcohol or uses illegal drugs • Individuals did not treated correctly for TB infection in the past
Put on TB respiratory precaution, masks, they can infect people
Medication • Latent TB infection: • isoniazid (INH) • rifampin (RIF) • rifapentine (RPT) • Active TB: • isoniazid (INH) • rifampin (RIF) • ethambutol (EMB) • pyrazinamide (PZA)
NCLEX Question 1 • A client with pulmonary tuberculosis (TB) asks the nurse how this disease was contracted. The nurse replies that TB is commonly spread by which of the following methods?1. Sneezing2. Shaking hands3. Contact with stool4. Contact with urine
NCLEX Question 2 • A client with tuberculosis asks the nurse how long he will have to take medication. The nurse should tell the client that: • Medication is rarely needed after 2 weeks. • He will need to take medication the rest of his life. • The course of therapy is usually 18–24 months. • He will be re-evaluated in 1 month to see if further medication is needed.
A male client is asking the nurse a question regarding the Mantoux test for tuberculosis. The nurse should base her response on the fact that the: 1. Presence of a wheal at the injection site in 2 days indicates active tuberculosis. 2. Area of redness is measured in 3 days and determines whether tuberculosis is present. 3. Skin test doesn’t differentiate between active and dormant tuberculosis infection. 4. Test stimulates a reddened response in some clients and requires a second test in 3 months.
References • http://ccn.aacnjournals.org/content/29/2/34.full • http://www.cdc.gov/tb/topic/basics/personalstories.htm • http://ccn.aacnjournals.org/content/29/2/34/F4.expansion.html