Asthma Refresher
Asthma Refresher. Jeremy and Anthony. Statistics. 10% of the population has asthma 30 % of elderly people (>65) have undiagnosed asthma 40% of survey respondents believed that their asthma was not well controlled 1

Asthma Refresher
E N D
Presentation Transcript
Asthma Refresher Jeremy and Anthony
Statistics • 10% of the population has asthma • 30% of elderly people (>65) have undiagnosed asthma • 40% of survey respondents believed that their asthma was not well controlled1 • Only 40% of adults and 63% of parents/ carers said they had a written action plan • Barriers to asthma management: • 25% said cost of medication • 15% said cost of seeing a GP/ specialist • 31% of parents of children with asthma said difficulty getting an appointment with a GP/ specialist
Statistics (cont.) • Asthma is the second most common cause of hospitalisation of Indigenous Australians.2 • Higher prevalence of asthma among Indigenous Australians (16.5%) compared to Non-Indigenous Australians (10.2%). • Indigenous Australians are twice as likely to be hospitalised for asthma and three times as likely to die of asthma as other Australians.
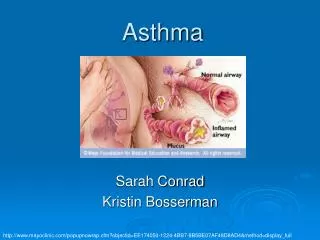
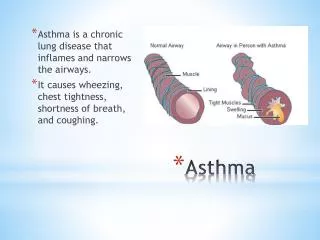
What is asthma? • Sensitive airways disease which, when triggered, makes it difficult for a person to breathe. • Three components • Inflammation – swelling of airway lining • Excess mucus production – airway blockage • Muscles contract around the airways – bronchoconstriction • If untreated, asthma can result in permanent airway damage
Symptoms • Persistent cough • Shortness of breath • Chest tightness • Wheezing • Additionally, children may complain of sore chest or tummy • Symptomstend to occur at night, in the early morning and following activity
Triggers • Differs between individuals • Set off symptoms or worsen them • If multiple triggers are worsening a patient’s asthma, it could be an indication that their preventer medication is insufficient • E.g. • Cold or flu • Smoke • Exercise • Inhaled allergens • Dust and other forms of pollution • Changes in temperature/ weather • Some medications • Stress
Diagnosing Asthma3 • History • Examination • Spirometry • Only useful for children 6+
Management • According to asthma management guidelines, the goal of treatment is “good asthma control”. This entails: • Symptoms less than twice a week • Use of reliever less than three times a week • No interference with activity or exercise due to asthma • No disturbance to sleep
Management (cont.) • Avoidance of triggers • E.g. quit smoking • Medications • Regular reviews by a doctor (guidelines suggest 6 monthly reviews)
Types of Medications • Relievers - Blue • Preventers - Orange • Symptom controllers - Green • Combination - Purple
Relievers • Relaxes the muscles around the airways • Act quickly • Use: • When symptomatic • Asthma first aid • Before exercise • Side effects: • Shakes • Tachycardia • Ask a doctor for an asthma review if using more than three times a week • E.g. Airomir, Asmol, Ventolin
Preventers • Reduces swelling and mucus production • Work within one day of use • Should be taken daily as prescribed • Side effects • Oral thrush • Voice change • Sore throat and mouth • Headaches • Stomach ache • E.g. Flixotide, Pulmicort, Singulair
Devices • Puffers • Spacers • Accuhalers • Turbuhalers • Autohalers
Devices • Things to consider when choosing an asthma treatment device: • Age • Breath intake • Coordination • Hand strength • Whether or not a spacer would be beneficial • Up to 90% of people use their devices incorrectly
Devices (cont.) • Spacers: • Spacers are easier to use than puffers alone • More medication reaches the lungs • Less side effects due to better delivery • Nebulisers: • Sometimes recommended by doctors if using a puffer and spacer is difficult. • However a puffer and spacer, when used correctly, is as effective as a nebuliser.
Using a spacer • Put the spacer together. • Remove the cap from the puffer. • Shake the puffer well and insert into the end of the spacer. • Place the mask over the nose and mouth and ensure there is a good seal. On older children, the mouthpiece might be better than the mask. • Breathe out gently. • Press the puffer once to release into the spacer. Do not remove the puffer. • Breathe in and out 4 or 5 times. Keep the spacer in position and do not remove. • If further puffs are needed, shake the puffer again and repeat steps 4-7.
Using a Puffer • Remove cap from puffer • Hold puffer upright and shake well • Breathe out away from the puffer • Tilt chin upward and put the puffer mouthpiece in mouth, creating a seal with lips • Start breathing in through mouth, then fire one puff. Continue breathing in deeply. • Remove puffer, close mouth and hold for 10 seconds. • Breathe out gently • Repeat steps 2-7 for more medication
Asthma Action Plans • Set of instructions to manage asthma • Helps recognise worsening symptoms and provides different treatment options in order to stop symptoms deteriorating • http://www.rch.org.au/clinicalguide/forms/Asthma_Action_Plan/ • Rates of possession of asthma action plans among Indigenous patients (24.9%) are similar to those among other Australians (22.5%)4
Where to get more information • Asthma Foundation– www.asthmaaustralia.org.au • Asthma Info Line - 1800 ASTHMA (1800 278 462) • Royal Children’s Hospital Melbourne guidelines • Asthma Management Handbook
References • NSW Asthma Survey 2007 • CR Jenkins, B Chang, LM Poulos and GB Marks. Asthma in Indigenous Australians: so much yet to do for Indigenous lung health. MJA. Vol.190(10) 18 May 2009 • Asthma Management Handbook 2006 • Australian Centre for Asthma Monitoring. Asthma in Australia 2008. Canberra: Australian Institute of Health and Welfare, 2008. (AIHW Asthma Series No. 3. AIHW Cat. No. ACM 14.) http://www.aihw.gov.au/publications/index.cfm/title/10584