Asthma Management and Prevention: A Comprehensive Overview
Understand the chronic disease of the airways, including symptoms, pathology, and prevalence in the US. Learn about asthma management and prevention strategies. Explore the impact of asthma on different demographics and regions.

Asthma Management and Prevention: A Comprehensive Overview
E N D
Presentation Transcript
Asthma A Presentation on Asthma Management and Prevention
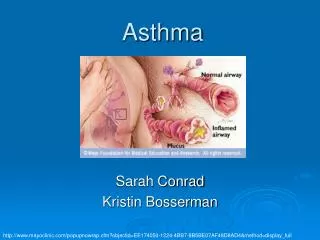
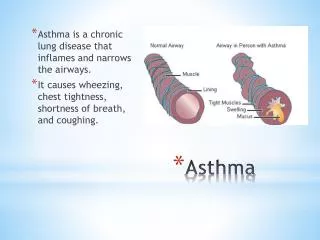
What is Asthma? Chronic disease of the airways that may cause Wheezing Breathlessness Chest tightness Nighttime or early morning coughing Episodes are usually associated with widespread, but variable, airflow obstruction within the lung that is often reversible either spontaneously or with treatment.
Pathology of Asthma Asthma involves inflammation of the airways Asthma Normal Source: “What You and Your Family Can Do About Asthma” by the Global Initiative For Asthma Created and funded by NIH/NHLBI, 1995
Asthma Prevalence in the United States June 2014 National Center for Environmental Health Division of Environmental Hazards and Health Effects
Introduction Asthma: • affects 25.7 million people, including 7.0 million children under 18; • is a significant health and economic burden to patients, their families, and society: • In 2010, 1.8 million people visited an ED for asthma-related care and 439,000 people were hospitalized because of asthma
Introduction Asthma prevalence is an estimate of the percentage of the U.S. population with asthma. Prevalence estimates help us understand the burden of asthma on the nation. • Asthma “period prevalence” is the percentage of the U.S. population that had asthma in the previous 12 months. • “Current” asthma prevalence is the percentage of the U.S. population who had been diagnosed with asthma and had asthma at the time of the survey. • Asthma “period prevalence” was the original prevalence measure (1980-1996). The survey was redesigned in 1997 and this measure was replaced by lifetime prevalence (not presented in slides) and asthma episode or attack in the past 12 months. In 2001, another measure was added to assess current asthma prevalence.
Asthma Period Prevalence and Current Asthma Prevalence: United States, 1980-2010 Currentasthmaprevalence, 2001-2010 Asthma period prevalence, 1980-1996 The percentage of the U.S. population with asthma increased from 3.1% in 1980 to 5.5% in 1996 and 7.3% in 2001 to 8.4% in 2010.
Current Asthma Prevalence: United States, 2001-2010 Percent Total number of persons Year One in 12 people (about 26 million, or 8% of the U.S. population) had asthma in 2010, compared with 1 in 14 (about 20 million, or 7%) in 2001.
Current Asthma Prevalence by Race and Ethnicity:United States, 2001-2010 Blacks are more likely to have asthma than both Whites and Hispanics.
Current Asthma Prevalence by Age Group, Sex, Race and Ethnicity, Poverty Status, Geographic Region, and Urbanicity: United States, Average Annual 2008-2010 Children, females, Blacks, and Puerto Ricans are more likely to have asthma. People with lower annual household income were more likely to have asthma. Residents of the Northeast and Midwest were more likely to have asthma. Living in or not in a city did not affect the chances of having asthma.
Child and Adult Current Asthma Prevalence by Age and Sex: United States, 2006-2010 Among children aged 0-14, boys were more likely than girls to have asthma. Boys and girls aged 15-17 years had asthma at the same rate.. Among adults women were more likely than men to have asthma.
Asthma Attack Prevalence among Children and Adults with Current Asthma: United States, 2001-2010 Children aged 0-17 years Adults aged 18 and over From 2001 to 2010 both children and adults had fewer asthma attacks. For children, asthma attacks declined from at least one asthma attack in the previous 12 months for 61.7% of children with asthma in 2001 to 58.3% in 2010. For adults, asthma attacks declined from at least one asthma attack in the previous 12 months for 53.8% of adults with asthma in 2001, to 49.1% in 2010.
Asthma Attack Prevalence among Persons with Current Asthma by Age Group, Sex, Race and Ethnicity, Poverty Status, and Geographic Region: Unites States, Average Annual 2008-2010 From 2008 to 2010 asthma attacks occurred more often in children and women, among families whose income was below 100% of the federal poverty threshold, and in the South and West. Race or ethnicity did not significantly affect asthma attack prevalence.
Technical Notes Asthma Period Prevalence and Current Asthma Prevalence: Estimates of asthma prevalence indicate the percentage of the population with asthma at a given point in time and represent the burden on the U.S. population. Asthma prevalence data are self-reported by respondents to the National Health Interview Survey (NHIS). Asthma period prevalence was the original measure (1980-1996) of U.S. asthma prevalence and estimated the percentage of the population that had asthma in the previous 12 months. From 1997-2000, a redesign of the NHIS questions resulted in a break in the trend data as the new questions were not fully comparable to the previous questions. Beginning in 2001, current asthma prevalence (measured by the question, ‘‘Do you still have asthma?’’ for those with an asthma diagnosis) was introduced to identify all persons with asthma. Current asthma prevalence estimates from 2001 onward are point prevalence (previous 12 months) estimates and therefore are not directly comparable with asthma period prevalence estimates from 1980 to 1996 Behavioral Risk Factor Surveillance System (BRFSS): State asthma prevalence rates on the map come from the BRFSS. The BRFSS is a state-based, random-digit-dialed telephone survey of the noninstitutionalized civilian population 18 years of age and older. It monitors the prevalence of the major behavioral risks among adults associated with premature illness and death. Information from the survey is used to improve the health of the American people.More information about BRFSS can be found at: http://www.cdc.gov/brfss/.
What is Epidemiology? The study of the distribution and determinants of diseases and injuries in human populations. Source: Mausner and Kramer, Mausner and Bahn Epidemiology- An Introductory Text, 1985.
Risk Factors for Developing Asthma Genetic characteristics Occupational exposures Environmental exposures
Risk Factors for Developing Asthma: Genetic Characteristics Atopy The body’s predisposition to develop an antibody called immunoglobulin E (IgE) in response to exposure to environmental allergens Can be measured in the blood Includes allergic rhinitis, asthma, hay fever, and eczema
Risk Factors for Developing Asthma: Environmental Exposure Clearing the Air: Asthma and Indoor Air Exposures http://www.iom.edu (Publications) Institute of Medicine, 2000 Committee on the Assessment of Asthma and Indoor Air Review of current evidence about indoor air exposures and asthma
Clearing the Air:Categories for Associations of Various Elements Sufficient evidence of a causal relationship Sufficient evidence of an association Limited or suggested evidence of an association Inadequate or insufficient evidence to determine whether an association exists Limited or suggestive evidence of no association
Clearing the Air:Indoor Air Exposures & Asthma Development Biological Agents Sufficient evidence of causal relationship House dust mite Sufficient evidence of association None found Limited or suggestive evidence of association Cockroach (among pre-school aged children) Respiratory syncytial virus (RSV) Chemical Agents Sufficient evidence of causal relationship None found Sufficient evidence of association Environmental Tobacco Smoke (among pre-school aged children) Limited or suggestive evidence of association None found
Clearing the Air: Indoor Air Exposures & Asthma Exacerbation Biological Agents Sufficient evidence of causal relationship Cat Cockroach House dust mite Sufficient evidence of an association Dog Fungus/Molds Rhinovirus Limited or suggestive evidence of association Domestic birds Chlamydia and Mycoplasma pneumonia RSV Chemical Agents Sufficient evidence of causal relationship Environmental tobacco smoke (among pre-school aged children) Sufficient evidence of association NO2, NOX (high levels) Limited or suggestive evidence of association Environmental Tobacco Smoke (among school-aged, older children, and adults) Formaldehyde Fragrances
Reducing Exposure to House Dust Mites Use bedding encasements Wash bed linens weekly Avoid down fillings Limit stuffed animals to those that can be washed Reduce humidity level (between 30% and 50% relative humidity per EPR-3) Source: “What You and Your Family Can Do About Asthma” by the Global Initiative For Asthma Created and funded by NIH/NHLBI, 1995
Reducing Exposure to Environmental Tobacco Smoke Evidence suggests an association between environmental tobacco smoke exposure and exacerbations of asthma among school-aged, older children, and adults. Evidence shows an association between environmental tobacco smoke exposure and asthma development among pre-school aged children.
Reducing Exposure to Cockroaches Remove as many water and food sources as possible to avoid cockroaches.
Reducing Exposure to Pets • People who are allergic to pets should not have them in the house. • At a minimum, do not allow pets in the bedroom.
Reducing Exposure to Mold Eliminating mold and the moist conditions that permit mold growth may help prevent asthma exacerbations.
Other Asthma Triggers • Air pollution • Trees, grass, and weed pollen
Clinical Management of Asthma Expert Panel Report 3 National Asthma Education and Prevention Program National Heart, Lung and Blood Institute, 2007 Source: http://www.nhlbi.nih.gov/guidelines/asthma/asthgdln.pdf
2007 NAEPP EPR-3 Treatment recommendations based on: Severity Control Responsiveness Provide patient self-management education at multiple points of care Reduce exposure to inhaled indoor allergens to control asthma-multifaceted approach Source: http://www.nhlbi.nih.gov/guidelines/asthma/asthgdln.pdf
What is GIP? Guidelines Implementation Panel Report for Expert Panel Report 3 Recommendations and strategies to implement EPR-3 Six key messages Source: http://www.nhlbi.nih.gov/guidelines/asthma/gip_rpt.pdf
Inhaled Corticosteroids Asthma Action Plan Asthma Severity Asthma Control Follow-up Visits Allergen and Irritant Exposure Control GIP’s Six Key Messages Source: http://www.nhlbi.nih.gov/guidelines/asthma/gip_rpt.pdf
Diagnosing Asthma: Medical History Symptoms Coughing Wheezing Shortness of breath Chest tightness Symptom Patterns Severity Family History
Diagnosing Asthma Troublesome cough, particularly at night Awakened by coughing Coughing or wheezing after physical activity Breathing problems during particular seasons Coughing, wheezing, or chest tightness after allergen exposure Colds that last more than 10 days Relief when medication is used
Diagnosing Asthma Wheezing sounds during normal breathing Hyperexpansion of the thorax Increased nasal secretions or nasal polyps Atopic dermatitis, eczema, or other allergic skin conditions
Diagnosing Asthma:Spirometry Test lung function when diagnosing asthma
Medications to Treat Asthma Medications come in several forms. Two major categories of medications are: Long-term control Quick relief
Medications to Treat Asthma:Long-Term Control Taken daily over a long period of time Used to reduce inflammation, relax airway muscles, and improve symptoms and lung function Inhaled corticosteroids Long-acting beta2-agonists Leukotriene modifiers
Medications to Treat Asthma: Quick-Relief Used in acute episodes Generally short-acting beta2agonists
Medications to Treat Asthma: How to Use a Spray Inhaler The health-care provider should evaluate inhaler technique at each visit. Source: “What You and Your Family Can Do About Asthma” by the Global Initiative for Asthma Created and funded by NIH/NHLBI
Medications to Treat Asthma: Inhalers and Spacers Spacers can help patients who have difficulty with inhaler use and can reduce potential for adverse effects from medication.
Medications to Treat Asthma:Nebulizer Machine produces a mist of the medication Used for small children or for severe asthma episodes No evidence that it is more effective than an inhaler used with a spacer
Managing Asthma: Asthma Management Goals Achieve and maintain control of symptoms Maintain normal activity levels, including exercise Maintain pulmonary function as close to normal levels as possible Prevent asthma exacerbations Avoid adverse effects from asthma medications Prevent asthma mortality
Managing Asthma: Asthma Action Plan Develop with a physician Tailor to meet individual needs Educate patients and families about all aspects of plan Recognizing symptoms Medication benefits and side effects Proper use of inhalers and Peak Expiratory Flow (PEF) meters
Managing Asthma: Sample Asthma Action Plan Describes medicines to use and actions to take National Heart, Blood, and Lung Institute Expert Panel Report 3 (EPR 3): Guidelines for the Diagnosis and Management of Asthma. NIH Publication no. 08-4051, 2007.
Managing Asthma: Peak Expiratory Flow (PEF) Meters Allows patient to assess status of his/her asthma Persons who use peak flow meters should do so frequently Many physicians require for all severe patients
Managing Asthma: Peak Flow Chart People with moderate or severe asthma should take readings: Every morning Every evening After an exacerbation Before inhaling certain medications Source: “What You and Your Family Can Do About Asthma” by the Global Initiative For Asthma Created and funded by NIH/NHLBI
Managing Asthma:Indications of a Severe Attack Breathless at rest Hunched forward Speaks in words rather than complete sentences Agitated Peak flow rate less than 60% of normal
Managing Asthma:Things People with Asthma Can Do Have an individual management plan containing Your medications (controller and quick-relief) Your asthma triggers What to do when you are having an asthma attack Educate yourself and others about Asthma Action Plans Environmental interventions Seek help from asthma resources Join an asthma support group