Asthma
Asthma. SS Visser, Lung Unit, UP. Contents. Definition Disease Pattern Prevalence Mortality Etiology Pathogenesis Triggers of acute attacks. Contents. Pathophysiology Manifestations of Resp failure Diagnosis: clinical,physiologic,immunologic and radiologic Differential diagnosis

Asthma
E N D
Presentation Transcript
Asthma SS Visser, Lung Unit, UP
Contents • Definition • Disease Pattern • Prevalence • Mortality • Etiology • Pathogenesis • Triggers of acute attacks
Contents • Pathophysiology • Manifestations of Resp failure • Diagnosis: clinical,physiologic,immunologic and radiologic • Differential diagnosis • Management
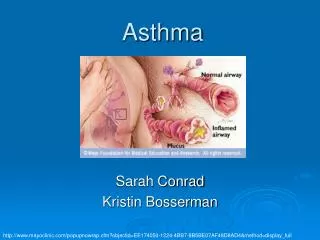
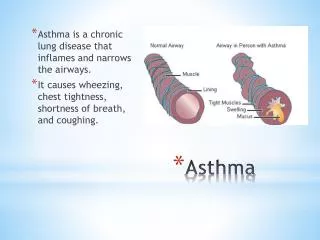
Definition • Chronic inflammatory disease of airways (AW) • responsiveness of tracheobronchial tree • Physiologic manifestation: AW narrowing relieved spontaneously or with BD Cster • Clinical manifestations: a triad of paroxysms of cough, dyspnea and wheezing.
Disease Pattern • Episodic --- acute exacerbations interspersed with symptom-free periods • Chronic --- daily AW obstruction which may be mild, moderate or severe superimposed acute exacerbations • Life-threatening--- slow-onset or fast-onset (fatal within 2 hours)
Prevalence • All ages, predominantly early life • Adults: 2-5% population • Children: 15% population • 50% dx <10y,85% dx <40y, 15% dx > 40y • 2:1 male/female preponderance in childhood
Mortality • Fatal asthma 1-7% asthmatics • ing death rate ?abuse of inhaled BDs • Risks for death:previous life-threatening asthma, severe disease, recent hospitalization or emergency room Rx, non-compliant and confusion re Rx, under- treatment with Corticosteroids, discontinued Rx, severe AW hyperreactivity.
Etiology • Allergic/atopic/early onset asthma---rhinitis, urticaria,eczema,(+)skin tests,IgE,(+) response to provocation tests with aeroallergens. • Idiosyncratic/non-atopic/late onset asthma--- no allergic diseases,(-)skin tests,normal IgE, symptoms when upper resp infection, sx lasting days or months. • Mixed group---usually onset later in life
Pathogenesis - 1 • Non-specific AW hyperreactivity: Sx more severe & persistent Nocturnal early awakening with dyspnea diurnal fluctuation in lung function Unstable lung function BD response, therapeutic needs • Cause of hyperreactivity = inflammation
Pathogenesis - 2 • Dual AW response to AG challenge 1.Early bronchospastic response- type1reaction within min after IH of AG: Mechanism: IH of aeroallergensensitizatiom formation of IgE & expression on mast cells re-exposure to AG mast cell degranulation & mediator release bronchospasm
Pathogenesis - 3 2.Late-bronchospastic reaction: in 30-50%, 6-10 hours after AG exposure. Minority only a late response Mechanism: recruitment of E, N, L and macro-phagesrelease lipid mediators(PG E2, F2 ,D2; LT C,D,E , PAF), O2radicals, toxic granule proteins, cytokines (TH1:IL-2, IFN; TH2: IL-4, IL-5) bronchoconstriction, vascular congestion, mucosal edema, mucus production, mucociliary transport.
Pathogenesis - 4 • Chronic asthmatic response: Destruction of AW epithelium by toxic granule contentsepithelial shedding into bronchial lumen exposure of sensory nerve endings and imbalance in cholinergic and peptidergic neuronal control AW remodelling with subendothelial fibrosis, goblet cell hyperplasia, smooth muscle hyper- trophy, vascular changes fixed AW obstruction.
Allergens - pollen Pharmacol stimuli such as aspirin, NSAIDS, - adrenergic blockers, preservatives,col agent Environment pollution- ozone, SO2, NO2 Occupational- metal salts, biol enzymes Infection- resp viruses Exercise –IH cold dry airthermally-induced hyperemia and micro-vascular engorgement Emotional stress Triggers of acute asthmatic episodes
Pathophysiology • Reduction in AW diameterAW resistance FeV and flow rates hyperinflation work of breathing altered respiratory muscle Fx and elastic recoil abnormal ventilation • Vascular congestion and edema of bronchial walls abnormal perfusion • V/P mismatch altered blood gases hypoxemia and hypocapnia with respiratory alkalosis, but with impending ventilatory failure normocapnia and later hypercapnia and respiratory acidosis
Manifestations of respiratory failure • Hypoxemia: cyanosis- very late sign, not dependable • Hypercapnia: sweating, tachycardia,widened pulse pressure • Acidosis: tachypnea • Blood gases the only accurate assessment of ventilatory status
DIAGNOSIS : CLINICAL • Episodic asthma: Paroxysms of wheeze, dyspnoea and cough, asymptomatic between attacks. • Acute severe asthma: Upright position, use accessory resp muscles, can’t complete sentences in one breath, tachypnea > 25/min, tachycardia > 110/min, PEF < 50% of pred or best, pulsus paradoxus, chest hyperresonant, prolonged expiration, breath sounds decreased, inspiratory and expiratory rhonchi, cough.
DIAGNOSIS : CLINICAL • Life-threatening features: PEF < 33% of pred or best, silent chest, cyanosis, bradycardia, hypotension, feeble respiratory effort, exhaustion, confusion, coma, PaO2 < 60, PCO2 normal or increased, acidosis (low pH or high [H+]). • Chronic asthma: Dyspnea on exertion, wheeze, chest tightness and cough on daily basis, usually at night and early morning; intercurrent acute severe asthma (exacerbations) and productive cough (mucoid sputum), recurrent respir-atory infection, expiratory rhonchi throughout and accentuated on forced expiration.
DIAGNOSIS : PHYSIOLOGIC • Demonstration of variable airflow obstruction with reversibility by means of FEV1 and PEF measurement (spirometer and peak flow meter). • FEV1 < 80% of pred – PEF < 80% of pred. • Reversibility: A good bronchodilator response is a 12% and 200ml improvement in FEV1 20 min after inhalation of 200ug salbutamol (2 puffs). • Diurnal peak flow variation: Normal variation: Morning PEF 15% lower than evening PEF. With asthma this variation is > 15% (morning dipping).
DIAGNOSIS : PHYSIOLOGIC • Provocation studies: (a) Exercise: A 15% drop in FEV1 post exercise indicates exercise induced asthma. (b) Metacholine challenge: A 20% reduction in FEV1 at Metacholine concentrations < 8mg/ml indicates bronchial hyperreactivity. This is expressed as a PC20 value of eg 0.5mg/ml (= a 20% reduction in FEV1 at 0.5mg/ml Metacholine).
DIAGNOSIS : IMMUNOLOGIC • Skin prick wheal and flare response. • IgE and RAST. • Eosinophil cationic protein (ECP). • Peripheral blood and sputum eosinophilia.
DIAGNOSIS : RADIOLOGY • Chest XR may be normal between attacks. • With attacks hyperinflation may be found. • In complicated asthma segmental lobar collapse (mucous plugs) and pneumothorax can occur.
DIFFERENTIAL DIAGNOSIS • Upper airway obstruction – glottic dysfunction. • Acute LV failure – pulmonary oedema. • Pulmonary embolism. • Endobronchial disease. • Chronic bronchitis. • Eosinophilic pneumonia. • Carsinoid syndrome. • Vasculitis.
MANAGEMENT 1 • Avoidance of allergen and triggers – may be impractical adjust Rx. • Occasional asthma: Rarely symptomatic 2 agonist prn. • Mild intermittent asthma (episodic): 2 agonist prn + low dose IH corticosteroid. • Mild persistent asthma: 2 agonist prn + high dose IH corticosteroid or long acting 2 agonist + low dose IH corticosteroid. • Moderate persistent asthma: 2 agonist prn + high dose IH corticosteroid + long acting 2 agonist or SR theophylline.
MANAGEMENT 2 • Severe, persistent asthma 2 agonist prn + high dose IH corticosteroid + long acting 2 agonist + SR Theophylline + oral corticosteroids. • Step up: If uncontrolled at any severity level, oral steroids – Prednisone 30-40-mg/day for 7-14 days. • Step down: When stable for at least 3 months – reduce or stop oral steroids first. • Leukotriene antagonists: for patients with aspirin/NSAIDS induced asthma. May also be added on for severe persistent asthma or in pts with steroid related side effects such as growth retardation or non-responsiveness to IHS or to allow low dose IHS instead of high dose.
MANAGEMENT 3 • Acute severe asthma: 1. Immediate Rx: O2 40-60% via mask or cannula + 2 agonist (salbutamol 5mg) via nebulizer + Prednisone tab 30-60mg and/or hydrocortisone 200mg IV. With life-threatening features add 0.5mg ipratropium to nebulized 2 agonist + Aminophyllin 250mg IV over 20 min orsalbutamol 250ug over 10 min. 2. Subsequent Rx: Nebulized 2 agonist 6 hourly + Prednisone 30-60mg daily or hydrocortisone 200mg 6 hourly IV + 40-60% O2.
MANAGEMENT 4 • No improvement after 15-30 min: Nebulized 2 agonist every 15-30 min + Ipratropium. • Still no improvement: Aminophyllin infusion 750mg/24H (small pt), 1 500mg/24H (large pt), oralternatively salbutamol infusion. • Monitor Rx: Aminophyllin blood levels + PEF after 15-30 min + oxymetry (maintain SaO2 > 90) + repeat blood gases after 2 hrs if initial PaO2 < 60, PaCO2 normal or raised and patient deteriorates. • Deterioration: ICU, intubate, ventilate + muscle relaxant.