Enhancing Occupational Asthma Management: Research and Education Initiatives
360 likes | 481 Views
This program aims to enhance the understanding and management of occupational asthma by addressing the physico-social environment at workplaces. Funded by IRSST and Lung Associations, with a budget of $400,000 from 2003-2009, the project supported studentships, fellowships, and project initiation. Led by 13 researchers from Université de Montréal and McGill, it promotes health professional education on the importance of early referral to improve the prognosis of occupational asthma. For more details, visit www.asthma-workplace.com.

Enhancing Occupational Asthma Management: Research and Education Initiatives
E N D
Presentation Transcript
Program: CIHR Centers for Research Development: Understanding/Addressing Physico-Social Environment, Financial partners: IRSST and Lung Associations of Canada and of Québec 13 researchers of various disciplines of UdM and McGill, as well as scientific (IRSST) and strategic partners (Québec CSST and WCBs of Atlantic provinces, Montreal Public Health) Annual budget of 400 000 $ (2003-2009) for supporting 1) studentships and fellowships, 2) initiation of projects (7/yr) and 3) continuous education of health professionals See details on website: www.asthma-workplace.com
Acknowledgements and thanks • The Canadian Occupational Health Nurses Association and the Occupational Health Nurses Association of Nova Scotia. • The organizers of this meeting. • Mme Sylvie Daigle, coordinator of the Center for Asthma in the Workplace. • Lecturers and coordinators of workshops. And all attendees !
General aim Inform and motivate health professionals on the importance of reducing referral delays in order to improve the prognosis of occupational asthma. Specific aims Explain the nature of the problem. Identify causal agents. Describe investigational tools. Be informed on the different steps to be included in surveillance programs and in assessing specific workers. Know on the natural history and persistence.
Asthma in the workplace: General considerations Jean-Luc Malo MD, professor, Université de Montréal, chest physician, clinical researcher, Hôpital du Sacré-Cœur de Montréal Supported by: Instituts canadiens de recherche en santé Institut Robert-Sauvé en santé et sécurité du travail du Québec (IRSST) L’Association pulmonaire du Canada et l’Association pulmonaire du Québec
Suggested references Book Bernstein IL, Chan-Yeung M, Malo JL, Bernstein DI. Asthma in the Workplace. New York, Francis & Taylor 2006. Summary article Malo JL, Chan-Yeung M. Occupational asthma. Journal of Allergy & Clin Immunol 2001; 108:317-328. 3. Series Controversies in occupational asthma. Six articles in the Eur Respir J 2003 UptoDate : four articles Proceedings of the first and second Jack Pepys Occupational Asthma Symposium. Am J Respir Crit Care Med 2003 ; 167 : 450-471; An ATS/ERS Report: 100 key questions and needs in occupational asthma. Eur Respir J 2006; 27:607-614. 4. WEB sites Asthma in the workplace Center: asthma-workplace.com CSST : asthme.csst.qc.ca/
Asthma in the workplace Definitions Frequency and risk factors Mechanisms 4. Identification and diagnosis 5. Medicolegal aspects 6. As a model for asthma
Asthma in the workplace Asthma caused by the workplace (occupational asthma) Asthma exacerbated by the workplace Variants of asthma ex: eosinophilic bronchitis; “potroom asthma” With a latency period Without a latency period « Irritant-induced asthma » or « Reactive airways dysfunction syndrome »
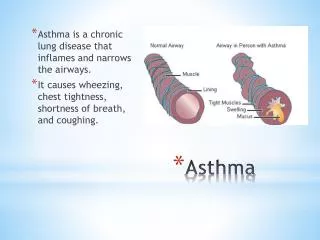
Definition of occupational asthma “Occupational asthma is a disease characterized by variable airflow limitation and/or hyperresponsiveness and/or inflammation due to causes and conditions attributable to a particular occupational environment and not to stimuli encountered outside the workplace.” Editors of Asthma in the Workplace: Bernstein IL, Chan-Yeung M, Malo JL, Bernstein DI, 3rd ed.
Occupational asthma with a latency period Confirmation of the “causal” relationship : changes in airway caliber (~ 20%) ± changes in bronchial responsiveness ± induction of airway inflammation (control asthmatic subjects do not react)
Occupational asthma without a latency period (“irritant-induced asthma”) Diagnosis based on the history : inhalation accident with acute respiratory symptoms. Possibility of several “less intense” inhalation accidents. What does “without a latency” mean ?
Asthma exacerbated at work Symptomatic status exacerbated at work. How to document it with objective means ? How to differentiate this condition from occupational asthma ?
Asthma in the workplace Definitions Frequency and risk factors Mechanisms 4. Identification and diagnosis 5. Medicolegal aspects 6. As a model for asthma
Frequency of asthma in the workplace Meta-analysis: ~ 9% of adult-onset asthmatic subjects report that their asthma is worse at work ( Blanc P, 1999) 2. Prevalence in the general population: surveys in general populations and answer to the following question : is your asthma worse at work, better at weekends and in vacation ? 5-35 % of adult asthmatic subjects answer yes (studies in Spain, Europe and several countries) Prevalence in adult-onset asthmatic subjects seen in a tertiary care hospital clinic : 15 % (Tarlo et al. 1999) 4. Sentinel-based projects: SWORD (UK), SENSOR (USA), OBSERVATOIRE (France) PROPULSE (Québec) : 10-100 / million workers
Frequency of asthma in the workplace 5. Medicolegal statistics: Finland (175 / million workers) and Québec (15 / million workers) 6. Prevalence studies in high-risk workplaces: < 5 % for high-molecular-weight agents 5 to 10% for low-molecular-weight agents 7. Incidence studies of probable occupational asthma: high-risk professions (Gautrin D et al. 1997 onwards) in person-year: 7.9% (animal health), 4.2% (bakers), 2.5% (dental hygiene)
Agents * Occupations • Flour and cereals Bakers • Isocyanates Spray-painters, • plastic industries • Wooddusts Carpenters • Seafood Seafood plants, restaurants • Metals Welders • Resins, glues Various • Animals Technicians, professionals • Latex and drugs Health professionals • * in bold : high-molecular-weight agents; others are low- • molecular-weight agents.
* en noir: agents dits de faible poids moléculaire en bleu: agents dits de haut poids moléculaire
Agents causing occupational asthma without a latency period Agents with irritant properties : vapors and aerosols, more frequently than dusts. Chlorine and ammoniac are the leading causes.
Personal risk factors Relevance of smoking history ? Occupatinal asthma is weakly associated with smoking for a minority of agents. Relevance of skin reactivity to ubiquitous aeroallergens ? • Identification of atopy…but • ~ 50% of the general population is atopic; • Atopy is associated with occupational asthma due to high-molecular-weight agents only but the association is weak Relevance of genes ?
Gautrin D et al. Am J Respir Crit Care Med 2001; 163:899-904
Asthma in the workplace Definitions Frequency and risk factors Mechanisms 4. Identification and diagnosis 5. Medicolegal aspects 6. As a model for asthma
Type of occupational asthma Mechanisms Occupational asthma with a latency period IgE (high-molecular-) weight agents ? (low-molecular- weight agents) Occupational asthma without a latency period (irritant-induced asthma) unknown Asthma exacerbated at work unknown
Asthma in the workplace Definitions Frequency and risk factors Mechanisms 4. Identification and diagnosis 5. Medicolegal aspects 6. As a model for asthma
Why should we consider intervention programs ? • occupational asthma is a disease that can be cured : importance of early removal (one year or less after onset of symptoms) • disease that affects young workers : sensitization and symptoms mainly occur in the first years after starting exposure • currently, 75% of workers are left with permanent asthma (though mild)
Asthma in the workplace Definitions Frequency and risk factors Mechanisms 4. Identification and diagnosis 5. Medicolegal aspects 6. As a model for asthma
In Canada • Asthma is accepted as an occupational lung disease by all provincial medicolegal authorities. • Ideally, diagnosis should be confirmed by objective means. • Assessment of permanent impairment/disability • two years or more after cessation of exposure
Evaluation of 134 cases accepted by the Québec CSST, 1986-1988 * • On average… symptoms had started four years after starting exposure • 8 % workers still unemployed two years after diagnosis (retraining into a new job in 22% workers) • total cost (readaptation + permanent disability) : ~ $ 50 000 • satisfactory quality of life after two years. * Dewitte JD et al. Eur Respir J 1994; 7:969
Scale for assessing permanent impairment/disability Based on airway caliber and hyperreponsiveness as well as need for medication (inhaled steroids). (other items: dose of inhaled steroids, use of long-acting bronchodilator, sputum cells). Endorsed by the American Medical Association.
Asthma in the workplace 1. Definitions 2. Frequency and risk factors 3. Mechanisms 4. Identification and diagnosis 5. Medicolegal aspects 6. As a model for asthma
Natural history of occupational asthma and of asthma Rhinoconjunctivitis; onset of airway inflammation end of exposure cure or persis- tence of asthma onset of exposure occupational asthma sensitization host markers: genetic; atopy; level of bronchial respon- siveness; smoking, psychosocial agent: nature, concentration; duration of exposure; other factors: viral infections, pollutants, smoking, etc. level of bronchial responsiveness duration of exposure, duration of exposure after onset of symptoms, asthma severity at the time of diagnosis anti- inflammatory treatment; compensation and psychosocioeconomic impact Basic research, environmental and psychosocial assessments Evaluative examination of surveillance and compensation programs Clinical and epidemiological expertise R & D projects
Asthma in the workplace Conclusion Definitions distinction between occupational asthma and other conditions 2. Frequency and risk factors asthma in the workplace : ~ 10% of adult-onset asthma 3. Mechanisms IgE-dependent or not identified 4. Identification and diagnosis intervention justified by possibility to cure and good prognosis 5. Medicolegal aspects objective diagnosis; scale to assess impairment/disability 6. As a model for human asthma