PATHOGENIC FUNGI
1.42k likes | 2.38k Views
PATHOGENIC FUNGI. Medical mycology. field of medicine concerned with the diagnosis, managements and prevention of mycoses. MYCOSES. diseases caused by fungi Mode of infection: Inhalation Trauma Ingestion Rarely from person to person Most mycoses are not contagious.

PATHOGENIC FUNGI
E N D
Presentation Transcript
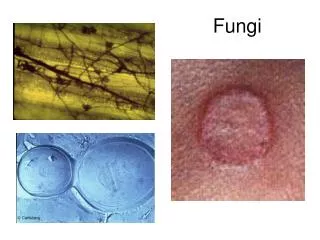
Medical mycology • field of medicine concerned with the diagnosis, managements and prevention of mycoses
MYCOSES • diseases caused by fungi • Mode of infection: • Inhalation • Trauma • Ingestion • Rarely from person to person • Most mycoses are not contagious
Clinical Manifestations of Mycoses • Fungal infections (most common) • Toxicoses (poisoning) • Allergies (hypersensitivity reactions)
DIAGNOSIS • Sabourad dextrose agar – the medium where fungi is cultured • Potassium hydroxide (KOH) preparations – dissolve keratin in skin scrapings or biopsy specimens, leaving only fungal cells for examination • Gomori methenamine silver (GMS) stain – used on tissue to stain fungal cells black • Direct immunofluorescence - labeling of antibodies or antigens with fluorescent dyes.
Mycoses are also among the most difficult diseases to heal.
WHY? • Fungi possess the biochemical ability to resist the oxidative damage perpetuated by T cells during cell-mediated immune response • Fungi are eukaryotic and thus biochemically similar to human cells, which means most fungicides are toxic to human tissues
The Gold Standard!!! • Amphotericin B – considered the best drug for treating systemic mycoses and other fungal infections that do not respond to other drugs
The downside….. It is still toxic to humans
The alternative.. • Azole drugs • which only inhibit the fungi (fungistatic) rather than kill it • less toxic to humans • e.g. ketoconazole, itraconazole and fluconazole
Categories of Fungal Agents • True fungal pathogens • Opportunistic fungi
True pathogens • Have the ability to actively attack and invade tissues • Can infect any host, regardless of its immune status
Opportunistic Fungi • Lack genes for proteins that aid in colonizing the body • Do not cause disease in healthy individuals • Can infect only susceptible individuals, those whose body’s defenses are low
The only fungi known to cause disease in humans: • Blastomyces dermatiditis • Coccidiodes immitis • Histoplasma capsulatum • Paracoccidiodes brasiliensis The remaining fungi that cause disease are considered opportunistic fungi.
The following slides may contain scenes not suitable for very young audiences. Those with weak constitutions are asked to continue paying attention no matter how utterly repulsive you may find it to be. VIEWER’S DISCRETION IS ADVISED.
SYSTEMIC MYCOSIS caused by TRUE PATHOGENS
those fungal infections that spread throughout the body result of infections by one of the four pathogenic, dimorphic fungi of the division Ascomycota. SYSTEMIC MYCOSES • Ascomycota:Blastomyces, Coccidioides, Histoplasma, and Paracocidioides
B L A S T O M Y C O S I S • Pathogen:Blastomyces dermatitidis. • B. dermatitidis normally grows in soil rich in organic material, such as decaying vegetation and animal wastes, where cool, damp conditions favor growth and sporulation.
B L A S T O M Y C O S I S • Mode of infection: Inhalation of dust disturbed from the environmental sources carries fungal spores and pieces of hyphae into the lungs.
B L A S T O M Y C O S I S • Pulmonary Blastomycosis – the most common manifestation of Blastomyces infection in humans. • Initial pulmonary lesions are asymptomatic. • If symptoms do develop, they are vague and include cough, fever, malaise, and weight loss.
B L A S T O M Y C O S I S • Cutaneous blastomycosis – consists of generally painless lesions on the face and upper body. • Can be raised and wartlike, craterlike due to the death of tissue.
B L A S T O M Y C O S I S • Osteoarticular blastomycosis – a condition where fungus spreads to the spine, pelvis, cranium, ribs, long bones, or subcutaneous tissues surrounding joints.
Patients with Cutaneous blastomycosis - • painless lesions on the face and upper body.
B L A S T O M Y C O S I S • Diagnosis – relies on identification of B. dermatitis following culture, or direct examination of various samples such as sputum, bronchial washings, biopsies, cerebrospinal fluid, or skin scrapings. • Treatment – amphotericin for 10 weeks.
COCCIDIOIDOMYCOSIS Pathogen: Coccidioides immitis • Can be recovered from desert soil, rodent burrows, archaeological remains, and mines. • Once inhaled in dust, anthrospores become trapped in the alveolar spaces of the lungs.
COCCIDIOIDOMYCOSIS • Major manifestation - pulmonary • Invasion of the CNS may result in meningitis, headache, nausea, and emotional disturbance
COCCIDIOIDOMYCOSIS • Diagnosis – based on the identification of spherules in KOH- or GMS- treated samples collected from patients • Amphotericin B – the drug of choice
H I S T O P L A S M O S I S • Pathogen: Histoplasma capsulatum • most common fungal pathogen affecting humans. • Two strains recognized: • a. strain capsulatum - intracellular parasite, first attacks alveolar macrophages in lungs • b. strain duboisii - limited to Africa.
H I S T O P L A S M O S I S • Diagnosis – based on the identification of the distinctive budding yeast in KOH- or GMS- prepared samples of skin scrapings, sputum, cerebrospinal fluid, or various tissues.
H I S T O P L A S M O S I S TREATMENT: • Amphotericin B - prescribed when symptoms do not resolve. • Ketoconazole – used to treat mild infections.
PARACOCCIDIOIDOMYCOSIS • Pathogen: Paracoccidioides brasiliensis • chronic granulomatous disease that characteristically produces a primary pulmonary infection, and then disseminates to form ulcerative granulomata of the buccal, nasal and occasionally the gastrointestinal mucosa.
Paracoccidiomycosis patients – ulcerative granulomata of the buccal, nasal mucosa…
PARACOCCIDIOIDOMYCOSIS • Diagnosis - KOH or GMS preparations of tissue samples revealing yeast cells with multiple buds in a “steering wheel” formation. Steering wheel apperance
PARACOCCIDIOIDOMYCOSIS • Treatment - Amphotericin B or Ketoconazole
End of slideshow, click to exit. Aww… sorry, wrong number..