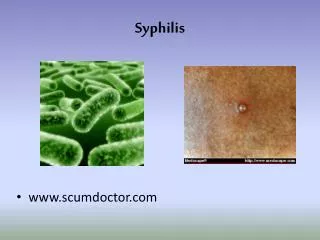
Syphilis
Syphilis. Definition. STI caused by spirochete Treponema pallidum Primary Syphilis- Chancre -papule that ulcerates Forms at the site of inoculation Highly infectious Resolves on its own within a few weeks. Definition cont’d. Secondary Syphilis- 25% go on to this

Syphilis
E N D
Presentation Transcript
Definition • STI caused by spirochete Treponemapallidum • Primary Syphilis- • Chancre -papule that ulcerates • Forms at the site of inoculation • Highly infectious • Resolves on its own within a few weeks
Definition cont’d • Secondary Syphilis- 25% go on to this • rash on the palms and soles • condylomalata (heaped wart-like lesions) • generalized lymphadenopathy, • Fever • Renal involvement • hepatic involvement
Definition cont’d • Tertiary or late syphilis- anywhere from 1-20yrs after infection • Can involve any organ system • Neurosyphilis • Gummas- skeletal, spinal, mucosa, and viscera • Cardiovascular syphilis- ascending aortic aneurysm, aortic insufficiency, or coronary ostial stenosis.
Definition cont’d • Early neurosyphilis- within months to years after infection • acute syphilitic meningitis • basilar meningitis (cranial nerves III, VI, VII and VIII) • meningovascular syphilis (stroke-like syndrome with seizures). • Late neurosyphilis-decades after infection • general paresis • tabesdorsalis
Congenital Syphilis • Early manifestations (in infants under 2yo)-inflammatory • lesions on skin or mucosa • Alopecia • generalized lymphadenopathy • hepatosplenomegaly • osteitis or osteochondritis, • hematologic problems (thrombocytopenia and anemia).
Congenital syphilis cont’d • Late manifestations (kids over 2yo)- destructive immunologic lesions • Interstitial keratitis (corneal scarring)- most common • Deafness (due to damage to CN 8) • bone and teeth involvement • saber shins • mulberry molars • Hutchinson incisors
Diagnosis • Do nontreponemal serological test. • VDRL • RPR • TRUST • USR
Diagnosis • If reactive, then a treponemal serological test is done. • TP-PA • FTA-ABS • EIA (enzyme immunoassay) • CIA (chemiluminescence immunoassays).
Screening • All pregnant women • People at high risk • Homosexuals • Bisexuals • Risky sexual behaviors
Treatment • Benzathine penicillin G IM • Penicillin allergic: Doxycycline or tetracycline orally • For syphilis in pregnancy use penicillin. • If mother is allergic, do desensitization. • For neurosyphilis, IM penicillin. • If allergic, can try ceftriaxone (if not allergic). • If allergic to both, desensitize and treat with penicillin.
Follow-Up • Recheck nontrep test at 6 and 12 months • 4 fold decrease in titers or retreat • Recheck CSF at 3 and 6 months. • If WBC counts not decreasing at 6 months, retreat.
A 23 y/o G1P0 presents at 23 weeks with a painless genital ulcer with a clean base and bilateral inguinal lymphadenopathy. An RPR and confirmatory FTA abs were both positive.What is the most appropriate treatment? • Clindamycin • Flagyl • Oral Penicillin • Penicillin G
Bibliography • Clark EG, Danbolt N. The Oslo study of the natural course of untreated syphilis: An epidemiologic investigation based on a re-study of the Boeck-Bruusgaard material, Med Clin North Am. 1964;48:613. • Sparling, FP, Hicks, CB, & Hynes, NA. Pathogenesis, clinical manifestations, and treatment of early syphilis. UpToDate. Accessed 2/24/14. Last updated 4/10/13. • Sparling, FP, Hicks, CB, & Hynes, NA. Pathogenesis, clinical manifestations, and treatment of late syphilis. UpToDate. Accessed 2/24/14. Last updated 9/28/12. • http://www2a.cdc.gov/stdtraining/self-study/syphilis/self_study_syphilis_clinical. Accessed on 2/24/14. Last updated 8/13. • http://www2a.cdc.gov/stdtraining/self-study/syphilis/self_study_syphilis_diagnostic_2.html. Accessed 2/24/14. Last updated 8/13.