mechanical ventilation
mechanical ventilation. Hashmi. mechanical ventilation method to mechanically assist or replace spontaneous breathing when patients cannot do so on their own currently is positive pressure ventilation

mechanical ventilation
E N D
Presentation Transcript
mechanical ventilation Hashmi
mechanical ventilation • method to mechanically assist or replace spontaneous breathing when patients cannot do so on their own • currently is positive pressure ventilation • increasing the pressure in the patient's airway and thus forcing additional air into the lungs • historically common negative pressure ventilators: "iron lung“ • creates a negative pressure environment around the patient's chest, thus sucking air into the lungs • potential complications • pneumothorax, airway injury, alveolar damage, and ventilator-associated pneumonia, etc
iron lung aka Drinker and Shaw tank developed in 1929 first negative-pressure machines used for long-term ventilation used in the 20th century largely as a result of the polio epidemic that struck the world in the 1940s large elongated tank, which encases the patient up to the neck neck is sealed with a rubber gasket so that the patient's face (and airway) are exposed to the room air
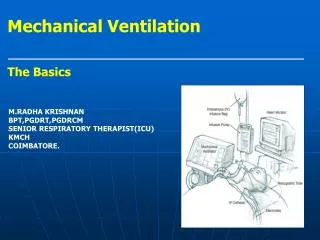
The design of the modern positive-pressure ventilators were mainly based on technical developments by the military during World War II to supply oxygen to fighter pilots in high altitude • Positive pressure hrough a tracheostomy/endotracheal tube led to a reduced mortality rate among patients with polio and respiratory paralysis • Such ventilators replaced the iron lungs as safe endotracheal tubes with high volume/low pressure cuffs were developed • Positive-pressure ventilators work by increasing the patient's airway pressure through an endotracheal or tracheostomy tube • positive pressure allows air to flow into the airway until the ventilator breath is terminated • then airway pressure drops to zero, and the elastic recoil of the chest wall and lungs push the tidal volume -- the breath -- out through passive exhalation
Common medical indications for use include: • Acute lung injury (including ARDS, trauma) • Apnea with respiratory arrest, including cases from intoxication • Chronic obstructive pulmonary disease (COPD) • Acute respiratory acidosis (pCO2 > 50 mmHg and pH < 7.25) • which may be due to paralysis of the diaphragm due to Guillain-Barré syndrome, Myasthenia Gravis, spinal cord injury, or the effect of anaesthetic and muscle relaxant drugs • Increased work of breathing as evidenced by significant tachypnea, retractions, and other physical signs of respiratory distress • Hypoxemia with arterial partial pressure of oxygen (PaO2) with supplemental fraction of inspired oxygen (FiO2) < 55 mm Hg • Hypotension including sepsis, shock, congestive heart failure • Clinical status of patient
Ventilation delivery • Hand-controlled ventilation: • Bag valve mask • Continuous-flow or Anaesthesia (or T-piece) bag • Mechanical ventilator: • Transport ventilators • small, more rugged, and can be powered pneumatically or via AC or DC power sources. • ICU ventilators • PAP ventilators • non-invasive ventilation. this includes ventilators for use at home, in order to treat sleep apnea
Modes of ventilation • volume-cycled • pre-set volume of gas with each breath • time-cycled • limits the length of the inspiratory cycle (I:E ratio) • I-time is set as a percentage of total time (usually 33%) • pressure-cycled • limits the pressure provided with each breath
Breath initiation • Assist Control (AC) • provides a mechanical breath with either a pre-set tidal volume or pressure • same setting every time the patient initiates a breath • Synchronized Intermittent Mandatory Ventilation (SIMV) • pre-set mechanical breath • allows for patients own breathing • Controlled Mechanical Ventilation (CMV) • ventilator provides a mechanical breath on a preset timing • patient respiratory efforts are ignored • used in an unconscious patient
AC Patient breathing 15 TV: 500 x 12 TV: 500 x 3 Patient breathing 10 TV: 500 x 12 SIMV Patient breathing 15 TV: 500 x 12 TV: ??? x 3 Patient breathing 10 TV: 500 x 12 TV: 500 - RR:12
Pressure Support Ventilation (PSV) • endotracheal tube airway results in higher resistance to airflow • higher work of breathing • method to decrease the work of breathing (helps to overcome dead-space) • Continuous Positive Airway Pressure (CPAP) • continuous level of elevated pressure is provided through the patient circuit to maintain adequate oxygenation, decrease the work of breathing • Positive End Expiratory Pressure (PEEP) • functionally the same as CPAP • refers to the use of an elevated pressure during the expiratory phase • volume of gas remaining in the lung after a normal expiration is termed the functional residual capacity (FRC) • FRC is reduced due to collapse of the unstable alveoli, atelectasis, leading to a decreased surface area for gas exchange and intrapulmonary shunting • PEEP can reduce the work of breathing (at low levels) and help preserve FRC • PEEP increases intrathoracic pressure, there can be a resulting decrease in venous return and decrease in cardiac output
Non-invasive ventilation • Continuous positive airway pressure (CPAP) • delivering a stream of compressed air via a hose to a nasal pillow, nose mask or full-face mask • splinting the airway (keeping it open under air pressure) • unobstructed breathing becomes possible, reducing and/or preventing apneas and hypopneas • blows air at a prescribed pressure • Bi-level Positive Airway Pressure (BIPAP) • Pressures alternate between Inspiratory Positive Airway Pressure (IPAP) and Expiratory Positive Airway Pressure (EPAP)
nasal cannula LPMO2 1 24% 2 28% 3 32% 4 36% 5 40% 6 44% venti mask 24% blue 28% yellow 31% white 35% green 40% pink 50% orange partial rebreather 50-70% non-rebreather >70%
FIO2: <60% • RR: 10-12/min • Peep: 5 • PS: 10 • TV: 6-8 ml/kg • As the amount of tidal volume increases, the pressure required to administer that volume is increased • This pressure is known as the peak airway pressure • peak airway pressure is persistently above 45 cmH2O for adults, the risk of barotrauma is increased • convert to pressure control ventilation
Factors effecting O2 FIO2 PEEP I-Time I:E Ratio Factors effecting CO2 TV RR
The best measure of when a patient may be extubated is the Rapid Shallow Breathing Index • is calculated by dividing the respiratory rate by the tidal volume in liters (RR/TV) • A rapid shallow breathing index of less than 100 is considered ideal for extubation • other measures such as patient's mental status such be considered
Oxygenation PaO2 of 60 mmHg w/FiO2 of 0.35 Alveolar-arterial PO2 gradient of <350 mmHg PaO2/FiO2 ratio of >200 Ventilation Vital capacity >10-15 ml/kg body weight negative inspiratory pressure < -30 cmH2O Minute ventilation <10 L/min Airway occlusion pressure <4-6 cmH2O Frequency to tidal volume ratio (f/VT) <100 b/min/liter CROP index >13 ml/breath/min Integrative index of Jabour et al <4/min respiratory system compliance work of breathing
NIF (Negative Inspiratory Force) • Amount of force generated by a patient against a closed valve • >20cmH2O indicates an adequately strong diaphragm • P/F Ratio • PaO2/FiO2 • <200 indicates ARDS • <300 indicates ALI • RSBI (Rapid Shallow Breathing Index) • RR/TV • <105 declares a patient can be extubated and maintain themselves • indicates patient has a good chance of staying extubated • MV (Minute volume or Minute Ventilation) • calculated by taking the TV x RR