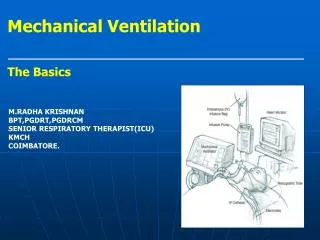
Mechanical ventilation
Mechanical ventilation. Dr.Poddutoori PGY3. Introduction. Specially designed pumps that support Ventilatory functions of RS and improve oxygenation through high O2 and positive pressure. Indications for MV. Hypercarbic resp failure:

Mechanical ventilation
E N D
Presentation Transcript
Mechanical ventilation Dr.Poddutoori PGY3
Introduction • Specially designed pumps that support Ventilatory functions of RS and improve oxygenation through high O2 and positive pressure.
Indications for MV • Hypercarbic resp failure: • Basically decreased Min Ventilation or increased Physiologic dead space. • Neuromuscular disease:M. Gravis, Ascending polyradiculopathy, Myopahty • Muscle fatigue diseases: Asthma, COPD, restrictive lung disease • Pco2 >50mm Hg and Ph <7.3 • Hypoxemic Resp Failure: • Basically a V/Q mismatch and shunt problem • Pneumonia, Pulm edema, ARDS, Pulm hemorrhage • Sao2 <90 despite >60% fio2.
Other indications for MV • Increased ICP – controlled Hyperventilation to reduce cerebral blood flow • Post Op pulmonary HTN: to improve pulmonary hemodynamics • CHF in presence of Myocardial ischemia: To reduce preload and afterload and to reduce work of breathing • Prevent aspiration of Gastric contents: unstable patients needing Lavage for drug overdose and EGD
Physiologic aspects of MV • Hypoxia : fio2 • Hypercarbia: TV x RR = Min Ventilation • PEEP helps maintain patency of alveoli – reverses hypoxemia and atelectasis by improving V/Q matching • Normal is 0-10. Can be increased if refractory hypoxemia needing Fio2 >0.6
Modes of ventilation • O2 by Nasal cannula, ventimask, Nonrebreather • Non Invasive Positive pressure ventilation: CPAP and BIPAP • Invasive ventilation: • Assist control • SIMV
Establishing and maintaining airway • Cuffed ETT is used to maintain Positive pressure and prevent aspiration • Medications used: • Sedatives – avoid long acting benzos. Use Propofol or etomidate • Analgesics – Avoids morphine – can worsen bronchospasm. Use fentanyl. • Paralyzing agents – Succinylcholine should be avoided in renal failure, Tumor lysis, Hyperkalemia.
Terminology • Modes:refers to the manner in which ventilator breaths are triggered,cycled and limited. SIMV, AC • Trigger: defines what the ventilator senses to initiate an assisted breath -an inspiratory effort or time based signal • Cycle: refers to factors that determine the end of inspiration – volume, pressure or flow or time cycled. • Limiting factors: are operator specific values: ex Airway pressure.
Assist control mode • Inspiratory cycle is initiated by inspiratory effort of pt or by timer signal ( back up rate) • Every breath delivered consists of operator specified TV. • Vent rate is determined by either by pt or Operator specified backup rate – which ever is higher
ACMV • Advantages: • Often used for initiation of MV – to ensure backup min Ventilation and synchronization of vent cycle with pts insp effort. Disadvantages: -Respiratory Alkalemia:leading to myoclonus and seizures -Dynamic hyperinflation – auto PEEP and barotrauma, decreased Cardiac output.
SIMV • Pt is allowed to breath spontaneously • Preferred in pts with intact resp drive • Fixed mandatory breaths are delivered in addition to pts RR. • Only the preset number of breaths are ventilator assisted. • Total respiratory rate is Pts RR + Preset rate
SIMV • Advantages: • Exercise respiratory muscles • Easy to wean Disadvantages: -difficult to use in tachypnea- as dysynchrony might occur -cannot be used paralyzed pts.
CPAP and BiPAP • Non invasive ventilation • Used early stages of respiratory distress • Pt should be alert and cooperative • CPAP can also be used to assess extubation potential in intubated pts.
General support in ventilated patients • Sedation – Propofol or etomidate • Analgesia - fentanyl is best • GI prophylaxis: H2 receptor blockers/ carafate/antacids – carafate is preferred as it doesn’t change gastric Ph – so less colonization by nosocomial organisms • Nutrition support: Early feeding is encouraged. • Delayed Gastric emptying: Consider Reglan
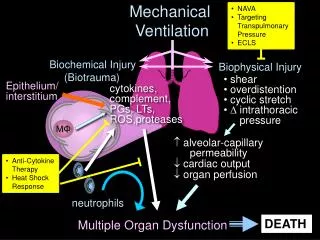
Complications of MV • Pulmonary: • Barotrauma ( if Pr >50cm H2O ) • Vent Associated Pneumonia –( If intubated >72 hrs) – G –ve rods, S.Aureus, Anaerobes. • O2 toxicity • Tracheal stenosis • Respiratory deconditioning • Hypotension – almost always responsive to Volume support • GI: • Stress ulceration– H2 receptor blockers / sucralfate • Cholestasis – Total bilirubin < 4 mg/dl
Weaning criteria - MV • Upper airway functioning should intact – stridor or aspiration. • Intact cough – mobilizes secretions • Alveolar ventilation: Ph 7.35 – 7.45, Sao2 >90 %,Fio2 <0.5, PEEP <5. • Respiratory drive and chest wall function should be assessed ( TV, Insp Pressure, RR, VC) • Weaning index: breathing frequency/ TV <105. • VC >10 ml/kg, Insp Pr> -30 cm H2O.
Methods of weaning • Short term ventilated pts: 5 min/ hr. Gradually increased every hour. • T Piece ( on O2) • CPAP • Long term ventilated pts: • SIMV – decrease mandatory backup rate 2-4 breaths/min and reasses each time( if >25 or worsening PH indicates difficulty in weaning) • PSV - Gradually reduce the pressure to below Peak insp pressures by 5cm H2O until the pressures Just equal to ET tube pressure (5-10 normally)