Mechanical Ventilation
Mechanical Ventilation. Wollongong CGD, October 31. “If you take a dead animal and blow air through its larynx [through a reed], you will fill its bronchi and watch its lungs attain the greatest distention.” Galen. Indications for Ventilation. ALI Apnoea and Respiratory Arrest COPD

Mechanical Ventilation
E N D
Presentation Transcript
Mechanical Ventilation • Wollongong CGD, October 31
“If you take a dead animal and blow air through its larynx [through a reed], you will fill its bronchi and watch its lungs attain the greatest distention.” Galen
Indications for Ventilation • ALI • Apnoea and Respiratory Arrest • COPD • Respiratory Acidosis (elevated PC02) • Increased work of breathing • Hypoxaemia • Hypotension (sepsis, shock, CCF) • Neurological Disease (ALS, Muscular Dystrophy)
Types of Ventilation • Invasive ventilation (Positive Pressure) • Volume Control • Pressure Control
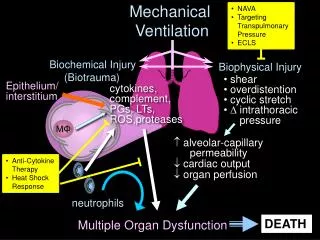
Complications • Barotrauma • VALI (Ventilator associated lung injury) • Diaphragmatic atrophy • Impaired mucociliary function • Ventilator associated pneumonia
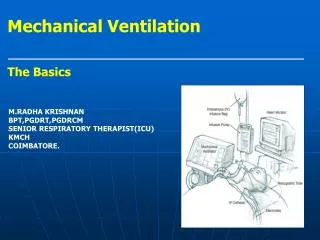
Ventilator Set-Up. • Select mode (CMV / SIMV) • Set tidal volume (PS in pressure controlled ventilation) • Set IFR • Set FIO2 and PEEP (oxygenation) • Set RR (ventilation)
Case 1 • 25 year old female with severe asthma is intubated shortly after arrival to the ED. • You have been asked to retrieve the patient. • On arrival to the ED you find a very unwell patient. (P 140, BP 70/40, Pulse Ox 80% on 100% oxygen) • She is chewing on the tube and is breathing up over the ventilator settings.
Case 1 • ABG; pH 7.30, PO2 60, PCO2 70, BE -1. • Acute respiratory acidosis with hypoxaemia.
Case 1 • Hypotension - likely due to breath-stacking. Disconnect from ventilator and allow to exhale. • Goals are to support fatigued patient and allow adequate time to expire.
Case 1 • Set mode to CMV • Patients tidal volume should be at a preset 8 mL/kg (based on ideal body weight) • Increase IFR to 80-100 L per minute (allows more prolonged expiratory phase)
Case 1 • Oxygenation is usually not a problem. • PEEP is for alveolar recruitment, which is not required in this setting. • Set PEEP to zero and adjust FIO2 to maintain O2 sats 88-92%.
Case 1 • Respiratory Rate - most important setting in asthmatic patient. • Set rate low (permissive hypercapnoea) • pH 7.0 - 7.1 and PCO2 up to 90 mmHg.
Case 1 • Low breath rate allows adequate exhalation time, preventing autoPEEP and air-trapping. • Check the waveform to ensure return to baseline between breaths. If not, then reduce the respiratory rate.
Case 1 • Check airway pressures. Peak airway pressure is not useful. Check the PLATEAU Pressure. • Press inspiratory hold button to measure. • Aim for pressure less than 30 mmHg. • If elevated, then reduce tidal volume.
Case 1 • Asthmatic patients require deep sedation. • Use propofol as it has a bronchodilatory effect. • Don't forget to give analgesia as well - use fentanyl infusion.
Case 1 • Don't forget to treat the underlying problem (asthma) • Steroids, bronchodilators, magnesium
Case 2 • 65 year old male - MVA 24 hour previously. • Admitted to HDU for observation with multiple rib fractures. • 18 hour after admission, he becomes severely SOB and requires intubation.
Case 2 • ARDSnet showed mortality reduction using a lung protective ventilation strategy.
Case 2 • Tidal volume of 6-8 mL/kg • Based on lean body weight • Start high and reduce rate as needed.
Case 2 • IFR set lower at 60-80 L per minute. • More comfortable for the patient.
Case 2 • Respiratory Rate (ventilation) • Start at 18 breaths per minute and titrate to PCO2.
Case 2 - FIO2 / PEEP • Oxygenation (SpO2 88-92%) • Increased PEEP does not cause PTx • Increased PEEP will cause reduced venous return and hypotension.
Case 2 • Benefits of PEEP • Reduced atelectasis • Reduced shunt • Increase in V/Q ratio
Case 2 • FIO2 / PEEP; Start at 100% oxygen for the intubation and then reduce down to 40%. • Titrate FIO2 and PEEP up to aim for target Sp02.
Case 2 • Plateau Pressure should be less than 30 mmHg (lung protective effect) • Reduce tidal volume if pressure too high.
Teaching Points • 2 main strategies - Obstructive Lung Disease and Acute Lung Injury. • COPD / Asthma - oxygenation NOT the issue - it’s fatigue. Permissive hypercapnoea and prolonged expiratory times. • ALI - “Baby Lungs” - aim to ventilate only the normal “uninjured alveoli” using lung protective strategy.