Birth control: hormonal methods
Birth control: hormonal methods. Maša Vikić-Topić Mentor: A. Žmegač Horvat. Introduction. Oral hormones: the pill Morning-after pill Injection: depot medroxypro- gesterone acetate (DMPA) Contraceptive patch Vaginal ring Contraceptive implants.

Birth control: hormonal methods
E N D
Presentation Transcript
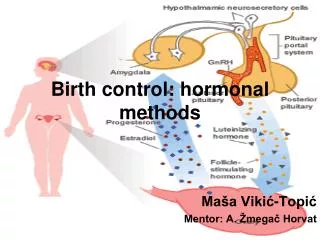
Birth control: hormonal methods Maša Vikić-Topić Mentor: A. Žmegač Horvat
Introduction • Oral hormones: the pill • Morning-after pill • Injection: depot medroxypro- gesterone acetate (DMPA) • Contraceptive patch • Vaginal ring • Contraceptive implants
Because of many side-effects, OCP can be bought only with a doctor’s prescription. • OCP is effective on some animals. • Because of its simple use, OCP were easily introduced in many parts of the world. • The first OCP were made out of wild yam root. • If pregnancy occurs under OCP, there is a higher risk of multiple pregnancies.
Oral contraceptive pills (OCP) • Oral contraceptive made from synthetic hormones • 97%-99% effective • Combined pill or mini-pill
Combined pill • Contains estrogen and progestin • 21-day or 28-day form • Monophasic or multiphasic (fewer side effects) • Effect: ova do not mature so there is no ovulation
Mini-pill • Contains only progestin • Used continuously 28 days • Effect: thickens the cervical mucus and makes the lining of the uterus less receptive to implantation • Indicated because of medical reasons and women breatsfeeding
Absolute: CV diseases, liver damage, hormone-dependent tumors Relative: age >35 + another risk factor (smoking, DM etc.) Contraindications
↓ Dysmenorrhea ↓ Ovarian carcinoma ↓ Endometrial carcinoma ↓ Ovarian cysts ↓ Breast cysts ↓ PID ↓ Risk of ectopic pregnancy ↓ Anemia ↓ Acne ↓ Hair growth ↓ Osteoporosis Pro’s
↑ Risk of CV disease ↑ Risk of breast cancer ↑ Risk of cervical cancer ↑ Risk of thromboembolic episodes ↑ Risk of liver adenoma Lipid metabolism disorders Nausea Depression Post-pill amenorrhea Weight gain Breast tenderness Con’s
Morning-after pill • Contains a progestin or a progesterone agonist-antagonist • Effect: prevents or delays ovulation, blocks fertilization, or keeps a fertilized egg from implanting in the uterus • Application: oral, up to 107 to 120 hours after intercourse • Side effects: nausea,abdominal pain, fatigue, headache, dizziness, and breast tenderness
Injection depot DMPA • Synthetic long-acting form of the hormone progesterone • Effect: prevents the release of the ova from the ovary (ovulation); promotes thick cervical mucus • Application: injected every three months (12 weeks) • Side effects: irregular menstrual cycles, cessation of menstrual periods, weight gain • Con: long time before pregnancy can occur
Contraceptive patch • Transdermal delivery system • Effect: same as OCP • Application: stuck on skin every week • Side effects: same as OCP, greater risk (con) • Pro: better compliance
Vaginal ring • Device that contains combined hormones • Effect: same as OCP • Application: placed in the vagina for 3 weeks • Side effects: same as OCP + increased vaginal discharge
Contraceptive implants • Slow release of a progestin over a period of three years • Effect: prevents the release of the egg from the ovary (ovulation); promotes thick cervical mucus • Application: inserted in the upper arm under local anesthesia • Side effects: irregular bleeding • Pro: fertility rapidly returns