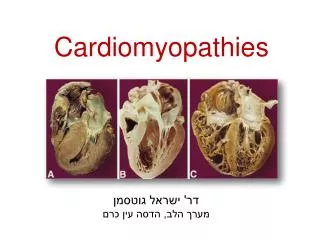
Cardiomyopathies
Cardiomyopathies. Introduction. Define Cardiomyopathy Primary Cardiomyopathies Hypertrophic Cardiomyopathy ARVD Ion Channelopathies Dilated Cardiomyopathy Restrictive Cardiomyopathy Myocarditis Others Secondary Cardiomyopathies Infiltrative Disease. Evolving Definition.

Cardiomyopathies
E N D
Presentation Transcript
Introduction • Define Cardiomyopathy • Primary Cardiomyopathies • Hypertrophic Cardiomyopathy • ARVD • Ion Channelopathies • Dilated Cardiomyopathy • Restrictive Cardiomyopathy • Myocarditis • Others • Secondary Cardiomyopathies • Infiltrative Disease
Evolving Definition • 1957 – Cardiomyopathy used for first time • 1980 WHO – “heart muscle disease of unknown cause” • 1984 WHO – “diseases of different and often unknown etiology in which the dominant feature is cardiomegaly and heart failure” • 1995 WHO – “disease of myocardium associated with cardiac dysfunction”
Current Consensus Definition • “a heterogeneous group of diseases of the myocardium associated with mechanical and/or electrical dysfunction that usually (but not invariably) exhibit inappropriate ventricular hypertrophy or dilation and are due to a variety of causes that frequently are genetic. Cardiomyopathies either are confined to the heart or are part of generalized systemic disorders, often leading to cardiovascular death or progressive heart failure-related disability.” Maron, BJ. Et al. Circulation. 2006; 113: 1807-1816.
That what is not… • Disease entities NOT included in current definition of cardiomyopathy (direct consequence of other cardiovascular abnormalities): • Ischemic Heart Disease • Valvular obstruction and Insufficiency • Hypertensive Heart Disease (poorly defined) • Congenital Heart Disease • Metastatic and primary intracavitary or intramyocardial cardiac tumors Maron, BJ. Et al. Circulation. 2006; 113: 1807-1816.
That what IS… • Primary Cardiomyopathies Maron, BJ. Et al. Circulation. 2006; 113: 1807-1816.
Secondary Cardiomyopathies • Secondary Cardiomyopathies (“specific cardiomyopathies”) • Infiltrative • Storage Diseases • Toxic injury, Cancer Therapy • Endomyocardial Disease • Inflammatory (Sarcoid) • Endocrinopathies • Cardiofacial • Rheumatologic Disease (Autoimmune) • Muscular Dystrophies • Nutritional/Electrolyte Maron, BJ. Et al. Circulation. 2006; 113: 1807-1816.
Work-up/Evaluation • History & Physical Examination • Biomarkers – May be elevated in myocarditis or acute injury • EKG • Echocardiogram • Segmental vs. Global wall abnormalities, chamber size, RV function • MRI • Distinguish ischemic from non-ischemic • Biopsy (Class IIb) • unexplained new-onset heart failure <2 weeks with normal size/dilated LV with hemodynamic compromise • Unexplained new-onset heart failure 2 weeks to 3 months with dilation and new arrhythmia or block
The Genetic Cardiomyopathies: Hypertrophic Cardiomyopathy
HCM Facts • Autosomal Dominant (1:500 phenotypic expression by echo) • Most common cause of SCD in young • Common cause of HF disability in all ages • Diagnosis by 2-D Echo or MRI after clinical suspicion (personal or family history) • Differentiate from physiologic athletic heart
Patient Presentation • Hypertrophy of myocardium (20-40 mm), usually in basal to mid-ventricular septum • Leads to subaortic obstruction (20-40% at rest, majority during stress) – worsened with decreased preload, decreased afterload, or increased contractility • Anterior mitral leaflet may contact the ventricular septum resulting in “systolic anterior motion” • Mitral regurgitation • Dyspnea or Pre-Syncope/ Syncope • Small-normal LV cavity size – Diastolic dysfunction • Increased left atrial pressure – Dyspnea with exertion • Myocardial ischemia -- Angina • Arrhythmia, Sudden Cardiac Death (1% per year) • Autonomic Dysfunction (25%)
HCM Physical Exam • Palpable double apical impulse – Large atrial kick, sustained LV impulse • Increased JVP with prominent “a wave” • Carotid with rapid upstroke with “bifid” • Murmur increase with maneuvers that drop LVED volume • Valsalva, pure vasodilators, Dehydration, decreased venous return • Decreases with squatting • S3 and S4 gallops common
HCM Pathophysiology • 11 identified mutant genes (beta-myosin heavy chain, myosin-binding protein C, et al.) and >400 individual mutations • Mutations alter sarcomeric function • Lead to hypertrophy and fibrosis • Myocardial diarray • Thrombosis and obliteration of small vessels • Other genetic diseases may mimic HCM • Mitochondrial derangements
Hypertrophic CM Screening • Adult family members of HCM patients should get surveillance echo every 5 years • Adolescents every 12-18 months • Genetic testing only 50% accurate
Management of HCM • Avoid dehydration • Avoid competitive athletics or stenuous activity • Pure vasodilators, high-dose diuretics, positive inotropes should be avoided • First-line therapy – beta blockers • Non-dihydropyridine Ca channel blockers • Septal myectomy or alcohol septal ablation for disabling effort related symptoms • ICD for patient’s with hx of cardiac arrest or VT • Also for patient’s with 2 of following: +Fam hx, syncope in young, NSVT episodes, >3 cm hypertrophy, autonomic dysfxn
A 42 y/o woman comes to the office for evaluation of progressive angina and dyspnea on exertion that she has noticed for the past 6 months. She has no history of cardiovascular disease, other than a longstanding murmur. She has never smoked, has no family history of CAD, does not have DM or HTN, and has normal Lipids. On phyical examination, BP 112/70, HR 86, with regular rhythm; JVP normal; carotid upstorkes are brisk without bruits; and lung fields are clear. Cardiac examination shows normal S1 and S2. An S4 is also noted. She has a grade II/VI late-peaking systolic ejection murmur that increased with the strain phase of Valsalva maneuver as well as when she rises from squatting to standing. The apical impulse is bifid. The abdomen and extrmities appear normal. • Chest radiography shows mild increase in pulmonary vascularity. Heart normal size. ECG shows LVG with deep T-wave inversions in precordial leads. Echocardiogram shows asymmetric septal hypertrophy, with maximum septal thickness of 22 mm. Significant systolic anterior motion of the mitral valve is noted and causes moderate mitral regurgitation. The patient has a left ventricular outflow tract obstruction of 64 mm Hg. • Which of the following is best initial management of this patient’s condition? • A. Isosorbide mononitrate 30 mg/d • B. Lisinopril 5 mg/d • C. Metoprolol 25 mg twice a day • D. Furosemide, 40 mg twice a day • E. Sustaine-release nifedipine, 60 mg/d
The Genetic Cardiomyopathies: Arrythmogenic RV Dysplasia
Arrhythmogenic RV Dysplasia • Autosomal dominant with incomplete penetrance: 1:5000 phenotypic expression • RV predominantly involved with myocyte loss with regional fatty of fibrofatty tissue replacement • LV involvement in 75% of patients • Presents with ventricular tachyarrhthmia • Most common cause of sudden death in competitive athletes in Italy
AVRD Diagnosis • Diagnosis based on: • Arrhythmia, syncope, or cardiac arrest • Global or segmental chamber dilation or wall motion abnormalities (usually in RV) • Diagnostic Testing: • ECG (T wave inversion in V1-V3, RBBB) • Echo, Cardiac MRI, Cardiac CT, and RV angiography • Endomyocardial biopsy
The Genetic Cardiomyopathies: Left Ventricular Noncompaction
LV Noncompaction • Distinctive “spongy” appearance of LV myocardium • Usually involves distal (apical) portion of LV chamber • Results from arrest in normal embryogenesis in both familial and nonfamilial forms • Diagnosed by 2D echo, MRI or LV angiography • Associated with HF, thromboemboli, arrythmia, and sudden death
The Genetic Cardiomyopathies: Ion Channelopathies
Ion Channelopathies • LQT Syndrome • Risk for torsade des pointes, syncope, and sudden cardiac death • Variable phenotypic expression • Jervell & Lange-Nielson syndrome • Associated with deafness • Autosomal recessive • 2 genes that code for slow potassium channel • Romano-Ward syndrome • More common autosomal dominant • 8 genes may have mutations (6 for K channels, 1 for Na channel, 1 for ankyrin)
Ion Channelopathies • Brugada Syndrome • First described in 1992 • Sudden cardiac death in young people • EKG with RBBB and coved ST-segment elevation in V1-V3 • If concealed can be unmasked with Class I antiarrythmics • Linked to mutations in cardiac sodium channel gene (LQT3) • Short QT Syndrome • Sudden cardiac death from VT/fibrillation • Tall peaked T waves as with hyperkalemia
Ion Channelopathies • Catecholaminergic Polymorphic Ventricular Tachycardia • Syncope, Sudden death, polymorphic VT triggered by vigorous exertion or emotion • Normal resting ECG • Autosomal dominant form linked to RYR2 gene which codes for “large ryanodine receptor protein” that regulates calcium • Ideopathic Ventricular Fibrillation
Mixed Cardiomyopathies: Dilated Cardiomyopathy
Dilated Cardiomyopathy • Common with prevalence of 1:2500 usually in 3rd to 4th decade with 3:1 male to female ratio • Most common cause of heart transplant • Ventricular enlargement, systolic dysfunction, and normal LV thickness • Diagnosis by 2D Echo • Progressive HF, arrhythmia, heart block, thromboembolism, sudden death
DCM Causes • Both genetic and acquired • Infectious agents (viral, bacterial, fungal, myobacterial, parastitic) • Toxins (alcohol, chemo/doxorubicin) • Autoimmune • Post-viral “Barney Clark’s Disease • Dermatomyositis/Connective Tissue Disease • Endocrinopathies (Pheo, Acromegally) • Neuromuscular disease (muscular dystrophy) • Infiltrative Diseases (hemochromatosis, sarcoid) • Mitochondrial defects • Metabolic/Nutritional • Familial (20-35% of cases)
Mixed Cardiomyopathies: Restrictive Cardiomyopathy
Restrictive Cardiomyopathy • Increased stiffness of myocardium • Impaired ventricular filling • Normal or reduced diastolic volume • Normal or near-normal systolic function • Right-sided HF symptoms (JVD, edema, ascites) more than left-sided symptoms
Pathogenesis of RCM • Pressure in walls of ventricle rise precipitously with minimal increase in volume • Early diastolic filling of ventricle • Deep and early decline in ventricular pressure • Rapid rise to plateau in early diastole (square root)
Restrictive CM vs. Constrictive Pericarditis • Must distinguish from constrictive pericarditis • Kussmaul’s (CP) • Rapid y-descent more common (CP) • LVEDP usually equal to RVEDP (CP) • Increased RV systolic velocity and decreased LV systolic velocity with inspiration (CP)
Etiologies • Idiopathic RCM/ Primary RCM • Amyloidosis • Infiltrative/Storage Disease • Endomyocardial Fibrosis/ Eosinophilic Disease
Primary Restrictive Cardiomyopathy • Rare • Either sporadic and familial forms • Mild to mod increase in cardiac weight with patchy interstitial fibrosis • Normal or decreased volume of ventricles, normal thickness but impaired ventricular filling with restrictive physiology • Normal systolic function • Biatrial enlargement with thrombi in atrial appendages common (1/3 of patients) • May require permanent pacing
Treatment of Restrictive Disease • Diuretics with caution (preload dependence) • Treat atrial fibrillation (rhythm or rate) • Chronotropic agents may worsen failure -- Fixed stroke volume • Pacemaker • Oral anticoagulation • Heart transplantation
Acquired Cardiomyopathies: Myocarditis
Myocarditis • Diagnosed as DCM over weeks to months • Slight male predominance • Symptoms range from fatigue, DOE, palpitations, precordial chest pain and syncope • Often associated with viral prodrome • Commonly associated with myopericarditis • Most resolve with few short-term sequelae over one to six months • Important cause of sudden death Cooper, LT. NEJM. 2009; 360:1526-1538.
Myocarditis Infectious Causes • Viral & Post-viral • Coxsackievirus B – 1950’s through 1990’s • Adenovirus – late 1990’s • Parvovirus B19 & other viruses – past 5 years • Hepatitis C • Less commonly: Epstein-Barr virus, CMV, HHV-6 • Borrelia burgdorferi (Lyme) • Transient/permanent heart block or arryhthmia • Coinfection with ehrlichia or babesia • Trypanosoma cruzi (South America) • With RBBB or LAFB (arryhthmia or heart block in 10-20%) • Left ventricular apical aneurysm, diffuse or regional • HIV – 50% or more of HIV patients on autopsy Cooper, LT. NEJM. 2009; 360:1526-1538.
Myocarditis Variants • Hypersensitivity Myocarditis -- Rash, fever, eosinophilia after medications -- Anticonvulsants, antibiotics, antipsychotics • Also seen with Churg-Strauss, Loffler’s endomyocardial fibrosis, cancer and parasitic infections • May see valvular fibrosis, CHF, and endocardial thrombi • May need treatment with corticosteroids • Giant-cell myocarditis -- DCM with thymoma, autoimmune disorder, VT, or heart block • Multinucleated giant cells and eosinophils • High need for Cardiac Transplant • Sarcoid myocarditis • Evidence of Granuloma formation • Acute Rheumatic Fever Cooper, LT. NEJM. 2009; 360:1526-1538.
Myocarditis Treatment • Myocarditis Treatment Trial showed no benefit to prednisolone plus cyclosporine or azathioprine vs. placebo for biopsy-proven lymphocytic myocarditis. • IMAC (Immune Modulation for Acute Cardiomyopathy) showed no benefit of IVIG over usual care in LV fxn Murphy, JG, & Lloyd, MA. Mayo Clinic Concise Textbook, 3rd Ed. 2007.
Acquired Cardiomyopathies: Others
Tako-Tsubo Cardiomyopathy • Acute but rapidly reversible LV systolic dysfunction • No atherosclerotic CAD • Triggered by profound psychological stress • Typically seen in older women • “apical ballooning” with basal LV hypercontractile
Peripartum Cardiomyopathy • Rare • Dilated Cardiomyopathy with impaired LV function • Seen in 3rd trimester or first 5 months postpartum • More frequently in obese, multiparous women >30, with preeclampsia • 50% with complete recovery in 6 months
A 35 y/o woman who is 39 weeks pregnant presents with progressive dyspnea. She was previously asymptomatic and has no history of cardiovascular disease. This pregnancy is her first. Physical examination shows a jugular venous pressure of 13 cm H20, a diffuse apical impulse, and an apical systolic murmur. S3 and S4 are noted at the apex. Crackles are noted in both lungs. An electrocardiogram shows sinus tachycardia, but is otherwise normal. • Base on this patient’s findings, which of the following is the most likely diagnosis? • A. Severe aortic valve stenosis • B. Severe tricuspid valve regurgitation • C. Atrial Septal Defect • D. Peripartum cardiomyopathy • E. Pulmonary embolism
Others • Tachycardia Induced Cardiomyopathy • Follows prolonged periods of SVT or VT • May mimic idiopathic DCM • Systolic function improves without impairment after tachycardia treated • Alcohol induced dilated cardiomyopathy • Reversible on cessation of alcohol intake
Secondary Cardiomyopathies: Infiltrative and Storage Diseases
Amyloid • Usually presents with hypertrophy, angina, and “restrictive physiology” (associated with 55% mortality) • May see thrombi in LAA • Myocardial tissue damaged and replaced with infiltrative interstitial deposits • “Scintillating granular sparkling” • Conduction abnormalities • Normal to Low voltage EKG • Etiologies • Primary– Caused by deposition of immunoglobulin light chains from plasma cells, as in multiple myeloma • Secondary – less commonly involving heart; result of inflammatory or rheumatic disease • Familial
Other Infiltrative CMs • Usually present as Restrictive Cardiomyopathies • In wall, valves, or coronary arteries • Gaucher Disease – Glucocerebroside • Hurler’s Disease -- Mucopolysaccharide • Hunter’s Disease -- Mucopolysaccharide
Storage Diseases • Hemochromatosis • Walls not thickened • Improvement in function with treatment • Fabry-Anderson Disease • Glycogen storage disease (Pompe, type II) • Niemann-Pick disease