Understanding the Excretory System: Functions, Organs, and Processes
440 likes | 578 Views
The excretory system plays a crucial role in maintaining homeostasis by regulating the internal environment of the body and eliminating metabolic waste products. Key organs involved includes the kidneys, lungs, and skin. The kidneys filter excess water, urea, and salts from the bloodstream, while the lungs excrete carbon dioxide. The skin helps eliminate waste through sweat. This system involves complex processes such as filtration, reabsorption, secretion, and excretion, ultimately producing urine that contains waste for removal from the body.

Understanding the Excretory System: Functions, Organs, and Processes
E N D
Presentation Transcript
Purpose • Contributes to homeostasis • Regulates internal environment by eliminating metabolic waste products: • Volume • Electrolyte composition • pH
Waste Products • Some are metabolic • E.g. Water, salts, CO2, and urea • Urea is a toxic compound that is produced when amino acids are used for energy (contain nitrogen).
Three Organs Kidneys Lungs Skin
1. Kidneys • Main organs of excretion. • Remove excess water, urea & other excess mineral wastes from the body. • Act as filters to remove wastes that are collected and transported by the blood. • E.g. Surplus in water or electrolyte (salt) in blood = kidneys excrete in the urine.
2. Lungs • Every time we exhale, we get rid of small amounts of water vapor and CO2. • CO2 is the waste product of cells that must be removed from the body so you can take in oxygen.
3. Skin • Excretes excess water, salts, and small amounts of urea through sweating.
The Urinary System • Made up of: • Left and right kidneys • Ureters • Bladder • Urethra • Removes wastes and toxins from the blood and produces urine. • Urine: made of water, excess salts, & urea
Kidney Structure • Bean shaped • Either side of the spinal column, near lower back • Size of your fist • Each are attached to a renal artery & a renal vein
Renal Vessels • Renal artery – blood from aorta • unfiltered and full of bodily wastes • Renal vein – filtered blood http://www.yoursurgery.com/ProcedureDetails.cfm?BR=1&Proc=69
Ureters and Bladder • Ureter leaves each kidney with fluid containing excess water, salts, urea & other waste products • Ureters lead to the bladder; liquid wastes are deposited/stored here • Expulsion of wastes controlled by specific sphincter muscles – voluntary control. http://www.etsy.com/listing/70476539/kidneys-crochet-plush-with-ureters-and http://www.emedicinehealth.com/prolapsed_bladder/page17_em.htm
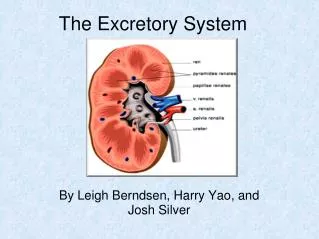
Kidney Regions • 2 distinct regions: • Inner Part: Renal Medulla • Outer Part: Renal Cortex
Nephrons • In the renal cortex • Working parts of the kidney • Each acts as an individual unit of filtration • About 1 million nephrons per kidney
http://www.agefotostock.com/age/ingles/enam01b.asp?foto=13173541&key1=&foto_clave=BSI-3555309&famp=1http://www.agefotostock.com/age/ingles/enam01b.asp?foto=13173541&key1=&foto_clave=BSI-3555309&famp=1
FYI The kidneys receive approximately 10% of the blood that is pumped out of our heart every minute. Adult kidneys filter approx. 180L of blood daily.
1. Filtration - Bowman’s Capsule (BC) • -Hollow bulb surrounding ball of capillaries (Glomerulus) http://www.pitt.edu/~anat/Abdomen/Kidneys/Kidneys.htm
http://www.as.miami.edu/chemistry/2086/chap26/chapter%2026-new_part1.htmhttp://www.as.miami.edu/chemistry/2086/chap26/chapter%2026-new_part1.htm
Filtration (cont’d) • Blood enters via renal artery • Blood filters through permeable walls under pressure • Filtered materials (urea, glucose, salts, & some vitamins) are called filtrates. http://physrev.physiology.org/content/88/2/451
Filtration (cont’d) • Platelets, red and white blood cells remain in the blood (too large to pass) • Adult kidneys filter approx. 180L of blood daily.
2. Re-Absorption - Tubules • Some filtrates reabsorbed by active transport • valuable & can’t be lost • Water returns to blood through osmosis • 99% of the water that is filtered out of BC is reabsorbed into your blood
3. Secretion - Tubules • Excess fluid leaves BC & enters tubules • URINE. • First part – Proximal Convoluted Tubule (PCT). • carries fluid down into the Loop of Henle (LH).
3. Secretion - Tubules • Urine concentrated in the tubule at the LH. • i.e.water reabsorbed • Urine moves up Distal Convoluted Tubule (DCT) & meets ureter
4. Excretion • Purified blood returns to the body through the renal vein, which runs to the Inferior Vena Cava • Urine moves from the nephrons to ureters and goes to the bladder for storage • Once urine is ready to leave the body, the urine will be expelled through the urethra. • Stretch receptors in bladder
Recap: http://www.as.miami.edu/chemistry/2086/chap26/chapter%2026-new_part1.htm
http://www.colorado.edu/intphys/iphy3410saul/outlines08fall/nephron.gifhttp://www.colorado.edu/intphys/iphy3410saul/outlines08fall/nephron.gif
Kidney Failure • You have two kidneys in the body located on either side of the spine and extend a little below the ribs. • Your kidneys are bean-shaped organs and is about the size of a fist. • The kidneys receive approximately 10% of the blood that is pumped out of our heart every minute.
Your kidneys are responsible for the following: • Regulate fluids • Balance chemicals • Remove wastes • Secrete hormones
Condition Explanation: • Progressive in nature • Anemia possible – lack of iron • Malnutrition (lack of appetite) • Decrease well-being • Increased risk for heart disease
Toxins build up in blood • Weight gain (excess fluids, swollen ankles, puffiness) • Fluid imbalances – dizziness – nausea
Treatment Options: • General • Limit fluid intake, high carb, low protein, low potassium diet • Too much potassium can cause irregular heartbeat
Haemodialysis • Most common method • Use of a machine (size of dishwasher) – blood flow through special filter to remove and filter wastes • Clean blood returned to body • Strict schedule – 3 times a week for 3 to 5 hours each time
Side effects • Less energy • Loss of time • Once a month blood is tested to see how effective dialysis is – may not work forever!
Peritoneal Dialysis • Removes extra water, wastes, and chemicals • Cleansing solution passed through catheter into abdomen • After a couple of hours the solution is drained • Does not require a machine • Strict diet • More recent advances, more flexibility (done at home)
Kidney Transplantation • Receive a healthy kidney from a living donor or a recently deceased donor • When effective recovers quality of health AND life • Yields longer life expectancy • Could be long waiting lists (shortage of donors) • Typical Surgery Risks (bleeding, infection, etc.) • Anti-rejection medications after surgery – may weaken immune system • Risk of rejection (body doesn’t accept kidney)