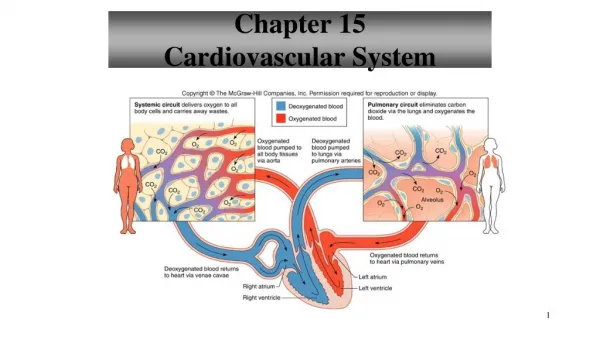
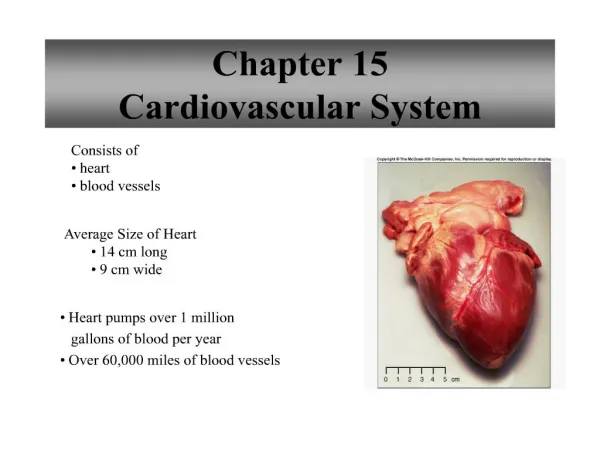
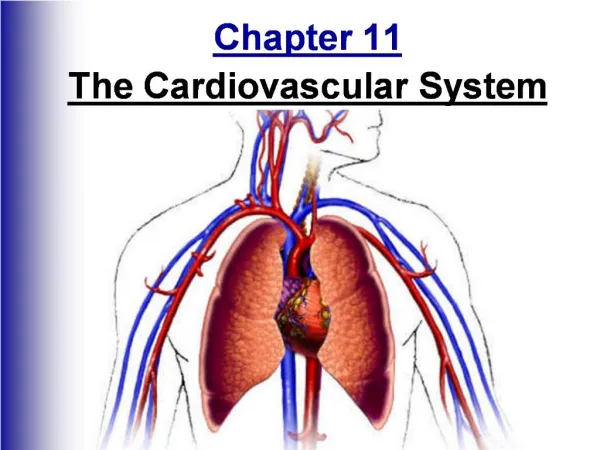
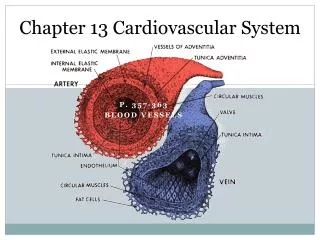
Chapter 13 Cardiovascular System
Chapter 13 Cardiovascular System. 13.3. 13.3. Heart Actions. Heart Actions. Systole = when a heart chamber contracts Diastole = when a heart chamber relaxes Cardiac Cycle = constitutes a complete heartbeat Atrial systole and ventricular diastole

Chapter 13 Cardiovascular System
E N D
Presentation Transcript
13.3 Heart Actions
Heart Actions • Systole = when a heart chamber contracts • Diastole= when a heart chamber relaxes • Cardiac Cycle = constitutes a complete heartbeat • Atrial systole and ventricular diastole • Ventricular systole and atrial diastole • Both the atrial and ventricular diastole
Cardiac Cycle • Important: fluids always move from high to low pressure • A-V valves open and blood moves through the heart mostly due to pressure changes • 70% of blood moves from the right atria to the right ventricle before atrial contraction • 30% is pushed through by contraction of the atria
Cardiac Cycle • Pressure rises in the ventricle as it contracts • Causes the A-V valves to close • Contraction of papillary muscles attached to cordaetendineae prevent the cusps from going back into atria • Now, low pressure in the atria causes it to fill with blood from veins
Cardiac Cycle • Pressure builds as the ventricle contracts, causing the semilunarvalves to open • Blood flows from the ventricle to the arteries • Pressure drops in the ventricle as blood leaves and it begins to relax • The semilunar valves close when the pressure in the arteries is greater than that in the ventricles
Heart Sounds • Lubb-dupp due to the vibrations in heart tissues associated with the closing of valves • Lubb – A-V valves closing • Dupp – Pulmonary and aortic valves closing
Cardiac Muscle Fibers • Functions like skeletal muscle fibers, except they connect in branching networks • Stimulation to any part of the network sends impulses through the heart • Causes the heart to contract as a unit
Cardiac Muscle Fibers • Functional syncytium – a mass of merging cells that function as a unit • 2 in the heart • In atrial walls • In ventricular walls • They are separated by the heart’s fibrous skeleton, except for a small area in the right atrial floor (connected by fibers of the cardiac conduction system)
Cardiac Conduction System • Cardiac conduction system – Special muscle fibers that initiate and distribute impulses throughout the myocardium, • Coordinates the events of the cardiac cycle
Cardiac Conduction System • Sinoatrial (S-A) node – specialized tissue in the wall of the right atrium that initiates the cardiac cycle • Pacemaker (can reach threshold 70-80 times per min) • Needs no stimulation from nerve fibers • Travels to atrialsyncytium (causes atria to contract) • Then to junctional fibers (delay impulse transmission)
Cardiac Conduction System • Atrioventricular (A-V) node – Specialized mass of cardiac muscle fibers in the interatrial septum of heart • Transmits impulses from the S-A node to the A-V bundle • A-V bundle (bundle of His) – specialized fibers that conduct impulses from the A-V node to the ventricular muscle of the heart • Divides to form the right and left bundle branches
Cardiac Conduction System • Purkinje fibers – conduct impulses from the bundle branches to the ventricular syncytium • The ventricle contacts with a twisting motion, squeezing blood out of its chambers and into the aorta and pulmonary trunk • Muscle fibers form irregular whorls
Electrocardiogram • Electrocardiogram (ECG) – a recording of the electrical activity associated with the heartbeat • Changes can be detected on the surface of the body because electrical currents can conduct through body fluids
Electrocardiogram • Waves are created on the electrocardiogram which correspond to electrical changes • P wave – depolarization of the atrial fibers and contraction of the atria • QRS complex – depolarization of the ventricular fibers • T wave – ventricular muscle fibers repolarize • Between cycles, it stays along the baseline • Repolarization of the atrial fibers is obscured by the QRS complex
Regulation of the Cardiac Cycle • Volume of blood pumped changes to accommodate cellular requirements • Strenuous exercise = requires more blood • S-A node changes rate as a response to sympathetic and parasympathetic nerve fibers
Regulation of the Cardiac Cycle • Parasympathetic stimulation = heart rate decreases • Continuously “braking” heart action • Can change heart rate by either increasing or decreasing impulses • Sympathetic stimulation = increases heart rate and force of myocardial contractions
Regulation of the Cardiac Cycle • Baroreceptor reflexes involving the cardiac control center of the medulla oblongata maintain the balance between sympathetic and parasympathetic stimulation • Baroreceptors detect blood pressure and sends that info to the brain which sends a message to the heart
Regulation of the Cardiac Cycle • The cerebrum and hypothalamus can also influence it • Causes fainting following emotional upset • Increases heart rate during anxiety • Temperature • Increased temperature increases heart rate • Colder temperatures decrease heart rate
Regulation of the Cardiac Cycle • Concentration of ions • Hyperkalemia (too much K+) decreases the rate and force of contractions • Hypokalemia (too little K+) produces a potentially life-threatening abnormal heart rhythm • Hypercalcemia (too much Ca+) increases heart actions, posing the danger that the heart will contract for an abnormally long time • Hypocalcemia (to little Ca+) depresses heart action