Cerebral Air Embolism and Stroke Following PICC: A Case Report
A case study on a patient who developed status epilepticus and stroke due to cerebral air emboli following PICC placement, leading to severe neurological impairment and poor outcome.

Cerebral Air Embolism and Stroke Following PICC: A Case Report
E N D
Presentation Transcript
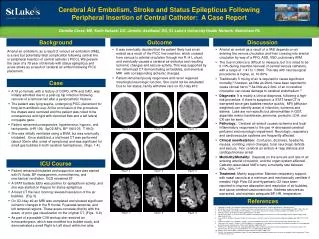
Cerebral Air Embolism, Stroke and Status Epilepticus Following Peripheral Insertion of Central Catheter: A Case Report References Background Patient remained intubated and supportive care was started with IV fluids, BP management, normothermia, and mechanical ventilation. GCS remained 6T A STAT bedside EEG was positive for epileptiform activity, and she was started on Keppra for status epilepticus A head CT the next morning revealed resolution of the air bubbles. (Fig. 5) On ICU day #2 an MRI was completed and showed significant ischemic changes in the R frontal, R parietal-temporal, and left temporal regions. These areas correlate directly with the areas of prior gas visualization on the original CT. (Figs. 6-8) As part of a possible CVA workup she received an echocardiogram, which was modified to a bubble study, and demonstrated a small Right to Left shunt within her atria. ICU Course Outcome A 79 yofemale, with a history of COPD, HTN and CAD, was initially admitted due to a post-op hip infection following removal of a femoral nail after a periprosthetic fracture. The patient was lying supine, undergoing PICC placement for long-term antibiotic use. At the conclusion of the procedure the drapes were removed and the patient was noted to be unresponsive and rigid with clenched fists and a left lateral conjugate gaze. Patient remained unresponsive, hypertensive, hypoxic, and tachycardic. (HR 109, SpO2 85%, BP 198/105, T 99.0). She was initially ventilated using a BVM, but was eventually intubated. Once stabilized, a stat head CT was performed (about 30min after onset of symptoms) and was significant for small gas bubbles in both cerebral hemispheres. (Figs. 1-4). Case Arterial air embolism, as a result of venous air embolism (VAE), is a rare but potentially fatal complication following central line or peripheral insertion of central catheter ( PICC). We present the case of a 79 year old female with status epilepticus and acute stroke as a result of cerebral air emboli following PICC placement. Danielle Cross, MD, Keith Habeeb, DO, Jennifer Axelband, DO, St. Luke’s University Health Network, Bethlehem PA It was eventually decided that the patient likely had an air emboli as a result of the PICC line insertion, which crossed from venous to arterial circulation through her R L shunt, and eventually caused a cerebral air embolus and resulting ischemic changes and seizure activity. This was supported by her initial head CT demonstrating air bubbles, and eventual MRI with corresponding ischemic changes. Patient remained poorly responsive and never regained meaningful neurologic function. She could not be extubated. Due to her status, family withdrew care on ICU day #10. Discussion Arterial air emboli as a result of a VAE depends on air entering the venous circulation and then crossing into arterial circulation by way of a PFO, ASD, VSD, pulmonary AVM. The true incidence is difficult to measure, but it is noted to be 0.13% during insertion/removal of central venous catheters, with a range of 1:47 to 1:3000. The rate with neurosurgical procedures is higher, at 10-80%. Traditionally 5 mL/kg of air is required to cause significant mortality,2however, as little as 20mL have been reported to cause clinical harm.10As little as 2-3mL of air in cerebral circulation can cause damage to cerebral endothelium.11 Diagnosis: It is mainly a clinical diagnosis, following a high-risk procedure. If there is suspicion, a STAT head CT is warranted since gas bubbles resolve quickly. MRI (diffusion weighted) can identify areas of infarction, ischemia and edema. Labs are non-specific but abnormalities in GGT, aspartate amino-transferase, ammonia, prolactin, LDH, and CK can be seen. Pathology: Cerebral air emboli causes ischemia and local inflammatory responses to the gas decreased cerebral perfusion and neurologic impairment. Neurologic, respiratory and cardiovascular systems are frequently affected. Clinical manifestation: Confusion, dizziness, headache, nausea, vomiting, vision changes, focal neurologic deficits and seizure. Non cerebral air emboli resp distress and cardiopulmonary arrest Morbidity/Mortality: Depends on the amount and rate of air entering arterial circulation, and the organ system affected. Catheter-associated VAE’s carry a mortality rate between 23%- 30%.3,4,8 Treatment: Mainly supportive. Maintain respiratory support, with nasal cannula at a minimum and mechanically ventilate if needed. High Flow O2 and Hyperbaric O2 have been reported to improve absorption and resolution of air bubbles, and cause cerebral vasoconstriction. Address seizures as warranted, and maintain adequate BP, HR, temperature. OrebaughS.Venous air embolism: clinical and experimental considerations. Critical Care Medicine. 1992;20(8):1169 MirskiMA, Lele AV, Fitzsimmons L, Toung TJ. Dianosis and treatment of vascular air embolism. Anesthesiology. Jan 2007; 106(1):164-167. SvriS, Woods WP, van Heerden PV. Air embolism- a case series and review. Critical Care Resuscitation. Dec 2004;6 (4): 271-276. Natal BL. Venous Air Embolism. Medscape Reference. Jan 2014. Van Hulst, RA, Klein J, Lachmann B. Gas Embolism: Pathophysiology and Treatment. Clinical Physiology and Functional Imaging. Sept 2003;23(5):237-246. VeselyTM. Air Embolism during instertion of central venous catheters. Journal of Vascular Interventional Radiology. Nov 2001;12(11):1291-1295. PalmonSC, Moore LE, Lundberg J, Toung T. Venous Air embolism: A review. Journal Clinical Anesth. May 1997;9(3)251-257. HeckmannJG, Lang CJ, Kindler K, Huk W, Erbguth FJ, Neundorfer B. Neurologic manifestations of cerebral air embolism as a complication of central venous catheterization. Critical Care Medicine. 2000;28(5):1621. PronovostPJ, Wu AW, Sexton JB. Acute decompensation after removing a central line: practical approaches to increasing safety in the intensive care unit. Annals of Internal Medicine. Jun 15, 2004;140(12):1025-1033. Moon R. Air or Gas Embolis. Hyperbaric Oxygen Committee Report. 2003;5-10. Ho AM. Is emergency thoracotomy always the most appropriate immediate intervention for systemic air embolism after lung trauma? Chest. Jul 1999;116(1):234-237. Figure 1 Figure 2 Figure 3 Figure 4 Figure 5 Figure 6 Figure 7 Figure 8 Figure 9
HeckmannJG, Lang CJ, Kindler K, Huk W, Erbguth FJ, Neundorfer B. Neurologic manifestations of cerebral air embolism as a complication of central venous catheterization. Critical Care Medicine. 2000;28(5):1621. http://www.ncbi.nlm.nih.gov/pubmed/10834723