Hypersensitivity
Hypersensitivity. A damage to the host, mediated by pre-existing immunity to self or foreign antigen. Dr. Sudheer Kher. Learning objectives. 1. C lassify the hypersensitivity reactions 2. List the diseases associated with hypersensitivity reactions

Hypersensitivity
E N D
Presentation Transcript
Hypersensitivity A damage to the host, mediated by pre-existing immunity to self or foreign antigen. Dr. SudheerKher Kher
Learning objectives 1. Classify the hypersensitivity reactions 2. List the diseases associated with hypersensitivity reactions 3. Describe the mechanisms of damage in hypersensitivity reactions 4. List the methods for diagnosing conditions due to hypersensitivity 5. Describe the modes of treating diseases due to hypersensitivity and their rationale Kher
What is hypersensitivity? • Injurious consequences in the sensitized host, following contact with specific antigen • Deals with injurious aspect of heightened and exaggerated immune response leading to tissue damage, disease or even death • Concerned with what happens to the host rather than what happens to the antigen. Kher
Musts for Hypersensitivity • Contact with allergen • Sensitizing/priming dose • Induction of AMI/CMI • Shocking dose Kher
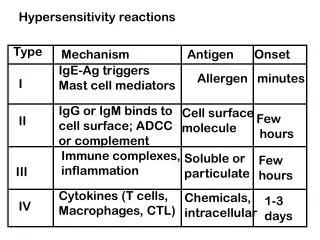
Classification : Hypersensitivity reactions • Immediate hypersensitivity • Anaphylaxis • Atopy • Antibody mediated cell damage • Arthus phenomenon/reaction • Serum sickness • Delayed hypersensitivity • Infection (Tuberculin) type • Contact dermatitis type Type I Type II Type III Type IV Kher
Hypersensitivity Reaction Hypersensitivity or allergy * An immune response results in exaggerated reactions harmful to the host * There are four types of hypersensitivity reactions: Type I, Type II, Type III, Type IV * Types I, II and III are antibody mediated * Type IV is cell mediated
Type-I hypersensitivity The common allergy Kher
Type I: Immediate hypersensitivity * An antigen reacts with cell fixed antibody (Ig E) leading to release of soluble molecules An antigen (allergen) soluble molecules (mediators) * Soluble molecules cause the manifestation of disease * Systemic life threatening; anaphylactic shock * Local atopic allergies; bronchial asthma, hay fever and food allergies
Anaphylaxis * Systemic form of Type I hypersensitivity * Exposure to allergen to which a person is previously sensitized * Allergens: Drugs: penicillin Serum injection : anti-diphtheritic / anti-tetanus serum/ AGGS, Anti snake venum Anesthesia or insect venom * Clinical picture: Shock due to sudden decrease of blood pressure, respiratory distress due to bronchospasm, cyanosis, edema, urticaria * Treatment: corticosteroids injection, epinephrine, antihistamines
Atopy * Local form of type I hypersensitivity * Exposure to certain allergens that induce production of specific Ig E * Allergens : Inhalants: dust mite faeces, tree or pollens, mould spores. Ingestants: milk, egg, fish, chocolate Contactants: wool, nylon, animal fur Drugs: penicillin, salicylates, anesthesia, insect venom * There is a strong familial predisposition to atopic allergy * The predisposition is genetically determined
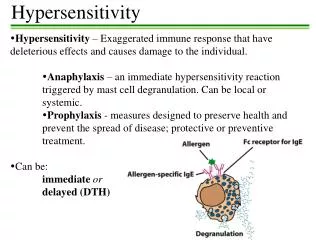
Pathogenic mechanisms * First exposure to allergen Allergen stimulates formation of antibody (Ig E type) Ig E fixes, by its Fc portion to mast cells and basophils * Second exposure to the same allergen It bridges between Ig E molecules fixed to mast cells leading to activation and degranulation of mast cells and release of mediators
B cell IL13 TH2 Newly synthesized mediators Sensitization against allergens and type-I hypersensitivity Histamine, tryptase, kininegenase, ECFA Leukotriene-B4, C4, D4, prostaglandin D, PAF Kher
Type I (Anaphylactic) Reactions Antigens combine with IgE antibodies bound to mast cells and basophils, causing them to undergo degranulation and release several mediators: • Histamine: Dilates and increases permeability of blood vessels (swelling and redness), increases mucus secretion (runny nose), smooth muscle contraction (bronchi). • Prostaglandins: Contraction of smooth muscle of respiratory system and increased mucus secretion. • Leukotrienes: Bronchial spasms. • Anaphylactic shock: Massive drop in blood pressure. Can be fatal in minutes.
Type I Reactions • Humans – • Itching of scalp & tongue, flushing of skin, difficulty in breathing, nausea, vomiting, diarrhea, acute hypotension, loss of consciousness, death (rare) • Causes • Serum therapy, antibiotics, insect stings • Treatment • Adrenalin 0.5 ml (1 in 1000 solution) SC/IM repeated up to 2 ml in 15 min Kher
Pathogenic mechanisms * Three classes of mediators derived from mast cells: 1) Preformed mediators stored in granules (histamine) 2) Newly synthesized mediators: leukotrienes, prostaglandins, platelets activating factor 3) Cytokines produced by activated mast cells, basophils e.g. TNF, IL3, IL-4, IL-5 IL-13, chemokines * These mediators cause: smooth muscle contraction, mucous secretion and bronchial spasm, vasodilatation, vascular permeability and edema
Mechanism of anaphylaxis • Mediators of anaphylaxis – • Primary mediators • Preformed contents of Mast cells & Basophils • Histamine, serotonin, eosinophils chemotactic factor of anaphylaxis (ECF-A), Neutrophil chemotactic factor (NCF), Heparin & various proteolytic enzymes • Secondary mediators – • Newly formed after stimulation by Mast cells, Basophils & other leucocytes • Slow reacting substance of anaphylaxix (SRS-A), Prostaglandins & Platelet activating factors (PAF) Kher
Primary Mediators of Anaphylaxis • Histamine – • Most important vasoactive amine of Human anaphylaxis, formed from histidine found in granules. Released into skin, causes burning & itching. Causes vasodilatation & hyperemia by an axon reflex (Flare) and edema by increasing capillary permeability (Wheal). Induces smooth muscle contraction of diverse tissues & organs. Kher
Primary Mediators of Anaphylaxis • Serotonin (5-HT) –Role in human not clear. • Base derived by decarbolxylation of Tryptophan. • Found in intestinal mucosa, brain & platelets. • Causes smooth muscle contraction, ↑ Vascular permeability & vasoconstriction. • Important in rats & mice. Kher
Primary Mediators of Anaphylaxis • Chemotactic factors – • ECF-A released from mast cell granules are strongly chemotactic for eosinophils. Accounts for high eosinophil counts in many hypersensitivity reactions. • NCF – Attracts neutrophils • Enzymatic mediatores such as proteases & hydrolases are also released from the mast cell granules. Kher
Secondary mediators of anaphylaxis • Prostaglandins & leukotrienes– • Derived from Arachidonic acid formed from the disruption of mast cell membrane, other leucocytes • Lipoxygenase pathway - Leukotrienes • Cycloxygenase pathway - Prostaglandins • One of the family of Leukotrienes is SRS-A(slow reacting substance of anaphylaxis) • Prostaglandins are bronchoconstrictors/broncodilators, affect secretions of mucus glands, platelet adhesion, permeability, dilatation of capillaries & pain threshold. Kher
Secondary mediators of anaphylaxis • Platelet activating factor – PAF • Low mol wt lipid released from basophils • Causes aggregation of platelets and release of their vasoactive amines • Other mediators – • Anaphylatoxin – Released by complement activation • Bradykinin & Other kinins formed from plasma kininigens Kher
Cutaneous anaphylaxis • If small shocking dose is given ID to sensitized host, there is a local wheal & flare reaction (local anaphylaxis). • Used for • Testing for hypersensitivity • Identification of allergens for atopy • Precaution – Keep adrenalin injection ready to combat severe fatal reaction. Kher
Anaphylactoid reaction • Intravenous injection of peptone, trypsin & certain other substances causes clinical reaction like anaphylaxis. • Resemblance due to participation of same chemical mediators. • Difference – Anaphylactoid shock has no immunological basis. It is nonspecific reaction involving activation of complement & release of anaphylatoxin. Kher
Methods of diagnosis 1) History taking for determining the allergen involved 2) Skin tests: Intradermal injection of battery of different allergens A wheal and flare (erythema) develop at the site of allergen to which the person is allergic 3) Determination of total serum Ig E level 4) Determination of specific Ig E levels to the different allergens
Management 1) Avoidance of specific allergen responsible for condition 2) Hyposensitization: Injection gradually increasing doses of extract of allergen - production of Ig G blocking antibody which binds allergen and prevent combination with Ig E - It may induce T cell tolerance 3) Drug Therapy: Corticosteroids injection, epinephrine, antihistamines, leukotriene receptor blockers, Chromolyn sodium inhibits mast cell degranulation
Animation & Quiz http://highered.mcgraw-hill.com/sites/0072556781/student_view0/chapter33/animation_quiz_2.html