THYROID GLAND
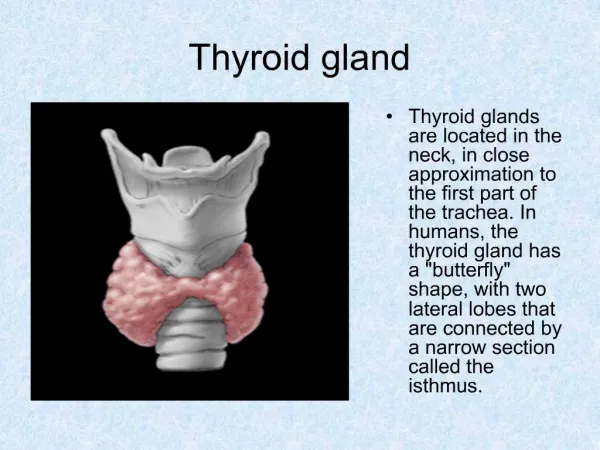
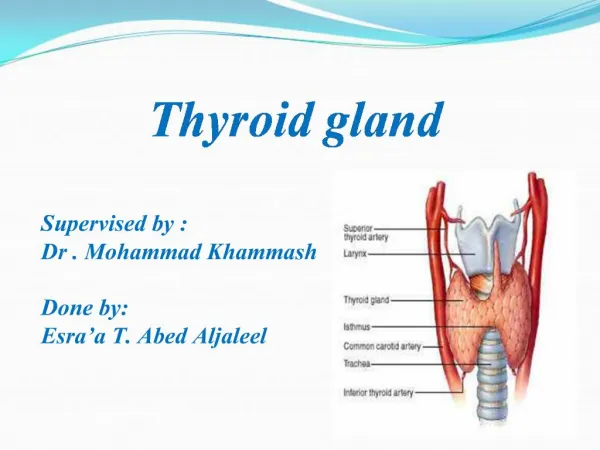
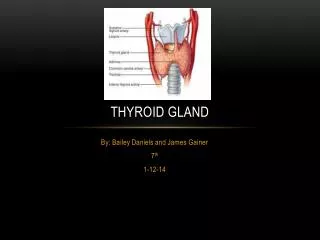
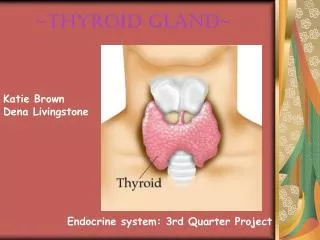
THYROID GLAND. George Liapakis , PhD. The thyroid glad is a butterfly-shaped organ, consisting of two lobes of endocrine tissue . It is located at the front of the neck. It is composed of spherical sacs, the thyroid follicles .

THYROID GLAND
E N D
Presentation Transcript
THYROID GLAND George Liapakis, PhD
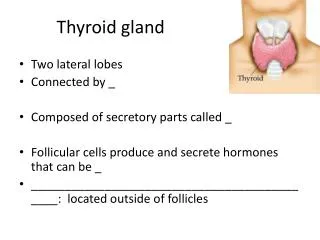
The thyroid glad is a butterfly-shaped organ, consisting of two lobes of endocrine tissue It is located at the front of the neck
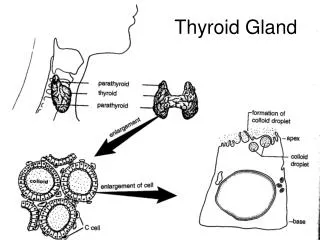
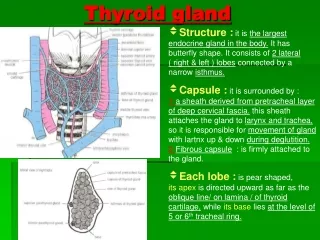
It is composed of spherical sacs, the thyroid follicles. The boundary of the follicles is formed by secretory cells, the follicular cells The follicular cells produce the thyroglobulin The sac is filled with a viscous substance, the colloid. The thyroglobulin in the colloid serves as a storage site for the thyroid hormones
Incorporation of the thyroid hormones into the large glycoprotein, thyroglobulin (Tg) Storage form of thyroid hormones Thyroglobulinis produced in the follicular cells Thyroglobulin is the major constituent of colloid. Follicular cell
Thyroid hormones. Tetraiodothyronine (T4, or thyroxine) Tri-iodothyronine (T3). • They contain tyrosine and iodide • Iodide is the reduced form of iodine (before absorption by intestine) that is obtained from dietary intake (iodized salt)
Thyroid follicles, follicular cells and colloid The colloid stores thethyroid hormones
How are the thyroid hormones synthesized by tyrosine and iodide? • Incorporation of tyrosine into thyroglobulin (Tg) in the follicular cells. • Exit of tyrosine-containing Tg from follicular cells into the colloid(exocytosis) 2 1
The follicular cells capture iodide from the blood (iodide pump) Exit of iodide from follicular cells into the colloid (luminal channel). 3 4
Production of monoiodotyrosine (MIT) within the colloid: Attachment of one iodide to tyrosine of Tg. Production of di-iodotyrosine (DIT)within the colloid: Attachment of two iodides to tyrosine of Tg. 5
6. Coupling of one MIT and one DIT, within the thyroglobulin molecule forms the tri-iodothyronine, or T3. Couplingof two DIT, within the thyroglobulin molecule forms the tetraiodothyronine(T4, or thyroxine). 6
Thyroid hormones remain attached to thyroglobulin (storage form)
Follicular cells engulf(by phagocytosis) a portion of colloid which contains thyroglobulin. Lysosomes of the follicular cells attack the engulfed vesicle and splitthe T3, T4, MIT and DIT from thyroglobulin. 2 1
T3 and T4 are lipophilic and diffuseinto the blood They bind to plasma proteins, which carry them to their target cells 5 4
RECYCLING OF IODIDE Iodide is removedfrom the MIT and DIT (not from T3, T4) by an enzyme Free iodide is recycled by entering(2A) the colloid and participating in the synthesis(2B) ofnew thyroid hormones. 2A 1 2B
Although thyroid gland secretes mostly T4, the T3 is the major biologically active form. • Why? • T3 is 10 times more biologically potentthat T4 • Most of the secreted T4 is converted outside the thyroid gland (in liver and kidneys) into T3, by losing one of its iodides.
Actions of thyroid hormones They increase the body’s overall basal metabolic rate, by regulating the rate of O2 consumption and energy expenditure (they burn calories) They act as sympathomimetics (they mimic the effects of catecholamines): vasoconstriction and increase of the heart rate and force (they increase the responsiveness of tissues to catecholamines, increasing the number of their receptors) They play a crucial role in the normal development of the central nervous system. They are essential for normal growth: they stimulate GH secretion, increase the production of IGF, and promote the effects of GH and IGF on protein synthesis and skeletal growth.
Thyroid-stimulating hormone (TSH) • It stimulates the secretion of thyroid hormones • It is secreted from the anterior pituitary. • It maintains the structural integrity of the thyroid gland. • In the absence of TSH the thyroid decreases in size (atrophy). • In excess stimulation by TSH the thyroid gland increases in size (hypertrophy, hyperplasia).
Regulation of the secretion of TSH Stimulation by the thyrotropin-releasing hormone (TRH): It is released from the hypothalamus and through the portal system goes to the anterior pituitary Inhibition by thyroid hormones by a negative-feedback mechanism, by acting on the anterior pituitary and the hypothalamus.
Abnormalities of thyroid function : DISORDERS Hypothyroidism Deficiency of thyroid hormone secretion Hyperthyroidism Excess of thyroid hormone secretion
Hypothyroidism Inadequate dietary supply of iodine (consumption of iodine, iodized salt) Primary failure of the thyroid gland Atrophy of thyroid gland due to a deficiency of TRH, TSH, or both Reduction in overall metabolic activity: poor tolerance of cold, tendency to gain excessive weight, fatigue. Slow, weak pulse, feel tired. Slow mental responsiveness, such as diminished alertness, slow speech, and poor memory.
Hypothyroidism • Myxedema • Adults • Fluid accumulation in skin: Swollen face, hands, and feet • Cretinism • Hypothyroidism from birth • Dwarfism and mental retardation. • It is preventable if thyroid hormone replacement therapy is started promptly • It is not reversible once it has developed for a few months after birth.
Hyperthyroidism • Graves’ disease • The body (immune system) produces the thyroid-stimulating immunoglobulin(TSI) • TSI, like TSH, stimulates secretion and growth of the thyroid • Unlike TSH, TSI is not subject to negative-feedback inhibition by thyroid hormone. • TSI promotes thyroid secretion without any control.
Graves’ disease Elevated metabolic rate: Loss of weight, mass reduction and weakness Increase of heart rate and strength (palpitations). Irritability, anxiety and poor emotional control. Exophthalmos: the eyes pop out of head due to the accumulation of fluid behind eyes.
Goiter • Enlarged thyroid gland. It looks like a fat neck. • A goiter may appear either in hypothyroidism or in hyperthyroidism. • However it is also possible for a patient to have hypothyroidism or hyperthyroidism without having a goiter. Rule Anything that hyper-stimulates thyroid, will cause goiter. Graves’ disease (TSI production) Increased secretion of TSH from the anterior pituitary
Goiter Hyperthyroidism Tumor in the hypothalamus or the pituitary Excess of secretion of TSH
Goiter Hypothyroidism Failure of thyroid gland or lack of iodine Low circulating levels of thyroid hormones No inhibition of TSH secretion Over-secretion of TSH from pituitary However the thyroid gland is incapable to produce T3 and T4 because it lacks either a critical enzyme or iodine.
SUMMARY Location of the thyroid gland Thyroid follicles: follicular cells, colloid The colloid stores the thyroid hormones Thyroid hormones: Tetraiodothyronine (T4, or thyroxine) and Tri-iodothyronine (T3) Thyroid hormones: They contain tyrosine and iodide Thyroglobulin (Tg): Storage form of thyroid hormones Thyroglobulin is produced in the follicular cells and it is the major constituent of colloid. Synthesis and secretion of thyroid hormones
SUMMARY • T3 is more potent that T4. Conversion of T4 into T3 • Actions of thyroid hormones: Increase of the metabolic rate, sympathomimetic action, development of the central nervous system, growth. • Thyroid-stimulating hormone (TSH): tropic hormone • Regulation of the secretion of TSH: negative-feedback mechanism • Disorders: 1) Hypothyroidism (Myxedema, Cretinism), 2) Hyperthyroidism (Graves’ disease), 3) Goiter
NEXT LECTURE ADRENAL GLANDS