Skeletal System
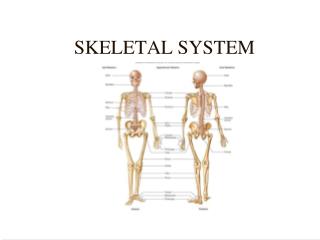
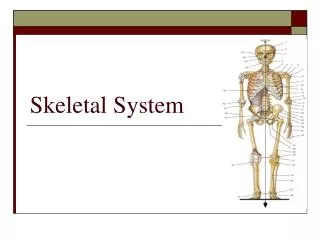
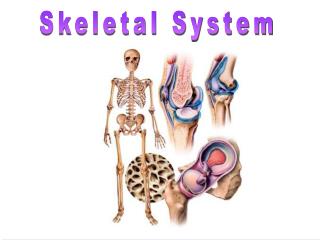
Skeletal System. Chapter 7. The Skeleton. Support Storage Strength Attachment scaffold for tendons, ligaments and muscle Blood cell production. Types of Bone. Long Bones – long, as in the arm (radius, ulna, humerus) and thigh (femur)

Skeletal System
E N D
Presentation Transcript
Skeletal System Chapter 7
The Skeleton • Support • Storage • Strength • Attachment scaffold for tendons, ligaments and muscle • Blood cell production
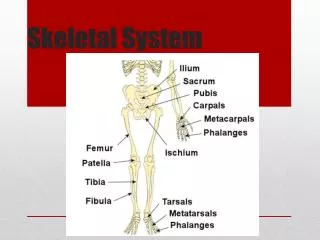
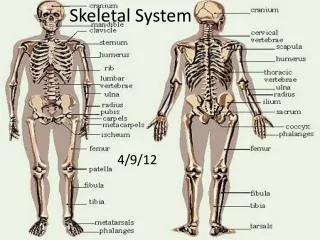
Types of Bone • Long Bones – long, as in the arm (radius, ulna, humerus) and thigh (femur) • Short Bones – cube-like, as in wrists (carpal) and ankles (tarsal) • Flat Bones – plate-like, as in ribs, scapulae, some skull bones (parietal) • Irregular Bones – vertebrae, facial bones • Round or Sesamoid Bones – small, round, reside in tendons and next to joints – Knee cap or patella is an example
Parts of a Long Bone • Epiphysis – wider, thicker region at the ends of long bones. This usually forms a joint (articulates) with another bone. Mostly made of spongy bone • Diaphysis – the long bone shaft between two epiphyses • Periosteum – the tough, vascular, fibrous covering that is firmly attached to bone and continues into tendons and ligaments. Helps form and repair bone.
Parts of a Long Bone • Spongy Bone (cancellous bone) • mostly found in the epiphyses • Composed of loosely packed bone matrix with gaps arranged in branching bony plates called trabeculae. • Spongy bone is surrounded by a thin layer of compact bone.
Parts of a Long Bone • Compact Bone • found in the wall of the bone, especially in the diaphysis • Exists as a rigid long tube with a hollow called the medullary cavity that issurrounded by a thin layer of spongy bone • The thin layer of spongy bone is further lined with a thin membrane called endosteum, which contains bone-forming cells • The medullary cavity lined by the endosteum is filled with soft connective tissue called marrow (usually yellow; red marrow is usually found in spongy bone) • densely packed matrix, having no gaps
Red vs. Yellow Marrow • Red blood cells, platelets and most white blood cells form in red marrow; some white blood cells develop in yellow marrow. The color of yellow marrow is due to the much higher number of adipocytes. Both types of bone marrow contain numerous blood vessels and capillaries. • At birth, all bone marrow is red. With age, more and more of it is converted to the yellow type. Adults have on average about 2.6 kg of bone marrow, with about half of it being red. • Red marrow is found mainly in the flat bones such as hip bone , breast bone, skull, ribs, vertebrae and shoulder blades, and in the cancellous ("spongy") material at the proximal ends (epiphysis) of the long bones such as femur and humerus. • Yellow marrow is found in the hollow interior of the middle portion of long bones (diaphysis).
(Haversian System) A Journey into Compact Bone
Inside an Osteon (Haversian System) (Volkman’s canal)
Bone Development and Growth • The skeletal system begins to develop in the first few weeks of gestation • Bones develop from connective tissue such as cartilage. They can form in two ways: • Bone can develop in sheet-like layers of connective tissue. These types of bone are called Intramembranous bone. • Bone can also develop from hyaline cartilage. These bones are called Endochondral bone.
Intramembranous Ossification • Unspecialized (primordial or primitive) connective tissue cells form membrane-like layers at sites of future bones • These primordial cells are supplied with O2 and nutrition through a dense network of blood vessels and the primordial cells actually form layers around the blood vessels • The primordial cells grow large and specialize into osteoblasts (bone-forming cells) • Osteoblasts secrete bone matrix around themselves, creating spongy bone along the blood vessels • Further along in development some spongy bone can become more dense and form compact bone
Endochondral Ossification Most bones of the human skeleton are endochondral bones • Hyaline cartilage is what exists in the place of endochondral bone early in development • Chondrocytes reside in lacunae and keep growing – their lacunae grow as well • The matrix of the cartilage begins to disintegrate and the chondrocytes die • As cartilage decomposes, a periosteum develops all round • Blood vessels and primordial connective tissue cells invade the decomposing sites • Invading primordial cells differentiate into osteoblasts and start forming spongy bone in place of the cartilage (just like intramembranous bone formation) • Once the osteoblasts are completely trapped in their bony matrix, they are called osteocytes • Osteoblasts from the periosteum deposit compact bone around the spongy bone forming in the diaphysis – this thickens the bone
Endochondral Ossification, cont’d. • In long bones endochondral ossification begins in the middle of the diaphysis – this is called the primary ossification center • The epiphyses remain cartilaginous and continue to grow • Eventually, spongy bone forms from the cartilage in the epiphyses – this is called the secondary ossification center • The primary ossification center (diaphysis) and the secondary ossification centers (epiphyses) are separated from each other by a band of cartilage called the Epiphyseal plate
Growth at the Epiphyseal Plates The chondrocytes in this plate are arranged in 4 layers • The first layer - layer closest to the end of the epiphyses contain resting chondrocytes – they do not actively grow. This layer also attaches the epiphyseal plate to the spongy bone tissue of the epiphysis • The second layer contains chondrocytes dividing mitotically. As they divide and form cartilaginous matrix around them, the epiphyseal plate thickens • As the cells divide, the older chondrocytes enlarge and thicken the plate even more – this forms the third layer • This activity lengthens the bone • Osteoblasts invade the growing plate and deposit a calcified matrix around the older cells. The old cartilage cells die. • The fourth layer is basically made up of dead chondrocytes trapped in a calcium matrix
(1st Layer – resting chondrocytes) (2nd Layer – chondrocyte mitosis) (3rd Layer- chondrocytes enlarging) (4th Layer) Layers of the Epiphyseal Plate Spongy bone and red marrow http://medocs.ucdavis.edu/CHA/402/labsyl/01/10.htm
Growth at the Epiphyseal Plates, cont’d. • Eventually, the fourth layer of the epiphyseal plate is invaded by cells called osteoclasts, which are large, multinucleated cells that are created from the fusion of white blood cells called monocytes • Osteoclasts dissolve the calcified matrix with lysosomes and phagocytize it • That allows bone-forming osteoblasts to invade the area and deposit bone matrix • Osteoclasts also invade the center of the diaphysis and dissolve some of the matrix. This forms the medullary cavity
Growth Arrest • The growth and ossification of the diaphysis and the epiphysis continues until the two ossification centers meet. • Once the sites meet, bone growth is no longer possible in that area • Some hyaline cartilage remains at the end of epiphyses as articular cartilage • Children have epiphyseal plates in their bones – indicating the possibility of further growth
67% inorganic components 33% Organic (protein) components
Bone Growth and Repair • Balanced nutrition, adequate exposure to sunlight, hormones and exercise all contribute to bone growth and repair • Calcium and phosphate salts • Vitamin D3 (Cholecalciferol) – helps in calcium absorption and is found in eggs, milk and foods fortified with it • Vitamin A is needed for osteoblast and osteoclast activity • Vitamin C is needed for collagen development, so a lack of it will inhibit bone development • Vitamin K and B12 are needed for protein synthesis in bones
Bone Growth and Repair • Growth hormone from the pituitary gland in the brain stimulates division of chondrocytes in epiphyseal plates • Lack of it will cause pituitary dwarfism • Too much will cause pituitary gigantism • Some adults acquire an excess of growth hormone and develop an exaggerated growth of certain body parts like the jaw and hands – this is called acromegaly • Male and female hormones (estrogen and testosterone) becomes active at puberty and promote bone growth • Physical exercise stimulates bone growth – this is called hypertrophy and lack of exercise causes bone loss – called atrophy
Calcium Resorption and Deposition All through life, osteoclasts reabsorb bone and octeoblasts replace bone • When blood calcium levels are low, parathyroid hormone stimulates osteoclasts to break down bone tissue, releasing calcium from bone matrix into blood • When there is too much calcium in the blood, the thyroid gland releases calcitonin which stimulates osteoblasts to pick up calcium from blood and store it in bone matrix – thus forming new bone tissue • Too much calcium in the blood also inhibits osteoclast activity
Bone and Joint Pathology • Rheumatoid arthritis - autoimmune disease, affects smaller joints (e.g., hands) • Osteosarcoma - malignant bone tumor • Osteoporosis - porous bones • Gout - deposition of sodium urate crystals • Osteoarthritis - wear and tear arthritis, major joints (e.g., knees)
Arthritis • The most common form of arthritis, osteoarthritis is also known as degenerative joint disease and occurs following trauma to the joint, following an infection of the joint or simply as a result of aging. There is emerging evidence that abnormal anatomy may contribute to early development of osteoarthritis.
Osteogenesis Imperfecta • Osteogenesis imperfecta (OI) literally means imperfectly formed bones. People with OI have an error (mutation) in the genetic instructions on how to make strong bones. As a result, their bones break easily. • One of the genes that tells the body how to make a specific protein (type I collagen) is defective in people with OI. Type I collagen is a major component of the connective tissues in bones, ligaments, teeth, and the white outer tissue of the eyeballs (sclera). As a result of the defect, the body may not produce enough type I collagen or it may produce poor quality collagen. The result in both cases is the same: fragile bones that break easily. However, the bones heal at a normal rate.
Osteoporosis • Osteoporosis is a term that means "porous bones." It is a skeletal disease affecting women and men. Osteoporosis is a condition in which bones have lost minerals—especially calcium—making them weaker, more brittle, and susceptible to fractures (broken bones). Any bone in the body can be affected by osteoporosis, but the most common places where fractures occur are the back (spine), hips, and wrists. • Women are 4 times as likely than men to develop it – usually after menopause