Liver and gall bladder
Liver and gall bladder. Lecture 25 Monday, March 5, 2007 Refs. Ross Chapter 18, Wheater’s Chapter 15, Pathologic Basis of Disease 7th ed. Chapter 18, Moore and Dalley Chapter 2, and Moore and Agur Chapter 3. Liver. Largest gland in body, necessary for life Many functions in homeostasis:

Liver and gall bladder
E N D
Presentation Transcript
Liver and gall bladder Lecture 25 Monday, March 5, 2007 Refs. Ross Chapter 18, Wheater’s Chapter 15, Pathologic Basis of Disease 7th ed. Chapter 18, Moore and Dalley Chapter 2, and Moore and Agur Chapter 3
Liver • Largest gland in body, necessary for life • Many functions in homeostasis: • Detoxification of metabolic waste and exogenous toxic compounds • Glycogen synthesis, gluconeogenesis • Synthesis of plasma proteins e.g. albumin • Synthesis of most clotting factors • Except von Willebrand factor - made in endothelial cells • Removes aged red blood cells • Synthesis of lipoproteins • Synthesis of bile
Anterior and visceral views of the liver. Lobes are right, left, caudate, and quadrate. M/D 2.50C&D
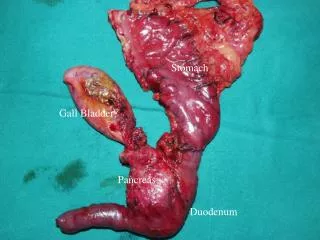
Relationship of the liver to stomach and lesser omentum. Porta hepatis is site where hepatic artery and portal vein enter and bile ducts exit . M/D 2.52
Porcine liver has connective tissue outlining hepatic lobules. WFH 15.1b
Liver terminology • Hepatocytes are large polyhedral epithelial cells. • Hepatocytes are arranged in plates or cords. • Sinusoids are vascular channels between hepatocytes that conduct blood from portal triads to the terminal hepatic venule (central vein). • Blood from the terminal hepatic venules collects into larger veins that drain into the hepatic vein. • Hepatocytes secrete bile into canaliculi; canaliculi drain into collecting ducts (canals of Hering) that drain into bile ductules.
Normal human liver has very little connective tissue WFH 15.5
Schematic of hepatic lobule- traditional unit is centered on the central vein (terminal hepatic venule) WFH 15.1a
Acinus Model: Functional unit is centered on portal tract.WFH 15.1d
Based on blood flow, zone 1 receives the most oxygen and zone 3 the least. PBD 18-1
3D schematic:In the triad, bile flows the opposite direction from blood.Blood from terminal hepatic venules is collected into the hepatic vein which joins the inferior vena cava. WFH 15.2
Portal triad:1. Terminal branch of portal vein (largest) 2. Hepatic arteriole(s) 3. Bile ductules(s) Also lymphatics and nerves.Limiting plate is the layer of hepatocytes next to the portal tract. WFH 15.3
Hepatocytes are arranged in anastomosing plates or cords of cells WFH 15.6
Characteristics of hepatocytes • Abundant cytoplasm • Cytoplasm eosinophilic, many mitochondria • Store glycogen, process lipids • Many free ribosomes and extensive RER • Large, central, round nucleus • Dispersed chromatin (transcriptionally active) • Prominent nucleolus • Variation in nuclear size and ploidy-often tetraploid • Most are in G0 but can reenter the cell cycle.
Kupffer cells, phagocytic cells of monocyte/macrophage lineage have ingested iron-sugar particles. WFH 15.8
Sinusoidal lining cells • Sinusoids: large, irregular vessels lined by endothelial cells. • Discontinuous endothelium lining in the liver. • Fenestrated lining in endocrine organs. • Usually hepatocytes are exposed to blood on at least 2 sides. • Kupffer cells are scattered along wall of sinusoid • Remove senescent erythrocytes • Phagocytose particulate debris • Stellate cells
Stellate cells • Other names: Ito cells or hepatic lipocytes • Not distinguishable by LM. • Lipid droplets containing vitamin A. • Production of extracellular matrix and collagen • Important in cirrhosis
Reticulin fibers (collagen type III) support hepatocytes and endothelial cells WFH 15.9
Bile canaliculi demonstrated by iron deposited in the walls of the canaliculi.WFH 15.10b
Extramedullary hematopoiesis • Hematopoiesis= formation and development of blood cells • In adult, it normally occurs in bone marrow. • Extramedullary= outside the bone marrow • In fetus, hematopoiesis occurs in liver and spleen. • Blood forming cells are in the sinusoids. • Hepatocytes appear normal. • Important to distinguish from inflammation
Ultrastructure of hepatic cords • Sinusoids are lined by a discontinuous layer of sinusoidal lining cells (endothelium). • Space of Disse= space between sinusoidal lining cell and hepatocyte. • Space is continuous with sinusoid lumen through gaps in endothelium. • Hepatocytes are exposed to plasma. • Hepatocytes have irregular microvilli extending into space of Disse and into bile canaliculi • Hepatocyte cytoplasm contains numerous mitochondria, RER, SER, endocytic vesicles, and lipid droplets. • Polarity of hepatocytes • Bile canalicular membrane is apical. • Sinusoidal membranes is basolateral.
EM of space of Disse and bile canaliculus with microvilliW 15.12b
Bile formation and storage • Bile is made by hepatocytes and is usually stored in the gallbladder. • Canaliculi carry bile from hepatocytes to peripheral lobule where they open into canals of Hering which join bile ductules in the portal area. • Ductules come together forming ducts, lobar ducts, and finally right and left hepatic ducts which leave the liver and join forming the common hepatic duct. • The cystic duct from the gall bladder joins the common hepatic duct forming the common bile duct. • In 60-70% of humans the bile duct joins the main pancreatic duct forming the ampulla of Vater.
Bile duct sphincters • Choledochal = sphincter of the bile duct where it joins ampulla. When closed, bile from liver enters cystic duct and is stored and concentrated in the gall bladder. • Spiral valve of Heister may help retain bile between meals. • The hepatopancreatic sphincter (sphincter of Oddi) controls the flow of bile and pancreatic juice into the duodenum.
Gall Bladder WFH 15.13bLining cells concentrate bile 5-10 fold