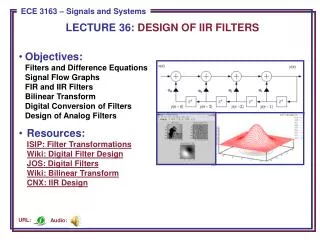
Objectives
Pediatric Oncology for the Primary Care Provider Kate A. Mazur, MSN, RN, CPNP Texas Children’s Hospital Advanced Practice Provider 1 st Annual Conference Houston, TX February 8, 2014. Objectives. Review the incidence of childhood cancer

Objectives
E N D
Presentation Transcript
Pediatric Oncology for the Primary Care ProviderKate A. Mazur, MSN, RN, CPNPTexas Children’s Hospital Advanced Practice Provider 1st Annual ConferenceHouston, TXFebruary 8, 2014
Objectives • Review the incidence of childhood cancer • Describe the most common childhood malignancies, with a focus on initial evaluation and diagnosis, red flags, and when to refer to specialist • Analyze the unique precautions for patients with oncologic illnesses
The Scope of the Problem • 13,400 children ages birth to 19 years are diagnosed with cancer each year • Cancer is the #1 cause of disease-related death in children Source: Surveillance, Epidemiology, and End Results Program, 1975-2003, Div. of Cancer Control and Pop. Sciences, NCI, 2006
The Good News… • Overall 5 year survival rate across all cancers is now 80% • Estimated 270,000 childhood cancer survivors in the U.S. • However, two-thirds of survivors face at least one chronic health problem • 25% of survivors face a late effect from treatment that is classified as severe or life-threatening
Where do I start? • Early diagnosis and initiation of treatment is imperative to improved survival • Diagnosis of cancer starts with a thorough history and physical • Most symptoms of childhood cancer due to either a mass, its effect on the surrounding tissues, invasion of the bone marrow, or secretion of a substance by the tumor that disturbs normal functions • Most common presenting signs and symptoms of many malignancies include weight loss, failure to thrive, anorexia, malaise, fever, pallor, and lymphadenopathy
High Risk Patients • Familial cancer pre-disposition syndromes • Li-Fraumeni Syndrome • Familial adenomatosispolyposis • Beckwith-Wiedemann Syndrome • Family history of cancer • Retinoblastoma • Autoimmune diseases in patient or family • Down Syndrome • Neurofibromatosis Type 1 • HIV/AIDS
Leukemia • Cancer of the bone marrow • Uncontrolled proliferation of immature white blood cells (“blasts”) • Most common type of cancer in children and adolescents under 20 years of age (~30%) • Incidence • 4900 new cases each year • Males > Females; Hispanics > Caucasians > African Americans • Peak age 2-5 years • Risk factors • Down Syndrome: 14-fold increase • Klinefelter Syndrome • Fanconi anemia • Immunodeficiencies: ataxia telangiectasia, Wiskott-Aldrich, Bloom syndrome • Past exposure to chemotherapy or ionizing radiation
Most Common Types of Childhood Leukemia • Acute lymphoblastic leukemia (ALL) ~ 80% • Acute myelogenous leukemia (AML) ~ 15% • Chronic myelogenous leukemia (CML) ~ 5%
Leukemia: Presenting Signs and Symptoms • Relate to the infiltration of the bone marrow • History • Fatigue • Persistent fevers • Bone pain • Anorexia • Weight loss • Recurrent infections • Physical Exam • Pallor • Bleeding, bruising, or petechiae • Hepatosplenomegaly • Lymphadenopathy
Lymphadenopathy: When to Worry • Supraclavicular, axillary, or epitrochlearadenopathy • Adenopathy that persists longer than 6 weeks or is increasing in size • Asymmetric lymphadenopathy • Leukemia usually presents with generalized lymphadenopathy; localized LAD more likely to be infectious in origin • Malignant nodes generally hard and nontender; infectious/inflammatory nodes usually tender, freely moveable, overlying erythema • For localized cervical adenitis with inflammation and fever, treat with ONE course of antibiotics, if no response refer • DO NOT START STEROIDS
Leukemia: Initial Diagnostic Tests • CBC with manual differential, reticulocyte count, and peripheral blood smear • Chem 10: Electrolytes, BUN, creatinine, Ca2+, Mg2+, PO4-, uric acid, LDH • Hypocalcemia, hyperkalemia, hyperphosphatemia, hyperuricemiamay indicate tumor lysis syndrome oncologic emergency • Elevated LDH (non-specific tumor marker) • Bone marrow aspirate and biopsy is the only definitive diagnostic test • Done by oncology service only
Complete Blood Count: A Review • White blood cells/Neutrophils • Responsible for fighting infection • Red blood cells/Hemoglobin • Carries O2 from lungs to blood tissues and CO2 from tissue to lungs • Platelets • Necessary for clotting and control of bleeding
CBC Findings in Leukemia • Leukocytosis - ~50% with WBC >10,000 and ~20% > 50,000 • Elevated blasts and low neutrophils • Anemia • Thrombocytopenia • 2 or more cell lines decreased REFER • 90% present with hemoglobin < 11g/dL, 45% < 7g/dL • 75% present with platelets < 100,000/mm3
Lymphoma • Tumor of the lymphatic system • Incidence • 1500 new cases each year • More common in adolescents and older teenagers, males, Caucasians • Risk factors • Immunodeficiency syndromes: Wiskott Aldrich, SCIDS, HIV/AIDS • Autoimmune diseases: RA, SLE • Some viruses: Epstein-Barr (particularly for Burkitt’s lymphoma)
Types of Lymphoma • Non-Hodgkin’s Lymphoma – 60% • Lymphoblastic • Anaplastic • Burkitt’s • Diffuse large B-cell • Hodgkin’s Lymphoma – 40%
Lymphoma: Presenting Signs and Symptoms • History – 75% asymptomatic • Unexplained fever for more than 3 days • Weight loss of 10% within 6 months • Drenching night sweats • Malaise • Anorexia • Physical Exam – based on location of disease • Head/Neck: supraclavicular or cervical adenopathy, jaw swelling, unilateral tonsillar enlargement • Abdomen: splenomegaly, abdominal distention, jaundice • Mediastinum: cough, chest pain, stridor
Lymphoma: Evaluation and Diagnostic Work Up • DO NOT START STEROIDS • Blood work: CBC w/diff, liver and renal fxn tests, including alkaline phosphatase; ESR, ferritin, LDH may be elevated • Imaging Studies • CT scans (neck, chest, abdomen, pelvis) • PET scan • Bone scan • Biopsy of affected node • Required for definitive diagnosis • Done under guidance of oncology team only
Brain Tumors • Can be malignant or “benign” • Much slower rate of treatment advances than other malignancies • Unique challenges in children – brain still developing • Incidence • 3400 new cases every year • More common in ages < 15 years • Risk factors • Little known • Hereditary cancer predisposition syndromes (i.e. Li-Fraumeni Syndrome)
Most Common CNS Tumors • Astrocytoma • Most supratentorial but can originate in cerebellum, brainstem, or hypothalamus • Brain Stem Glioma • Medulla, pons • Medulloblastoma • Cerebellum • Ependymoma • Ependymal tissue within the ventricular system, most commonly the fourth ventricle Picture from The Children’s Hospital at Montefiore, http://www.montekids.org/services/neurosurgery/neurologicaldisorders/brain_tumor/
CNS Tumors: Presenting Signs and Symptoms • Depends on site and severity of disease as well as child’s age & development • History • Seizures • Visual changes • Headache • Nausea/vomiting, often in morning • Poor concentration or mental status change • Physical Exam • Hemiparesis • Endocrinopathies • Ataxia • Cranial nerve deficits
Headache: When Further Evaluation is Warranted • Recurrent morning headache • Headache that awakens the child • Intense, incapacitating headache • Changes in the quality, frequency, or pattern of headaches • Presence or onset of neurologic abnormality • Ocular findings such as papilledema, decreased visual acuity, or loss of vision • Associated with vomiting that is persistent, increasing in frequency, or preceded by recurrent headaches • Age 3 years or less • DO NOT START STEROIDS
CNS Tumors: Diagnostic Tests • Imaging studies are the only diagnostic tests • MRI brain and spine • CT often obtained first due to easy access • LP if clinically indicated and safe to perform
Solid Tumors: Evaluation of an Abdominal Mass • ALWAYS suspect a malignant solid tumor in a child with a palpable abdominal mass • Avoid abdominal palpation as much as possible; palpate gently if necessary • In younger children, often renal neuroblastoma or Wilms’ tumor • In older patients, may be related to leukemia or lymphoma with enlargement of the spleen or liver • Obtain comprehensive GU and GI histories • Associated symptoms of flushing, palpitations, diarrhea, failure to thrive, and fever could point to disseminated process such as neuroblastoma • Complete exam with focus on skin, extremities (bone pain), neuro exam (Horner’s syndrome, spinal cord compression), organomegaly, measurement of abdominal girth • Obtain diagnostic imaging STAT • Usually start with abdominal ultrasound
Wilm’s Tumor • Large, rapidly growing, vascular renal tumor • Second most common intra-abdominal malignancy in children • Can be bilateral or unilateral • Incidence • 500 new cases/year • Peak incidence 3 years of age • Slight female predominance; African-Americans > Caucasians > Asians • Risk factors • Congenital anomalies: GU malformations, hemihypertrophy, Beckwith-Wiedemann syndrome, Denys-Drash syndrome • Familial pre-disposition syndromes: Li-Fraumeni syndrome
Wilm’s Tumor: History and PE Findings • Abdominal mass – smooth, firm, rarely crosses midline but 5-10% are bilateral • Diffuse abdominal distention with large masses • Usually asymptomatic, but 25% have abdominal pain, vomiting, hematuria, hypertension • Signs of thrombosis: leg swelling, prominent veins over abdomen • Signs of hemorrhage into tumor (occurs rarely): anemia, fever, rapid abdominal distension
Wilm’s Tumor: Diagnostic Tests • Blood work – CBC, liver function, renal function • Coagulation screen – may acquire Von Willebrand’s • Abdominal ultrasound usually first test ordered – will reveal mass arising from within kidney • Doppler US to assess patency of renal vein and inferior vena cava • Abdominal CT
Neuroblastoma • Cancer of the sympathetic nervous system; derived from neural crest cells • Second most common solid tumor of childhood and the most common extracranial solid tumor • Incidence • 650 new cases every year in the U.S. • 90% cases in children < 5 years old • Boys > girls; Caucasian predominance • Risk factors • Most cases sporadic • Has been identified in other disorders of neural crest cells • Neurofibromatosis • Hirschsprung’s disease • Beckwith-Wiedemann syndrome • DiGeorge syndrome
Neuroblastoma: Clinical Presentation • Can arise anywhere along sympathetic nervous system • Signs and symptoms depend on location of primary tumor and presence of metastasis • Two-thirds have primary site in abdomen, usually adrenal • Thoracic region is the next most common primary site • About 60% have metastatic disease at presentation due to vague initial symptoms and late presentation • Bone marrow • Bone • Liver • Skin • Orbits
Neuroblastoma: Presenting Signs and Symptoms • Firm, irregular, non-tender abdominal mass • Hepatomegaly • Abdominal pain • Urinary obstructions • Flushing • Sweating • Diarrhea • Anorexia • Malaise • Site-specific symptoms from metastases to bone, skin, liver, or CNS • Opsoclonus-myoclonus syndrome – “dancing eyes and dancing feet”
Neuroblastoma: Diagnostic Tests • CBC – cytopenias • Chem 10 • Ferritin, LDH, uric acid • Liver panel • Urine catecholamines (VMA/HVA) • CT chest/abdomen/pelvis • Tissue biopsy for definitive diagnosis • Bilateral bone marrow aspirate and biopsy to evaluate for BM involvement • MIBG scan or bone scan to evaluate for metastasis
Osteosarcoma • Tumor of the bone; usually at the end of long bones • Incidence • 400 new cases/year • More prominent during adolescent growth spurt; periods of rapid bone growth • Males > females; African-Americans > Caucasians • Risk factors • Ionizing radiation • Hereditary retinoblastoma • Li-Fraumeni Syndrome
Osteosarcoma: Signs and Symptoms • Dull, aching pain, usually worse at night • +/- soft tissue swelling, warmth • May have vascularity over the mass • Decreased range of motion • Often long duration of symptoms prior to diagnosis; can be up to 6 months
Osteosarcoma: Diagnostic Tests • Diagnostic Imaging • Plain radiograph of affected area – “sunburst pattern” • MRI to further examine tumor boundaries, soft tissue component, relationship to joints, blood vessels, neurovascular bundle • Chest XR or CT to evaluate for mets • Bone scan to evaluate for skeletal mets • Blood Tests • Elevations in LDH, alkphos may be present • Tumor Biopsy • Necessary for definitive diagnosis
Supportive Care of a Patient with CancerInfection Prophylaxis • Good hand washing!! • Proper dental hygiene – daily brushing with a soft brush, use of chlorhexidine mouth rinse • Avoidance of crowded, enclosed spaces • Cleanliness of perirectal area – avoid constipation • No rectal temperatures! • Prophylaxis for Pneumocystiscariniipneumonia (PCP) from time of diagnosis until 6 months after completion of therapy – Trimethoprim-sulfamethoxazole, Pentamidine, Dapsone • Viral and fungal prophylaxis may be indicated
Management of Fever in the Child with Cancer • Defined as a single temperature of ≥ 101°F or two temperatures ≥ 100.4°F taken 1 hour apart • Do not give anti-pyretics! • No rectal temperatures • Every cancer patient who presents with fever should be considered septic until proven otherwise • Prompt evaluation and management essential for improved survival • Goal is to administer first dose of IV antibiotics within 1 hour of presentation
Initial Evaluation of Fever • Prompt tx essential – send to ER or urgent care center for immediate evaluation and management and call oncology service • Evaluate for signs of septic shock • Tachycardia – usually the first sign of shock. Ideally, aggressive treatment starts here. • Check perfusion – delayed capillary refill; pulses weak and thready or bounding • Hypotension – LATE sign • Mental status changes; lethargy – OMINOUS • Examine for focal signs of infection • Often there are none • Oral cavity, perianal area, skin, respiratory tract, abdomen (typhlitis)
Fever: Diagnostic Work Up • CBC with differential – risk-based management based on neutrophil count • Blood cultures – all CVC lumens and peripheral; important to have prior to first dose of antibiotics • Urinalysis/urine culture, if feasible based on clinical status – no catheterization • Additional cultures of any potential sources of infection – skin lesions, stool sample if diarrhea, mouth sores • Do NOT I & D any skin lesions • Chest XR if respiratory symptoms – obtain portable or delay until after initial antibiotics • Do NOT perform LP until oncology service is consulted
Empiric Therapy of the Febrile Patient • DO NOT wait for culture results • Broad-spectrum antibiotics must be started immediately; will tailor antibiotic choice when culture results known • Antibiotics chosen based on individual institution’s local microbial prevalence and antibiotic susceptibility patterns • Regimen also based on risk criteria – high risk if ANC < 100, infant ALL, AML, in any phase of leukemia tx other than maintenance (induction at highest risk), < 7 days from last chemotherapy, focal signs of infection, or concern for sepsis • Admission often indicated • Anti-virals and/or anti-fungals may be added as clinically indicated • Septic shock treated aggressively with normal saline fluid boluses and triple antibiotics
Immunizations and the Cancer Patient • Cannot assume adequate immunization even if patient’s vaccines are up to date prior to diagnosis • NO LIVE VACCINES • Siblings or household contacts should not receive the oral polio vaccine • All other vaccines may continue as scheduled, but will need to check titers at completion of treatment to ensure adequate immunity. Boosters or full re-immunization may be needed after completion of therapy • Highly recommend seasonal influenza vaccination in patient and household contacts
References • Howlader N. et al. SEER Cancer Statistics Review, 1975-2010, National Cancer Institute. Bethesda, MD, http://seer.cancer.gov/csr/1975_2010/, based on November 2012 SEER data submission, posted to the SEER web site, April 2013. • Hastings, C. (2002). The Children’s Hospital Oakland Hematology/Oncology Handbook. St. Louis, MO: Mosby, Inc. • Kline, N. & Tomlinson, D. (2005). Pediatric Oncology Nursing. Heidelberg, Germany: Springer Publishing. • Lowry, A., Bhakta, K., & Nag, P. (2011). Texas Children’s Hospital Handbook of Pediatrics and Neonatology. McGraw-Hill Publishing. • Pizzo, P. & Poplack, D. (2005). Principles and Practice of Pediatric Oncology, 5th edition. Philadelphia, PA: Lippincott, Williams & Wilkins. • Zorc, J. (2013). Clinical Handbook of Pediatrics, 5th edition. Philadelphia, PA: Lippincott, Williams & Wilkins.