Unveiling the Complement System: A Comprehensive Overview
Discover the intricate workings of the complement system, a vital component of the body's immune response. Learn about the classical, alternative, and lectin pathways, from activation to amplification and cellular lysis.

Unveiling the Complement System: A Comprehensive Overview
E N D
Presentation Transcript
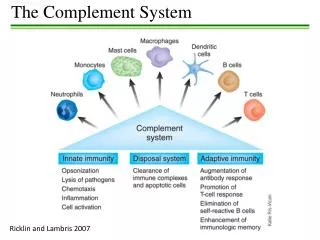
Introduction • The complement system consists of a number of smallproteins found in the blood, in general synthesized by the liver, and normally circulating as inactive precursors (pro-proteins) • When stimulated ---release cytokines and initiate an amplifying cascade of further cleavages. • The complement system is part of the innate immune response (vs adaptive)
In 1899, Paul Ehrlich named as complement • It is named “complement system” because it was first identified as a heat-labile component of serum that “complemented” antibodies in the killing of bacteria • It is now known that it consists of over 30 proteins and contributes 3 g/L to overall serum protein quantities
“Classical” Pathway (Specific immune response) • Begins with antibody binding to a cell surface and ends with the lysis of the cell • The proteins in this pathway are named C1-C9 (the order they were discovered and not the order of the reaction) • When complement is activated it is split into two parts • a – smaller • B – larger part and usually the active part • Remember 3 Key Words • ACTIVATION • AMPLIFICATION • ATTACK
“Classical Pathway” • ACTIVATION • C1q portion of C1 attaches to the Fc portion of an antibody • Only IgG and IgM can activate complement • Once activated C1s is eventually cleaved which activates C4 and C2 • C4b & C2a come together to form the C4b2a which is the C3 convertase • C3 convertase activates C3 to C3a and C3b
“Classical Pathway” • ACTIVATION • C3a binds to receptors on basophils and mast cells triggering them to release there vasoactive compounds (enhances vasodilation and vasopermeability). • C3a is called an anaphylatoxin (a fragment that activate the complement system) • C3b serves as an opsonin which facilitates immune complex clearance
“Classical Pathway” • AMPLIFICATION • Each C1s creates many C4b and C2b fragments • Each C4bC2a creates many C3b (activated C3) • Each C3b goes on to create many Membrane Attack Complexes • Example • 1 C1S makes 100 C4bC2b • 100 C4bC2b makes 10,000 C3b • 10,000 C3b makes 1,000,000 MAC
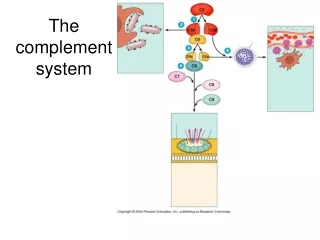
“Classical Pathway” • ATTACK • Most C3b serves an opsonin function • Some C3b binds to C4bC2a to form the C5 convertase C4bC2aC3b • C5 convertase cleaves C5 leading to the formation of the Membrane attack Complex (C5-C6-C7-C8-C9) • The MAC (memberane attack cells/Unit) “punches holes” in cell walls resulting in lysis
“Alternative Pathway”(Non specific immune response) • Properdin (Regulator- complement activation) Pathway • Requires no specific recognition of antigen in order to cause activation
“Alternative Pathway” • ACTIVATION • Spontaneous conversion from C3 to C3b occurs in body • Normally, C3b is very short lived and quickly inactivated by proteins on the surface of the body’s own cell walls • However, bacteria or other foreign material may lack these surface proteins allowing C3b to bind and stay active
“Alternative Pathway” • AMPLIFICATION • Factor B binds to C3b • Factor B is then cleaved by factor D into Ba and Bb • C3bBb remains which acts as a C3 convertase (C3 C3a and C3b) • C3bBbC3b is formed which acts as a C5 convertase
“Alternative Pathway” • ATTACK • C5 is cleaved to C5a and C5b • C5b then starts the assembly of the Membrane Attack Complex
Lectin pathway • Activate mannose-binding lectin • Antibody not involved • The lectin pathway is homologous to the classical pathway but with the opsonin, mannose-binding lectin (MBL), and ficolins, instead of C1q
Lectin pathway • This pathway is activated by binding of MBL to mannose residues on the pathogen surface, which activates the MBL-associated serine proteases, MASP-1, and MASP-2 (very similar to C1r and C1s, respectively), which can then split C4 into C4a and C4b and C2 into C2a and C2b. C4b and C2a then bind together to form the classical C3-convertase, as in the classical pathway.
Lectin pathway • Ficolins are homologous to MBL and function via MASP in a similar way.
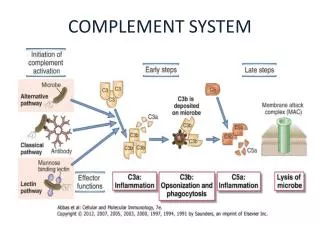
Summary - Activation • Complement can be activated by the binding of antibody (Classical) or by the adherance of C3b to foreign material (Alternative) • The two pathways converge at the formation of the C5 convertase (C4b2a3b or C3bBbC3b) • The final common pathway is the formation of the membrane attack complex
Summary - Function • Opsonization – C3b • Chemotaxis – C5a (attracts neutrophils) • Increases vasodilation & permeability(Inflammation) of capillary beds via mast cell and basophil activation – C3a & C5a (Anaphylatoxins) • Cellular Lysis via the MAC (Membrane attack cells )(by rupturing membranes of foreign cells)