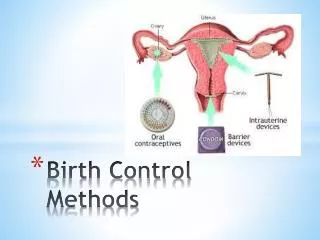
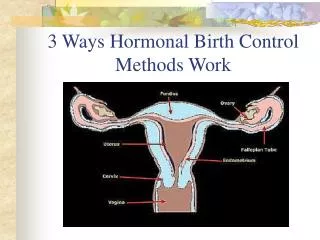
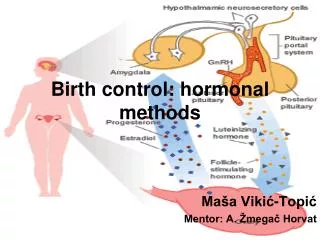
Birth Control Methods
Birth Control Methods. Planned Parenthood of Houston and Southeast Texas, Inc. www.pphouston.org. Key Dates in History. Key Dates in History. 1564 : Fallopius, Italian doctor, describes the use of linen CONDOMS to protect against syphilis.

Birth Control Methods
E N D
Presentation Transcript
Birth Control Methods Planned Parenthood of Houston and Southeast Texas, Inc. www.pphouston.org
Key Dates in History • 1564: Fallopius, Italian doctor, describes the use of linen CONDOMS to protect against syphilis. • 1840: First patented Diaphragm available in the United States. • 1873: COMSTOCK LAW: restrict birth control by forbidding mailing and transportation of contraceptives and in some state their sale and use.
Key Dates in History • 1937: America Medical Association ends the 25 year opposition to contraception; recognized that birth control needs to be taught in medical school. • 1960: BIRTH CONTROL PILL becomes available in the in the U.S. • 1966: Griswold Decision: Supreme Court declares laws prohibiting sale and use of contraceptive are unconstitutional.
Oral Contraceptive Pills “OCP’s” Available in many shapes, sizes, strengths, colors, and combinations. Pills per pack may vary: 21-day, 28-day, and new Seasonale, which is 3-months
Description: Estrogen and Progestin 1 pill is taken daily Time sensitive, the pill is to be taken at the same time every day Oral Contraceptives: the Pill
Effectiveness: Perfect Use Failure Rate in First Year: 0.1% (of every 1,000 women who take pills for one year 1 will become pregnant in the first year) Typical Use Failure Rate in First Year: 5 % (of every 1,000 women who take pills for one year 5 will become pregnant in the first year) Oral Contraceptives: the Pill
Mechanism: Suppresses ovulation Thickens cervical mucus Thins endometrium Slows tubal motility Oral Contraceptives: the Pill
DISADVANTAGES Mood Changes, depression, anxiety Daily pill taking may be stressful No Protection against STI (Sexually Transmitted Infections), including HIV Nausea, breast tenderness, especially in the first few cycles Weight gain Oral Contraceptives: the Pill ADVANTAGES • Regulates menses • Decreases blood loss/ menstrual cramps • No disruption at time of intercourse • Decrease risk of ovarian/endometrial cancer • Treatment for acne
Special Considerations: Adolescents Failure rates are high in teens, due the regimented pill schedule At risk for STI, encourage condom use Most common reason for sick days at work/school, due to uncomfortable menstrual symptoms (under 25) Treats acne Oral Contraceptives: the Pill
Description: Estrogen and Progestin 1 Patch a week, for 3 weeks 4th week patch free, Menstruation Usually worn lower abdomen or buttocks Ortho Evra: The Patch
Effectiveness: Perfect Use Failure Rate in First Year: 1 women of every 1,000 women will become pregnant in the first year Overall Failure Rate: ? Ortho Evra: The Patch
Mechanism: Prevents pregnancy in the same way that oral contraceptives do (Ovulation, cervical mucus, endometrium, tubal motility) Ortho Evra: The Patch
Disadvantages: Mood Changes, depression, anxiety No Protection against STI (Sexually Transmitted Infections), including HIV Nausea, breast tenderness, especially in the first few cycles Weight gain Cannot use if breastfeeding Ortho Evra: The Patch Advantages: • Menstrual (Similar to the Pills) • Nothing to do on a daily basis • No disruption at time of intercourse
Special Considerations: Avoid placing the patch on exactly the same site two consecutive weeks NEVER PLACE PATCH ON THE BREAST!!! Location of patch should not be altered mid-week No band aide, tattoos or decals on top of patch as it may alter absorption of hormones It is unknown if tanning beds interfere with efficacy Avoid placing lotion/creams/powderson site Ortho Evra: The Patch
Nuva Ring: the Ring Description: • Combined estrogen and progestin • Thin flexible transparent ring • Left in place in the vagina for three weeks and removed for a week to allow a menstrual period the fourth week. • Maintains a steady low release rate while in place.
Nuva Ring: the Ring Effectiveness: • Overall pregnancy rate:1.2 per 100 women
Nuva Ring: the Ring Mechanism: • Suppresses ovulation • Similar to combined pills
Nuva Ring: the Ring Disadvantages: • Some women dislike placing/removing objects into/out of their vagina • Adverse side effects similar to the pill • Possible devise expulsion Advantages: • Only TWO TASKS: Insertion/Removal 1x month • Steady even hormonal levels in blood are achieved • Privacy/No visible patch or pill packages • 95% of women say they cannot feel device
Nuva Ring: the Ring Special Considerations: • Excellent option for adolescents: Require less discipline than taking pills • Women wanting regular menstrual periods
DepoProvera “The Shot” • Private • Don’t have to remember to take a pill • Four times a year
DepoProvera “The Shot” Description: • Injected intra-muscularly into the deltoid or gluteus-maximums every 11 to 13 weeks. • Progestin only
Depo Provera Effectiveness: • Perfect use failure rate in first year: 0.3% • Typical use failure rate in first year: 3%
Depo Provera Mechanism: * Suppresses Ovulation * Thickens cervical mucus * Slows tubal and endometrial mobility
Depo Provera Advantages: • Less menstrual blood loss and anemia • After one year 50% of users will develop amenorrhea • 80% will develop amenorrhea in 5 years • Only need to remember 1x every three months Disadvantages: • Irregular menses during first several months • Unpredictable spotting and bleeding • Possible weight gain: Progressive-Significant (5.4 1st year, after 5 years 16.5) • Patient fear of pregnancy or build up of menses in uterus if not explained well • Decreased libido • Fear of needles • Return to fertility is long average 10 months from last injection
Depo Provera Special Considerations: • Adolescent women: Extremely effective with long carry over if patient returns late for reinjection • All women, including teens, should be encouraged to take calcium tabs and exercise regularly
Intrauterine Device “IUD” • This is not your Mother’s IUD…. • Most popular method in the world, although it is not very popular in the United States.
Intrauterine Contraception: ParaGard/Mirena Description: • T-shaped device with two flexible arms that bend down for insertion but open into the uterus. • Two straw-colored strings protrude through the cervix into the vaginal canal
ParaGard/Mirena Effectiveness: ParaGard • 99.2%-99.4% Effectiveness: Mirena • 99.9%
Intrauterine Contraception: ParaGard/Mirena Mechanism: Mirena • Progestin Only • Causes cervical mucus to become thicker then by preventing sperm from moving up the reproductive track • Prevents implantation Mechanism: Paragard • Works by preventing fertilization • Works primarily as a spermicide,Copper ions inhibit sperm motility so they rarely reach the tube
ParaGard Advantages: • Effective long term (10 years) contraception from a single decision. • Requires no action at time of intercourse • Cost effective • Rapid return to fertility • Good option for women who cannot use hormones • 95% user satisfaction, the highest of any other contraceptive currently begin used by women. Disadvantages: • Blood loss during menstruation increased by 35% and increase cramping • Must check strings monthly after menstruation • Requires office procedure for insertion and removal, can be uncomfortable • Increase risk of infection PID • Uterine perforation • May be expelled
Mirena Advantages: • After 3-4 months it decreases menstrual blood loss more than 70% • Amenorrhea: 20% by 1 year, 60% by 5 years • Reduced risk PID, ectopic pregnancy by 60% • As effective, or more effective than female sterilization • Long lasting method, up to 5 years • Immediate return to fertility Disadvantages: • Possible expulsion • Acne, Headaches, discomfort after insertion or removal • Risk of PID increased • Ovarian cysts, most regress spontaneously
ParaGard/Mirena Special Considerations: • Women at risk for STI’s may be discouraged from usage. (Paragard/Mirena) • Some clinicians require chlamydia and gonorrhea testing prior to insertion. (Paragard/Mirena)
Implanon Description: • Progestin only • Thin, flexible, plastic implant about the size of a matchstick. • Inserted under the skin by the bicep muscle. • Implanted in the arm for3 years.
Implanon Effectiveness: • Perfect Use Failure Rate in First Year: 0.3% • Typical Use Failure Rate in First Year: 3%
Implanon Mechanism: • Constantly releases progestin into the bloodstream • Suppresses ovulation • Thickens the cervical mucus
Implanon Advantages: • Insertion only takes a few minutes • Protection against pregnancy is immediate if you get the implant during the 1st five days of your period • Ability to get pregnant is immediate after removal • Gives continuous long-lasting birth control without sterilization • No medicine to take every day Disadvantages: • Irregular bleeding is the most common side effect • Periods become lighter and may stop altogether or periods may become heavier and last longer • Some women will have longer heavier periods • Acne, change in appetite, or sex drive • Pain at the site of insertion
Cervical Cap • Inserted into vagina to cover cervix. • Was once a very popular method. Used with spermicidal jelly or sometimes foam. • Must be fitted by a clinician.
Diaphragm • Inserted into vagina to cover cervix. • Was once a very popular method. Used with spermicidal jelly or sometimes foam. • Like the Cervical Cap, it must be fitted by a clinician. • 84%-94% Effective
Emergency Hormonal Contraception: Plan B Description: • Progestin Only (More effective less side effects than combine EC) • ASAP, but can be used up to 120 hours, sooner is better • Pills must be taken 12 hours apart • Over-the-counter for women ages 18 and over • FDA recently passed a ruling allowing EC to be OTC for women beginning at 17 yearsof age, but it has not gone effect as of yet
Emergency Hormonal Contraception: Plan B Effectiveness: • Pregnancies/100 women: < 12 hours: 0.4% 1-3 days: 2.7% Average: 1.1%
Emergency Hormonal Contraception: Plan B Mechanism: • Prevents pregnancy and never by disrupting an implanted pregnancy • Inhibits ovulation • Thicken cervical mucus • May effect tubal transport of sperm or ova
Emergency Hormonal Contraception: Plan B Advantages • Opportunity to prevent pregnancy after, rape, mistake or method failure • Reduces anxiety • Process attaining EC may initiate women to use ongoing contraception Disadvantages • Time limitation • Next menses may be early • Notable changes in flow for next menses • Not as effective as other forms of birth control • Can be more expensive • 23% experience nausea few experience vomiting
Emergency Hormonal Contraception: Plan B Special Considerations: • There is no limit to the number times in a year a woman can use EC, but it is not to be used in place of birth control (it is also expensive).
Non-Prescription Methods • Female Condom • Male Condom • Spermicidal Foam • Spermicidal Film • Natural Family Planning • Abstinence
FEMALE CONDOMS • Popular in developing nations because of its durability - in fact, women have been known to wash and reuse it. This is NOT recommended. • NOT REUSABLE • Purchase at a drug store
Female Condom Description: • Inserted into vagina with the moveable ring inside the vagina creating an internal sheath. The large ring externally covers the labia. • Disposable single use sheath made of polyurethane • Shelf life: 3-5 years • More expensive than male condom
Female Condom Effectiveness: • Perfect use failure rate in first year of use: 5% • Typical use failure rate in first year: 21% • 79% - 95% Effective
Female Condom Advantages: • Can be inserted up to 8 hours before sex to allow more spontaneity • Woman can make sure she is somewhat protected against STIs • No medical visit required, available over the counter • Can be safely used with individuals who have latex allergies Disadvantages: • Requires careful sexual practices during intercourse • Noise made during intercourse can be distracting, if occurs add more lubricant • In one study, 88% of females disliked using the female condom • Somewhat difficult for new users • Possible increase risk of UTI • Possible difficulty inserting and removing devise