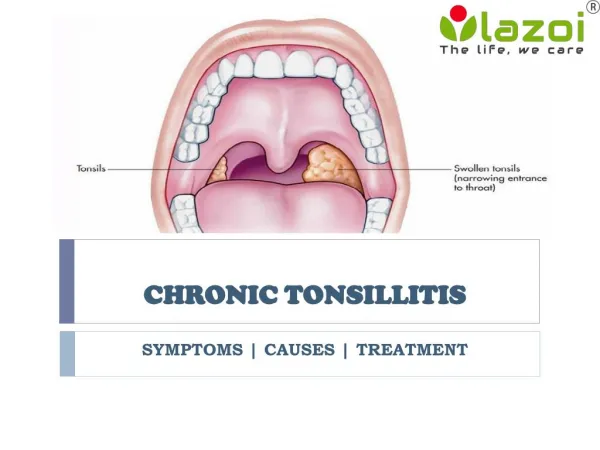
Chronic Tonsillitis Pharyngitis
Chronic Tonsillitis. Chronic Tonsillitis. Halitosis

Chronic Tonsillitis Pharyngitis
E N D
Presentation Transcript
1. Chronic Tonsillitis & Pharyngitis By Adnan AL-Maaitah
3. Chronic Tonsillitis Halitosis � due to crushing of tonsilloliths
More resistant to antibiotics
Obstruction to breathing � snoring, sleep apnea
Blockage of Eustachian Canal
Dysphagia
Constants feeling of fullness and pain in the throat
Accompany multiple infections
May be with peritonsilar abscess
Persistent tender cervical nodes
4. Tonsillolith
7. Tonsillectomy Surgical removal of tonsils or a tonsil
One of the most common surgical procedures among children
Controversy regarding indications for surgery
8. Tonsillectomy / Indications The American Academy of Otolaryngology�Head and Neck Surgery (AAO-HNS) publishes clinical indicators for surgical procedures:
Absolute indications
Enlarged tonsils that cause upper airway obstruction, severe dysphagia, sleep disorders, or cardiopulmonary complications
Peritonsillar abscess�that is unresponsive to medical management and drainage documented by surgeon, unless surgery is performed during acute stage
Tonsillitis resulting in febrile convulsions
Tonsils requiring biopsy to define tissue pathology
Relative indications
Three or more tonsil infections per year despite adequate medical therapy
Persistent foul taste or�breath�due to chronic tonsillitis that is not responsive to medical therapy
Chronic or recurrent tonsillitis in a streptococcal carrier not responding to beta-lactamase-resistant antibiotics
Unilateral tonsil hypertrophy that is presumed to be neoplastic
Other indications: cleft palate, carrier to TB or diphtheriaOther indications: cleft palate, carrier to TB or diphtheria
9. Tonsillectomy/Contraindications Bleeding diathesis
Poor anesthetic risk or uncontrolled medical illness
Anemia
Acute infection (tonsillitis: wait 3 weeks)
Peritonsillar abscess
11. Tonsillectomy/Procedure Patient lying flat on their backs, with the shoulders elevated on a small pillow so that the neck is hyperextended � the so-called 'Rose' position.
Tonsil is held by forceps and removed by blunt scalpel or electrocautery
Bleeding is stopped with electrocautery
15. Tonsillectomy/Postop. Painful � give adequate analgesia
Hydration
Tonsil beds maybe covered with white or yellowish exudate (up to 2 weeks) � normal, not pus
Complications:
Bleeding: primary, reactionary (first 24Hr), secondary (3-7 days)
Sepsis
Chest complications
Otitis media
Peritonsillar abcess
18. Pharynx/Anatomy The musculomembranous cavity behind the nasal cavities, mouth and larynx communicating with them and with the esophagus.
Composed of skeletal muscles lined by mucous membrane.
Respiratory and digestive function
Divided into:
Nasopharynx
Oropharynx
Hypopharynx (Laryngopharynx)
19. Pharynx/Anatomy
20. Pharyngitis Inflammation of the mucous membrane and underlying part of the pharynx
One of the most common causes of absence from school or work
Vast majority due to viruses
More common in children (peak 4 � 7 yrs)
Affects all races and both sexes equally
Usually associated with URTI
21. Pharyngitis Causes:
Viral: rhinovirus, adenovirus, EBV, HSV, influenza virus
Bacterial: GABHS
Other: allergy, trauma, toxins, neoplasia
Predisposing factors:
Smoking (including passive)
Mouth breathing
Rhinosinusitis
Periodontal disease
Viral: self limiting
Bac.: self limiting, concerns about suppurative and non-suppurative complicationsViral: self limiting
Bac.: self limiting, concerns about suppurative and non-suppurative complications
22. Pharyngitis Pathophysiology:
Viral and bacterial directly invades the mucosa causing local inflammatory response.
Some viruses causes inflammation to the mucosa secondary to nasal secretion
23. Pharyngitis Symptoms:
Sore throat is the main CCx
Fever, headache
Acute: rapid onset, short duration, with dysphagia and malaise
Chronic: persistent, mild soreness, dryness. Eliminate underlying cause.
Signs:
Edema and erythema of the pharynx
Exudate can be present Edema does not correlate with the degree of sore throatEdema does not correlate with the degree of sore throat
24. Pharyngitis Bacterial Exposure to known carrier
High fever, chills, headache, abdominal pain
Painful cervical adenopathy
Rare pathogen < 2 yrs
Viral Involvement of other mucous membrane
With sneezing, rhinorrhea and cough
27. Phryngitis/Complications Usually self limiting
Primary concern in children (3 � 18 yrs) is that untreated GABHS may cause rheumatic fever
Adjacent organs: otitis media, sinusitis, peritonsillar abscess
Acute respiratory inflammation
Acute glomerulonephritis
Toxic shock syndrome
Mortality due to airway obstruction (rare)
29. Pharyngitis/DDx
Streptococcal pharyngitis
Non-infectious pharyngitis
Peritonsilar abscess
Pharyngeal candidia
Diphtheria
30. Pharyngitis/RRx Symptomatic
Rest, oral-fluids, and salt-water gargling are the main supportive measures
Paracetamol (Acetaminophen) is the DOC in high pain and fever
Antibiotics are indicated for clinically suspected and culture or antigen verified GAS infection. Prevent rheumatic fever if given 9 days from onset