Blood cells Disorders
170 likes | 397 Views
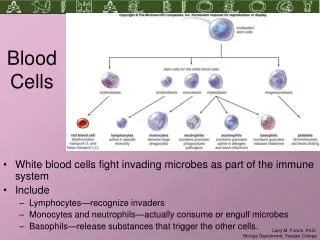
Blood cells Disorders. Leucocytosis: A raised WBCs count. Due to elevation of a single lineage. Neutophilia: Physiologic causes: Pregnancy, newborns, after parturition or after exercise.

Blood cells Disorders
E N D
Presentation Transcript
Blood cells Disorders Leucocytosis: A raised WBCs count. Due to elevation of a single lineage. • Neutophilia: • Physiologic causes:Pregnancy, newborns, after parturition or after exercise. • Pathological causes:1- Infections: pyogenic bacteria.2- Neoplasia: all types.3- Hge / haemolysis.4- Corticosteroids. Dr. Rania Alhady
Leucocytosis Left shift: A "left shift" refers to the presence of increased proportions of younger, less well differentiated neutrophils and neutrophil-precursor cells in the blood. A severe neutrophilia with left shift is referred to as a leukemoid reaction. Neutophilia may be associated with the presence of toxic granulations and Dohle bodies. Dr. Rania Alhady
Leucocytosis • Eosinophilia: Eosinophilia is a condition in which the eosinophil count in the peripheral blood exceeds 450/ cm in P.B. Causes: 1- Allergic disorders • Asthma • Drug allergies • Allergic skin diseases 2- Parasitic infections 3- Some forms of malignancy • Hodgkin's lymphoma • Some forms of Non-Hodgkin lymphoma 3- Systemic autoimmune diseases(e.g. SLE) Dr. Rania Alhady
Leucocytosis • Monocytosis: An increase in the number of monocytes circulating in the blood Causes: • Chronic inflammation: tuberculosis, syphilis and malaria • Blood and immune causes: Myeloproliferativedisorders. • Malignancies: Certain leukaemias, such as chronic myelomonocyticleukaemia (CMML) and monocyticleukemia. • Basophilia: Causes: • Infections: Pox virus (chicken pox, small pox) • Neoplasia: MPD (myeloproloferative disorders). Dr. Rania Alhady
Leucocytosis • Lymphocytosis: Increase in the number or proportion of lymphocytes in the blood. Causes: 1. Infections: • Acute viral infections: infectious mononucleosis (glandular fever), hepatitis, herpes virus, and Cytomegalovirus infection • Acute bacterial infections: T.B., scarlet fever, typhoid fever. • Protozoal infections: toxoplasmosis and malaria • Chronic lymphocytic leukemia (CLL). • Acute lymphoblastic leukemia (ALL). Lymphocytosis, peripheral blood smear Dr. Rania Alhady
Leucopenia Leucopenia: Reduced total leucocytic count. Neutropenia: Reduced neutrophil count < 2000 / cm Classification: Classify the severity of neutropenia based on the absolute neutrophil count (ANC) measured in cells per microliter of blood: Mild neutropenia: minimal risk of infection Moderate neutropenia: moderate risk of infection Severe neutropenia: severe risk of infection. Signs and symptoms Neutropenia can go undetected, but is generally discovered when a patient has developed severe infections or sepsis. Feversand frequent infections. These infections can result in conditions such as mouth ulcers, diarrhea, a burning sensation during urinating, or a sore throat. Dr. Rania Alhady
Leucopenia Causes of Neutropenia: Causes can be divided into the following groups: • Decreased production in the bone marrow due to: • Aplastic anemia • Cancer, particularly blood cancers • Certain medications • Radiation Blood film with a striking absence of neutrophils, • Increased destruction:leaving only red blood cells and platelets • Autoimmune neutropenia: (occur with: SLE, R.A., Hodgkin disease, Felty syndrome) {Felty syndrome: R.A., splenomegally, prominent neutropenia, lymphopenia} • Chemotherapy treatments, such as for cancer and autoimmune diseases Dr. Rania Alhady
Leucopenia • Drugs induced neutopenia: Medications are very common cause of neutropenia.such a Flecainide (anti-arrhythmic drug) Once drugs stopped, neutrophil recovery in 4 -7 days occur provided that precursors cells are normal. • Congenital neutropenia syndromes:1- Kostmann‘s Syndrome: • Severe chronic neutropenia with frequent pyogenic infections. • Eosinophil and basophils are normal or increased. • Progression of leukemia (Very poor prognosis) • Marrow transplantation may be curative. Dr. Rania Alhady
Leucopenia 2-Chediak-Higashi Syndrome: • Oculocutaneous albinism • Photophobia • Sun sensitivity • Neuropathy • Recurrent Infections, esp Staph aureus • Granules in granulocytes, monocytes and lymphocytes • Treatment: BMT 3- Reticular Dysgenesis: • Thymic aplasia. • Inability to produce neutrophil. • Patient die at early age from bacterial and viral infections. • BMT should be considered Dr. Rania Alhady
Thrombocytopenia Thrombocytopenia or thrombopenia: is a relative decrease of platelets in blood Symptoms and signs: Bruising, particularly purpura in the forearms, petechia (pinpoint hemorrhages on skin and mucous membranes), nosebleeds and/or bleeding gums. PURPURADefined as: - A purplish discoloration of the skin and mucous membrane due to subcutaneous and sub mucous extravasation of blood. - Purpuramay be due to deficient and defective platelets or due to an unexplained increase in capillary fragility Dr. Rania Alhady
Thrombocytopenia Causes: Increased platelets destruction: (I) Immune Thrombocytopenia: 1. Auto-Abs • ITP (Immune Thrombocytopenic Purpura) • 2ry to SLE & AIDS 2. Allo-Abs • Post- transfusion • Post- natal • Post transplatation 3.Drug – induced: e.g. Quinin, sulphonamide Dr. Rania Alhady
Thrombocytopenia (II) Non – Immune Thrombocytopenia: • 1. Excess platelet consumption (DIC) • 2. TTP- HUS • 3. Sever burn or snake venom • 4. Structural platelet defects (short life span) Immune thrombocytopenic purpura (ITP): Immune disorder characterized by: • Thrombocytopenia. • B.M.: normal with normal megakaryocytes in number, or even increased number with defective budding. • Evidence of Abs against platelets • Spleen in NOT enlarged. Dr. Rania Alhady
Thrombocytopenia Dr. Rania Alhady
Thrombocytopenia Thrombotic Thrombocytopenic Purpura. Hemolytic – Uremic Syndrome: 1. Idiopathic TTP-HUS: A syndrome characterized by: 1. Neurological abnormalities 2. Thrombocytopenia 3. Microangiopathic hemolytic anemia 4. Renal involvement 5. Fever 2. 2ry TTP-HUS: Causes: 1. Pregnancy 2. Cancer assiociated 3. Drugs e.g. Cyclosporin 4. Marrow Transplantation Dr. Rania Alhady