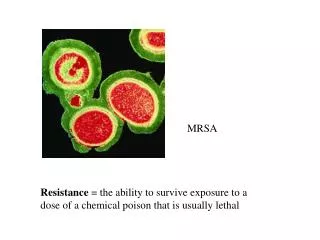
MRSA
MRSA. Dorothy MacEachern, MS, MPH October 2007 509.324.1569. What is MRSA?. Methicillin-resistant Staphylococcus aureus Staphylococcus aureus , often called “staph” is a bacteria commonly found on skin and in the nose. A person can self-inoculate cuts or wounds.

MRSA
E N D
Presentation Transcript
MRSA Dorothy MacEachern, MS, MPH October 2007 509.324.1569
What is MRSA? • Methicillin-resistant Staphylococcus aureus Staphylococcus aureus, often called “staph”is a bacteria commonly found on skin and in the nose. A person can self-inoculate cuts or wounds. • (A staph infection that is) resistant to methicillin and other common antibiotics.
Spectrum of Staphylococcal Effects • Harmless inhabitant of nose/skin (colonization)> • Auto inoculation of cuts or wounds > • Skin infections, folliculitis, impetigo, boils, etc.> • Abscesses, cellulitis, sinusitis > • Osteomyelitis, arthritis, pneumonia > • Endocarditis, meningitis, septicemia
History of MRSA • Penicillin resistant staph appeared in 1942. • Methicillin introduced in 1959. • Methicillin resistant staph appeared in United Kingdom in the 1960s. • United States saw first MRSA cases in 1968, usually in hospital settings, and it spread through health care facilities in the 1970s. Healthcare acquired (HA-MRSA)
HA-MRSA Associated Risk Factors • prolonged stays in hospital settings (esp. ICUs or Burn Units) or long term care settings. • broken skin, from surgical wounds or pressure ulcers. • recent use of antibiotics, especially prolonged or broad spectrum antibiotics. • severe underlying illness. Generally transmitted by health care workers.
MRSA Shows up in the Community • 1980 Injection drug users • 1990s Children in child care • 1990s Native Americans • 1990s Prison and jail populations • 1999 Urban homeless populations Usually these were people who had no recent contact with health care facilities.
CA-MRSA Associated Risk Factors • Recent antibiotic use • Injection Drug Use • Incarceration • Contact Sports • close skin-to-skin contact • openings in the skin such as cuts or abrasions • contaminated items and surfaces • crowded living conditions • poor hygiene • sharing personal items Transmission within households is common.
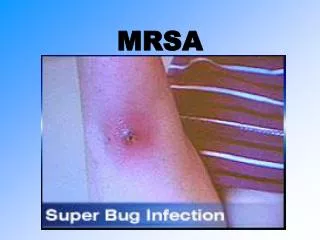
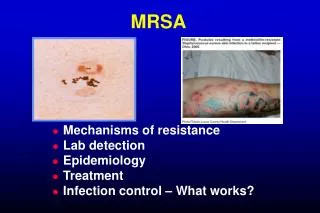
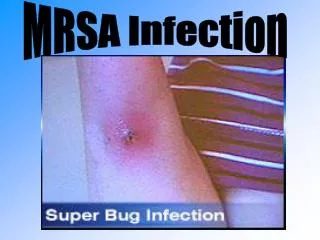
MRSA Infections • Most often occur in skin and soft tissue.
How are MRSA skin infections treated? • At home: • Wash with soap and water • Apply an over-the counter antibiotic cream • Cover with a bandage, if possible • If wound is not healing, see a health care provider: • A health care provider may: • drain the infection and/or • prescribe an antibiotic based on culture results
MRSA spreads 2 ways: • Direct contact – skin to skin contact, or contact with drainage • Example: Shaking hands • Indirect contact – touching contaminated objects and then touching skin or membranes • Example: Touching a door handle, then touching broken skin
Hand Hygiene The single most effective practice to reduce the spread of infection. • Use warm water and soap. Wash for 20 seconds. • Use a paper towel to turn off water and open door. • Antiseptic gels are great when soap and water are not available! • Use one with a concentration of >60% ethyl alcohol.
Clean & Disinfect Surfaces • Clean first – remove soil w/soap and water • Disinfect – wipe down surfaces with an EPA-approved disinfectant effective against staph, such as: • Solution of 1 T bleach in 1 quart of water • Clorox or Lysol wipes
Help reduce the spread of MRSA at home • Do not share personal items (razors, clippers, towels, etc.) • Care for and cover wounds. • If a wound is not healing, see a health care provider. • If a wound is draining and cannot be covered and contained, stay home! • Wash your hands well. Wash your hands often. • Clean and disinfect surfaces often, especially in high traffic areas. • Take prescribed antibiotics appropriately.
Help reduce the spread of MRSA in public settings • Shower • After using public gym equipment • After using sauna/pool benches • After participating in sports practice or competition • Use barriers • Gloves for cleaning • Towels on equipment/benches • Clean and disinfect surfaces
Help reduce the spread of MRSA in school • Encourage students & staff to wash their hands regularly • Clean and disinfect: • Sports equipment such as wrestling gear (after each use), floor mats (before and after each practice session) AND • Surfaces that come in direct contact with skin such as phones & keyboards, desktops, tables, door knobs, light switches (daily)
So, remember • Wash your hands well. Wash your hands often. • Do not share personal items. • Keep cuts covered. • Seek medical care for non-healing skin infections. • Take prescribed antibiotics as directed. • Clean and disinfect surfaces regularly.
Great resources for MRSA info: • http://www.tpchd.org/page.php?id=12 • http://www.doh.wa.gov/Topics/Antibiotics/MRSA • http://www.cdc.gov/ncidod/dhqp/ar_mrsa_ca.html • Your local health department!