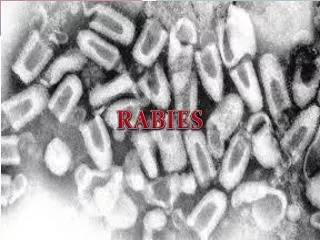
Tetanus & Rabies
Tetanus & Rabies. Chapt. 146-147 January 12, 2005 Dr. Kiss slides by Scott Gunderson PGY-2. Tetanus – Epidemiology. Uncommon in the US but not worldwide 1 million cases worldwide per year Mortality rate of 20-50% Highest prevalence in developing countries. Epidemiology.

Tetanus & Rabies
E N D
Presentation Transcript
Tetanus & Rabies Chapt. 146-147 January 12, 2005 Dr. Kiss slides by Scott Gunderson PGY-2
Tetanus – Epidemiology • Uncommon in the US but not worldwide • 1 million cases worldwide per year • Mortality rate of 20-50% • Highest prevalence in developing countries
Epidemiology • Fewer than 50 cases per year in the US • Majority of cases in temperate climates (Texas, California, and Florida) • Mortality rate of 11% • Most who develop it have an inadequate immunization history • Only 27% of Americans older than age 70 have adequate immunity to tetanus
Pathophysiology • Wound contamination with Clostridium tetani • Motile, nonencapsulated, anaerobic, gram positive rod • Spore forming and ubiquitous in soil and animal feces
Pathophysiology • Usually introduced in the spore forming state, then germinates to the toxin producing vegetative form • Requires decreased tissue oxygen tension to germinate • Vegetative state produces two exotoxins • Tetanolysin • Tetanospasmin
Toxins • Tetanolysin – clinically insignificant • Tetanospasmin • Neurotoxin responsible for the clinical manifestations of tetanus • Reaches peripheral nerves by hematogenous spread and retrograde intraneuronal transport • Does not cross blood brain barrier • Reaches CNS by retrograde transport
Tetanospasmin • Acts on the motor end plates of skeletal muscle, in the spinal cord, and in the sympathetic nervous system • Prevents release of inhibitory neurotransmitters glycine and gamma-aminobutyric acid (GABA)
Clinical Features • Tetanospasmin responsible for generalized muscular rigidity, violent muscular contractions, and instability of the ANS. • Typical wound is a puncture, but no wound is identified in up to 10% • Other routes are surgical procedures, otitis media, abortion, umbilical stump and drug abusers
Four Clinical Forms • Local • Generalized • Cephalic • Neonatal
Local Tetanus • Rigidity of the muscles in proximity to the site of injury • Usually resolves completely in weeks to months • May develop into generalized
Generalized Tetanus • Most common form • Most common presenting complaint is pain and stiffness of the masseter muscles (Lockjaw) • Short axon nerves affected initially therefore starts in the face, then neck, trunk, and extremities
Generalized Tetanus • Muscle stiffness leads to rigidity • Trismus and characteristic sardonic smile develops (risus sardonicus) • Reflex convulsive spasms and tonic muscle contraction create dysphasia, opisthotonos (arching of back and neck), flexing arms, clenching fists, and lower extremity extension
Generalized Tetanus • Autonomic nervous system • Hypersympathetic state • Usually in the second week • Tachycardia • HTN • Diaphoresis • Increased urinary catecholamines • Significant morbidity and mortality
Cephalic Tetanus • Results from an injury to the head or otitis media • Cranial nerves affected most commonly the seventh • Poor prognosis
Neonatal Tetanus • 400,000 worldwide deaths annually • Results from inadequately immunized mothers • Frequent after unsterile treatment of the cord stump
Neonatal Tetanus • Signs • Weakness • Irritability • Inability to suck • Presents in the 2nd week of life
Diagnosis • Clinical diagnosis • No laboratory confirmatory tests • Wound cultures not very useful as C. tetani may be recovered without tetanus • Immunization history usually unknown or inadequate
Strychnine poisoning Dystonic reaction Hypocalcemic tetany Peritonsillar abscess Peritonitis Meningeal irritation Rabies TMJ Tetanus Ddx
Treatment • Admit to ICU • Be prepared for intubation with neuromuscular blockade as respiratory compromise may develop • Minimal environmental stimuli to avoid reflex convulsive spasms • Initial wound debridement to improve oxygenation
Treatment • Tetanus Immunoglobulin (TIG) • Neutralizes wound and circulating tetanospasmin • Does not neutralize toxin already bound to the nervous system • Does not improve clinical symptoms • Decreases mortality
Treatment • TIG • Usual dose is 3,000 to 6,000 units • Administered IM opposite side as Td given • Give before wound debridement
Treatment • Antibiotics • Questionable utility but usually given • Metronidazole • antibiotic of choice • Avoid penicillin • it is a GABAA antagonist and may worse symptoms
Treatment • Muscle relaxants • Tetanospasmin • prevents neurotransmitter release at inhibitory interneurons and therapy of tetanus is aimed at restoring balance • Midazolam • preferred agent as it is water soluble • Baclofen • specific GABAB agonist that has also been used
Treatment • Neuromuscular blockade • Blockade often required to allow respiration and to prevent fractures and rhabdomyolysis • Succinylcholine • recommended for initial airway management • Vecuronium • treatment of choice for long term blockade
Treatment • ANS dysfunction treatment • Labetalol • useful for treatment due to combined alpha and beta activity • Magnesium sulfate • inhibits the release of epinephrine and norepinephrine from the adrenal glands • Clonidine • central alpha receptor agonist for cardiac stability
Immunization • Disease does not confer immunity so those that recover must undergo immunization • Tetanus toxoid • 0.5 cc IM at presentation, 6 weeks, and 6 months • Local reactions are common • Less common serous reactions include urticaria, anaphylaxis, or neurologic complications
Immunization and TIG guide • Td dose: 0.5cc IM • TIG dose: 250 U IM • DPT given if under 7, Td given if over 7
Rabies • Rabies ranks number 10 worldwide as a cause of mortality • 50,000 – 60,000 deaths annually worldwide • Rare human cases in US but 35,000 people provided prophylaxis annually
Microbiology • Lyssavirus genus prototype • Single-stranded, negative-sense, nonsegmented RNA • 7 rabies groups in genus • Classic rabies virus – common rabies • 6 others with less than 10 reported human cases of disease
Pathophysiology • Virus course • Initial uptake of virus by monocytes in 48-96 hours • Crosses motor end-plate to travel up the axon to the dorsal root ganglia to the spinal cord and the CNS • Then spreads outward via peripheral nerves to infect almost all tissue of the body
Pathophysiology • Histologically resembles other encephalitis • Monocellular infiltration with focal hemorrhage • Demyelination • Perivascular gray matter • Basal ganglia • Spinal cord • Negri bodies • Eosinophilic intracellular lesions in cerebral neurons • Highly specific for rabies • Present in 75% of rabies cases
Epidemiology • Primarily a disease of animals • Human cases reflect the prevalence in animals and degree of human contact with them • Major vectors include • Dogs • Foxes • Raccoons • Skunks • Coyotes • Mongooses • bats
Wild animals (93%) Raccoons (37.7%) Skunks (30.2%) Bats (16.8%) Foxes (6.2%) Others (2.2%) Domestic animals (7%) Cats (3.4%) Dogs (1.6%) Cattle (1.1%) Horses, donkeys, mules (0.71%) Sheep, goats, camels (0.15%) Others and ferrets (0.06%) Epidemiology 7,369 cases of animal rabies in the US in 2000
http://www.cdc.gov/ncidod/dvrd/rabies/Epidemiology/Epidemiology.htmhttp://www.cdc.gov/ncidod/dvrd/rabies/Epidemiology/Epidemiology.htm
http://www.cdc.gov/ncidod/dvrd/rabies/Epidemiology/Epidemiology.htmhttp://www.cdc.gov/ncidod/dvrd/rabies/Epidemiology/Epidemiology.htm
Epidemiology • Dogs • Less than 5% of animal cases in US, Canada and Europe • Greater than 90% of animal cases in developing countries • Very rare documented rabies in: • Squirrels, hamsters, guinea pigs, gerbils, chipmunks, rats, mice, domesticated rabbits and other small rodents • Almost never requires post exposure prophylaxis
Epidemiology • Transmission • Saliva though bite of an rabid animal most common • Aerosolized in bat caves • Mucus membrane transmission also reported • Bites and scratches • Risk of developing rabies dependant on the location injury, depth, an number of bites
Infection Risk • Risk of infection
Epidemiology • 32 cases reported from 1980 to 1996 in the US • 7 had a known animal bite • 6 dog bites in a foreign country • 1 bat bite • Animal contact identified in 12 • 8 with a bat • 2 with a dog • 1 with a cow • 1 with a cat • No identifiable source in the other 13
Preexposure Prophylaxis • Prophylaxis • Individuals with occupations or recreation that place them at risk should receive the series • 4 shot series with booster shots required • Does not eliminate need for postexposure prophylaxis • No need for HRIG and less doses of vaccine
Postexposure Prophylaxis • Indicated for all persons possibly exposed to a rabid animal • Exposure is a bite, scratch, abrasion, open wounds, or mucous membrane exposure • Contact alone, and contact with blood, urine, or feces does not constitute and exposure • Cleansing wound with 20% soap and water has been show in experimental animals to markedly reduce the rate of infection
Bats • Increasingly important wildlife vectors of transmission of rabies • All cases of possible bat bites the bat should be collected and tested for rabies • Bat unavailable • Begin postexposure prophylaxis
Dogs, Cats, and Ferrets • Observation • CDC recommends 10 days of observation of a healthy dog, cat, or ferret after a bite • Normal behavior • No action needed • Unusual behavior • Sacrifice animal, test for rabies, and initiate HRIG and vaccine • Positive – Complete course of vaccine • Negative – Discontinue course