Total Knee Replacement
Total Knee Replacement. General anatomical overview What is TKR Knee implant components Types of knee joint prosthesis Implant materials material criteria Cemented and Cementless Implants Benefits of knee replacement surgery Indications for TKR. Contents. Risk factors leading to TKR

Total Knee Replacement
E N D
Presentation Transcript
General anatomical overview • What is TKR • Knee implant components • Types of knee joint prosthesis • Implant materials • material criteria • Cemented and Cementless Implants • Benefits of knee replacement surgery • Indications for TKR Contents
Risk factors leading to TKR • Diagnosis • Contraindications for TKR • TKR surgical procedure • Surgical technique • Complications after Surgery • Rehabilitation Exercise Protocols • Home exercises • Precautions after TKR
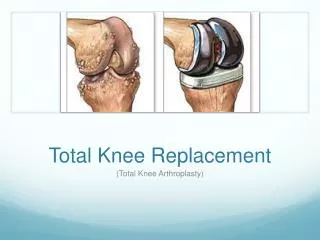
Knee replacement surgery involves replacing some or all of the components of the knee joint with a synthetic implant, to repair the damaged weight-bearing surfaces that are causing pain. • A total knee replacement surgery replaces all three compartments of the diseased knee joint. A partial knee replacement involves an implant in just one or two compartments of the knee, retaining any undamaged parts.
Up to three bone surfaces may be replaced in a total knee replacement: • The lower ends of the femur. • The top surface of the tibia. • The back surface of the patella. * helps improve outcomes and pain free functions Knee implant components
Posterior-Stabilized Designs • Cruciate-Retaining Designs • Unicompartmental Implants
Fixed-Bearing Prosthesis • Mobile-Bearing Prosthesis Types of knee joint prosthesis
Metal parts of the implant: made of titanium or cobalt-chromium based alloys. • Plastic parts: made of ultra high molecular weight polyethylene. • All together, the components weigh between 15 and 20 ounces, depending on the size selected. Implant Materials
They must be biocompatible; should not be creating a rejection response. • Strong enough to take weight bearing loads • Able to move smoothly against each other as required. • Able to retain their strength and shape for a long time. Material Criteria
Cemented fixation: uses a fast-curing bone cement (polymethylmethacrylate). Cobalt-chromium alloy femur articulating with standard polyethylene tibial surface is most common • Cementless fixation: relies on new bone growing into the surface of the implant for fixation. Cementless implants are made of a material that attracts new bone growth. Most are textured or coated so that the new bone actually grows into the surface of the implant. Cemented and Cementless Implants
Hybrid fixation: for total knee replacement, the femoral component is inserted without cement, and the tibial and patellar components are inserted with cement.
Elimination of pain. • Improved range of motion. Benefits of knee replacement surgery
Osteoarthritis • Rheumatoid arthritis • Trauma: Damage to the knee from a fall, automobile accident, or workplace or athletic injury Indications for TKR
Genetic: Both OA and RA tend to run in families. • Age: Knee cartilage becomes thinner and weaker. • Sex: Women athletes have three times as many knee injuries as men. • Biomechanical: Certain types of leg or foot deformities, such as bowlegs or difference in leg length, are at increased risk of knee disorders because the stresses on the knee joint are not distributed normally. Risk factors leading to TKR
Gait-related factors: Irregular walking patterns . • Shoes: High heels, Poorly fitted or worn-out shoes contribute to knee strain by increasing the force transmitted upward to the knee when the foot strikes the sidewalk or other hard surface. • Work or other activities that involve jumping, jogging, or squatting: Tends to loosen the ligaments that hold the parts of the knee joint in alignment
Patient history General medical history, but also about the patient's occupation, exercise habits, past injuries to the knee, and any gait-related problems and patient's ability to move or flex the knee • Diagnostic tests Physical examination of the knee: signs of inflammation, abnormal postures, gait abnormality and ROM Diagnosis
Imaging studies X-ray, CT Scan or MRI • Aspiration Blood in the fluid usually indicates a fracture or torn ligament; the presence of bacteria indicates infection; the presence of uric acid crystals indicates gout. Clear, straw-colored fluid suggests osteoarthritis. • Arthroscopy Drain fluid from the knee. Sterile saline fluid is pumped into the knee to enlarge the joint space and make it easier for the surgeon to view the knee structures and to cut, smooth, or repair damaged tissue.
Knee sepsis • A remote source of ongoing infection • Extensor mechanism dysfunction • Severe vascular disease • Recurvatum deformity secondary to muscular weakness • Presence of a well-functioning knee arthrodesis Contraindications for TKR
Skin conditions within the field of surgery (eg, psoriasis) • Past history of osteomyelitis around the knee • Neuropathic joint • Obesity
Shorter incision • Quadriceps sparing • Early, limited results: • Better ROM • Less blood loss • Shorter LOS • Less need for assistive devices at 2 weeks post-op Surgical techniqueMinimally invasive TKA
Infection • Blood clot/deep vein thrombosis • Implant loosening • Implant breakage- The most common components to break are the plastic tibial, or shinbone, spacer and the patella, or kneecap, implant, which is also plastic. • Excessive joint stiffness Complications after Surgery
Pre.op (1-2 weeks prior to surgery) • Education on the surgical process and outcomes • Instruction on a post. op exercise program • Assessment of the home environment Rehabilitation Exercise Protocols
Post. Op day 1 • Bedside exercises: ankle pumps, quadriceps sets, gluteal sets • Review of weight bearing status • Bed mobility and transfer training: bed to/from chair
Post. op day 2 • Exercises for active ROM, AAROM, and terminal knee extension • Strengthening exercises:
Gait training with an assistive device and functional transfer training: sit to/from stand, toilet transfers bed mobility
Post .op day 3-5/on discharge to the rehabilitation unit • Progression of ROM and strengthening exercises to the patient tolerance • Progression of ambulation on level surfaces and stairs (if applicable) with the least restrictive device • Progression of ADL training
Post. op day 5- 4 weeks • Strengthening exercises: long arc quads/seated leg extension, standing hip abduction and extension, knee bends, short arc quads • Strengthening of quadriceps and hamstring muscles • progression of ambulation distance • Progression of independence with ADL
Quadriceps sets • Ankle pumps • Straight leg raises • Supported leg raise • Prone knee flexion • Standing knee curls • Stepups • Stationary cycling Home exercises
Do not attempt to do these exercises unless your doctor or physical therapist has given consent to do so • Doing advanced exercises too early in your rehabilitation can damage the prosthesis as well as set your recovery back • Avoid exercises that are not prescribed by your doctor, especially those that place excessive pressure on the knee joint, such as lunges or squats. Precautions after TKR
Knee Society recommendations: • Suitable: cycling, swimming, low-resistance rowing, walking, hiking, low-resistance weight-lifting, ballroom dancing, square dancing • Suitable but more risky: downhill skiing, ice-skating, speed walking, hunting, low-impact aerobics, volleyball • Avoid: Baseball, basketball, football, hockey, soccer, high-impact aerobics, jogging, parachuting, power-lifting Sports & activity recommendations