ABSTRACT
Comparing Cleaning and Disinfection using the Traditional Cloth and Bucket Method versus the Ready to Use Wipe Method: Process Compliance and Time-Related Costs

ABSTRACT
E N D
Presentation Transcript
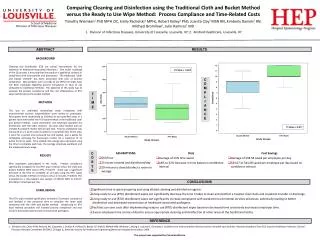
Comparing Cleaning and Disinfection using the Traditional Cloth and Bucket Method versus the Ready to Use Wipe Method: Process Compliance and Time-Related Costs Timothy Wiemken1PhD MPH CIC, Emily Pacholski1MPHc, Robert Kelley1PhD, Juanita Clay2MSN RN, Kimberly Daniels2RN, Michael Bromilow2, Julio Ramirez1MD 1. Division of Infectious Diseases, University of Louisville, Louisville, KY; 2. Kindred Healthcare, Louisville, KY ABSTRACT RESULTS • BACKGROUND • Cleaning and disinfection (CD) are critical interventions for the reduction of healthcare-associated infections.1One major challenge of the CD process is ensuring that the product is applied to surfaces in compliance with local policies and procedures. The traditional “cloth and bucket method” has been associated with lack of process compliance. New products such as ready to use (RTU) CD wipes have not been evaluated regarding process compliance or ease of use compared to traditional methods. The objective of this study was to evaluate the process compliance and the cost effectiveness of RTU wipe method versus the bucket method. • METHODS • This was an unblinded randomized study. Employees with environmental services responsibilities were invited to participate. Participants were randomized to disinfect six pre-specified areas in a patient room with either the RTU wipe method or the traditional cloth and bucket method. Upon completion, the employee repeated the disinfection with the other method. All areas were marked with an invisible fluorescent marker before each task. Process compliance was measured on a 3 point scale: 0 points for a complete miss of the area, 1 point for a partial miss (smeared but still visible), and 2 points for completely removing the fluorescent marker, for a maximum of 12 points for all six tasks. Time-related cost savings were calculated using the time to complete each task, the average employee workload, and the employee hourly wage. • RESULTS • Nine employees participated in the study. Process compliance significantly increased for the RTU wipe method versus the cloth and bucket method (92% versus 67%, P=0.017). There was a significant decrease in the time to complete all six tasks using the RTU wipes versus the bucket method (3 minutes versus 4 minutes, P=0.003). This translated to a time-related cost savings of $38.58 (95% CI $34.07-$41.08) per employee per day. • CONCLUSIONS • The RTU wipe method significantly increased CD process compliance and resulted in less personnel time to complete the same tasks compared with the cloth and bucket method. Introducing an RTU wipe method procedure will increase process compliance and may result in decreased transmission of nosocomial pathogens. C O M P T L I I M A E N C E • ASSUMPTIONS • $10/hour • 15 rooms cleaned and disinfected/day • 20 minues to clean/disinfect a room on average • Data • Average of 23% time saved • 18% to 32% decrease in time based on confidence interval • Cost Savings • Average of $38.58 saved per employee per day • $34.07 to $41.08 saved per employee per day based on confidence interval C O S T S CONCLUSIONS • Significant time is spent preparing and using diluted cleaning and disinfection agents. • Using ready to use (RTU) disinfectant wipes can significantly decrease the time it takes to clean and disinfect a hospital room daily and at patient transfer or discharge. • Using ready to use (RTU) disinfectant wipes can significantly increase compliance with standard environmental services processes, potentially leading to better disinfection and decreased transmission of healthcare associated pathogens. • Facilities can save costs after implementing ready to use (RTU) disinfectant wipes based on decreased time constraints and excess employee time. • Excess employee time can be utilized to ensure appropriate cleaning and disinfection of other areas of the healthcare facility. REFERENCE SehulsterLM, Chinn RYW, Arduino MJ, Carpenter J, Donlan R, Ashford D, Besser R, Fields B, McNeil MM, Whitney C, Wong S, Juranek D, Cleveland J. Guidelines for environmental infection control in health-care facilities. Recommendations from CDC and the Healthcare Infection Control Practices Advisory Committee (HICPAC). Chicago IL; American Society for Healthcare Engineering/American Hospital Association; 2004. This project was supported by Clorox Healthcare