High-Resolution Optical Coherence Tomography for Early Detection of Epithelial Neoplasia
This study investigates the application of Optical Coherence Tomography (OCT) as a non-invasive tool to assess epithelial neoplasia progression in the hamster cheek pouch model for oral cancer. We evaluated morphological changes captured by OCT against histological findings using DMBA carcinogen modeling. The OCT system demonstrated the ability to visualize mucosal layers and correlated with histopathological changes, making it a promising technique for early detection of oral dysplasia and neoplasia. Results indicate the potential of OCT in local staging and monitoring treatment responses.

High-Resolution Optical Coherence Tomography for Early Detection of Epithelial Neoplasia
E N D
Presentation Transcript
HIGH RESOLUTION OPTICAL COHERENCE TOMOGRAPHY FOR EARLY DETECTION OF EPITHELIAL NEOPLASTIC TRANSFORMATION Asem Ahmed ElFert *, Pankaj Jay Pasricha *, Brent Bell **, Richard Johnigan , Shu-Yuan Xiao , Karen H. Calhoun , Massoud Motamedi** Division of Gastroenterology *, Biomedical Engineering Center**, Department of Pathology, and Department of Otolaryngology , University of Texas Medical Branch at Galveston,Texas, USA
Abstract • Optical coherence tomography (OCT) is a new high spatial-resolution, optical imaging system that can be used endoscopically. The aim of this study was to examine the potential application of OCT to non-invasively assess the progression of epithelial neoplasia in hamsters’ cheek pouch model for oral cancer by comparing the observed morphological changes in tissue as detected by OCT to that of histological findings. • 20 adult male Syrian hamsters were studied. The right cheek pouch was painted with the carcinogen 0.5% 9,10-dimethyl-1, 2-benzanthrcene (DMBA) 3 times a week. Going from the sixth week onwards, 4 hamsters were randomly chosen and examined weekly. Areas with small suspicious lesions as well as apparently normal spots were examined with our prototype OCT scanning system. Areas with fungating cancer were avoided. The scanned areas were marked, biopsied and histological sections were then compared with the OCT images. • For comparison, we have also examined 6 more hamsters, the right cheek pouch of 3 of them were painted with sodium lauryl sulphate (SLS) daily for 4 consecutive days to produce inflammation and the other 3 were untreated. On the fifth day, the cheek pouches of all of them were scanned with OCT and the scanned areas were marked and biopsied. • OCT imaging clearly showed the three wall layers of the normal cheek mucosa. It also significantly correlated with the histological findings in both the inflammation model and the cancer model ranging from hyperplasia to carcinoma in situ. In inflammation model, we found slightly increased thickness and brightness of the mucosal layer with clearly defined straight underlying layers comparable to histologically diagnosed hyperplasia. In cancer model, we found increased mucosal thickness and heterogeneous brightness and wavy but well-preserved underlying layers. These changes increased in proportion with the grade of histologically diagnosed dysplasia. For detection of grossly invisible lesions, OCT had a sensitivity of 58.6% and a specificity of 75%. Although our model had no cases of invasive or microinvasive cancer, the degree of resolution suggests that OCT has the potential for local staging of mucosal cancer. • As new methods are continuously needed to increase the accuracy of T-staging, OCT may offer a great potential in cases of Carcinoma in situ and dysplasia that are difficult to be diagnosed using EUS. OCT will not replace EUS especially in nodal staging or to define local metastasis. These technologies will complement one another.
Background • Optical coherence tomography (OCT) is a method of imaging the internal cross-sectional microstructure of tissues using measurements of optical backscattering or backreflection.1 • OCT is based on the principle of interferometry. In its simplest form, light from a source is divided into two identical beams. While one beam is directed into the target tissue, the other beam is directed toward a moveable reference mirror whose location can accurately be measured. When the light backscattered from the tissue and reflected from the mirror reach the detector at the same time, an interference signal is noted. Signal processing algorithms transform interference patterns into images that can be displayed in real time.2 • OCT can provide images of tissue on the micrometer scale in situ and in real time. 3 • Pitris et al. (2000) were able to detect changes in the mucosal/submucosal microstructure in various parts of the gastrointestinal tract including normal esophagus, Barrett’s esophagus, esophageal adenocarcinoma, normal colon, ulcerative colitis, and colon carcinoma.4 • OCT is now an established optical biopsy method, imaging 2-3 mm into opaque tissue. It is analogous to ‘ultrasound’ but has an outstanding resolution. 5
Aim of the work • The aim of this study was to test the ability of OCT to monitor the progression of oral mucosal cancer in early stages of precancerous development and the correlation with histopathology. • Also, in our randomized blinded study, we aimed to set some parameters for OCT scanning of normal, inflammatory and early neoplastic mucosa.
Methods • Twenty adult male golden Syrian hamsters (Mesocricetus auratus) 10 weeks old were housed three per cage and fed standard laboratory chow and water ad libitum. Under light Isoflourane anesthesia, multiple applications of 0.5% 9,10-dimethyl-1, 2-benzanthrcene (DMBA) in acetone on the right cheek pouch using a No. 3 sable hair brush were done three times a week. This painting was done with inserting the brush into the gently lifted pouch without exposing it. • To monitor the progression of preccancerous lesions, we have divided them into 5 random groups, examining 4 hamsters weekly between 6 and 10 weeks of continuous painting. • Using ketamine & Xyalzine intraperitoneal injection, the right cheeck pouch was exposed, stretched, washed and fixed with hair pins, then examined using fixed OCT probe. • To differentiate the OCT changes of precancerous development from inflammatory changes, we have induced pure inflammation in the right cheek pouch of 3 more hamsters, by painting them with sodium lauryl sulphate (SLS) daily for 4 consecutive days. On the fifth day, all of them were examined with OCT. • We have also examined the normal right cheek pouch of 3 untreated hamsters for comparison. • The tiny suspicious lesions were marked and scanned with our prototype OCT device (Optimec Ltd., Nizhny Novgorod, Russia). Its operating wavelength is 1300nm and this gives 15-20 m resolution. • The suspected lesions were marked using a pin inserted at the red light pointer of the device, biopsied with a cylindrical biopsy knife. The animals were euthanized using intracardiac KCl injection. • All samples were sent to the blinded pathologist and examined in one session.
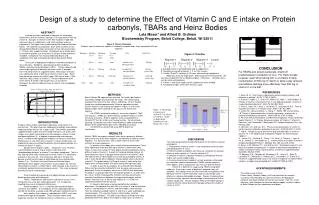
Schematic diagram of a fiber optic OCT scanner SLD 50/50 Sample Detector Reference Demodulator A/D Computer
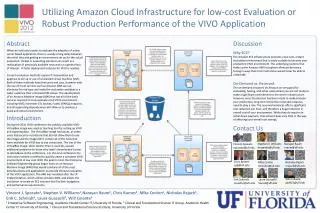
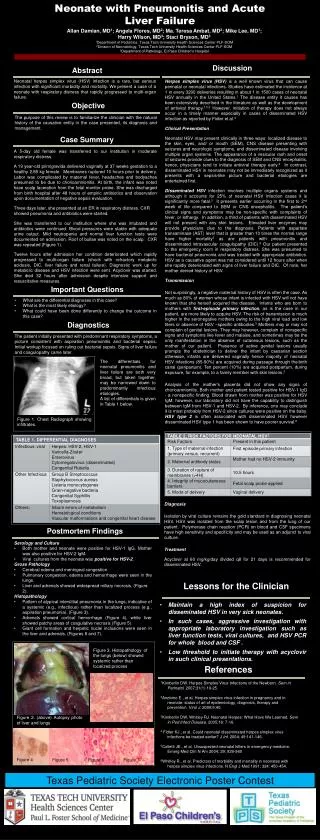
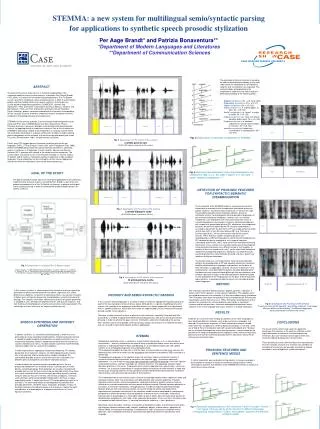
Results • In the normal cheek pouch, we’ve found an excellent 3 layer demonstration of histological layers (Panels A & D). The first layer is a highly reflective (bright) layer representing the mucosa, the brightest of which is the outer surface representing the keratin layer. The second is a less reflective layer representing the submucosa. The line between the mucosa and submucosa represents the basement membrane or the interface between both layers. The third layer is the least reflective layer representing the muscle layer. The bright line in-between the second and the third layers represents the interface between the submucosa and muscle layer as the light waves transits between different densities. • In our inflammatory model, we have found excellent OCT pictures (Panels B & E) representing hyperplasia. The mucosa is increased both in thickness and reflectivity, but the layers are clearly defined in straight alignment. Compared with the normal mucosa, the scattering is more in the mucosa and less in the depper layers.There was no difference between hyperplasia in inflammation and precancerous groups. • In the precancer model, we have found increased thickness and brightness in both the keratin and mucosal layers, which correlates well within histological sections taken from the same spots. Also, the little changes in shape and architecture of the mucosa are well represented in our OCT scans. Panels C & F show the OCT scan and the histology of a mucosal polyp with moderate degree dysplasia. There isenhanced heterogenous scattering of the mucosa and less reflectivity of the depper layers, but still clearly seen. • OCT has an overall sensitivity of 58.6% and a specificity of 75%..
Keratin Mucosa Submucosa Interface Muscle layer L Keratin Mucosa BM Submucosa Interface Muscle layer
Keratin Mucosa Submucosa Muscle layer Keratin Mucosa BM Submucosa Interface Muscle layer
Polyp Mucosa Submucosa Interface Muscle layer Polyp Mucosa Submucosa Muscle layer
Discussion • Painting the right hamster’s cheek pouch with DMBA for 6-10 weeks produced a range of lesions ranging from hyperplasia to Carcinoma in situ. This was more or less in accordance with Salley 6 who described four degrees of change: hyperplasia, benign papilloma, carcinoma in situ, and SCC with local invasion and metastases. • Because our goal was early detection of pregression of precancerous lesion, our biopsies were taken much earlier than the stage of invasive cancer. Also, we’ve avoided areas of fungating cancer. • Using OCT, we’ve found a good correlation with the histoological findings ranging from normal to Carcinoma in situ. • This was in accordance with Bouma et al.7 who found that OCT give a relatively good identification of the layers of normal esophagus and of Barrett’s esophagus, and a good differentiation between normal esophageal and gastric mucosa. • As imaging depth is limited by optical attenuation of the light beam in tissue, we were concerned with the early detection of mucosal cancer before it causes invasion. However, the depth of our OCT scans ranged from 2-3 mm. This is more or less the same as the depth of conventional endoscopic biopsy.
Discussion, ctn.. • Tearney et al. 8 agreed with that and have used this principle for ‘optical biopsy’ from the rabbit gastrointestinal and respiratory tracts at 10 m resolution. • In future pre-clinical and clinical studies we will try to define the ability of OCT to detect the local invasion and if it will help in staging of early cancer. • The most prominent feature of OCT is that it can differentiate between normal and abnormal mucosa in terms of preserved or disrupted architecture respectively. Also, any increase in thickness is clearly represented in our OCT scans. • We agree with what Van Dam and Fugimoto 9 that more studies are needed to understand how OCT might be integrated into diagnostic protocols. They stated that if OCT can differentiate and grade dysplasia, then it could be used to guide excision biopsy, reducing sampling error and associated false-negative rates. • We predict that OCT has the potential for detection of minimally invasive epithelial cancer and follow up of precancerous lesions. We have observed that the lines representing the interface between different mucosal layers were clearly defined. This may be also of help in local staging of mucosal cancer and high-resolution imaging of microinvasion.
Conclusion • OCT has a great potential for follow up of the progression of early precancerous mucosal lesions as well as staging of microinvasive carcinoma. • OCT after being refined will pave the way for in vivo histological imaging.
References 1- Huang D, Swanson EA, Lin CP, Schuman JS, Stinson WG, Chang W, Hee MR, Flotte T, Gregory K, Puliafito CA, and Fugimoto JG. OCT. Science 1991; 254: 1178-1181. 2- Van Dam J. and Fujimoto J.G. Imaging beyond the endoscope [editorial]. Gastroint. Endosc. 2000; 51-4 (1): 512-516. 3- Fugimoto JG, Pitris C, Boppart SA, and Brezinski ME. OCT: an emerging technology for biomedical imaging and optical biopsy. Neoplasia 2000; 2(1-2): 9-25. 4- Pitris C, Jesser C, Boppart SA, et al. Feasibility of OCT for high-resolution imaging of human GIT. J Gastroenterol 2000; 35:87-92. 5- Tadrous PJ. Methods for imaging the structure and function of living tissues and cells: I. Optical coherence tomography [Review]. J Pathology 2000; 191: 115-119. 6- Salley J.J. Experimental carcinogenesis in the cheeck pouch of the Syrian hamster. J. Dent. Res. 1954; 33:253-62. 7- Bouma B.E, Tearney G.J, Compton CC, and Nishioka N.S. High resolution imaging of the human esophagus and stomach in vivo using OCT. Gastrointest. Endosc. 2000; 51(4)1: 467-79. 8- Tearney GJ, Brezinski ME, Bouma BE, Boppart SA, Pitris C, Southern JF, and Fugimoto JG. In vivo endoscopic optical biopsy with OCT. Science 1997; 276: 2037-9. 9- Van Dam J. and Fujimoto J.G. Imaging beyond the endoscope [editorial]. Gastroint. Endosc. 2000; 51-4 (1): 512-16.