Neonatal Herpes Simplex Virus: A Case of Pneumonitis and Acute Liver Failure
This case study highlights a rare yet severe neonatal herpes simplex virus (HSV) infection presenting with respiratory distress, rapidly leading to multi-organ failure, including acute liver failure and disseminated intravascular coagulopathy (DIC). The infant, a 5-day-old female, initially treated for bacterial pneumonia, demonstrated delayed recognition of HSV due to non-specific symptoms. Despite the mother's negative HSV history, the transmission risk was high due to her first-episode primary infection. This review emphasizes the importance of timely diagnosis and intervention in managing neonatal HSV.

Neonatal Herpes Simplex Virus: A Case of Pneumonitis and Acute Liver Failure
E N D
Presentation Transcript
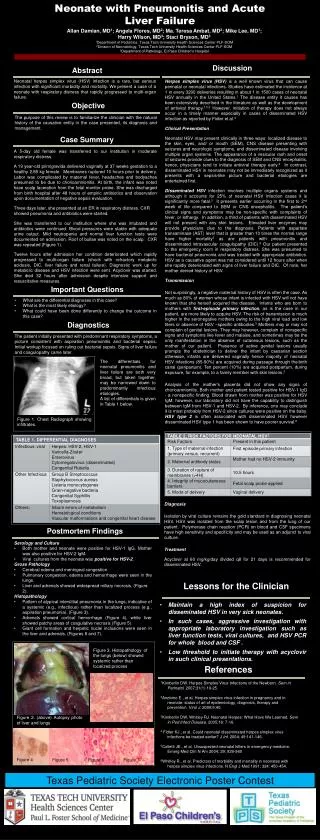
Neonate with Pneumonitis and Acute Liver Failure Allan Damian, MD1; Angela Flores, MD2; Ma. Teresa Ambat, MD2; Mike Lee, MD1; Harry Wilson, MD3; Staci Bryson, MD3 1Department of Pediatrics, Texas Tech University Health Sciences Center PLF-SOM 2Division of Neonatology, Texas Tech University Health Sciences Center PLF-SOM 3Department of Pathology, El Paso Children’s Hospital Discussion Abstract Neonatal herpes simplex virus (HSV) infection is a rare, but serious infection with significant morbidity and mortality. We present a case of a neonate with respiratory distress that rapidly progressed to multi-organ failure. Herpes simplex virus (HSV) is a well known virus that can cause perinatal or neonatal infections. Studies have estimated the incidence at 1 in every 3200 deliveries resulting in about 1 in 1500 cases of neonatal HSV annually in the United States.1 The disease entity it causes has been extensively described in the literature as well as the development of antiviral therapy.1,2,3 However, initiation of therapy does not always occur in a timely manner especially in cases of disseminated HSV infection as reported by Fidler et al.4 Clinical Presentation Neonatal HSV may present clinically in three ways: localized disease to the skin, eyes, and/ or mouth (SEM), CNS disease presenting with seizures and neurologic symptoms, and disseminated disease involving multiple organ systems. The appearance of a vesicular rash and onset of seizures provide clues to the diagnosis of SEM and CNS encephalitis, hence, physicians tend to initiate antiviral therapy early.4 In contrast, disseminated HSV in neonates may not be immediately recognized as it presents with a sepsis-like picture and bacterial etiologies are entertained first. Disseminated HSV infection involves multiple organs systems and although it accounts for 25% of neonatal HSV infection cases it is significantly more fatal.3 It presents earlier occurring in the first to 2nd week of life compared to SEM or CNS encephalitis. The patient’s clinical signs and symptoms may be non-specific with complaints of fever, or lethargy. In addition, a third of patients with disseminated HSV will not present with any skin lesions. Elevated liver enzymes may provide physicians clue to the diagnosis. Patients with aspartate transaminase (AST) level that is greater than 10 times the normal range have higher mortality5 as are patients with pneumonitis and disseminated intravascular coagulopathy (DIC).6 Our patient presented to the emergency room in respiratory distress. She was presumed to have bacterial pneumonia and was treated with appropriate antibiotics. HSV as a causative agent was not considered until 12 hours after when she rapidly deteriorated with signs of liver failure and DIC. Of note, her mother denied history of HSV. Transmission Not surprisingly, a negative maternal history of HSV is often the case. As much as 80% of women whose infant is infected with HSV will not have known that she herself acquired the disease. Infants who are born to mothers with first-episode primary infection, as is the case in our patient, are more likely to acquire HSV. The risk of transmission is much higher in the seronegative mothers owing to the high viral load and low titers or absence of HSV –specific antibodies.3 Mothers may or may not complain of genital lesions. They may however, complain of nonspecific signs and symptoms like fever and malaise, and sometimes may be the only manifestation in the absence of cutaneous lesions, such as the mother of our patient. Presence of active genital lesions usually prompts the obstetrician to deliver the infant by caesarian section otherwise, infants are delivered vaginally hence majority of neonatal HSV infections (85-90%) are acquired during passage through thebirth canal (peripartum). Ten percent (10%) are acquired postpartum, during exposure, for example, to a family member with skin lesions.3 Analysis of the mother’s placenta did not show any signs of chorioamnionitis. Both mother and patient tested positive for HSV-1 IgG - a nonspecific finding. Blood drawn from mother was positive for HSV IgM; however, our laboratory did not have the capability to distinguish between IgM from HSV-1 and HSV-2. By inference, one may conclude it is most probably from HSV-2 since cultures were positive on the baby. HSV type 2 is often associated with disseminated HSV however disseminated HSV type 1 has been shown to have poorer survival.6 Objective The purpose of this review is to familiarize the clinician with the natural history of the causative entity in the case presented, its diagnosis and management. Case Summary A 5-day old female was transferred to our institution in moderate respiratory distress. A 19 year-old primigravida delivered vaginally at 37 weeks gestation to a healthy 2.89 kg female. Membranes ruptured 10 hours prior to delivery. Labor was complicated by maternal fever, headaches and bodyaches presumed to be due to chorioamnionitis. At birth, the infant was noted have scalp laceration from the fetal monitor probe. She was discharged from birth hospital after 48 hours of empiric antibiotics and observation upon documentation of negative sepsis evaluation. Three days later, she presented at an ER in respiratory distress. CXR showed pneumonia and antibiotics were started. She was transferred to our institution where she was intubated and antibiotics were continued. Blood pressures were stable with adequate urine output. Mild neutropenia and normal liver function tests were documented on admission. Roof of bullae was noted on the scalp. CXR was repeated (Figure 1). Twelve hours after admission her condition deteriorated which rapidly progressed to multi-organ failure (shock with refractory metabolic acidosis, DIC, liver failure and renal failure). Diagnostic work up for metabolic disease and HSV infection were sent. Acyclovir was started. She died 32 hours after admission despite intensive support and resuscitative measures. Important Questions • What are the differential diagnoses in this case? • What is the most likely etiology? • What could have been done differently to change the outcome in this case? Diagnostics The patient initially presented with predominant respiratory symptoms, a picture consistent with aspiration pneumonitis and bacterial sepsis. Initial workup focused on ruling out bacterial sepsis. Signs of liver failure and coagulopathy came later. The differentials for neonatal pneumonitis and liver failure are both very broad, but taken together, may be narrowed down to predominantly infectious etiologies. A list of differentials is given in Table 1 below. Figure 1. Chest Radiograph showing infiltrates. Diagnosis Isolation by viral culture remains the gold standard in diagnosing neonatal HSV. HSV was isolated from the scalp lesion and from the lung of our patient. Polymerase chain reaction (PCR) on blood and CSF specimens have high sensitivity and specificity and may be used as an adjunct to viral culture. Treatment Acyclovir at 60 mg/kg/day divided q8 for 21 days is recommended for disseminated HSV. Postmortem Findings • Serology and Culture • Both mother and neonate were positive for HSV-1 IgG. Mother was also positive for HSV-2 IgM. • Viral cultures from the neonate was positive for HSV-2. • Gross Pathology • Cerebral edema and meningeal congestion • Pulmonary congestion, edema and hemorrhage were seen in the lungs. • Liver and adrenals showed widespread miliary necrosis. (Figure 2). • Histopathology • Pattern of atypical interstitial pneumonia in the lungs, indicative of a systemic (e.g., infectious) rather than localized process (e.g., aspiration pneumonia). (Figure 3). • Adrenals showed cortical hemorrhage (Figure 4), while liver showed patchy areas of coagulative necrosis (Figure 5) • Giant cell formation and herpetic nuclei inclusions were seen in the liver and adrenals. (Figures 6 and 7). Lessons for the Clinician • Maintain a high index of suspicion for disseminated HSV in very sick neonates. • In such cases, aggressive investigation with appropriate laboratory investigation such as liver function tests, viral cultures, and HSV PCR for whole blood and CSF . • Low threshold to initiate therapy with acyclovir in such clinical presentations. Figure 3. Histopathology of the lungs (below) showed systemic rather than localized process References 1Kimberlin DW. Herpes Simples Virus Infections of the Newborn. Sem in Perinatol. 2007;31(1) 19-25. 2Anzivino E., et al. Herpes simplex virus infection in pregnancy and in neonate: status of art of epidemiology, diagnosis, therapy and prevention. Virol J. 2009;6:40. 3Kimberlin DW, Whitley RJ. Neonatal Herpes: What Have We Learned. Sem in Ped Infect Disease. 2005;16: 7-16. 4 Fidler KJ., et al. Could neonatal disseminated herpes simplex virus infections be treated earlier? J Inf. 2004; 49:141-146. 5Colletti JE., et al. Unsuspected neonatal killers in emergency medicine. Emerg Med Clin N Am 2004; 29: 929-960 6Whitley R., et al. Predictors of morbidity and mortality in neonates with herpes simplex virus infections. N Engl J Med 1991; 324: 450-454. Figure 2. (above) Autopsy photo of liver and lungs Figure 4 Figure 5 Figure 6 Figure 7 Texas Pediatric Society Electronic Poster Contest