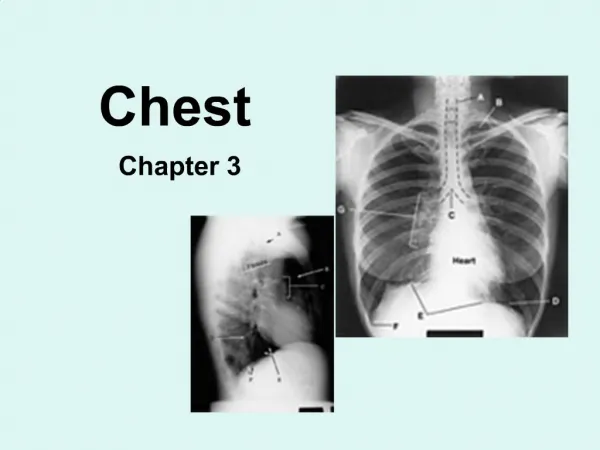
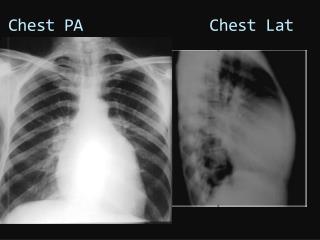
Chest Injuries
Chest Injuries. Chapter 27. Organs of the Chest. Structures of the Chest. Mechanics of Ventilation. Inspiration Intercostal muscles contract and diaphragm flattens. Expiration Intercostal muscles and diaphragm relax; tissues move back to normal position.

Chest Injuries
E N D
Presentation Transcript
Chest Injuries Chapter 27
Mechanics of Ventilation • Inspiration • Intercostal muscles contract and diaphragm flattens. • Expiration • Intercostal muscles and diaphragm relax; tissues move back to normal position. • Phrenic nerves exit the spinal cord at C3, C4, and C5. • Spinal cord injury below C5 • Loss of ability to move intercostal muscles • Diaphragm can still contract; patient can still breathe. • Spinal cord injury at C3 or higher • No ability to breathe
Injuries to the Chest • Closed chest injuries • Caused by blunt trauma • Open chest injuries • Caused by penetrating trauma
Signs and Symptoms • Pain at site of injury • Pain aggravated by increased breathing • Bruising to chest wall • Crepitus with palpation of chest • Penetrating injury to chest • Dyspnea • Hemoptysis • Failure of chest to expand normally • Rapid, weak pulse and low blood pressure • Cyanosis around lips or fingernails
Scene Size Up • Observe for hazards • Do not disturb potential evidence • Put several pairs of gloves in your pocket. • Consider spinal immobilization • Ensure that police are on scene if incident involved violence
Initial Assessment • General impression • Quickly evaluate ABCs • Difficulty speaking may indicate several problems • Patients with significant chest injuries will look sick • Airway and breathing • Ensure that patient has a clear, patent airway • Protect the spine • Inspect for DCAP-BTLS
Inspection (AB) • Decreased breath sounds usually indicate significant damage to a lung • If both sides of chest do not have equal rise and fall, chest muscles have lost ability to work properly • If one section of chest moves in opposite direction from the rest of the chest (paradoxical motion), this is a life threat
Immediate Interventions • Apply an occlusive dressing to any penetrating chest injury • Stabilize paradoxical motion with a large bulky dressing and 2'' tape • Apply oxygen via nonrebreathing mask at 15 L/min • Provide positive pressure ventilations if breathing is inadequate
Circulation (C) • Assess patient’s pulse • Consider aggressive treatment for shock • Internal bleeding can quickly cause death
Transport Decision • Rapidly transport if patient has problems with ABCs. • Pay attention to subtle clues. • Skin signs • Level of consciousness • Sense of impending doom
Focused History and Physical Exam • Focused physical exam • For a patient with isolated chest injury and limited MOI • Rapid physical exam • For a patient with a significant MOI • Use DCAP-BTLS • Do not focus just on the chest wound • Obtain baseline vital signs • Obtain SAMPLE history quickly
Interventions • Provide complete spinal immobilization • Maintain open airway; be prepared to suction • Provide assisted ventilations if needed • Control bleeding • Place occlusive dressing over penetrating chest wound • Stabilize flail segment with a bulky dressing • Treat aggressively for shock • Do not delay transport
Detailed Physical Exam • Perform enroute to the Hospital if time allows
Ongoing Assessment • Assess effectiveness of interventions • Reassess vital signs • Communication and documentation • Communicate with hospital early if patient has significant MOI • Describe injuries and treatment given
Complications of Chest Injuries • A pneumothorax occurs when air leaks into the space between the pleural surfaces.
Pneumothorax • Air accumulates in the pleural space • Air enters through a hole in the chest wall • The lung may collapse in a few seconds or a few minutes • An open or penetrating wound to the chest is called a sucking chest wound
Care for Open Pneumothorax • Flutter valve dressing
Spontaneous Pneumothorax • Some people are born with or develop weak areas on the surface of the lungs • Occasionally, the area will rupture spontaneously, allowing air into the pleural space • Patient experiences sudden chest pain and trouble breathing • Consider a spontaneous pneumothorax for a patient with chest pain without cause
Tension Pneumothorax • Can occur from sealing all four sides of the dressing on a sucking chest wound • Can also occur from a fractured rib puncturing the lung or bronchus • Can also result from a spontaneous pneumothorax
Signs and Symptoms • Respiratory distress • Distended neck veins • Tracheal deviation • Tachycardia • Low blood pressure • Cyanosis • Decreased lung sounds • Treatment • If a tension pneumothorax develops from sealing an open chest wound, partly remove the dressing to let the air escape. • If there is no open wound, follow local protocol
Hemothorax • Collection of blood in the pleural space • Suspect if the following are seen: • Signs and symptoms of shock • Decreased breath sounds on affected side • If both air and blood are present in the pleural space, it is a hemopneumothorax
Rib Fractures • They are very common in the older people. • A fractured rib may lacerate the surface of the lung • Patients will avoid taking deep breaths and breathing will be rapid and shallow • The patient often holds the affected side to minimize discomfort • Administer oxygen
Flail Chest • Segment of chest wall detached from rest of thoracic cage • Occurs when: • Three or more ribs are fractured in two or more places. • Sternum is fractured along with several ribs. • Creates paradoxical motion
Care for Flail Chest • Maintain airway • Provide respiratory support with BVM if needed • Perform ongoing assessments for pneumothorax and other respiratory complications • Immobilize flail segment
Pulmonary Contusions • Bruising of the lung • Develops over hours • Alveoli fill with blood, and edema accumulates in the lung, causing hypoxia • Provide oxygen and ventilatory support
Traumatic Asphyxia • Sudden, severe compression of chest • Produces rapid increase in pressure within chest • Results in neck vein distention, cyanosis, and bleeding into the eyes • Provide supplemental oxygen and monitor vital signs • Transport immediately
Blunt Myocardial Injury • Bruising of heart muscle • Pulse is often irregular • There is no prehospital treatment for this condition • Check patient’s pulse and note irregularities • Provide supplemental oxygen and transport immediately
Pericardial Tamponade • Blood or other fluids collect in the pericardium
Pericardial Tamponade • Signs and symptoms: • Very soft and faint heart tones • Weak pulse • Low blood pressure • Decrease in difference between systolic and diastolic blood pressure • Jugular vein distention (JVD) • Provide oxygen and transport quickly
Laceration of the Great Vessels • The superior vena cava, inferior vena cava, pulmonary arteries and veins, and aorta are contained in the chest • Injury to these vessels can cause fatal hemorrhage • Treatment includes: • CPR • Ventilatory support • Supplemental oxygen • Transport immediately