Immune System: Overview
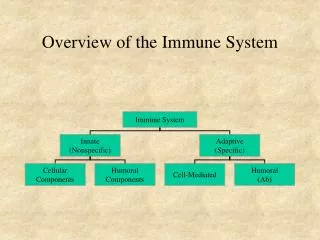
Immune System: Overview . The immune system has three types of components Lymphoid tissues Various types of immune cells Chemical signals that coordinate responses. Immune System: Functions . Protects against pathogens Bacteria Viruses Parasites

Immune System: Overview
E N D
Presentation Transcript
Immune System: Overview • The immune system has three types of components • Lymphoid tissues • Various types of immune cells • Chemical signals that coordinate responses
Immune System: Functions • Protects against pathogens • Bacteria • Viruses • Parasites • Protects against foreign molecules (e.g., toxins) • Removes dead or damaged cells • Attempts to recognize and remove abnormal cells
Immune System: Pathologies • Incorrect immune responses • Autoimmune disease (e.g., Type 1 diabetes) • Overactive immune responses • Allergies • Lack of immune response • Immunodeficiency disease (e.g., SCID and AIDS)
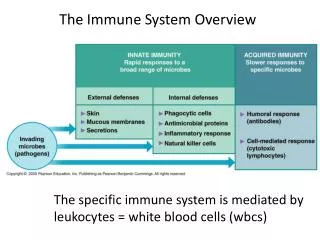
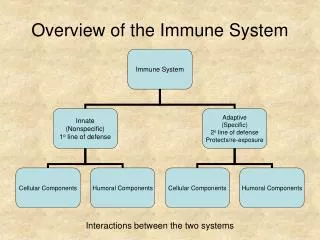
Immunity: Two Intrinsic Defense Systems • Innate system responds quickly and consists of: • First line of defense – skin and mucosae prevent entry of microorganisms • Second line of defense – antimicrobial proteins, phagocytes, and other cells • Inhibit spread of invaders throughout the body • Inflammation is its most important mechanism • Adaptive defense system • Third line of defense – mounts attack against particular foreign substances • Takes longer to react than the innate system • Works in conjunction with the innate system
Innate and Adaptive Defenses First line Second line Third line Figure 21.1
Neutrophils Plasma cells Macrophages Naturalkiller cells Antibodytiter CytotoxicT cells Number of active immune cells Time (weeks)
Figure 22-11 Innate Defenses (Part 1 of 2) Innate Defenses Physical barriers Duct of eccrinesweat gland Secretions Hair keep hazardousorganisms andmaterials outsidethe body. Epithelium Phagocytes engulf pathogensand cell debris. Fixedmacrophage Freemacrophage Monocyte Neutrophil Eosinophil Immunologicalsurveillance Lysedabnormalcell is the destruction ofabnormal cells by NKcells in peripheral tissues. Naturalkiller cell Interferons are chemical messengersthat coordinate thedefenses against viralinfections. Interferons released by activatedlymphocytes, macrophages, orvirus-infected cells
Figure 22-11 Innate Defenses (Part 2 of 2) Innate Defenses Complementsystem consists of circulatingproteins that assistantibodies in thedestruction of pathogens. Lysedpathogen Complement Inflammatoryresponse 1. Blood flow increased 2. Phagocytes activated is a localized, tissue-levelresponse that tends tolimit the spread of aninjury or infection. 3. Capillary permeability increased 4. Complement activated 5. Clotting reaction walls off region 6. Regional temperature increased Mast cell 7. Adaptive defenses activated Fever is an elevation of bodytemperature that acceleratestissue metabolism and theactivity of defenses. Body temperature rises above 37.2ºC inresponse to pyrogens
First line of defense: Surface Barriers • Skin, mucous membranes, and their secretions make up the first line of defense • Keratin in the skin: • Presents a physical barrier to most microorganisms • Is resistant to weak acids and bases, bacterial enzymes, and toxins
First line of defense: Epithelial Barriers • Epithelial membranes produce protective chemicals that destroy microorganisms • Skin acidity (pH of 3 to 5) inhibits bacterial growth • Sebum contains chemicals toxic to bacteria • Stomach mucosae secrete concentrated HCl and protein-digesting enzymes • Saliva and lacrimal fluid contain lysozyme • Mucus traps microorganisms that enter the digestive and respiratory systems • Mucus-coated hairs in the nose trap inhaled particles • Mucosa of the upper respiratory tract is ciliated • Cilia sweep dust- and bacteria trapped by mucus away from lower respiratory passages
Second line of defense: Cells and Chemicals • The body uses nonspecific cellular and chemical devices to protect itself • Phagocytes and natural killer (NK) cells • Antimicrobial proteins in blood and tissue fluid • Inflammatory response enlists macrophages, mast cells, WBCs, and chemicals
Second line of defense: Phagocytes • Macrophages are the main phagocytic cells • Two general types: • Macrophages – most derived from monocytes • Fixed (ex. Kupffer cells in liver) • Free/mobile - wander throughout a region in search of cellular debris • Microphages – circulating neutrophils and eosinophils Figure 21.2a
Second line of defense: Phagocytes • Neutrophils become phagocytic when encountering infectious material • Eosinophils are weakly phagocytic against parasitic worms • Mast cells bind and ingest a wide range of bacteria • Mast cells are found in the connective tissue and are similar to basophiles • Originate in the bone marrow • contain special cytoplasmic granules which store mediators of inflammation
Phagocytes Ingest Foreign Material Figure 24-4 (2 of 4)
Microbe adheres to phagocyte. 1 Phagocyte forms pseudopods that eventually engulf the particle. 2 Phagocytic vesicle containing antigen (phagosome). Lysosome Phagocytic vesicle is fused with a lysosome. 3 Phagolysosome Microbe in fused vesicle is killed and digested by lysosomal enzymes within the phagolysosome, leaving a residual body. 4 Acid hydrolase enzymes Residual body Indigestible and residual material is removed by exocytosis. 5 (b) Figure 21.2b
Second line of defense: Inflammation • The inflammatory response is triggered whenever body tissues are injured • Prevents the spread of damaging agents to nearby tissues • Disposes of cell debris and pathogens • Initiate repair processes • The four signs of acute inflammation are • Swelling • Redness • Heat • Pain
Inflammation Response • Begins with chemical “alarm” • a flood of inflammatory chemicals released into the extracellular fluid • Macrophages and epithelial cells of boundary tissues have Toll-like receptors (TLRs) • TLRs recognize specific classes of infecting microbes (even though we consider macrophages to be “non-specific”) • Activated TLRs trigger the release of cytokines that promote inflammation and attract WBC
Inflammatory Response • Some of the inflammatory mediators • Histamine – amino acid derivative produced by basophiles and must cell- promote vasodilation • Kinins – plasma proteins that are activated by tissue injury and promote vasodilation • prostaglandins (PGs) – promote neutrophil diapedesis • Leukotrienes – stimulate vasodilation and netrophil cemotaxis • Complement – set of proteins that promote phgocytosis, activates cells of the immune system • Colony-Stimulating Factors – hormones that promote WBC count • Cells that are involved • WBC, helper T cells, platelets, endothelial cells
Five Steps of Inflammation • Macrophages engulf debris and foreign matter • Capillaries dilate and become more permeable • Foreign matter contained • More leukocytes migrate to area • Leukocytes clear infection
1. Phagocytosis of Pathogens • Proteins on microbes bound by macrophages • Triggers phagocytosis and secretions • Secretory products trigger subsequent steps
2. Dilation and Increased Permeability in Capillaries • Damaged mast cells secrete histamine • Histamine triggers dilation and increases permeability • Result: increased blood flow and increased movement of proteins and cells to injured tissue
2. Vasodilation and Increased Vascular Permeability • The most immediate requirement is to bring WBC to the injury site! • Vasodilation – causes hyperemia (increased blood flow) (Which sign of inflammation?) • Increase permeability of blood walls (cells separate slightly) – causes edema (leakage of exudate) (Which sign of inflammation?) • Exudate—fluid containing proteins, clotting factors, and antibodies • Exudate moves into tissue spaces causing local edema (swelling), which contributes to the sensation of pain
3. Containment of Foreign Matter • Clotting factors eventually form clot in tissue, prevents spread of foreign matter • Eventually forms a scab
4. Inflammatory Response: Phagocytic Mobilization • Four main phases: • Leukocytosis – neutrophils are released from the bone marrow in response to leukocytosis-inducing factors released by injured cells • Margination – neutrophils cling to the walls of capillaries in the injured area • Endothelial cells in the injury site produce cell-adhesion molecules that make the surface “sticky” to help in this process • Diapedesis – neutrophils squeeze through capillary walls and begin phagocytosis • Chemotaxis – inflammatory chemicals attract neutrophils to the injury site
4. Leukocyte Migration and Proliferation • 1 hour: neutrophil migration • 10 hours: monocyte migration macrophages
Fever • Abnormally high body temperature in response to invading microorganisms • Maintenance of a body temperature above 37.2oC (99oF) • The body’s thermostat is reset upwards in response to pyrogens, chemicals secreted by leukocytes and macrophages exposed to bacteria and other foreign substances • High fevers are dangerous because they can denature enzymes • Moderate fever can be beneficial: • Promotes INF activity • May inhibit some viruses and bacteria reproduction • Increase body metabolism so enzymatic reactions occur faster and so is tissue repair
Second line of defense: Antimicrobial Proteins • Enhance the innate defenses by: • Attacking microorganisms directly • Interfering with microorganisms’ ability to reproduce • The most important antimicrobial proteins are: • Interferon • Complement proteins
Second line of defense: Interferons – defense against viruses • Interferons (INF) provide rapid response. • Produced by a variety of body cells • Lymphocytes produce gamma (), or immune, interferon • Most other WBCs produce alpha () interferon • Fibroblasts produce beta () interferon • INF alpha and beta are the most potent against viruses • All three interferons increase expression of class I MHC molecules and thus promote recognition by cytotoxic T cells. • All three interferons can activate NK cells which can then kill virus-infected cells.
Figure 22-13 Interferons Alpha ()-interferons areproduced by cells infectedwith viruses. They attractand stimulate NK cells andenhance resistance to viralinfection. Beta ()-interferons,secreted by fibroblasts,slow inflammation in adamaged area. Gamma ()-interferons,secreted by T cells and NKcells, stimulatemacrophage activity.
Second line of defense: Interferon (IFN) • when a host cell is invaded by a virus it activates the genes that synthesize IFN • Interferon molecules leave the infected cell and enter neighboring cells • Interferon stimulates the neighboring cells to activate genes for PKR (an antiviral protein) • PKR nonspecifically blocks viral reproduction in the neighboring cell • Interferons also activate macrophages and mobilize NKs • Interferon can not save the infected cell but can prevent the virus from infecting other cells
Innate defenses Internal defenses Virus 1 Virusenters cell. New viruses Viral nucleic acid 5 Antiviralproteins blockviralreproduction. 2 Interferongenes switch on. DNA Nucleus mRNA 4 Interferonbindingstimulates cell toturn on genes forantiviral proteins. 3 Cell producesinterferonmolecules. Interferon Host cell 2Binds interferon from cell 1; interferon induces synthesis ofprotective proteins Host cell 1Infected by virus;makes interferon;is killed by virus Figure 21.5, step 5
Second line of defense: Complement“complete the action of antibody” • 30 or so proteins synthesized mainly by the liver • circulate in the blood in an inactive form and activated in the presence of pathogen • Proteins include C1 through C9, factors B, D, and P, and regulatory proteins
Second line of defense: Complement system functions • Destruction of target cells membrane (MAC) • Stimulation of inflammation – C3a stimulates mast cells and basophils to secrete histamine • Attraction of phagocytes • Enhancement of phagocytosis – • Phagocytes membrane carry receptors that can bind to the complex of the complement proteins and antibodies. • The binding results in much more efficient phagocytosis. • The antibodies in such a complex are called opsonins and the effect is called opsonization (enhanced attachment )
Second line of defense: Natural killer (NK) cells • Are a small, distinct group of large granular lymphocytes • React nonspecifically and eliminate cancerous and virus-infected cells • Kill their target cells by releasing perforins and other cytolytic chemicals • Secrete potent chemicals that enhance the inflammatory response • NK cells • Recognize cell surface markers on foreign/abnormal cells • Recognize variety of antigens (less selective) • Immediate response when contact abnormal cells • Destroy cells with foreign antigens
Properties of specific immunity • Specificity – activated by and responds to a specific antigen • Versatility – is ready to confront any antigen at any time • Memory – “remembers” any antigen it has encountered • Tolerance – responds to foreign substances but ignores normal tissues
Complete Antigens • Substances that can mobilize the immune system and provoke an immune response • mostly large, complex molecules not normally found in the body (nonself) • Important properties of antigene: • Immunogenicity – ability to stimulate proliferation of specific lymphocytes and antibody production • Reactivity – ability to react with products of activated lymphocytes and the antibodies released in response to them • Complete antigens include foreign protein, nucleic acid, some lipids, and large polysaccharides
Haptens (Incomplete Antigens) • Small molecules, such as peptides, nucleotides, and many hormones, thatare not immunogenic but are reactive when attached to protein carriers • If they link up with the body’s proteins, the adaptive immune system may recognize them as foreign and mount a harmful attack (allergy) • Haptens are found in poison ivy, dander, some detergents, and cosmetics
Figure 19.14 2 The formation of an antigen-antibody complex Carrier molecule Antibodies bind not to the entire antigen, but to specific portions of its exposed surface—regions called antigenic determinant sites. Partial antigen (hapten) Antibody Antibody Partial antigens, or haptens, do not ordinarily cause B cell activation. However, they may become attached to carrier molecules, forming combinations that can function as complete antigens. The antibodies produced will attack both the hapten and the carrier molecule. If the carrier molecule is normally present in the tissues, the antibodies may begin attacking and destroying normal cells. This is the basis for several drug reactions, including allergies to penicillin. Antigen-antibody complex A complete antigen is an antigen with at least two antigenic determinant sites, one for each of the antigen binding sites on an antibody molecule.
Cells of the Adaptive Immune System • Two types of lymphocytes • B lymphocytes – oversee humoral immunity • T lymphocytes – non-antibody-producing cells that constitute the cell-mediated arm of immunity • Antigen-presenting cells (APCs): • Do not respond to specific antigens
Lymphocytes can become immunocompetent • Immature lymphocytes released from bone marrow are identical • During their development the lymphocyte: • Must become able to recognize its one specific antigen – become immunocompetent • Must be relatively unresponsive to self so it will not attack the body’s own cells – self tolerance • Location of becoming immunocompetent is the key for a lymphocyte to become B cell or a T cell • B cells mature in the bone marrow • T cells mature in the thymus
Immunocompetent B or T cells • It is genes, not antigens, that determine which foreign substances our immune system will recognize and resist • Become immunocompetent before they encounter antigens they may later attack • Immunocompetence - displaying a unique type of receptor that responds to a specific antigen
Immunocompetent B or T cells • An immunocompetent cell divides rapidly to form a clone of cells with identical receptors. All clones yet to encounter an antigen are called the virgin/naive lymphocyte pool. • Are exported to secondary lymphoid tissue where encounters with antigens occur • Mature into fully functional antigen-activated cells upon binding with their recognized antigen • Clonal selectionof B or T cells occurs when antigens bind to their receptors, causing them to proliferate.
Antigen-Presenting Cells (APCs) • Major functions in immunity are: • To engulf foreign particles • To present fragments of antigens on their own surfaces, to be recognized by T cells • Major APCs are • Dendritic cells (DCs), • Dendritic cells (DC) are bone marrow-derived cells that are specialized to take up, process and present antigen • Dendritic cells are present in small quantities in tissues that are in contact with the external environment, mainly the skin (where they are often called Langerhans cells) and the inner lining of the nose, lungs, stomach and the intestines. • Macrophages that are found all over the body • Activated B cells
Antigen-Presenting Cells Display Foreign Proteins Figure 24-4 (4 of 4)
Importance of Cellular and humoral Responses • Importance of Humoral Response (Soluble antibodies) • The simplest ammunition of the immune response • Interact inextracellular environments such as body secretions, tissue fluid, blood, and lymph • Importance of Cellular Response (T-cells) • T cells recognize and respond only to processed fragments of antigen displayed on the surface of body cells • T cells are best suited for cell-to-cell interactions, and target: • Cells infected with viruses, bacteria, or intracellular parasites • Abnormal or cancerous cells • Cells of infused or transplanted foreign tissue
Antigen Primary Response (initial encounter with antigen) Antigen binding to a receptor on a specific B lymphocyte (B lymphocytes with non-complementary receptors remain inactive) Proliferation to form a clone B lymphoblasts Plasma cells Memory B cell Secreted antibody molecules Secondary Response (can be years later) Subsequent challenge by same antigen Clone of cells identical to ancestral cells Plasma cells Secreted antibody molecules Memory B cells Figure 21.10
Antibodies • Also called immunoglobulins • Plasma cells make over a billion types of antibodies • makes the gamma globulin portion of blood proteins • Are soluble proteins secreted by activated B cells and plasma cells in response to an antigen • Are capable of binding specifically with that antigen • Antibodies themselves do not destroy antigen; they inactivate and tag it for destruction
Basic Antibody Structure • Consists of four polypeptide chains linked together with disulfide bonds • Two identical heavy (H) chains and two identical light (L) chains • The four chains bound together form an antibody monomer • Each chain has a variable (V) region at one end and a constant (C) region at the other • Variable (FAB) regions of the heavy and light chains combine to form the antigen-binding site • Constant (FC) region Determine the class of the antibody (one of the 5 groups)
Classes of Antibodies • IgD – monomer attached to the surface of B cells, important in B cell activation • IgM – pentamer released by plasma cells during the primary immune response • IgG – monomer that is the most abundant and diverse antibody in primary and secondary response; crosses the placenta and confers passive immunity • IgA – dimer that helps prevent attachment of pathogens to epithelial cell surfaces • IgE – monomer that binds to mast cells and basophils, causing histamine release when activated