Understanding the Urinary System: Anatomy, Function, and Physiology
Explore the intricate details of the urinary system, including the organs involved such as kidneys, ureters, and the bladder. Learn about the primary functions, regulation of blood volume and composition, and the essential role in metabolism. Discover the anatomy of nephrons, renal tubules, and the filtration process. Dive into renal physiology, hormonal regulation, and the processes of tubular reabsorption and secretion. Uncover the complexities of urinary physiology and how the body maintains proper kidney function.

Understanding the Urinary System: Anatomy, Function, and Physiology
E N D
Presentation Transcript
Urinary System Exercises 40 and 41
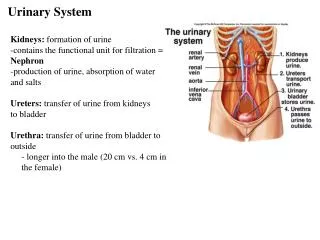
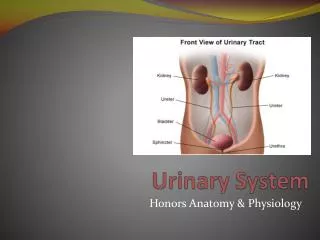
Organs of the Urinary System • 2 kidneys • Urinary bladder • 2 ureters • Urethra • Primary function is to filter blood, and reabsorb water and needed substances back into blood. Remaining water and wastes are removed in urine.
Regulate blood volume and composition • Regulate blood pH • Regulate blood pressure • Contribute to metabolism • Calcitriol • Erythropoietin • Gluconeogenesis
Location of kidneys • Between T12 and L3 • Partially protected by 11th and 12th ribs • Right kidney is lower than left • Kidneys and ureters are retroperitoneal • Protected by three layers: • Renal capsule • Adipose capsule • Renal fascia
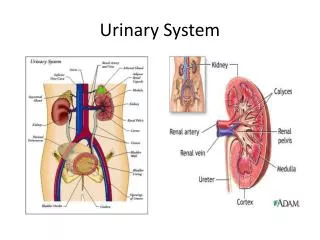
Anatomy • Renal hilum – ureter, blood and lymphatic vessels • Renal sinus • Renal cortex • Renal medulla • Renal pyramids • Renal papilla • Renal columns
Nephron Functional unit of kidney Number constant from birth Can function on 2/3 of one kidney Forms the urine
Duct system • Minor calyces • Major calyces • Renal pelvis • Ureter • Urine is not changed after it leaves the collecting duct
Kidneys = 1% of body mass • Receive 15-30 % of blood flow • Blood supplied to kidney by renal artery • Afferent arteriole divides into ball shaped capillary network called the glomerulus. • Capillaries rejoin to form efferent arteriole, then peritubular capillaries • Vasa recta
Functions of the Nephron • Filtration • Tubular reabsorption • Tubular secretion
Structure of a nephron • Renal corpuscle • Glomerulus • Glomerular capsule or Bowman’s capsule • Renal tubule • Proximal convoluted tubule • Nephron loop or loop of Henle • Distal convoluted tubule • Collecting duct
Bowman’s capsule • Outer layer - simple squamous epithelium • Inner layer – modified simple squamous epi. • Cells called podocytes • Projections are pedicels • Endothelium of capillary and podocytes form the endothelial-capsular (filtration) membrane.
Filtration membrane • Fenestrated endothelium – prevents the passage of cells • Basement membrane of glomerulus – prevents passage of large proteins • Slit membrane (between pedicels) – prevents the passage of medium sized proteins
Wall of renal tubules made up of single layer of epithelial cells and a basement membrane. • Proximal convoluted tubule – cells are cuboidal and have microvilli. • About 65 % of water and 100 % of some solutes are reabsorbed here.
Renal Physiology • Glomerular filtration – most substances easily filtered • Filtrate = 180 L/ day but urine = 1-2 L /day • Filter is thin • Glomerular capillaries are long • Capillary blood pressure is high (afferent arteriole diameter > efferent arteriole)
Filtration fraction is the percentage of plasma that becomes filtrate, usually 16-20 %. • Glomerular Filtration Rate (GFR) is the amount of filtrate formed in both kidneys per minute; normally about 125 ml / min.
Renal autoregulation • JGA senses Na+, Cl- and water • When these ↓, JGA dilates afferent arteriole, ↑ blood pressure in glomerulus
Hormonal regulation • When BP ↓, JGA secretes renin which converts angiotensinogen to angiotensin I, angiotensin I is converted to angiotensin II in the lungs. Angiotensin II is a potent vasoconstrictor. It also stimulates the release of aldosterone, and stimulates the thirst center in the hypothalamus and release of ADH from the posterior pituitary gland.
Tubular reabsorption • Volume of fluid that enters the proximal convoluted tubule in ½ an hour > total plasma volume. • Reabsorb water, glucose, amino acids, urea and ions, esp. Na+, Cl- and K+ • Na+ diffuses into cells, but is actively pumped out into interstitial fluid • Promotes reabsorption of water
DCT and collecting ducts • By end of DCT 90 % of water and solutes reabsorbed. • Aldosterone causes principal cells to synthesize sodium pumps. Also causes potassium to be secreted into urine. • ADH stimulates cells to put water channels into membranes. ADH is responsible for facultative (responding to need) water reabsorption.
Tubular secretion • Two main functions: • Secretion of substances to eliminate them from body – ions, nitrogen-containing waste (urea, creatinine) and certain drugs • Secretion of H+ helps to maintain blood pH
Urinary bladder • Posterior to pubic symphysis • Stores urine prior to micturition • Trigone – between openings of ureters and internal urethral orifice – mucosa is firmly bound to muscularis. • Muscosa, submucosa, muscularis (detrusor muscle), and serous coat.
Evaluation of kidney function • Blood Urea Nitrogen (BUN) – urea is a breakdown product of proteins • Influenced by diet • Creatinine – end product of muscle metabolism • Normally constant • Can determine creatinine clearance
Normal urine • Transparent yellow • Contains ions : Na+, Cl-, K+ ; nitrogenous wastes: ammonia, creatinine, urea and uric acid; and foreign chemicals: drugs, pesticides, food additives, etc. • Suspended solids in trace amounts: bacteria, blood cells, casts.
Not normally present • Albumin • Glucose, Acetone– diabetes mellitus • Bile – liver disease, obstruction of bile ducts, hemolytic disease • pH 4.6 -8.0
Specific gravity • 1.001 -1.035 • Damage to tubules , s.g. fixed at 1.010 = filtrate • Diabetes insipidus (lack of ADH) - • 1.003 • Diabetes mellitus – “sugar diabetes” • 1.030 osmotic diuresis • Emesis or fever – • 1.040