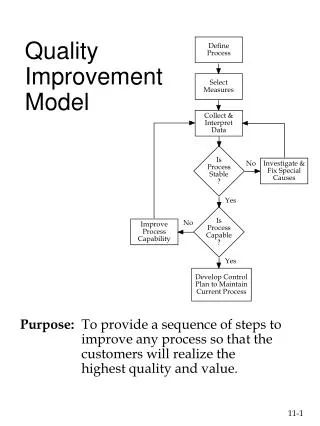
Model for Improvement
Model for Improvement National Combined Councils Meeting February 3, 2008 Act Plan Study Do Model for Improvement What are we trying to accomplish? How will we know that a change is an improvement? What change can we make that will result in improvement?

Model for Improvement
E N D
Presentation Transcript
Model for Improvement National Combined Councils Meeting February 3, 2008
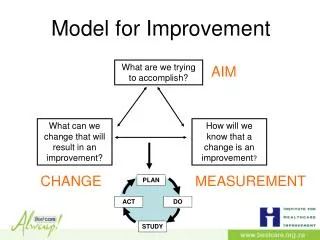
Act Plan Study Do Model for Improvement What are we trying to accomplish? How will we know that a change is an improvement? What change can we make that will result in improvement?
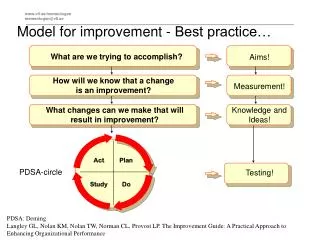
Fundamental Questions for Improvement • What are we trying to accomplish? • How will we know that a change is an improvement? • What change can we make that will result in improvement ?
The PDSA Cycle for Learning and Improvement Act Plan • Objective • Questions and • predictions (why) • Plan to carry out • the cycle (who, • what, where, when) • What changes • are to be made? • Next cycle? Study Do • Complete the • analysis of the data • Compare data to • predictions • Summarize what • was learned • Carry out the plan • Document problems • and unexpected • observations • Begin analysis • of the data
Why Test? • Increase the belief that the change will result in improvement • Predict how much improvement can be expected from the change • Learn how to adapt the change to conditions in the local environment • Evaluate costs and side-effects of the change • Minimize resistance upon implementation
A P S D D S P A A P S D A P S D Repeated Use of the Cycle Changes That Result in Improvement DATA Hunches Theories Ideas
Testing on a Small Scale • Have others that have some knowledgeable about the change review and comment on its feasibility. • Test the change on the members of the team that helped developed it before introducing the change to others. • Incorporate redundancy in the test by making the change side-by-side with the existing system. • Conduct the test in one facility or office in the organization, or with one patient. • Conduct the test over a short time period. • Test the change on a small group of volunteers. • Develop a plan to simulate the change in some way.
Do Study • Reasons for failed tests 1. Change not executed well 2. Support processes inadequate 3. Hypothesis/hunch wrong: - Change executed but did not result in local improvement - Local improvement did not impact access or efficiency Collect data during the Do Phase of the Cycle to help differentiate the these situations.
Questions for Users of the PDSA Cycle • Is the planning based on theory? Stated? • Are the predictions made prior to data collection? • Are multiple cycles run? • Is there documentation of what was learned? • Does the learning provide a basis for action?
Act Plan Study Do Accelerating Learning and Improvement What Cycle can we complete by next Tuesday? Willing to compromise on scope, size, rigor, and sophistication, but the Cycle must be completed by Tuesday.
D S P A A P S D D S P A A P S D A P S D Aim: Improve primary care appointment availability through reducing and standardizing appoint types Improved access DATA Cycle 5: Staff education in new standards Cycle 4: Standardize appointment types Cycle 3:Test the types with 1-3 physicians Reduction of appointment types will increase appointment availability Cycle 2:Compare requests to the types for one week Cycle 1:Define a small number of appointment types
P P P P A A A A D D D D S S S S S S S S D D D D A A A A P P P P A A A A P P P P S S S S D D D D P P P P A A A A D D D D S S S S Overall Aim: Increase Access Specific Test Cycles Standardpanel size Scheduling protocols Appointment types Team approach to care
Measurement for Improvement • Develop a measurement system to guide improvement work and assess results • Summary measures to monitor status of system (vital signs, not estimates of parameters, plot over time, balanced) • More focused measures to determine how well changes are being adapted • Integrate data collection into daily work
Minimum Standard for Monthly Reporting in the Collaborative:Annotated Time Series
Track your PDSA cycles and Key measure(s). Annotate your graph to reflect whether a change led to an improvement NE Team: Actual team PDSA cycles and graph
Monitor and evaluate patient outcomes - Consider measuring the following: • Clinical outcomes, such as A1c, blood pressure, lipid levels, and weight. • Physical activity levels. • Patient satisfaction. • Health care service utilization. • Quality of life. • Costs. • Hospital admissions. From the Indian Health Diabetes Best Practices: Diabetes Systems of Care (Page 6)