FEMALE REPRODUCTIVE SYSTEM
890 likes | 1.71k Views
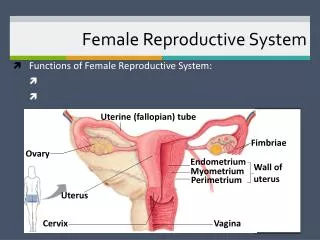
FEMALE REPRODUCTIVE SYSTEM. Dr. Ayisha Qureshi Assistant Professor MBBS, Mphil. THE REPRODUCTIVE SYSTEM. The reproductive system does NOT contribute to HOMEOSTASIS and is NOT essential for survival of an individual. . Functions of the Female Reproductive System.

FEMALE REPRODUCTIVE SYSTEM
E N D
Presentation Transcript
FEMALE REPRODUCTIVE SYSTEM Dr. Ayisha Qureshi Assistant Professor MBBS, Mphil
THEREPRODUCTIVE SYSTEM The reproductive system does NOT contribute to HOMEOSTASIS and is NOT essential for survival of an individual.
OVARIES It is the gonad or the primary sex organ in the Female. A woman has 2 ovaries. An ovary performs 2 functions: Gametogenesis (OOGENESIS): leads to the production & release of ovum or egg (the female gamete). Endocrine Function: secretion of female sex hormones (ESTROGENS & PROGESTERONE).
STRUCTURE OF THE OVARY: Ovaries are flattened ovoid bodies, with the dimensions of 4 x 2 x 1 cm. Each ovary is attached at the hilum to the broad ligament, by means of mesovarium and ovarian ligament. Each ovary has 2 portions: 1. CORTEX: is the outer portion & is lined by the germinal epithelium underneath a fibrous layer known as Tunica Albuginea. It consists of ovarian follicles at different stages, connective tissue & Interstitium. 2. MEDULLA: is the inner portion & contains blood vessels, lymphatics, nerve fibers and smooth muscle fibers near the hilum.
OVARY IN THE INTRAUTERINE LIFE PRIMORDIAL GERM CELLS (the most primitive germ cells) 3rd Week of Gestation ↓ OOGONIA (the female germ cell) 6th Week of Gestation Undergoes Mitosis ↓ PRIMARY OOCYTE 8th week of gestation till BIRTH Completes Mitosis . Meiosis starts & gets arrested at the Diplotene stage. Meiosis stays in the arrested stage until a Primary Oocyte becomes destined for Ovulation at/after Puberty ↓ Primordial Follicle containing the Primary oocyte (The primary oocyte becomes surrounded by a single layer of flattened granulosa cells) MITOSIS + MEIOSIS + ATRESIA 6-7 million oogonia at 20th week of gestation are reduced to only 1-2 million Primary Oocytes at BIRTH
In the Intrauterine life, the germ cell (the undifferentiated gonad cell) forms the OOGONIA in the females. It then completes the mitotic replication and Meiosis by 5th month of fetal development at which point it is called the Primary Oocyte . The Primary Oocyte is actually the egg arrested in the Prophase of the Meiosis and its follicular development shows a single layer of zonagranulosa around the oocyte , thus it is also called the Primordial Follicle. The Primary Oocyte remains arrested in this phase from birth to the time of its ovulation which comes after puberty has been reached….
THE MENSTRUAL CYCLE • Definition: Menstrual cycle is defined as cyclic events that take place in a rhythmic fashion during the reproductive period of a female’s life. Menstrual cycle starts with Menarche which also marks the onset of puberty. Duration:Usually 28 days (may vary b/w 20 & 40 days).
CHANGES DURING MENSTRUAL CYCLE During each menstrual cycle, series of changes occur in the ovaries & the accessory sex organs. These changes are divided into 4 groups: • Ovarian Changes • Uterine Changes • Vaginal Changes • Changes in the Cervix
OVARIAN CHANGES • After the onset of puberty, the ovary alternates b/w 2 phases: 1. Follicular Phase: (Day 1-14) - characterized by presence of maturing follicles. - the recruitment & development of primordial ovarian follicles starts during menstruation. 2. Luteal Phase: (Day 15-28) - starts with ovulation and formation of the corpus luteum. - the luteinized granulosa cells start producing progesterone. Normally, this cycle is interrupted only by pregnancy and terminates with menopause.
FOLLICULAR PHASE OF THE OVARIAN CYCLE: It extends from Day 1 to day 14 of the Menstrual cycle. At Day 14, Ovulation takes place. During this phase, a few primordial follicles start growing but only 1 reaches maturity and is released during ovulation as the Mature ovum.
PRIMORDIAL FOLLICLE • Ovum surrounded incompletely by the granulosa cells. These cells provide nutrition to the ovum during the childhood & also secrete the oocyte maturation inhibiting factor which keeps the ovum in the immature stage from birth till puberty. ↓ At the onset of puberty, with each menstrual cycle, under influence of FSH, about 6-12 primordial follicles start developing into the Primary Follicles. This is called Recruitment of Primary Follicles. ↓ PRIMARY FOLLICLE • Ovum is completely surrounded by the granulosa cells. • Increase in size of the ovum. • Onset of formation of connective tissue capsule around the follicle called the Theca cells. ↓ VESICULAR FOLLICLE / ANTRAL FOLLICLE/ SECONDARY FOLLICLE
VESICULAR FOLLICLE / ANTRAL FOLLICLE/ SECONDARY FOLLICLE • Accelerated proliferation of granulosacells giving rise to many more layers of cells. These cells develop receptors for FSH, increasing their sensitivity to FSH which brings about more proliferationof the follicles. • Granulosa cells secrete liquor folliculi into a cavity between the granulosa cells called the follicular cavity or antrum. This liquid has a high concentration of Estrogen. • Ovum increases in size and is pushed to one side and is surrounded by the granulosa cells called the cumulus oophorus or germ hill. • A thick, glycoprotein membrane is secreted by the granulosa cells around the ovum and is called zonapellucida. • Theca cells differentiate into: • Theca interna: which becomes secretory in nature & starts secreting Estrogens & Progesterone. • Theca externa: forms the capsule of the developing follicle. (Thecal cells synthesize androgens that diffuse into the neighboring granulosa cells, where the enzyme aromatase converts them to estrogens.) ↓ GRAAFIAN FOLLICLE/ MATURE OVARIAN FOLLICLE • About 7 days later. • One follicle outgrows all others; the remaining 5-11 involute, a process called atresia. These follicles are said to become atretic. • The oocyte completes Meiosis I and forms the Secondary Oocyte & First Polar body. Secondary Oocyte starts Meiosis II & is arrested in the Metaphase. It will only progress if fertilized. ↓ OVULATION
OVULATION • Definition: It is the process by which the Graafian Follicle ruptures with consequent discharge of ovum into the abdominal cavity. It is under influence of LH. Ovulation occurs on the 14th day of menstrual cycle in a 28 day cycle. The ovum enters the Fallopian tube. Process: • Rupture of Graafian Follicle at the stigma (small area in the middle of the follicular capsule that swells rapidly & protrudes like a nipple). • Follicular fluid oozes out. • Ovum expelled into the abdominal cavity (Ovum+ Corona radiata). • From there it enters the Fallopian tube through the fimbriated end. The ovum is viable only for 24-48 hours. So it must be fertilized within that time.
ROLE OF LH IN OVULATION: LH SURGE The increase in LH concentrations just before ovulation is called the LH Surge and is necessary for Ovulation. Without this hormone, even when large quantities of FSH are available, there will be no ovulation. This is because: • About 2 days before ovulation, LH secretion by the anterior pituitary gland increases 6 to 10-fold and peaks about 16 hours before ovulation. • LH & FSH synergistically cause rapid swelling of the follicle during the last few days before ovulation. • LH converts the theca cells into progesterone-secreting cells, thus, the rate of secretion of estrogen falls 1 day before ovulation. Under these effects, 2 things happen: • Theca externa begins to release proteolytic enzymes (esp. collagenase) that dissolve the follicular capsule wall leading to degeneration of the stigma. • Secretion of Prostaglandins into the follicular tissue which leads to the smooth muscle contraction of the follicle leading to expulsion of the ova. This leads to degeneration of the stigma and discharge of the ovum.
Role of the LH Surge 1. It halts estrogen synthesis by the follicular cells. 2. It reinitiates meiosis in the oocyte of the developing follicle by blocking release of an oocyte maturation–inhibiting substance produced by the granulosa cells. This substance is responsible for arresting meiosis in the primary oocytes once they are wrapped within granulosa cells in the fetal ovary. 3. It triggers production of local prostaglandins, which induce ovulation by promoting vascular changes that cause rapid follicular swelling while inducing enzymatic digestion of the follicular wall. Together these actions lead to rupture of the weakened wall that covers the bulging follicle. 4. It causes differentiation of follicular cells into luteal cells. Because the LH surge triggers both ovulation and luteinization, formation of the corpus luteum automatically follows ovulation. Thus, the midcycle burst in LH secretion is a dramatic point in the cycle; it terminates the follicular phase and initiates the luteal phase.
LUTEAL PHASE: It extends between 15th and 28th day of the menstrual cycle. During this phase Corpus luteum is developed & thus it is called luteal phase.
CORPUS LUTEUM Corpus luteumis the glandular yellow structure developed from the ruptured Graafian follicle after the release of the ovum. It is also called yellow body. Ovulation ↓ Corpus Hemorrhagicum (follicle is filled with blood which clots slowly) ↓ Corpus Luteum (granulosa & theca interna cells are transformed into lutien cells & secrete Progesterone) If fertilization occurs: Corpus luteum of Pregnancy If no fertilization: Corpus albicans (white scar tissue)
Functions of Corpus Luteum 1. Secretion of hormones: It acts as a temporary endocrine gland. Secretes largequantities of Progesterone & small quantities of Estrogens. LH influences the secretion of these 2 hormones. 2. Maintenance of Pregnancy: If pregnancy occurs, corpus luteum remains active for 3 months and maintains the pregnancy by secreting various hormones. The pregnancy cannot survive if corpus luteum is removed in the early weeks of pregnancy. i.e. before placenta starts secreting the same hormones.
Primordial Follicle ↓ Primary Follicle (Primary Oocyte) ↓ Secondary Follicle ↓ Vesicular Follicle ↓ GraafianFollicle (Secondary Oocyte) (Growth takes place under the influence of FSH) ↓ OVULATION (Takes place under the influence of LH) ↓ Corpus Hemorrhagicum (follicle is filled with blood which clots slowly) ↓ Corpus Luteum (granulosa & theca interna cells are transformed into lutien cells ) FOLLICULAR PHASE LUTEAL PHASE
APPLIED ANATOMY OF OVULATION • Why is it significant to determine the Ovulation time? Determination of time of Ovulation is significant for: - Family Planning by rhythm method. - Encouraging fertility in couples trying to conceive. • How is the ovulation time determined? Various indirect methods are available to determine the ovulation time: 1. Determination of Basal body temperature: There is an increase in the temperature of 0.3-0.5° C due to thermogenic effect of Progesterone. A temperature chart plotted during the month can indicate the time of ovulation. 2. Determination of Hormonal levels in Plasma: Plasma levels of FSH, LH, Estrogen & Progesterone is measured. Hormone level is altered at the time of ovulation. 3. Ultrasound Scanning: Process of ovulation can be observed during ultrasound scanning.
UTERINE CHANGES • During each menstrual cycle, along with ovarian changes, the uterus also undergoes changes simultaneously. Average blood lost during a menstrual cycle is 30-50 ml. They occur in 3 phases: • Menstrual Phase • Proliferative Phase • Secretory Phase
Menstrual Blood Flow: POINTS TO NOTE • The volume of the blood loss during the menstrual phase is about 30-50 ml. More than 80 ml is considered pathological and is termed menorrhagia. • Bleeding continues for 3-7 days (average 4 days). • Most of the blood lost (75%) is arterial blood. • The menstrual blood flow is not clotted because of the Fibrinolysin acting on the blood in the uterine cavity and because it has clotted previously and therefore, it lacks fibrinogen. • Presence of clots signifies excess, pathological blood loss. • The uterine myometrium (muscle) shows strong contractions that expel the contents of the uterine cavity. If very strong these contractions can cause pain during menstruation called Dysmenorrhea.
HORMONES & THEIR ROLE IN MENSTRUAL CYCLE Hypothalamus: releases GnRH. Anterior Pituitary: releases FSH & LH. Ovarian Hormones: Estrogens & Progesterone
APPLIED PHYSIOLOGY • AMENORRHEA: Absence of menstruation • HYPOMENORRHEA: Decreased menstrual bleeding. • MENORRHAGIA: Excess menstrual bleeding. • OLIGOMENORRHEA: Decreased frequency of menstrual bleeding. • DYSMENORRHEA: Menstruation with pain.
The following hormones are produced by the ovary: • Steroid Hormones: - Estrogens - Androgens - Progesterone 2. Peptide Hormones: - Inhibin A: from granulosa and theca cells of the corpus luteum. Has a negative feedback effect on FSH but has little importance. - Inhibin B: from granulosa cells. Has a negative feedback effect on FSH secretion that is more potent than Inhibin A. - Activin: stimulates the FSH secretion. - Folliculostatin: inhibits the FSH secretion by binding and inactivating Activin. - Anti-Mullerian hormone: from the granulosa cells. It inhibits the recruitment of primordial follicles into the follicular pool by inhibiting aromatase production.
The main function of estrogen is to proliferate and promote the growth of specific cells in the body that are responsible for the development of most secondary sexual characteristics of the female. estrogen
ESTROGENS • Source: Estrogens are secreted in large quantities by the theca interna cells of the ovaries& the corpus luteum & to a smaller amount by the placenta and adrenal cortex. Estrogen is derived from androgens, esp. androstendione, which are secreted in large amounts in the theca interna cells. Androgens migrate from theca cells to the granulosa cells, where it is converted into estrogen by the activity of the aromatase enzyme (theca cells do not have the enzyme aromatase). • Chemistry: It is a steroid. • Different forms: - β- Estradiol or Estradiol (the most potent estrogen) - Estrone - Estriol (the least potent estrogen) • Half-life: 30-60 minutes • Transport: Only 2% is free; while 98% is bound with plasma proteins. mostly by albumin & to a lesser extent by the globulin called as sex hormone binding globulin (SHBG).
Functions of Estrogens: • Effect on Ovarian Follicles: Stimulatory • Effect on Uterus: prepares the uterus for pregnancy thru the following changes: - enlargement of uterus. - increased blood supply to endometrium. - Proliferation & dilatation of blood vessels & endometrial glands. 3. Effect on Fallopian tubes: Stimulatory aiding in the fertilization process in the fallopian tubes. 4. Effect on Vagina: stimulatory thus preventing certain common vaginal infections. 5. Feminizing Effects & Puberty: - Secondary Sexual characteristics: 1. Hair distribution 2. Skin: smooth & increased vascularity. 3. Body shape becomes feminine. 4. Pelvis: broadening of pelvis with increased transverse diameter. 5. Voice: high-pitched voice. 6. Effect on Breasts: aids in breast development preparing the breast for lactation. However, at birth due to expulsion of placenta, it leads to a decrease in estrogen levels and prolactin secretion starts. Administration of large amounts of estrogen prevents lactation as it has an anti-prolactin action.
7. Effect on Bones:Stimulates Osteoblastic activities. Because of decreased amounts of estrogen after menopause, it leads to Osteoporosis in old age. 8. Effect on Metabolism: - anabolism in proteins increasing total body proteins. - deposition of fat in the female body. 9. Effect on Electrolyte balance: causes sodium & water retention. This effect becomes more pronounced in pregnancy. 10. Effects on Gonadotropin secretion: Estrogen decreases the secretion of FSH and LH by inhibiting the secretion of GnRH of the hypothalamus as well as by a direct inhibitory effect on the adenohypophysis. 11. Effect on Blood Pressure: It increases the production of angiotensinogen in the liver leading to an increase in Blood pressure. This effect is likely to occur in women using contraceptives containing an estrogen. 12. Effects on blood clotting: It leads to an increase in the formation of blood clotting factors while causing a decrease in anti-thrombin III levels. These effects lead to blood clotting. In women on estrogen contraceptives, venous thrombosis can occur. 13. Carcinogenesis: In women, treatment with estrogen has been shown to increase the incidence of breast cancer.
The main function of the Progestins is to prepare the uterus for pregnancy & the breasts for lactation. progesterone: