Female Reproductive System
570 likes | 1.23k Views
Female Reproductive System. The Highlights. Hormones of the Female Reproductive Cycle. Control the reproductive cycle Coordinate the ovarian and uterine cycles. Hormones of the Female Reproductive Cycle. Key hormones include: FSH Stimulates follicular development LH

Female Reproductive System
E N D
Presentation Transcript
Female Reproductive System The Highlights
Hormones of the Female Reproductive Cycle • Control the reproductive cycle • Coordinate the ovarian and uterine cycles
Hormones of the Female Reproductive Cycle • Key hormones include: • FSH • Stimulates follicular development • LH • Maintains structure and secretory function of corpus luteum • Estrogens • Have multiple functions • Progesterones • Stimulate endometrial growth and secretion
Female Reproductive Organs • Ovary: female gonad • Uterine Tubes (fallopian tube, oviduct) - three parts: infundibulum, ampulla, isthmus
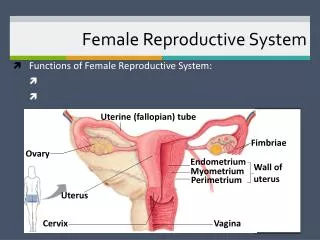
The Female Reproductive System in Midsagital View Figure 28.13
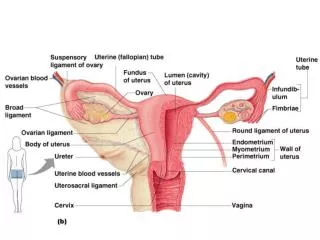
The Ovaries and Their Relationships to the Uterine Tube and Uterus Figure 28.14a, b
The Uterus • Muscular organ • Mechanical protection • Nutritional support • Waste removal for the developing embryo and fetus • Supported by the broad ligament and 3 pairs of suspensory ligaments
Uterine Wall Consists of 3 Layers: • Myometrium – outer muscular layer • Endometrium – a thin, inner, glandular mucosa • Perimetrium – an incomplete serosa continuous with the peritoneum • The site of implantation of developing embryo • And 3 parts: fundus, body, and cervix
Female Accessory Sex Organs: Uterus • Uterine endometrium has two layers: - basal layer - functional layer: built up and shed each cycle
The Uterus Figure 28.18c
The Uterine Wall Figure 28.19b
The Uterine CycleTo be discussed below Figure 28.20
Functions of the Ovary • Production of a mature oocyte, capable of fertilization and embryonic development. • Production of ovarian steroids (estradiol, progesterone). • Production of gonadal peptides (inhibin, activin).
Structural Organization of the Ovary • The main functional unit of the ovary is the follicle. • Follicles are composed of the oocyte, granulosa cells, and theca cells.
Stages of Follicular Growth • Follicles are present in a number of different stages of growth: - primordial follicles (resting) - primary, secondary, and antral follicles - preovulatory (Graafian) follicles
The Corpus Luteum • After the preovulatory follicle ovulates (releases its egg), it forms the corpus luteum.
FEMALE REPRODUCTIVE SYSTEM The Ovarian Cycle OVARY 3 to 5 million OOGONIA differentiate into PRIMARY OOCYTES during early development OOCYTES becomes surrounded by squamous (follicular) cells to become PRIMORDIAL FOLLICLES most PRIMORDIAL FOLLICLES undergo atresia leaving 400,000 at birth oocytes at birth arrested at Meiosis I (prophase)
OOGENESIS FEMALE REPRODUCTIVE SYSTEM OVARY THREE STAGES OF OVARIAN FOLLICLES CAN BE IDENTIFIED FOLLOWING PUBERTY: (each follicle contains one oocyte) (1) PRIMORDIAL FOLLICLES - very prevalent; located in the periphery of the cortex - a single layer of squamous follicular cells surround the oocyte (2) GROWING FOLLICLES - three recognizable stages: (a) early primary follicle (b) late primary follicle (c) secondary (antral) follicle (3) MATURE (GRAAFIAN) FOLLICLES - follicle reaches maximum size
FEMALE REPRODUCTIVE SYSTEM OVARIAN FOLLICLES (1) PRIMORDIAL FOLLICLES (2) GROWING FOLLICLES (a) early primary follicle - follicular cells still unilaminar but now are cuboidal in appearance - oocyte begins to enlarge (b) late primary follicle - multilaminar follicular layer; cells now termed granulosa cells - zona pellucida appears; gel-like substance rich in GAGs - surrounding stromal cells differentiate into theca interna and theca externa (b) secondary (antral) follicle - cavities appear between granulosa cells forming an antrum - follicle continues to grow - formation of cumulus oophorus and corona radiata (3) MATURE (GRAAFIAN) FOLLICLES
FEMALE REPRODUCTIVE SYSTEM HORMONAL REGULATION OF OOGENSIS AND OVULATION HYPOTHALAMUS release of GnRF which stimulates release of LH and FSH from the adenohypophysis (ANTERIOR PITUITARY)
CNS hypothalamus GnRH Pituitary FSH LH OVARY Neuroendocrine Regulation of Ovarian Functions Follicle Development E2, P Ovulation inhibin, activin Luteinization
Effects of GnRH on Gonadotropins • GnRH is released in a pulsatile manner, stimulating the synthesis and release of LH and FSH. • GnRH acts through its receptor on the pituitary gonadotroph cells, stimulating production of phospholipase C. • Recall that IP3 pathway causes gonadotropin release, while the DAG/PKC pathway causes gonadotropin synthesis.
Actions of FSH on Granulosa Cells FSH AC ATP Gs cAMP PKA CREB CRE Gene Expression Steroidogenic enzymes LH Receptor Inhibin Subunits Plasminogen activator
LH androgens Theca cells aromatase Granulosa cells FSH Ovarian Estradiol Production estradiol
Regulation of Progesterone Production • Progesterone is produced from theca cells, mature granulosa cells, and from the corpus luteum. • In this case, gonadotropins induce expression of - steroidogenic acute regulatory protein - P450 side chain cleavage
Actions of Estradiol • Estradiol also has important actions in a number of other tissues: - causes proliferation of uterine endometrium - increases contractility of uterine myometrium - stimulates development of mammary glands - stimulates follicle growth (granulosa cell proliferation) - effects on bone metabolism, hepatic lipoprotein production, genitourinary tract, mood, and cognition • Effects are mediated through the intracellular estrogen receptors (alpha and beta), and possible membrane effects.
Actions of Progesterone • Progesterone exerts positive and negative feedback effects on gonadotropin synthesis and release. • Progesterone also acts on many tissues: - stimulates secretory activity of the uterine endometrium - inhibits contractility of the uterine myometrium - stimulates mammary growth • The actions of progesterone are mediated through an intracellular P receptor, which acts as a transcription factor.
10-20 primordial follicles begin to develop in response to FSH and LH levels theca and granulosa cells transform into the corpus luteum and secrete large amounts of progesterone FSH and LH stimulate theca and granulosa production of estrogen and progesterone if fertilization does not occur, corpus luteum degenerates ... if fertilization does occur, HCG released from the embryo maintains corpus luteum surge of LH induces ovulation FEMALE REPRODUCTIVE SYSTEM The Menstrual Cycle HORMONAL REGULATION OF OOGENSIS AND OVULATION OVULATION FOLLICULAR PHASE LUTEAL PHASE
FEMALE REPRODUCTIVE SYSTEM The Menstrual Cycle HORMONAL REGULATION OF OOGENSIS AND OVULATION OVULATION: sharp surge in LH with simulataneous increase in FSH Meiosis I resumes; oocyte and surrounding cumulus break away and are extruded oocyte passes into oviduct ECTOPIC IMPLANTATIONS
The Menstrual Cycle • Women have ovulatory cycles of about 28 days in length. • Day 1 of the cycle is defined as the first day of menstruation. • There are two phases of the cycle, named after ovarian and uterine function during that phase: - first two weeks: follicular or proliferative stage - second two weeks: luteal or secretory stage • The preovulatory gonadotropin surges occur in the middle of the cycle (around day 14).
The Menstrual Cycle: The Ovary • Follicular phase: small antral follicles develop, a dominant follicle is selected and grows to the preovulatory stage. • Midcycle: the gonadotropin surges cause ovulation of the dominant follicle. • Luteal phase: the corpus luteum forms and becomes functional, secreting large amounts of progesterone, followed by estradiol (results in negative feedback, not positive feedback, because P increases before E2). • If pregnancy does not take place, the corpus luteum regresses, and P and E2 levels decrease.
The Menstrual Cycle: The Uterus • Proliferative stage: increasing estradiol levels stimulate proliferation of the functional layer of the uterine endometrium. - Results in increased thickness of the endometrium. - Increased growth of uterine glands (secrete mucus) and uterine arteries. • Secretory stage: progesterone acts on the endometrium. - uterine glands become coiled and secrete more mucus - uterine arteries become coiled (spiral arteries)
The Menstrual Cycle: The Uterus • If pregnancy doesn’t occur, P and E2 levels decrease at the end of the secretory stage. - vasospasm of arteries causes necrosis of tissue - loss of functional layer with bleeding of uterine arteries (menstruation)
FEMALE REPRODUCTIVE SYSTEM UTERUS ENDOMETRIUM undergoes cyclic changes which prepare it for implantation of a fertilized ovum TWO LAYERS: (1) FUNCTIONAL LAYER (stratum functionalis) - BORDERS UTERINE LUMEN - SLOUGHED OFF AT MENSTRATION - CONTAINS UTERINE GLANDS (2) BASAL LAYER (stratum basale) - RETAINED AT MENSTRATION - SOURCE OF CELLS FOR REGENERATION OF FUNCTIONAL LAYER STRAIGHT AND SPIRAL ARTERIES
FEMALE REPRODUCTIVE SYSTEM HORMONAL REGULATION OF UTERINE CYCLE (1) PROLIFERATIVE PHASE concurrent with follicular maturation and influenced by estrogens (2) SECRETORY PHASE concurrent with luteal phase and influenced by progesterone (3) MENSTRUAL PHASE commences as hormone production by corpus luteum declines
Male Reproductive System The Highlights
The Male Reproductive System in Midsagital View Figure 28.1
MALE REPRODUCTIVE SYSTEM TESTIS TUNICA ALBUGINEA - thick connective tissue capsule - connective tissue septa divide testis into 250 lobules - each lobule contains 1-4 seminiferous tubules and interstitial connective tissue (1) SEMINIFEROUS TUBULES - produce sperm INTERSTITIAL TISSUE - contains Leydig cells which produce testosterone (2) RECTUS TUBULES (3) RETE TESTIS (4) EFFERENT DUCTULES (5) EPIDIDYMIS
MALE REPRODUCTIVE SYSTEM SPERMATOGENESIS SPERMATOGONIA 1º SPERMATOCYTE 2º SPERMATOCYTE SPERMATIDS SPERMATIDS 2º SPERMATOCYTE 1º SPERMATOCYTE SERTOLI CELLS: - columnar with adjoining lateral processes - extend from basal lamina to lumen - Sertoli-Sertoli junctions divide seminiferous tubules into basal and adluminal compartments SERTOLI CELLS SPERMATOGONIA
Basal Lamina Daughter cell Type A spermatogonium remain at basal lamina as a precursor cell 2n 2n Spermatogonia (stem cells) 2n mitosis Daughter cell Type B Spermatagonium Moves to adluminal compartment n 1° spermatocyte Meiosis I completed n 2° spermatocyte n Meiosis II n n n n Early spermatids n n n n Late spermatids
MALE REPRODUCTIVE SYSTEM SPERMATOGENESIS THREE PHASES: (1) Spermatogonial Phase (Mitosis) (2) Spermatocyte Phase (Meiosis) (3) Spermatid Phase (Spermiogenesis) - acrosome formation; golgi granules fuse to form acrosome that contains hydrolytic enzymes which will enable the spermatozoa to move through the investing layers of the oocyte - flagellum formation; centrioles and associate axoneme (arrangement of microtubules in cilia) - changes in size and shape of nucleus; chromatin condenses and shedding of residual body (cytoplasm)
MALE REPRODUCTIVE SYSTEM HORMONAL REGULATION OF MALE REPRODUCTIVE FUNCTION HYPOTHALAMUS REGULATES ACTIVITY OF ANTERIOR PITUITARY (ADENOHYPOPHYSIS) ADENOHYPOPHYSIS SYNTHESIZES HORMONES (LH and FSH) THAT MODULATE ACTIVITY OF SERTOLI AND LEYDIG CELLS Luteinizing Hormone (LH): stimulates testosterone production by Leydig cells Follicle Stimulating Hormone (FSH): stimulates production of sperm in conjunction with testosterone by regulating activity of Sertoli cells SERTOLI CELLS STIMULATED BY FSH AND TESTOSTERONE RELEASE ANDROGEN BINDING PROTEIN WHICH BINDS TESTOSTERONE; THEREBY INCREASING TESTOSTERONE CONCENTRATION WITHIN THE SEMINIFEROUS TUBULES AND STIMULATING SPERMATOGENESIS