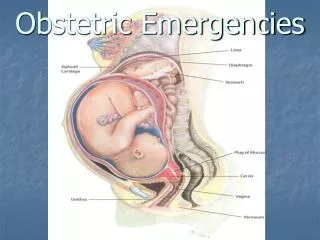
Obstetric Emergencies
Obstetric Emergencies. Dr Mohamed Abdul Hakim Kotb,MBBCH,MSC,MD Anaesthesia & ICU. Obstetric emergencies. Massive obstetric haemorrhage Non-haemorrhagic shock: Amniotic fluid embolism Acute uterine inversion Shoulder dystocia Eclampsia Cord prolapse Cardiac Arrest Anaphylaxis TRAUMA.

Obstetric Emergencies
E N D
Presentation Transcript
Obstetric Emergencies Dr Mohamed Abdul Hakim Kotb,MBBCH,MSC,MD Anaesthesia & ICU
Obstetric emergencies • Massive obstetric haemorrhage • Non-haemorrhagic shock: • Amniotic fluid embolism • Acute uterine inversion • Shoulder dystocia • Eclampsia • Cord prolapse • Cardiac Arrest • Anaphylaxis • TRAUMA
BASIC PRINCIPLES FOR OBSTETRIC EMERGENCIES. • Physiological changes in pregnancy modify: • Presentation of the problem • Normal physiological variables • Response to treatment • Both mother & fetus are affected by the pathology & subsequent treatment. • Mother’s welfare always takes precedence over fetal concerns --- Fetal survival is usually dependant on optimal maternal management.
MASSIVE OBSTETRIC HAEMORRHAGE • Major contributor to maternal mortality • Definition • Blood loss requiring replacement of patient’s total blood volume • Transfusion requiring > 10 u of blood in 24 hs • 50% replacement of blood vol. <3 hs period • Difficult to estimate blood loss • Problem of concealed bleeding • Uterus • Broad lig. • Peritoneal cavity
10 – 15% 500-1000ml Normal BP No signs. 15-25% 1000-1500ml BP ~ 100mmHg Dizziness, tachycardia 25-35% 1500-2000ml. BP ~ 70-80mmHg. Restlessness,pallor, oliguria. 35-45% 2000-3000ml 50-70mmHg Collapse, air hunger, anuria RECOGNISING SIGNIFICANT BLOOD LOSS
General Increased oxygen and cardiac output requirements of pregnancy may hamper adequate blood / volume replacement Placental bed perfusion 600 mls/min Blood loss underestimated Delayed or inadequate management Inadequate resources / personnel Specific Failure to anticipate coagulopathy PET, abruption, sepsis, IUFD, AFE. Abnormal placentation Placenta praevia / accreta Jehovah’s witness** Factors contributing to maternal death from catastrophic PPH
Mechanism of DIC • 1) intravascular infusion of thromboplastic substances that initiate the extrinsic coagulation system • placental abruption, IUFD • 2) conditions associated with endothelial cell damage, which activates both the extrinsic and intrinsic coagulation systems • eclampsia/ PET • 3) indirect effects of other disease, such as G- sepsis, AFE etc
Preventative Management PPH • Detect and treat antenatal anaemia • Active Management of Third Stage • Administration of a prophylactic oxytocin • Early cord clamping • Controlled cord traction of the umbilical cord. • Advantage of active management = reduction in the incidence of PPH by 40% • IV access plus collect blood for grouping and cross matching if assessed as at risk.
Available from Royal Women’s Hospital, Carlton, Clinical Practice Guidelines: http://www.rwh.org.au/rwhcpg/womenshealth.cfm?doc_id=3333
Management Principles • Organisation • restoration of blood volume • correction of coagulopathy • evaluating response to treatment • monitoring PR, BP, CVP, ABG, UOP • If resuscitation is adequate P & BP should return to normal • treat the cause • abruption • placenta praevia • uterine rupture • placenta accreta
Available from Royal Women’s Hospital, Carlton, Clinical Practice Guidelines: http://www.rwh.org.au/rwhcpg/womenshealth.cfm?doc_id=3333
NON-HAEMORRHAGIC OBSTETRIC SHOCK Uncommon but responsible for majority of maternal deaths in developed countries. -Amniotic fluid embolus -Acute uterine inversion
Amniotic Fluid Embolism Passage of amniotic fluid debris into maternal circulation Obstructs pulmonary circulation Cardio-respiratory arrest
AMNIOTIC FLUID EMBOLISM • Clinical features • Multiparous women • Precipitous labour • Presence of intact membranes • Sudden dyspnea • Hypotension • Seizure activity not uncommon • If survive initial insult • 70% suffer non-cardiogenic pulmonary oedema • ARDS
AMNIOTIC FLUID EMBOLISM • Diagnosis • Consider in all obstetric patients with sudden collapse. • Differential • PTE • Septic shock • MI • Aspiration pneumonia • Allergy to drug
Management • Secure airway • treat cardiovascular collapse • central venous line • acute left ventricular failure: digoxin • dopamine • correct coagulopathy • treat metabolic/electrolyte abnormalities
Acute Uterine Inversion Most commonly arises from mismanaged 3rd stage
Presentation • Sudden collapse in 3rd stage • Degree of shock inconsistent with blood loss • Shock is neurogenic in nature • Traction on infundibular pelvic ligament • May be no palpable fundus • Mass in vagina/introitus
Management • Avoid mismanagement of 3rd stage of labour • Once occurs • Anti-shock measures • If placenta still attached remove after uterus is replaced • Manual replacement of uterus • O’Sullivans hydrostatic pressure • Surgical correction
‘It all comes,’ said Pooh crossly, ‘of not having front doors big enough’
Macrosomia (>4kg) maternal diabetes post dates maternal obesity high maternal wgt gain in pregnancy advanced maternal age previous large infant previous shoulder dystocia Intrapartum protracted late active phase prolonged 2nd stage delay in head descent in 2nd stage mid-pelvic operative delivery Risk Factors The combination of macrosomia and delay in 2nd stage predicts 35% of shoulder dystocia
Eclampsia 1/1500
Complications • Cerebrovascular injury • pulmonary oedema • coagulopathy • maternal/fetal death • HELLP syndrome
Presentation • Hypertension, hyperreflexia, clonus, headache, visual changes, seizure • 20% have diastolic BP<90, normal reflexes, and urinary protein <2+ • 70% of deaths due to intracerebral haemorrhage
Management • Goals: – Stabilization of the mother/seizure control • MgSO4 therapy: 4-6 g over 20 min followed by infusion of 1-3 g/hr, OR • Thiopental or diazepam followed by MgSO4 infusion – Airway management – Avoiding aspiration
Prolapsed Cord 1/500 deliveries Most occur during ARM
Presentation • Cord visible outside the introitus • CTG abnormalities appear • variable decelerations • fetal bradycardia Note: fetal or maternal injury due to hasty intervention
Management • Keep cord warm - replacing in vagina may help • Keep pressure off cord by gloved hand in vagina lifting fetal part off the cord • Positioning,Maternal O2, IV access • If fetus is alive, operative delivery - CS if not able to deliver vaginally • If fetus is dead, vaginal delivery if presentation allows
Anaphylaxis • vasodilatation, smooth muscle contraction, glandular secretion, increased capillary permeability • Management: • oxygen • colloid • bronchodilator • adrenaline (despite Ux stimulatory effect) • anti-histamine (if angioneurotic oedema) • steroid (for refractory bronchospasm)
Maternal cardiac emergency • Acute: • AMI • Tocolytic therapy • Aortic dissecting aneurysm • Peripartum cardiomyopathy: • 1 in 50000, 50% progress to end-stage heart failure (heart Tx), 50% recurrence. • Suspect if acute SOB, chest pain, abN ECG, signs LVF/RVF • Traumatic myocardial contusion: ie: MCA
Drug Overdose • Illicit drugs: heroin, cocaine and amphetamines (these 2 can cause hypertension, ^ C.O., decrease Uterine blood flow, APH, cerebral haemorrhage, convulsions, arrhythmias). • Drug overdose • Drug error • Anaphylaxis • Hypermagnesaemia: • wide QRS on ECG, 5-6mmol/l lose tendon reflex • resp. paralysis, SA and AV node block • cardiac arrest. • Treatment: CaGluconate 10% 10ml slow IV
CARDIO-PULMONARY ARREST • Cardiac arrest rare in pregnancy (1 in 30000 deliveries) • Usually associated with particular obstetric complications like amniotic fluid embolism, drug toxicity from Magnesium sulphate & local anesthetics.
Technique for external cardiac massage: • External cardiac massage in non-obstetric patient provides 30% cardiac output. • After 20 weeks reduced further due to veno-caval compression. • Relief of aorto-caval compression part of BLS: • left lateral tilt --- decreased efficacy of compressions • wedge 270 angle allows 80% of maximal force to be dissipated • rescuer’s thigh as wedge. • Sodium bicarbonate controversial as it leads to fetal acidosis but pH has to be kept above 7.30 to prevent uterine vasoconstriction. • International Liaison Committee on Resuscitation (ILCOR) “ if there is no response to ALS, peri-mortem caesarean delivery should be made within 5 minutes of arrest”
TRAUMA • Occurs in 6-7% of all pregnancies. • Hospital admissions only 0.3- 0.4 % of all pregnancies. • 1% of all trauma cases are pregnant. • Maternal deaths associated most commonly with head injuries & severe hemorrhage. • Fetal deaths associated with placental abruption & maternal death.
Management • Initial resuscitation should follow normal plan of ABC. • Hypotension may not be present until 35% or more blood volume is lost. • Aorto-caval compression release • Rule out pelvic fractures, uterine injury & retro-peritoneal hemorrhage • Fetal monitoring with cardio-tocographic monitor • Rh immunoglobulin – within 72 hours. • Radiation hazards: 1st trimester >5 rads Chest x-ray < 5 rads Pelvic film <1 rads Abdomino-pelvic CT scan 5-10 rads
BURNS • Increased levels of prostaglandins predispose to pre-term labour. • Replacement of fluids vis-à-vis increased volumes in pregnancy. • Inhalational injury- hypoxia & carbon monoxide poisoning • Infections- prophylactic antibiotics controversial • Topical Povodine iodine- affects fetal thyroid functions
Thank You Thank You Thank You Thank You