Chapter 16 - Enterobacteriaceae
Chapter 16 - Enterobacteriaceae. MLAB 2434 – Clinical Microbiology Cecile Sanders & Keri Brophy-Martinez. Chapter 16 - Enterics. Family Enterobacteriaceae often referred to as “enterics” Four major features: All ferment glucose (dextrose) All reduce nitrates to nitrites

Chapter 16 - Enterobacteriaceae
E N D
Presentation Transcript
Chapter 16 - Enterobacteriaceae MLAB 2434 – Clinical Microbiology Cecile Sanders & Keri Brophy-Martinez
Chapter 16 - Enterics • Family Enterobacteriaceae often referred to as “enterics” • Four major features: • All ferment glucose (dextrose) • All reduce nitrates to nitrites • All are oxidase negative • All except Klebsiella, Shigella and Yersinia are motile
Microscopic and Colony Morphology • Gram negative bacilli or coccobacilli • Non-spore forming • Colony morphology on BAP or CA of little value, as they look the same, except for Klebsiella • Selective and differential media are used for initial colony evaluation (ex. MacConkey, HE, XLD agars)
Classification of Enterics • Due to the very large number of organisms in the Family Enterobacteriaceae (see Table 16-11), species are grouped into Tribes, which have similar characteristics (Table 16-1, page 466) • Within each Tribe, species are further subgrouped under genera
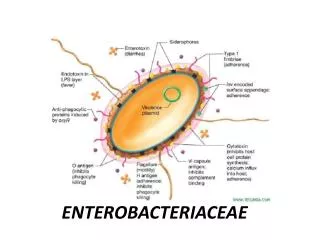
Virulence and Antigenic Factors of Enterics • Ability to colonize, adhere, produce various toxins and invade tissues • Some possess plasmids that may mediate resistance to antibiotics • Many enterics possess antigens that can be used to identify groups • O antigen – somatic, heat-stable antigen located in the cell wall • H antigen – flagellar, heat labile antigen • K antigen – capsular, heat-labile antigen
Clinical Significance of Enterics • Enterics are ubiquitous in nature • Except for few, most are present in the intestinal tract of animals and humans as commensal flora; therefore, they are sometimes call “fecal coliforms” • Some live in water, soil and sewage
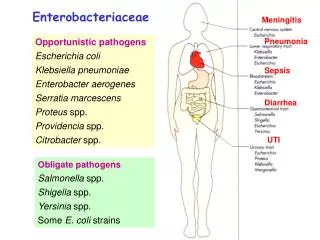
Clinical Significance of Enterics (cont’d) • Based on clinical infections produced, enterics are divided into two categories: • Opportunistic pathogens – normally part of the usual intestinal flora that may produce infection outside the intestine • Primary intestinal pathogens – Salmonella, Shigella, and Yersinia sp.
Escherichia coli • Most significant species in the genus • Important potential pathogen in humans • Common isolate from colon flora
Escherichia coli (cont’d) • Characteristics • Dry, pink (lactose positive) colony with surrounding pink area on MacConkey
Escherichia coli (cont’d) • Ferments glucose, lactose, trehalose, & xylose • Positive indole and methyl red tests • Does NOT produce H2S or phenylalanine deaminase • Simmons citrate negative • Usually motile • Voges-Proskauer test negative
Escherichia coli (cont’d) • Infections • Wide range including meningitis, gastrointestinal, urinary tract, wound, and bacteremia • Gastrointestinal Infections • Enteropathogenic (EPEC) – primarily in infants and children; outbreaks in hospital nurseries and day care centers; stool has mucous but not blood; identified by serotyping
Escherichia coli (cont’d) • Enterotoxigenic (ETEC) – “traveler’s diarrhea”; watery diarrhea without blood; self-limiting; usually not identified, other than patient history and lactose-positive organisms cultured on differential media • Enteroinvasive (EIEC) – produce dysentery with bowel penetration, invasion and destruction of intestinal mucosa; watery diarrhea with blood; do NOT ferment lactose; identified via DNA probes
Escherichia coli (cont’d) • Enterohemorrhagic (EHEC serotype 0157:H7) – associated with hemorrhagic diarrhea and hemolytic-uremic syndrome (HUS), which includes low platelet count, hemolytic anemia, and kidney failure; potentially fatal, especially in young children; undercooked hamburger, unpasteurized milk and apple cider have spread the infection; does NOT ferment sucrose; identified by serotyping
Escherichia coli (cont’d) • Enteroaggregative (EaggEC) – cause diarrhea by adhering to the mucosal surface of the intestine; watery diarrhea; symptoms may persist for over two weeks • Urinary Tract Infections • E. coli is most common cause of UTI and kidney infection in humans • Usually originate in the large instestine • Able to adhere to epithelial cells in the urinary tract
Escherichia coli (cont’d) • Septicemia & Meningitis • E. coli is one of the most common causes of septicemia and meningitis among neonates; acquired in the birth canal before or during delivery • E. coli also causes bacteremia in adults, primarily from a genitourinary tract infection or a gastrointestinal source • Escherichia hermannii – yellow pigmented; isolated from CSF, wounds and blood • Escherichia vulneris - wounds
Klebsiella, Enterobacter, Serratia & Hafnia sp. • Usually found in intestinal tract • Wide variety of infections, primarily pneumonia, wound, and UTI • General characteristics: • Some species are non-motile • Simmons citrate positive • H2S negative • Phenylalanine deaminase negative • Some weakly urease positive • MR negative; VP positive
Klebsiella species • Usually found in GI tract • Four major species • K. pneumoniae is mostly commonly isolated species • Possesses a polysaccharide capsule, which protects against phagocytosis and antibiotics AND makes the colonies moist and mucoid • Has a distinctive “yeasty” odor • Frequent cause of nosocomial pneumonia
Klebsiella species (cont’d) • Significant biochemical reactions • Lactose positive • Most are urease positive • Non-motile
Enterobacter species • Comprised of 12 species; E. cloacaeand E. aerogenes are most common • Isolated from wounds, urine, blood and CSF • Major characteristics • Colonies resemble Klebsiella • Motile • MR negative; VP positive
Serratia species • Seven species, but S. marcescens is the only one clinically important • Frequently found in nosocomial infections of urinary or respiratory tracts • Implicated in bacteremic outbreaks in nurseries, cardiac surgery, and burn units • Fairly resistant to antibiotics
Serratia species (cont’d) • Major characteristics • Ferments lactose slowly • Produce characteristic pink pigment, especially when cultures are left at room temperature S. marscens on nutrient agar →
Hafnia species • Hafnia alvei is only species • Has been isolated from many anatomical sites in humans and the environment • Occasionally isolated from stools • Delayed citrate reaction is major characteristic
Proteus, Morganella & Providencia species • All are normal intestinal flora • Opportunistic pathogens • Deaminate phenylalanine • All are lactose negative
Proteus species • P. mirabilis and P. vulgaris are widely recognized human pathogens • Isolated from urine, wounds, and ear and bacteremic infections • Both produce swarming colonies on non-selective media and have a distinctive “burned chocolate” odor • Both are strongly urease positive • Both are phenylalanine deaminase positive
Proteus species (cont’d) • A exhibits characteristic “swarming” • B shows urease positive on right
Morganella species • Morganella morganii is only species • Documented cause of UTI • Isolated from other anatomical sites • Urease positive • Phenylalanine deaminase positive
Providencia species • Providencia rettgeri is pathogen of urinary tract and has caused nosocomial outbreaks • Providenicia stuartii can cause nosocomial outbreaks in burn units and has been isolated from urine • Both are phenylalanine deaminase positive
Citrobacter species • Citrobacter freundii associated with nosocomial infections (UTI, pneumonias, and intraabdominal abscesses) • Ferments lactose and hydrolyzes urea slowly • Resembles Salmonella sp.
Salmonella • Produce significant infections in humans and certain animals • On differential selective agar, produces clear, colorless, non-lactose fermenting colonies with black centers (if media contains indicator for hydrogen sulfide)
Salmonella (cont’d) • Salmonella on MacConkey
Salmonella (cont’d) • Lactose negative • Negative for indole, VP, phenylalanine deaminase, and urease • Most produce H2S • Do not grow in potassium cyanide • Large and complex group of organisms; grouped by O, H, and Vi (for virulence) antigens
Salmonella (cont’d) • Clinical Infections • Acute gastroenteritis or food poisoning • Source = handling pets, insufficiently cooked eggs and chicken, and contaminated cooking utensils • Occurs 8 to 36 hours after ingestion • Requires a high microbial load for infection • Self-limiting in health individuals (antibiotics and antidiarrheal agents may prolong symptoms)
Salmonella (cont’d) • Typhoid and Other Enteric Fevers • Prolonged fever • Bacteremia • Involvement of the RE system, particularly liver, spleen, intestines, and mesentery • Dissemination to multiple organs • Occurs more often in tropical and subtropical countries
Salmonella (cont’d) • Salmonella Bacteremia • Carrier State • Organisms shed in feces • Gallbladder is the site of organisms (removal of gallbladder may be the only solution to carrier state)
Shigella species • Closely related to the Escherichia • All species cause bacillary dysentery • S. dysenteriae (Group A) • S. flexneri (Group B) • S. boydii (Group C) • S. sonnei (Group D)
Shigella (cont’d) • Characteristics • Non-motile • Do not produce gas from glucose • Do not hydrolyze urea • Do not produce H2S on TSI • Lysine decarboxylase negative • ONPG positive (delayed lactose +) • Fragile organisms • Possess O and some have K antigens
Shigella (cont’d) • Clinical Infections • Cause dysentery (bloody stools, mucous, and numerous WBC) • S. sonnei is most common, followed by S. flexneri (“gay bowel syndrome”) • Humans are only known reservoir • Oral-fecal transmission • Fewer than 200 bacilli are needed for infection in health individuals
Yersinia species • Consists of 11 named species • Yersinia pestis • Causes plague, which is a disease primarily of rodents; transmitted by fleas • Two forms of plague, bubonic and pneumonic • Gram-negative, short, plump bacillus, exhibiting “safety-pin” or “bipolar” staining
Yersinia species • Yersinia enterocolitica • Most common form of Yersinia • Found worldwide • Found in pigs, cats and dogs • Human also infected by ingestion of contaminated food or water • Some infections result from eating contaminated market meat and vacuum-packed beef • Is able to survive refrigerator temperatures (can use “cold enrichment” to isolate) • Mainly causes acute gastroenteritis with fever
Yersinia species • Yersinia pseudotuberculosis • Pathogen of rodents, particularly guinea pigs • Septicemia with mesenteric lymphadenitis, similar to appendicitis • Motile at 18 to 22 degrees C
Laboratory Diagnosis of Enterics • Collection and Handling • If not processed quickly, should be collected and transported in Cary-Blair, Amies, or Stuart media • Isolation and Identification • Site of origin must be considered • Enterics from sterile body sites are highly significant • Routinely cultured from stool
Laboratory Diagnosis of Enterics (cont’d) • Media for Isolation and Identification of Enterics • Most labs use BAP, CA and a selective/differential medium such as MacConkey • On MacConkey, lactose positive are pink; lactose negative are clear and colorless
Laboratory Diagnosis of Enterics (cont’d) • For stools, highly selective media, such as Hektoen Enteric (HE), XLD, or SS is used along with MacConkey agar • Identification • Most labs use a miniaturized or automated commercial identification system, rather than multiple tubes inoculated manually
Laboratory Diagnosis of Enterics (cont’d) • Identification (cont’d) • All enterics are • Oxidase negative • Ferment glucose • Reduce nitrates to nitrites
Laboratory Diagnosis of Enterics (cont’d) • Common Biochemical Tests • Lactose fermentation and utilization of carbohydrates • Triple Sugar Iron (TSI) • ONPG • Glucose metabolism • Methyl red • Voges-Proskauer
Laboratory Diagnosis of Enterics (cont’d) • Common Biochemical Tests (cont’d) • Miscellaneous Reactions • Indole • Citrate utilization • Urease production • Motility • Phenylalanine deaminase • Decarboxylase tests
Screening Stools for Pathogens • Because stools have numerous microbial flora, efficient screening methods must be used to recover any pathogens • Enteric pathogens include Salmonella, Shigella, Aeromonas, Campylobacter, Yersinia, Vibrio, and E. coli 0157:H7
Screening Stools for Pathogens (cont’d) • Most labs screen for Salmonella, Shigella, and Campylobacter; many screen for E. coli 0157:H7 • Fecal pathogens are generally lactose-negative (although Proteus, Providencia, Serratia, Citrobacter and Pseudomonas are also lactose-negative)