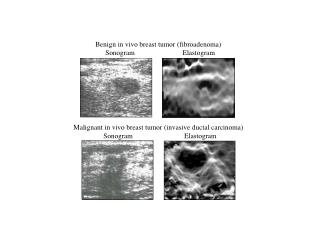
Benign Breast Problems
Benign Breast Problems. Folake Falaki, MD PGY 2 Emory Family Medicine May 28, 2009. Outline. Introduction Anatomy Structure of the breast Classification Initial approach to breast problems Diagnostic workup Conclusion References. Introduction.

Benign Breast Problems
E N D
Presentation Transcript
Benign Breast Problems Folake Falaki, MD PGY 2 Emory Family Medicine May 28, 2009
Outline • Introduction • Anatomy • Structure of the breast • Classification • Initial approach to breast problems • Diagnostic workup • Conclusion • References
Introduction • Breast problems are a major reason why women visit the primary care physician • Breast diseases in women constitute a spectrum of benign and malignant disorders • The most common breast problems for which women consult a physician are breast pain, nipple discharge and a palpable mass. • Benign breast lesion is a non-cancerous lesion. According to American Cancer society , when tissue biopsy is examined under the microscope, nine out of every 10 women will have some type of abnormality AAFP journal , April 15, 2000. Volume 61/ No. 8
Anatomy • The breast is a modified sweat gland with a mass of glandular, fatty and fibrous tissues on the pectoralis muscles in the chest wall • It is attached to the chest wall by fibrous strands called coopers ligaments • The glandular tissues of the breast consist of lobules, lobes and ducts • Fatty and fibrous tissues surround the milk producing system ( lobules and ducts)
Anatomy Major hormones responsible for breast development are estrogen, progesterone and prolactin. The blood supply is through the internal mammary artery, axillary artery intercostal artery Venous drainage is through the Internal mammary vein, axillary vein and intercostal veins
Anatomy • Lymphatic drainage • Majorly to the Axillary nodes • Inter mammary and the supra clavicular lymph nodes. • Three Lymph Node Levels • Level I – Lateral and inferior to Pectoralis Minor • Level II – Deep to Pectoralis Minor • Level III – Medial to Pectoralis Minor • Rotter’s – Between Pectoralis Minor & Major • Nerves • Long Thoracic Nerve: • Serratus Anterior m. • Winged Scapula • Thoracodorsal Nerve: • Latissimus Dorsi • Intercostobrachial Nerve
Classification Based On Histologic Types • Non Proliferative Lesion • Simple Cyst • Complex cyst • Proliferative Lesions – Without Atypia • Ductal hyperplasia • Fibroadenoma • Intraductal papilloma • Sclerosing Adenoma • Radial Scars • Atypical Hyperplasia • Atypical ductal hyperplasia • Atypical lobular hyperplasia Schnitt, SJ. Benign breast disease and breast cancer risk: morphology and beyond. Am J surg pathology 2003;27:836
Classification Based On Clinical Features • Mastalgia • Cyclic • Non Cyclic • Tumors and Masses • Nodularity or glandular • Cysts • Galactoceles • Fibroadenoma • Sclerosing Adenosis • Lipoma • Harmatoma • Diabetic Mastopathy • Cystosarcoma Phylloides AAFP journal , April 15, 2000. Volume 61/ No. 8
Classification Based On Clinical Features (Cont’d) • Nipple discharge • Galactorrhea • Abnormal nipple discharge • Breast infections and Inflammation • Intrinsic mastitis • Postpartum engorgement • Lactation mastitis • Lactation breast abscess • Chronic recurrent subareolar abscess • Acute mastitis associated with macrocystic breasts • Extrinsic infections • Mondor’s Disease • Hidradenitis suppurativa J khosa, Benign breast disease including mastalgia ppt
Classification • Lesions with Increased Risk of Ca • Ductal hyperplasia • Sclerosing adenosis • Complex fibroadenomas • Atypical hyperplasia • Radial scars Micheal S sabel .Overview of benign breast disease. Uptodate 2008, November 14
Classification • Lesions with no Increased risk of Ca • Fibrocystic disease • Duct ectasia • Solitary papillomas • Simple fibroadenomas • Mastitis or breast abscess • Galactocele • Fat necrosis • Lipoma
Breast Pain (Mastalgia) • Most common breast symptom for which women consult the physician • More common in premenopausal women than in post menopausal women • Can be cyclical (physiological) or non cyclical Micheal S Sabel. Initial approach to the woman with breast problems. http://uptodateonline.com 2008, November 6
Breast Pain (Mastalgia) Cyclic Pain ( Physiologic) • Usually Bilateral and poorly localized. • Occurs in about 60% of premenopausal women except menopausal women on hormonal replacement therapy • Often described as heaviness , swelling or tenderness that radiates to the arm and axilla • Associated with menstrual cycle , Most severe before menstruation • Has variable Duration and Resolve spontaneously after menses • Attributed to fibrocystic breast changes • Etiology unknown, thought to be related to Gonadotrophic and ovarian hormones
Mastalgia Non-Cyclic Pain • Most common in women 40 to 50 yrs of age • Often unilateral • Usually described as sharp, burning pain localized in the breast • Occasionally secondary to the presence of Fibroadenoma and or cyst • Menstrual irregularity, emotional stress, trauma, MSK, scars from previous biopsies and medications have been associated Micheal S Sabel. Initial approach to the woman with breast problems. http://uptodateonline.com 2008, November 6
Evaluation & Management of Breast Pain • Mastalgia should be treated when: • It is severe enough to interfere with a woman’s life style • It occurs more than a few days every month. • History and Physical • Diagnostic work up • Mammogram Micheal S sabel .Overview of benign breast disease. Uptodate 2008, November 14
Management of Breast Pain Treatment Goals • Alleviate pain • Reduce or relieve irregularity • Rule out cancer of the breast
Management of Breast Pain • Diet and Lifestyle Modification • Elimination of Methylxanthines, Caffeine and Chocolates • Reassurance • Supportive Bra • Low fat and high complex carbohydrate • Vitamin E supplementation • Evening Primrose oil Micheal S sabel .Overview of benign breast disease. Uptodate 2008, November 14
Management of Breast Pain • Pharmacological Treatment • NSAIDs • OCPs • Danazol 100- 400mg per day • 75% of women with non cyclic pain will be symptom free • SE: Weight gain , menstrual irregularity , acne , hirsutism • Tamoxifen 10mg • Bromocriptine – prolactin antagonist • Surgery has no role in management of breast pain Micheal S sabel .Overview of benign breast disease. Uptodate 2008, November 14
Evaluation & Management of Breast Pain AAFP journal , April 15, 2000. Volume 61/ No. 8
Breast Masses • Normal glandular tissue of the breast is nodular • This is a general pattern or consistency of the breast which include persistent lumpiness or nodularity which is generally not abnormal when it is related to the menstrual cycle. • Dominant masses are characterized by persistence throughout the menstrual cycle
Breast Masses: Cysts Cystic Breast Mass • Common cause of dominant breast mass • May occur at any age, but uncommon in post menopausal women • Fluctuates with menstrual cycle • Well demarcated from the surrounding tissue • Characteristically firm and mobile • May be tender • Difficult to differentiate from solid mass Micheal S sabel .Overview of benign breast disease. Uptodate 2008, November 14
Breast Masses: Cysts • Fibrocystic Breast Disease • Most common of all benign breast disease • Most common between ages 20- 50 • 50% of women with Fibrocystic changes have clinical symptoms • 53% have histologic changes • Believed to be associated the Imbalance of progesterone and estrogen. • May present with bilateral cyclic pain, breast swelling, palpable mass and heaviness
Fibrocystic Breast Disease • Physical Examination • Tenderness • Increased engorgement and more dense breast • Increased lumpiness / glandular • Occasional spontaneous nipple discharge Micheal Sabel .Overview of benign breast disease. Uptodate 2008, November 14
Mammogram Cystic outline No calcification No increased density Ultra Sonogram Cyst Fine Needle Aspiration Outpatient procedure Non bloody fluid Cyst disappears If bloody fluid, surgical biopsy of cyst is required Reexamination 4-6 weeks after aspiration Breast Cysts: Diagnostics
Management of Breast Cysts AAFP journal , April 15, 2000. Volume 61/ No. 8
Breast Mass: Fibroadenomas • Simple: Second most common benign breast lesion • Benign solid tumors containing glandular as well as fibrous tissue . Usually present as well defined, mobile mass • Commonly found in women between the ages of 15 and 35 years • Cause is unknown, thought to be due to hormonal influence • May increase in size during pregnancy or with estrogen therapy • Giant: Fibroadenomas over 10cm in size • Excision is recommended • Juvenile • Variant of fibroadenomas • Found in young women between the ages of 10 -18. • Vary in size from 5 - 20cm in diameter. Usually painless, solitary, unilateral masses • Excision is recommended
Breast Mass: Fibroadenomas (Cont’d) • Complex • Complex fibroadenomas contain other proliferative changes such as sclerosing adenosis, duct epithelial Hyperplasia, epithelial calcification. • Associated with slightly increased risk of cancer Dupont, WD page, DL, parl, FF, et al. Long term risk cancer in women with fIbroadenoma. NEJM 1994;331:10 Carty, NJ, Carter, c, Rubin, C et al management of fibroadenoma of the breast. Annals of royal college of surgeon England 1995:77:127 Micheal S sabel .Overview of benign breast disease. Uptodate 2008, November 14
Breast Mass • Phylloides Tumors: • Rapidly growing • One in four malignant • One in Ten Metastasize • Create bulky tumors that distort the breast • May ulcerate through the skin due to pressure necrosis • Treatment consists of wide excision unless metastasis has occurred • Fat Necrosis: • Rare • Secondary to trauma- often not remembered • Tender, ill defined mass • Occasionally skin retraction • Treat with excisional biopsy
Breast Mass • Galactocele • Milk filled cyst from over distension of a lactiferous duct. • Presents as a firm non tender mass in the breast, • Commonly in upper quadrants beyond areola. • Diagnostic aspiration is often curative. • Duct ectasia: • Generally found in older women. • Dilatation of the subareolar ducts can occur. • A palpable retroareolar mass, nipple discharge, or retraction can be present. • Tx involves excision of area
Breast Mass • Gynecomastia: • Benign growth of the glandular tissue of the male breast. • Due to an imbalance in the estrogen to androgen activity. • May be unilateral or bilateral • Common in infancy, adolescence and adult life • Pseudogynecomastia may be seen obese individuals • Causes include; drugs, chronic dxs, metabolic, pubertal, • Hormonal, tumors, idiopathic, hypogonadism. Braunstein, GD. Gynecomastia. NEJM 1993;328:490
Nipple Discharge • Majority of causes are benign • Most common cause is lactational • Overstimulation also common • Prolactin secreting tumors • Hypothyroidism • Drugs • Intraductal and other carcinomas • Unilateral, spontaneous, bloody discharge is suspicious
Nipple Discharge • Intraductal Papilloma • Benign growth within ductal system • Presents as bloody nipple discharge • Excision is the only way to differentiate from carcinoma • Galactorrhea • Bilateral milky discharge • Obtain prolactin level, TSH level
Nipple Discharge • Good history • Prolactin & TSH levels • Mammogram • Decrease stimulation
Breast Inflammation & Infections • Mastitis • Most common in lactating female • Dry, cracked fissured areola/nipple complex provides portal for infection • Usually caused by Staph/Strep organisms • Rule out malignancy • Treat with heat, continued breast feeding, • Antibiotics for 10-14 days to cover staph and strept infections
Breast Inflammation & Infections • Abscess • May present with breast swelling, tenderness and fever • On PE, breast is tender , warm and fluctuant, may also have purulent discharge • Treated by surgical drainage
Breast Inflammation & Infections • Mondor’s Disease • Phlebitis of the thoracoepigastric and lateral thoracic vein • Palpable, visible, skin retraction over tender extending to chest wall • Spontaneous or related to trauma • Ultrasound may be helpful in confirming this diagnosis. • Treatment self-limited, can use NSAIDs • Mammogram if over 35yo to r/o malignancy
Breast Inflammation & Infections • Chronic Subareolar Abscess • Occurs at base of lactiferous duct, and squamous metaplasia of duct may occur. • Sinus tract to areola develops • Treatment requires complete excision of sinus tract • Recurrence is common • Mastitis Neonatorum • Occurs within few weeks of birth • Response to mothers hormone exposure (prolactin, estrogen) • Resolves spontaneously • Occasionally becomes infected
Congenital Breast Disease • About 1-5 % of the population have accessory nipples, and less commonly accessory breast • Usually develop along the milk line • Most common site for accessory nipple is below the breast • Most common site for accessory breast is in the axilla • Rarely require treatment except for cosmetic reasons • Subject to the same diseases as the normal breast. J Micheal Dixon .ABC of breast diseases. 3 rd edition BMJ 2005 Gershon Efron. Benign breast disease ppt , google health search
Approach to Breast Problems • History • Age • Family history (Cancer) • Onset • Duration Discharge • Frequency • Lump , Nodules Trauma • Menstruation (menarche, menopause, contraceptives) Pain • Inspection • Symmetry • Skin / Nipple Change • Bulges / Retractions
Approach to Breast Problems • Palpation • Breast • Axilla • Supraclavicular
Breast Examination • The breast examination starts with inspection of both breast • Sitting up with arms in relaxed position, • Both arms raised over the head • Hands on the hips • Complete regional lymph node examination while patient is in the sitting position. • Bimanual may be done while patient is still in the sitting position, useful in patient with large pendulous breast • Complete with the patient in a supine position, with the arms raised above the head, breast exam can be accomplished with either concentric circles, radial approach, or vertical strip approach • Areas examined should extend from the clavicle superiorly to the rib cage inferiorly and from the sternum medially to the mid axillary line laterally Micheal S Sabel. Initial approach to the woman with breast problems. http://uptodateonline.com 2008, November 6
Diagnostic Work Up • Ultrasound • Mammography • FNA vs. Core Biopsy • Incisional biopsy • Excisional biopsy • Cyst aspiration • MRI
Diagnostic Work Up • Ultrasonography: First diagnostic test of choice to differentiate a cystic mass from a solid mass • Mammogram: Not routinely done in women younger than 35yo, however not inappropriate in a suspicious mass in younger women • Digital mammography is superior to conventional • A normal mammogram at any age does not eliminate the need for further evaluation of a suspicious mass. • MRI: Not indicated for the work up of undiagnosed mass. Reserved for diagnostic dilemmas and should be used with discretion due to false positive results • FNA: Useful for cystic lesions. If lesion is completely drained and fluid not bloody or cloudy, no further evaluation needed Micheal S Sabel. Initial approach to the woman with breast problems. http://uptodateonline.com 2008, November 6
Diagnostic Work Up • Core Needle Biopsy: This provides a best diagnostic information for solid palpable mass which can be visualized on the USS or mammogram • Excisional Biopsy: Useful in cases where core needle biopsy is non diagnostic, non concordant with imaging results or yield any high risk changes • Incisional Biopsy: useful when core needle biopsy is not helpful in confirming diagnosis Micheal S Sabel. Initial approach to the woman with breast problems. http://uptodateonline.com 2008, November 6
BI-RADS Classification BI-RADS Classification – features 0 - Need additional imaging 1 - Negative – routine in 1 yr 2 - Benign finding – routine in 1 yr 3 - Probably benign, 6mo follow-up 4 - Suspicious abnormality, biopsy recommended 5 - Highly suggestive of malignancy; appropriate action should be taken
Conclusion • Benign breast problems account for the majority of breast problems seen in women • Breast complaints need careful assessment with thorough history and physical as well as diagnostic work up if indicated • Women with breast problems can present with a mass, pain, nipple discharge or skin changes. They can also be asymptomatic • It is important to rule out breast cancer Micheal S Sabel. Initial approach to the woman with breast problems. http://uptodateonline.com 2008, November 6
References 1. AAFP journal , April 15, 2000. Volume 61/ No. 8 2 Schnitt, SJ. Benign breast disease and breast cancer risk: morphology and beyond. Am J surg pathology 2003;27:836 3.J khosa, Benign breast disease including mastalgia ppt 4. Dupont, WD page, DL, parl, FF, et al. Long term risk cancer in women with fIbroadenoma. NEJM 1994;331:10 5. Carty, NJ, Carter, c, Rubin, C et al management of fibroadenoma of the breast. Annals of royal college of surgeon England 1995:77:127 6. Micheal S sabel .Overview of benign breast disease. Uptodate 2008, November 14 7. J Micheal Dixon .ABC of breast diseases. 3 rd edition BMJ 2005 8.Gershon Efron. Benign breast disease ppt , google health search 9. Micheal S Sabel. Initial approach to the woman with breast problems. http://uptodateonline.com 2008, November 6 10. Braunstein, GD. Gynecomastia. NEJM 1993;328:490