Heart Failure
Heart Failure. Jenny Looi. Heart failure is a chronic (or long term)condition that effects men and women , of which a problem with the structure or function of the heart can no longer supply a sufficient blood flow to meet the body’s needs.

Heart Failure
E N D
Presentation Transcript
Heart Failure Jenny Looi
Heart failure is a chronic (or long term)condition that effects men and women , of which a problem with the structure or function of the heart can no longer supply a sufficient blood flow to meet the body’s needs. Heart disease is when your coronary arteries (the arteries supplying blood and oxygen to the heart muscle) clog themselves with fatty material called ‘plaque’ or ‘atheroma’. Plaque slowly builds up on the tinner wall of the arteries, causing them to become narrow. The process is called ‘atherosclerosis’ and starts in early age. It can well advanced by Middle age.
There are a number of diseases, medical conditions and other factors that can place people at a higher-than-average risk for heart failure. Not everyone with these factors develop heart failure, but they put extra stress on the heart that may lead to the condition. The odds of developing heart failure are especially high in people who have more than one of these risk factors.
Common causes of heart failure include coronary heart disease, previous heart attack, long-term high blood pressure, heart rhythm disorder, alcohol and drug abuse, heart defects present at birth, diabetes and cardiomyopathy (disease of the heart muscle). The less common causes of heart failure include disease of the heart valves, an abnormally low number of red blood cells (severe anemia), and thyroid problems. Some of our lifestyle factors like cigarette smoking and a history of heart failure or other cardiovascular diseases, may also increase the chances of heart failure.
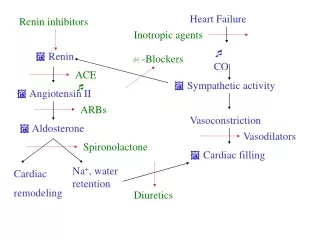
The treatment of heart failure is aimed at correcting both the underlying disorder, as well as the precipitating cause (i.e. ischaemia valvular heart disease, anaemia, thyrotociosisetc), as well as reducing cardiac work. Angiotensin converting enzyme (ACE) inhibitors, angiotensin receptor antagonists and spironolactone have all been associated with a reduction in morality in patients who suffer from chronic heart failure. Surgery (i.e. transplantation, mechanical assist devices) has a definite place in young patients with chronic dilated cardiomyopathy with severe heart failure. Other theraputic agents (i.e. growth hormone, thyroxine, and antioxidants) are yet to be shown to be of benefit. Management of heart failure (i.e. ischaemia, valvular disease, hypertension) maintenance of sinus rhythm, as well as reducing excessive neurohumoral activation can reduce morality and improve morbidity in patients with the underlaying disorder.
Symptoms of heart failure are traditionally divided into ‘left’ and ‘right’ sided, recognising that the left and right ventricles of the heart supply different proportions of the circulation. However, heart failure is not exclusively back failure. Left sided forward failure overlaps with the right sided backward failure. Additionally, the most common cause of right-sided heart failure is left-sided heart failure. It is common for patients to present with both sets of signs and symptoms.
Making changes in your lifestyle is the best way to prevent heart failure and lower your risk of developing heart disease. It’s also important to control certain medical conditions such as high blood pressure or diabetes, to lower your chances of development. Quit smoking. Smoking greatly increases your risk for heart disease. Also avoid second hand smoke. Lower your cholesterol. High cholesterol must be advised by your doctor to lower it. Eating a heart-healthy diet, exercising can help. Control your blood pressure. People who have high blood pressure have a high risk of developing heart disease. Studies have shown that the lowering of blood pressure to normal levels can reduce the cases of heart failure by half. Limiting alcohol intake (moderately drinking two drinks a day), and controlling stress will help keep your blood pressure in a healthy range. Control diabetes. Taking your medicines as directed and working with your doctor to manage your diet will help control diabetes.
Statistics (Australia)
Older people are more likely to develop have heart failure: 2.5% of Australians aged 55-64 years have heart failure increasing to 8.2% for those ages 75 years or over. Men are more likely to develop heart disease, but women make up more than two-thirds of Australians with heart failure. Death rates from heart failure are falling, but the reasons for this are not clear. Age standardised death rates for heart failure as an underlying or associated cause of death fell by 29% between 1997 and 2003. An estimate of at least 300,000 people over 45 have chronic heart failure.
Chronic heartfailure (CHF) places a heavy burden not only onpatients and their families but also on society, through enormoususe of health care resources. CHF has an overall populationprevalence of approximately 1–3%, rising to approximately10% in the very elderly. Following a first hospital admissionfor heartfailure, patients have a 5-year mortality of 75% —a survival rate worse than that for most forms of cancer. CHFimpairs quality of life more than almost any other chronic medicalproblem. Hospital admissions for CHF have increased markedlyover the past two decades. CHF accounts for about 5% of allmedical admissions and approximately 2% of total health careexpenditure. Despite improvements in medical management, under-treatmentis common. Because of the increase in survival after acute myocardialinfarction and ageing of the population, the number of patientswith CHF will increase rapidly in most industrialized countries.CHF will still pose one of the greatest health care challengesof the 21st century. Chronic heart failure (CHF) places a heavy burden not only on patients and their families, but also in society, through enormous use of health care resources.
Bibliography Wikipedia Mayoclinic.com goredforwomen.com.au hrspatients.org anzca.edu.au aihw.gov.au